Featured Case
-
Abstract
A 31-year-old female, suffered from chronic Irritable Bowel Disease and was provisionally diagnosed with Ulcerative colitis. The presenting complaints were frequent blood-stained watery stools, more than 6 times a day, and did not get relief even on taking conventional medicines for a period of 5 years. She now consulted Dr KG Raveendran, who diagnosed this clinical condition as Pittaja Grahani. The treatment protocol was to address the atipravrtti of vayu, tikshnamsha of pitta and mandyatva of kapha. With Ayurvedic treatments as an out-patient, for one1 year and in-patient treatment for a period of one month, she got complete relief from her symptoms. Post Ayurvedic treatment, she passed stools only once or twice a day, and with no blood stains.
Irritable Bowel Disease- Quality of Life Questionnaire and MAYO Score was used to assess the treatment outcomes. The questionnaire at baseline was 163 and at endpoint it reduced to 133, indicating a significant improvement in the Quality of Life. The MAYO Score was 8 at baseline indicating a severe disease activity. At endpoint, it was 3, indicating a mild disease activity.
This case report demonstrates the successful Ayurvedic management of a chronic case of Ulcerative colitis, where the patient did not get relief inspite of taking conventional medicine for 5 years.
-
Summaries
-
Listen
-
Watch
-
View
-
Read
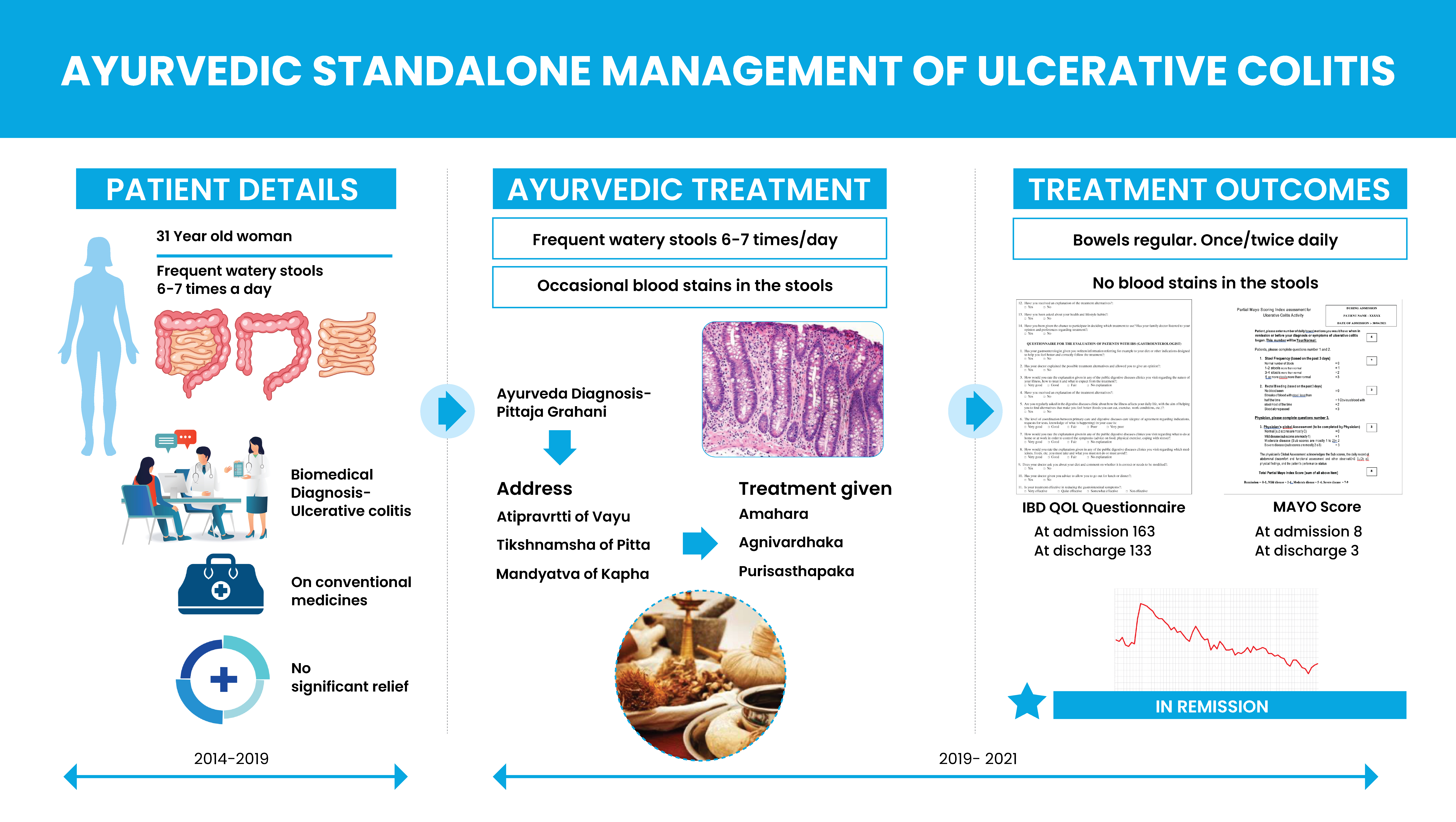
A 31-year-old female, suffered from chronic Irritable Bowel Disease and was provisionally diagnosed with Ulcerative colitis. The presenting complaints were frequent blood-stained watery stools, more than 6 times a day, and did not get relief even on taking conventional medicines for a period of 5 years. She now consulted Dr KG Raveendran, who diagnosed this clinical condition as Pittaja Grahani. The treatment protocol was to address the atipravrtti of vayu, tikshnamsha of pitta and mandyatva of kapha. With Ayurvedic treatments as an out-patient, for one1 year and in-patient treatment for a period of one month, she got complete relief from her symptoms. Post Ayurvedic treatment, she passed stools only once or twice a day, and with no blood stains.
Irritable Bowel Disease- Quality of Life Questionnaire and MAYO Score was used to assess the treatment outcomes. The questionnaire at baseline was 163 and at endpoint it reduced to 133, indicating a significant improvement in the Quality of Life. The MAYO Score was 8 at baseline indicating a severe disease activity. At endpoint, it was 3, indicating a mild disease activity.
This case report demonstrates the successful Ayurvedic management of a chronic case of Ulcerative colitis, where the patient did not get relief inspite of taking conventional medicine for 5 years.
