Featured Case
-
Abstract