-
-
Timeline
-
Tabulated Summary
-
Narrative
TITLE OF CASE
Successful Ayurvedic intervention in improving the Quality of Life in Chronic case of Ulcerative Colitis non-responsive to conventional medicine- A Case report
Dr KG Raveendran
ABSTRACT
A 31-year-old female, suffered from chronic Irritable Bowel Disease and was provisionally diagnosed with Ulcerative colitis. She did not get relief even on taking conventional medicines for a period of 5 years. She now consulted Dr KG Raveendran, with the presenting complaints of frequent blood-stained watery stools, more than 6 times a day. This was diagnosed as Pittaja Grahani and treatment protocol was to address the atipravrtti of vayu, tikshnamsha of pitta and mandyatva of kapha. With Ayurvedic treatments as an out-patient, for 1 year and in-patient treatment for a period of 1 month, she got complete relief from her symptoms. Post Ayurvedic treatment, she passes stools only once or twice a day, and with no blood stains.
Irritable Bowel Disease- Quality of Life Questionnaire and MAYO Score was used to assess the treatment outcomes. The questionnaire at baseline was 163 and at endpoint it reduced to 133, indicating a significant improvement in the Quality of Life. The MAYO Score was 8 at baseline indicating a severe disease activity. At endpoint, it was 3, indicating a mild disease activity.
KEYWORDS
Ayurveda, Ulcerative colitis, Irritable Bowel Disease, Grahani, Pittaja Grahani
INTRODUCTION
Ulcerative colitis (UC) is a type of Irritable Bowel Disease. This is a long-term pathology, where the colon and/or rectum are inflicted with inflammation and ulcers. The main symptoms are abdominal pain and diarrhea mixed with blood. The condition can also be accompanied by episodes of fever, weight loss and anemia. The intensity of the symptoms may vary from mild to severe at different time intervals. Sometimes, there may be absolutely no symptoms in-between flare-ups.
Diagnostic criteria: Detailed history taking, and clinical evaluation are the basic diagnostic criteria. Imaging (colonoscopy, ileocolonoscopy, upper endoscopy) helps in confirming the diagnosis.
Treatments given: The target of treatment in Ulcerative Colitis are threefold—improve quality of life, achieve steroid-free remission and minimize the risk of cancer. The choice of treatment depends on extent of being affected, severity and the course of the disease.
PATIENT INFORMATION
A 31-year-old female patient suffering from Ulcerative colitis since 6 and half years presented with frequent watery stools (more than 6 times a day) with blood. She did not get any relief despite taking conventional medicine for 5 years. She got good relief on taking Ayurvedic medicines on an Outpatient, but when an acute flare up happened, she had to get admitted.
Medical History: In the patient’s words, 6 and half years back, she ate a mango and developed acute diarrhoea. She was treated for food poisoning with antibiotics for a long period of time. Though that episode was completely cured, the symptoms persisted on & off. In 2014, a Distal Colonoscopy done diagnosed evidence of mild inflammation commencing from rectum till sigmoid. Further mucosa is free from inflammation/ulceration/stricture/growth (IBD in query). Patient refused to undergo further colonoscopy or biopsy, so a provisional diagnosis was made as Ulcerative Colitis. And she was prescribed Coolgut 800mg. She took it for 5 years (2014-2019). She did not get significant relief. In 2014 weight was 39 kg, in May 2015- 37kg, June 2015- was 39 kg (last recorded), but she became very weak and exhausted. She stopped the allopathic medicine and consulted Dr Raveendran in his OP in 2019. In 2019 her weight was 31kg. After starting Ayurvedic medicines, she had regular bowel movement with only occasional rectal bleeding. This continued until April 2021. But suddenly there was a flare-up in her symptoms with 6-7 episodes of watery stools in a day. Now she mentioned about frequent mouth ulcers and boils in the eye on & off. She noticed that anxiety and stress was aggravating her symptoms. So, she was admitted in the Ayurvedic hospital on 30-4-21 and took In patient treatment until 14/6/21. Past illness- H/o chicken pox, Measles, Herpes in childhood. Marital Status- Married, no kids. Planning for conception. Menstrual History- Regular cycles in 35 days, 5-6 days bleeding. Patient has no comorbidities.
Family History: Father has Diabetes mellitus & Hypertension. Mother has Hypertension. Mother’s Sister is diagnosed with Ulcerative colitis & Rheumatoid arthritis
Psychosocial History: Since the severe relapse occurred, she is very anxious and stressed and this aggravates her symptoms simultaneously.
PHYSICAL EXAMINATION/CLINICAL FINDINGS
CVS- S1, S2 Heard. GI system- P/A – On examination Bloated, On percussion – Resonance heard over the quadrants of abdomen, Tenderness: + Lower quadrant of abdomen, Warmth: +: Pulse – 62/min: Weight – 31.4 kgs. Blood pressure – 106/70 mm hg: Temperature – Normal. Appetite – Increased. Bowel – Loose with blood. Micturition – Normal. Tongue – Mildly coated.
Patient is very lean built and appears weak and febrile. IBD QOL SCORE – 163. MAYO SCORE - 8 (baseline on 30.4.21) (data attached) indicating the severity of the disease.
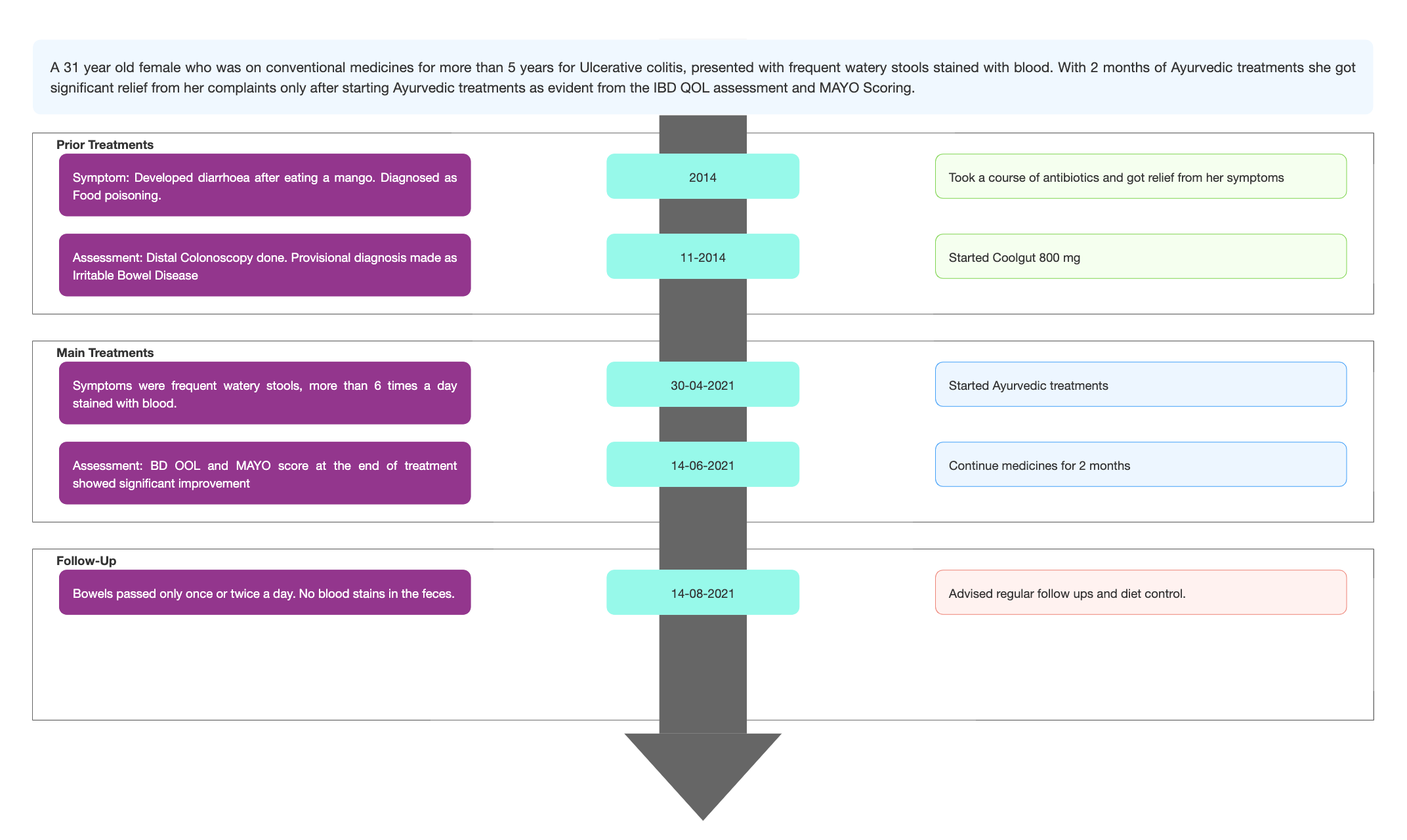
TIMELINE
Image 1. Timeline of events attached below
DIAGNOSTIC ASSESSMENT
Modern Diagnostic parameter: The records available from the modern hospital confirm the diagnosis as Irritable Bowel Disease. A colonoscopy would help confirm the diagnosis, but the patient refused to do it. So she was provisionally diagnosed as Ulcerative Colitis.
Image 2. Blood Parameters done at baseline attached below
Image 3. Images available to confirm the diagnosis attached below
Image 4. PARTIAL MAYO SCORING INDEX (at baseline) attached below
Ayurvedic Assessment was done based on the clinical evaluation by the ayurvedic physician.
Differential Diagnosis- This does not apply as the patient came in with a definite diagnosis.
Prognosis: Though the disease is not life-threatening, getting medical help is the most important aspect in the management of this condition. If left untreated, there is always a risk of getting colon cancer. The episodes may or may not be severe, but the right diet and lifestyle is very important. There is no cure for the condition, it must be managed with medical intervention. There can be complications like bleeding, dehydration, nutritional loss, inflammation of the inner organs and even a perforated bowel. Addressing the clinical condition is very important.
In this patient, the onset is chronic. Despite the long history of the complaints, and being non-responsive to conventional medicines, she could get relief with Ayurvedic interventions.
THERAPEUTIC INTERVENTION
See the tab ' Treatment Details'
FOLLOW-UP AND OUTCOMES
The patient is asked to come for a follow up after 6 months.
Clinician-based assessment:
Subjective parameters:
A physical examination was done before and after treatment and this revealed significant improvement.
Table 1. Vitals documented before and after treatment
During admission
During discharge
Appetite -- Increased
Appetite -- Normal
Bowel – Loose with blood
Bowel – Semisolid consistency, Once with no bleeding
Micturition – Normal
Micturition – Normal
Temperature – Normal
Temperature – Normal
Tongue – Mild coated
Tongue – Mild coated
Sleep – Disturbed
Sleep – Improved
Pulse – 62/min
Pulse – 66/min
Weight – 31.4 kgs
Weight – 31.8 kgs
Blood pressure – 106/70 mmhg
Blood pressure – 108/70 mmhg
Table 2. Physical examination/Clinical Findings documented before and after treatment
During admission
During discharge
P/A – On examination
Bloated
P/A – On examination
Mild Bloatedness present
On percussion – Resonance heard over the quadrants of abdomen
On percussion – Mild Resonance heard over the quadrants of abdomen
Tenderness - + Lower quadrant of abdomen
Tenderness - Nil
Warmth - +
Warmth – Localised
Objective Parameters: Blood parameters were assessed after the Ayurvedic treatment
Table 3. Blood parameters before and after Ayurvedic Treatment
On 04/05/2021 (After admission)
On 11/06/2021 (Before discharge)
Hb – 9.6
Hb – 10.8
Platelets count – 2.1 Lakhs/cumm
Platelets count – 2.6 Lakhs/cumm
ESR – 65
Esr – 48 mm/hr
C R P – 1.41 mg/L
C R P – 0.50 mg/L
Image 5. Endpoint Blood report attached below
Patient-assessed: MAYO Scoring and IBD QOL Questionnaire were done pre and post treatment.
At the baseline, the score was 8 indicating ‘severe’ disease activity. At the endpoint, the score was 3 indicating a ‘mild’ disease activity.
Image 6. MAYO Scoring Index at endpoint attached below
IBD - Quality of life assessment questionnaire was also filled up at the endpoint to assess the severity of the disease. At baseline, the score was 163. At the endpoint, it was 133 indicating the disease activity has reduced.
Table 4. The IBD QOL Questionnaire documented before and after treatment
IBD QOL Questionnaire
S No
QUESTIONNARE
SCORE (DURING ADMISSION) 30.4.21
SCORE (DURING DISCHARGE) 14.6.21
1
I feel helpless because of my bowel problems
5
3
2
I am embarrassed by the smell caused by my bowel problems
5
2
3
I am bothered by how much time I spend on the toilet.
5
3
4
I feel vulnerable to other illnesses because of my bowel problems
5
5
5
I feel fat because of my bowel problems.
1
1
6
I feel like I'm losing control of my life because of my bowel problems
5
3
7
I feel my life is less enjoyable because of my bowel problems
5
3
8
I feel uncomfortable when I talk about my bowel problems
3
3
9
I feel depressed about my bowel problems
5
5
10
I feel isolated from others because of my bowel problems
5
5
11
I have to watch the amount of food I eat because of my bowel problems
5
5
12
Because of my bowel problems, sexual activity is difficult for me
5
5
13
I feel angry that I have bowel problems
5
5
14
I feel like I irritate others because of my bowel problems
5
5
15
I worry that my bowel problems will get worse
5
5
16
I feel irritable because of my bowel problems
5
5
17
I worry that people think I exaggerate my bowel problems
5
3
18
I feel I get less done because of my bowel problems
5
5
19
I have to avoid stressful situations because of my bowel problems
5
5
20
My bowel problems reduce my sexual desire
5
4
21
My bowel problems limit what I can wear
5
5
22
I have to avoid strenuous activity because of my bowel problems
5
5
23
I have to watch the kind of food I eat because of my bowel problems
5
5
24
Because of my bowel problems, I have difficulty being around people I do not know well
4
2
25
I feel sluggish because of my bowel problems
5
2
26
I feel unclean because of my bowel problems
5
2
27
Long trips are difficult for me because of my bowel problems
5
3
28
I feel frustrated that I cannot eat when I want because of my bowel problems
5
5
29
It is important to be near a toilet because of my bowel problems
5
2
30
My life revolves around my bowel problems
5
5
31
I worry about losing control of my bowels
5
5
32
I fear that I won't be able to have a bowel movement
5
2
33
My bowel problems are affecting my closest relationships
5
5
34
I feel that no one understands my bowel problems
5
5
Total Score
163
133
Intervention adherence and tolerability – The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment- By monitoring the patient.
Adverse and unanticipated events- None reported.
DISCUSSION:
The treating physician diagnosed this condition as Pittaja Grahani and the line of treatment adopted was to reduce the atipravritti of vayu and simultaneously reduce the tikshnamsha of pitta and kapha mandyatva. The treatment targets were as follows.
a. Reduce the atipravritti of vayu and reduce the amatva of purisha
b. Purisha soshana cikitsa
c. Agni vardhaka cikitsa
d. Vatapittahara line
e. Purisha sthapana
Over all amahara, doshavarana hara, agnivardhaka and purisha sthapana cikitsa were adopted.
PATIENT’S PERSPECTIVE
Not available.
LEARNING POINTS/TAKE-HOME MESSAGES
Even in patients of Chronic conditions like Ulcerative colitis, where satisfactory outcomes were not obtained despite taking conventional medicines can keep Ayurvedic treatments as an alternative for an effective management.
INFORMED CONSENT
Written consent obtained from patient.
ACKNOWLEDGEMENTS
None
CONFLICT OF INTEREST
None declared.
FUNDING
None
REFERENCE
- Fabián O, Kamaradová K. Morphology of inflammatory bowel diseases (IBD). Cesk Patol. 2022 Spring;58(1):27-37. English. PMID: 35387455.
- Ordás I, Eckmann L, Talamini M, Baumgart DC, Sandborn WJ. Ulcerative colitis. Lancet. 2012 Nov 3;380(9853):1606-19. doi: 10.1016/S0140-6736(12)60150-0. Epub 2012 Aug 20. PMID: 22914296.
- Shakyawal et al. World Journal of Pharmaceutical Research. Grahani Roga and their management. Vol 10, Issue 3, 2021
Image 1. Timeline of events
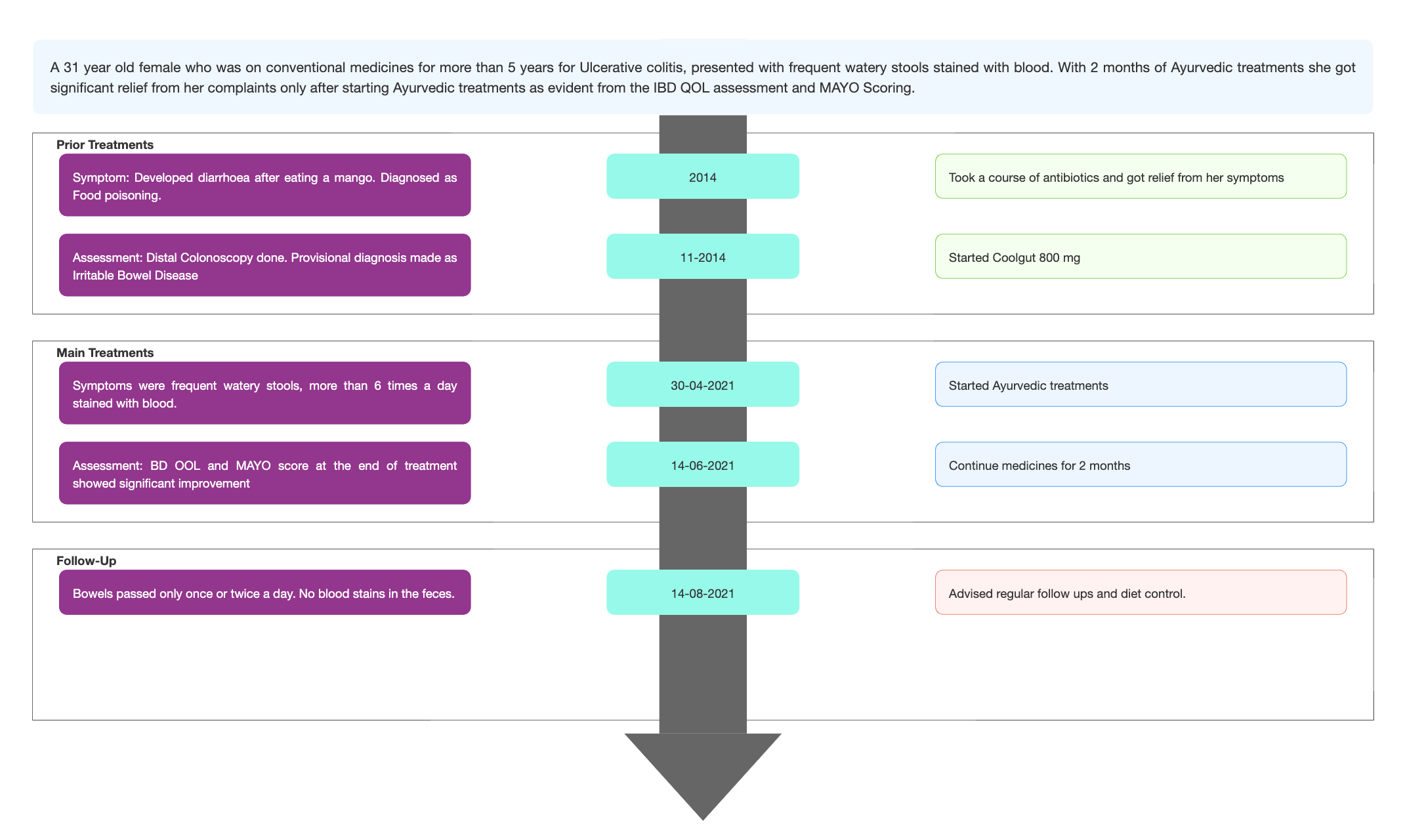
Image 2. Blood Parameters done at baseline May 2021
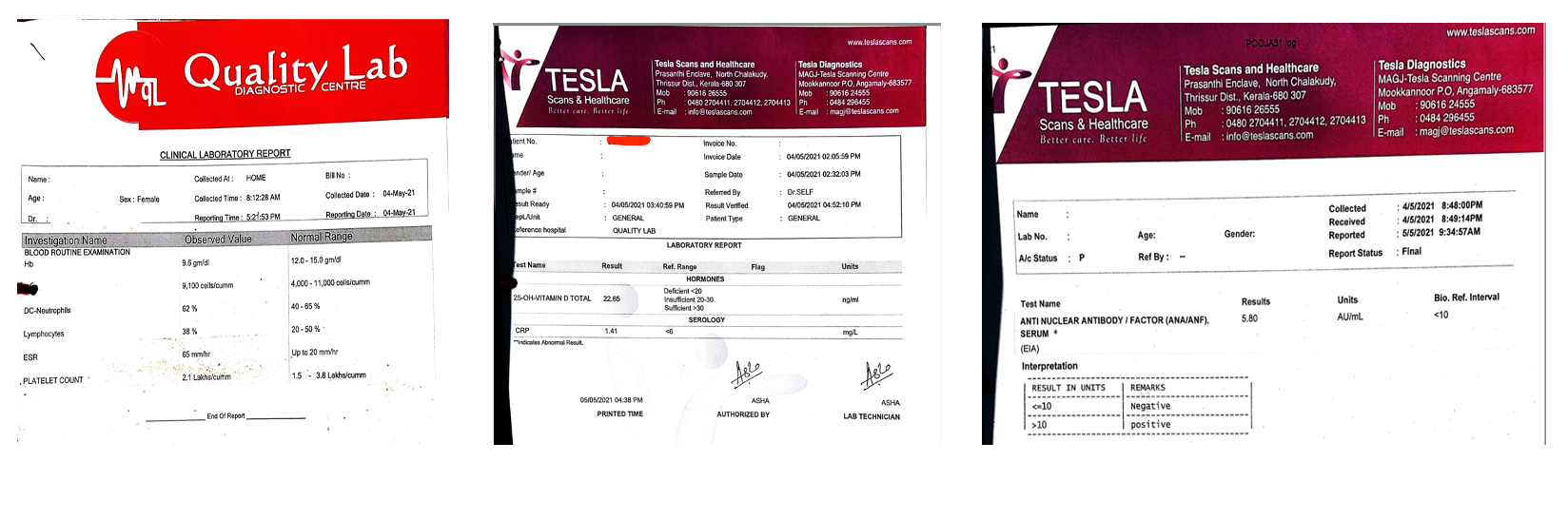

Image 3. Images available to confirm the diagnosis (Distal Colonoscopy 2014 and Ileocolonoscopy 2015)
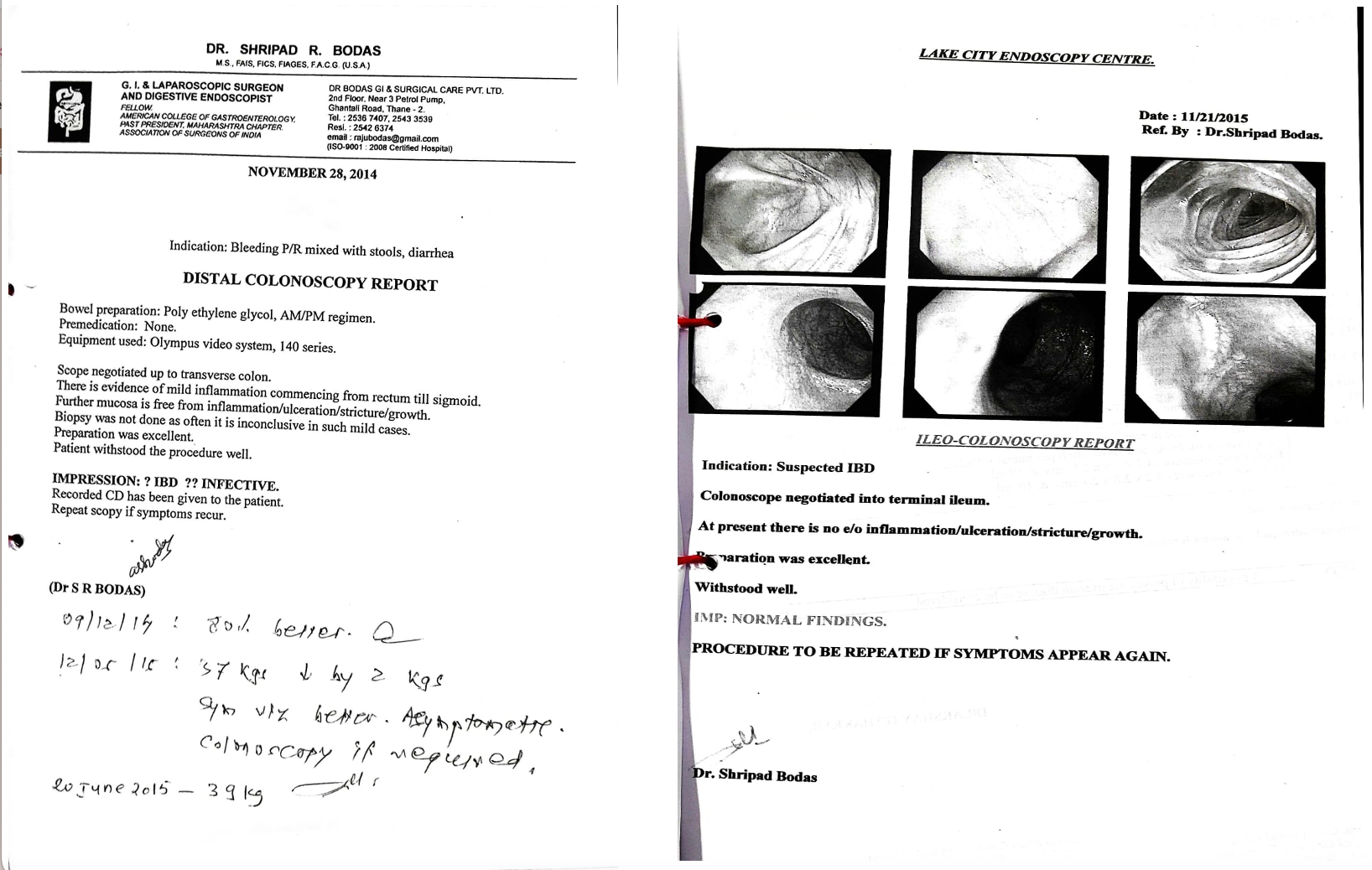
Image 4. PARTIAL MAYO SCORING INDEX (at baseline)

Image 5. Endpoint Blood report dated June 2021
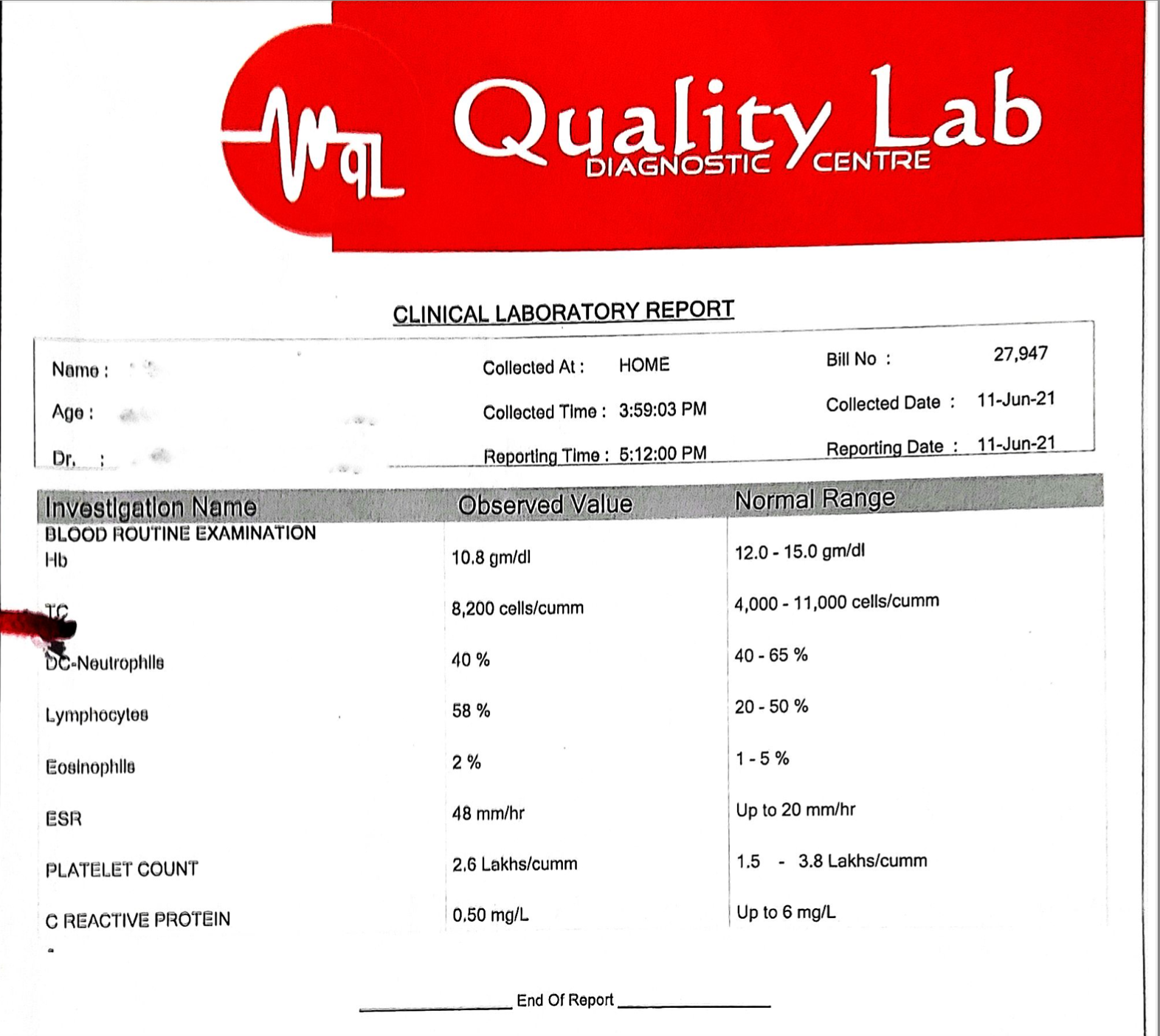
Image 6. Endpoint MAYO Score dated June 2021

-
Immersive Learning
-
Modern Diagnosis
MODERN DIAGNOSIS: Ulcerative colitis
About the disease:
Ulcerative colitis (UC) is a type of Irritable Bowel Disease. This is a long-term pathology, where the colon and/or rectum are inflicted with inflammation and ulcers. The main symptoms are abdominal pain and diarrhea mixed with blood. The condition can also be accompanied by episodes of fever, weight loss and anemia. The intensity of the symptoms may vary from mild to severe at different time intervals. Sometimes, there may be absolutely no symptoms in-between flare-ups.
In this 31-year-old female patient, the complaints of frequent watery stools started 6 and half years back, which was initially considered as food poisoning. That specific episode was treated with conventional medicine and cured. But since then, she has been suffering from the complaints of frequent watery stools on & off. Based on the colonoscopy report, a provisional diagnosis was made as Ulcerative colitis. Despite taking conventional medicines for more than 5 years, she got no relief. She was losing weight and was only 31kgs at baseline.
Diagnostic criteria: Detailed history taking, and clinical evaluation are the basic diagnostic criteria. Imaging (colonoscopy, ileocolonoscopy, upper endoscopy) helps in confirming the diagnosis.
In this patient, the clinical examination, blood parameters, assessment scoring and imaging were done.
Table 1. Irritable Bowel Disease - Quality of Life Questionnaire filled by the patient at baseline
S No
IBD QOL Questionnaire
QUESTIONNARE
SCORE (DURING ADMISSION) 30.4.21
1
I feel helpless because of my bowel problems
5
2
I am embarrassed by the smell caused by my bowel problems
5
3
I am bothered by how much time I spend on the toilet.
5
4
I feel vulnerable to other illnesses because of my bowel problems
5
5
I feel fat because of my bowel problems.
1
6
I feel like I'm losing control of my life because of my bowel problems
5
7
I feel my life is less enjoyable because of my bowel problems
5
8
I feel uncomfortable when I talk about my bowel problems
3
9
I feel depressed about my bowel problems
5
10
I feel isolated from others because of my bowel problems
5
11
I have to watch the amount of food I eat because of my bowel problems
5
12
Because of my bowel problems, sexual activity is difficult for me
5
13
I feel angry that I have bowel problems
5
14
I feel like I irritate others because of my bowel problems
5
15
I worry that my bowel problems will get worse
5
16
I feel irritable because of my bowel problems
5
17
I worry that people think I exaggerate my bowel problems
5
18
I feel I get less done because of my bowel problems
5
19
I have to avoid stressful situations because of my bowel problems
5
20
My bowel problems reduce my sexual desire
5
21
My bowel problems limit what I can wear
5
22
I have to avoid strenuous activity because of my bowel problems
5
23
I have to watch the kind of food I eat because of my bowel problems
5
24
Because of my bowel problems, I have difficulty being around people I do not know well
4
25
I feel sluggish because of my bowel problems
5
26
I feel unclean because of my bowel problems
5
27
Long trips are difficult for me because of my bowel problems
5
28
I feel frustrated that I cannot eat when I want because of my bowel problems
5
29
It is important to be near a toilet because of my bowel problems
5
30
My life revolves around my bowel problems
5
31
I worry about losing control of my bowels
5
32
I fear that I won't be able to have a bowel movement
5
33
My bowel problems are affecting my closest relationships
5
34
I feel that no one understands my bowel problems
5
35
163
The IBS-QOL consists of 34 items, each with a five-point response scale:
Items 1, 2, 4, 8-10, 12, 13, 16, 25-29, 34
1. Not at all 2. Slightly 3. Moderately 4. Quite a bit 5. Extremely
Items 3, 5-7, 11, 14, 15, 17-24, 30-33
1. Not at all 2. Slightly 3. Moderately 4. Quite a bit 5. A great deal
Table 2. Examination and Vitals documented at BaselineDuring admission
P/A – On examination. Bloated
On percussion – Resonance heard over the quadrants of abdomen
Tenderness - + Lower quadrant of abdomen
Warmthness - +
During admission
Appetite -- Increased
Bowel – Loose with blood
Micturition – Normal
Temperature – Normal
Tongue – Mild coated
Sleep – Disturbed
Pulse – 62/min
Weight – 31.4 kgs
Blood pressure – 106/70 mmhg
At Baseline MAYO score was done, indicated the disease activity was severe.
Image 1. MAYO Score done at baseline attached below
Image 2. Blood parameters at baseline: May 2021 attached below
Diagnosis: In this patient, clinical evaluation and imaging was the main diagnostic criterion.
Image 3. Distal colonoscopy (2014) and Ileocolonoscopy (2015) attached below
Prognosis: Though the disease is not life-threatening, getting medical help is the most important aspect in the management of this condition. If left untreated, there is always a risk of getting colon cancer. The episodes may or may not be severe, but the right diet and lifestyle is very important. There is no cure for the condition, practically the patient must live with the condition. There can be complications like bleeding, dehydration, nutritional loss, inflammation of the inner organs and even a perforated bowel. Addressing the clinical condition is very important.
In this patient, the onset is chronic. Despite the long history of the complaints, and being non-responsive to conventional medicines, she could get relief with Ayurvedic Outpatient and Inpatient interventions.
Treatments given: The target of treatment in Ulcerative colitis are threefold—improve quality of life, achieve steroid-free remission, and minimize the risk of cancer. The choice of treatment depends on extent of being affected, severity and the course of the disease. This patient had been taking cool gut 800mg for 5 years, but the outcome was not satisfactory.
Image 1. MAYO Score done at baseline. April 2021

Image 2. Blood parameters at baseline: May 2021

Image 3. Distal colonoscopy (2014) and Ileocolonoscopy (2015)

-
Ayurveda Diagnosis
AYURVEDIC DIAGNOSIS: Pittaja Grahani
About the Disease:
The uniqueness of the term ‘Grahani’ is that it implies to both the organ and the disease.
About Grahani:
अन्नस्य ग्रहणाद् ग्रहणी …
This organ is called as ‘Grahaṇi’ because it withholds the consumed food.
स्थिथा पक्वाशयद्वारि…..
Acarya mentions that the organ is located at the opening of the large intestine.
ग्रहण्या बलमग्निर्हि स चापि ग्रहणीबलः….
The functions of grahaṇi are withholding the food, stimulating the Agni, and proper movement of the food.
दुष्टा ग्रहणी रोगकारिणी…
When the organ grahani becomes weak, then it becomes a causative factor for all diseases.
दूषिते ∫ ग्नावतो …..
Grahani and Agni share a very deep mutual connection. They are mutually dependent on each other. Hence when Agni is vitiated, grahani also gets vitiated. Similarly, when grahani is vitiated Agni also gets vitiated. As these are two prominent factors in maintaining health, when one gets affected, it causes a pathology.
Cardinal symptoms of Grahani:
अतिसृष्टम् विबद्धं वा द्रवं तदुपदिश्यते । (Ca.Ci.15.53)
The stools can be either be hard causing difficulty in defecation or it can be watery.
In this patient, the Agni was also affected, it was atyagni. This was attributed to the increased tikshnamsha of pitta. The bowels were frequent watery stools, sometimes with blood. As all symptoms attribute to the aggravation of pitta, it was diagnosed as Pittaja Grahaṇi.
Treatment:
स्नेहमेव परं विद्याद्दुर्बलानलदीपनं ।
नालं स्नेहसमिद्धस्य शमायान्नं सुगुर्वपि ॥ ६८॥
The snehaprayoga is considered the best treatment option in the case of deranged Agni. Sneha can be administered in small doses taking into consideration the rogabala and the rogibala. Then supportive internal medications and external applications can also be done.
Treatment rationale of the physician:
In this patient, the treatment target was to correct the atipravṛtti of vayu, reduce the tikshnamsha of pitta and normalize the mandatva of kapha. At the same time the medicines and external applications had to be amaharam, normalizing the agni, and addressing the symptom of watery stools. So puriṣa sthapaka treatments were also given. The symptoms persisted since many years and was not responding to the conventional medicines.
Prognosis: It is a yapya vyadhi. Grahani is a cronic disease, that requires careful intervention. Diet equally plays an important role.
-
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Kanakasara kashayam + Patadi gulika Kasayam, Gulika 7.5 ml Kasayam, 1 gulika Mix the Kasayam with 30 ml of warm water and powdered gulika and 1 tsp honey, at 10 am and 3 pm 2021-04-30 - 2021-05-12 Kanakasaram- Anubhuta Yoga; Pathadi gulika- Proprietary Medicine Kanakasara kashayam + Vilwadi gulika Kasayam, Gulika 7.5 ml Kasayam, 1 gulika Mix the Kasayam with 30 ml of warm water and powdered gulika and 1 tsp honey, at 10 am and 3 pm 2021-04-30 - 2021-05-04 Vilwadi gulika- AH.Utt.36.84-85 Kanakasara kashayam + Vilwadi gulika Kasayam, Gulika 7.5 ml Kasayam, 1 gulika Mix the Kasayam with 30 ml of warm water and powdered gulika and 1 tsp honey, at 10 am and 3 pm 2021-05-12 - 2021-06-13 Yavanyadi Curnam Curnam 1 tsp Mix with 1 tsp honey, and taken before lunch and dinner 2021-05-05 - 2021-06-13 Sahasra yogam. Curna Prakaranam Hribeeradi Kashayam + Spl. Nagaradi Kashayam + Dadimashtaka Curnam Kasayam, Curnam 5 ml of Kasayam, 1/2 tsp curnam Mixed with 1 tsp of honey, and 20 ml of warm water at 10 am and 3 pm 2021-05-05 - 2021-06-13 Hriberadi – Sahasra yogam. Parishishta Prakaranam; Spl Nagaradi – Anubhuta Yoga; Dadimashtaka curnam- Sahasra yogam. Curna Prakararanam Aja Ksiram Panam 1 glass Oral, at bedtime 2021-05-12 - 2021-06-13 Anubhuta Yogam Laksha swarasam + Panamkalkandam Panam 25 ml svarasam, 1 tsp Panamkalkandam Mixed with 1 tsp of honey, taken now and then 2021-05-05 - 2021-06-13 Anubhuta Yogam Kanakasara kashayam + Vilwadi gulika Kasayam, Gulika 7.5 ml Kasayam, 1 gulika Mixed with 30 ml of warm and 1 tsp of honey, on empty stomach at 6 am and 6 pm 2021-06-14 - 2021-08-14 Hribeeradi kashayam + Spl. Nagaradi kashayam + Dadimashtaka Curnam Kasayam, Curnam 5 ml Kasayam, 1/2 tsp curnam Mixed with 1 tsp of honey, and 20 ml of warm water at 10 am and 3 pm 2021-06-14 - 2021-08-14 Yavanyadi Curnam Curnam 1 tsp Mixed with 1 tsp honey, taken before lunch and dinner 2021-06-14 - 2021-08-14 Ashoka Ghrtam Ghrtam 1 tsp Mixed with 25 ml of water at bedtime 2021-06-14 - 2021-08-14 Bhaishajya Ratnavali.Striroga Adhikara.17-20 -
Outcome Measures
OUTCOME MEASURES
In this 31-year-old female patient, the complaints of frequent watery stools started 6 and half years back, which was initially considered to be food poisoning (2014). That specific episode was treated with conventional medicine and cured. But since then, she has been suffering from these complaints on & off. Based on the colonoscopy report, a provisional diagnosis was made as Ulcerative colitis. Despite taking conventional medicines for more than 5 years, she got no relief. She was losing weight and was only 31kgs at baseline, when she came for ayurvedic consultation.
After Ayurvedic interventions, subjective and objective assessments were done to measure the outcome.
Subjective parameters:
A physical examination was done before and after treatment and this revealed significant improvement.
Table 1. Physical examination, vitals recorded before and after treatment
During admission
During discharge
Appetite -- Increased
Appetite -- Normal
Bowel – Loose with blood
Bowel – Semisolid consistency, Once with no bleeding
Micturition – Normal
Micturition – Normal
Temperature – Normal
Temperature – Normal
Tongue – Mild coated
Tongue – Mild coated
Sleep – Disturbed
Sleep – Improved
Pulse – 62/min
Pulse – 66/min
Weight – 31.4 kgs
Weight – 31.8 kgs
Blood pressure – 106/70 mmhg
Blood pressure – 108/70 mmhg
During admission
During discharge
P/A – On examination
Bloated
P/A – On examination
Mild Bloatedness present
On percussion – Resonance heard over the quadrants of abdomen
On percussion – Mild Resonance heard over the quadrants of abdomen
Tenderness - + Lower quadrant of abdomen
Tenderness - Nil
Warmth - +
Warmth – Localised
Objective parameters:
Blood parameters were checked before and after treatment.
Image 1. Blood parameters before and after treatment attached below
Table 2. Blood parameters before and after treatment
On 04/05/2021 (At baseline)
On 11/06/2021 (Before discharge)
Hb – 9.6
Hb – 10.8
Platelets count – 2.1 Lakhs/cumm
Platelets count – 2.6 Lakhs/cumm
ESR – 65
ESR – 48 mm/hr
C R P – 1.41 mg/L
C R P – 0.50 mg/L
PARTIAL MAYO SCORING INDEX was used for assessing the disease activity.
At the baseline, the score was 8 indicating ‘severe’ disease activity. At the endpoint, the score was 3 indicating a ‘mild’ disease activity.
Image 2. MAYO SCORING INDEX done post Ayurvedic treatment attached below
IBD - Quality of life assessment questionnaire was also filled up at the endpoint to assess the severity of the disease. At baseline, the score was 163. At the endpoint, it was 133 indicating the disease activity has reduced.
Table 3. IBD QOL Questionnaire filled pre and post Ayurvedic treatment attached below
IBD QOL Questionnaire
QUESTIONNARE
SCORE (DURING ADMISSION) 30.4.21
SCORE (DURING DISCHARGE) 14.6.21
I feel helpless because of my bowel problems
5
3
I am embarrassed by the smell caused by my bowel problems
5
2
I am bothered by how much time I spend on the toilet.
5
3
I feel vulnerable to other illnesses because of my bowel problems
5
5
I feel fat because of my bowel problems.
1
1
I feel like I'm losing control of my life because of my bowel problems
5
3
I feel my life is less enjoyable because of my bowel problems
5
3
I feel uncomfortable when I talk about my bowel problems
3
3
I feel depressed about my bowel problems
5
5
I feel isolated from others because of my bowel problems
5
5
I have to watch the amount of food I eat because of my bowel problems
5
5
Because of my bowel problems, sexual activity is difficult for me
5
5
I feel angry that I have bowel problems
5
5
I feel like I irritate others because of my bowel problems
5
5
I worry that my bowel problems will get worse
5
5
I feel irritable because of my bowel problems
5
5
I worry that people think I exaggerate my bowel problems
5
3
I feel I get less done because of my bowel problems
5
5
I have to avoid stressful situations because of my bowel problems
5
5
My bowel problems reduce my sexual desire
5
4
My bowel problems limit what I can wear
5
5
I have to avoid strenuous activity because of my bowel problems
5
5
I have to watch the kind of food I eat because of my bowel problems
5
5
Because of my bowel problems, I have difficulty being around people I do not know well
4
2
I feel sluggish because of my bowel problems
5
2
I feel unclean because of my bowel problems
5
2
Long trips are difficult for me because of my bowel problems
5
3
I feel frustrated that I cannot eat when I want because of my bowel problems
5
5
It is important to be near a toilet because of my bowel problems
5
2
My life revolves around my bowel problems
5
5
I worry about losing control of my bowels
5
5
I fear that I won't be able to have a bowel movement
5
2
My bowel problems are affecting my closest relationships
5
5
I feel that no one understands my bowel problems
5
5
TOTAL SCORE
163
133
The IBS-QOL consists of 34 items, each with a five-point response scale:
Items 1, 2, 4, 8-10, 12, 13, 16, 25-29, 34
1. Not at all 2. Slightly 3. Moderately 4. Quite a bit 5. Extremely
Items 3, 5-7, 11, 14, 15, 17-24, 30-33
1. Not at all 2. Slightly 3. Moderately 4. Quite a bit 5. A great deal
Disease modifying effect: The patient is free from her symptoms. The stools are passed only once or twice a day. There is no blood in the stools. Her weight is stable, and her disease score has reduced indicating a significant improvement.
Image 1. Blood parameters before and after treatment June 2021

Image 2. MAYO SCORING INDEX done post Ayurvedic treatment June 2021

-

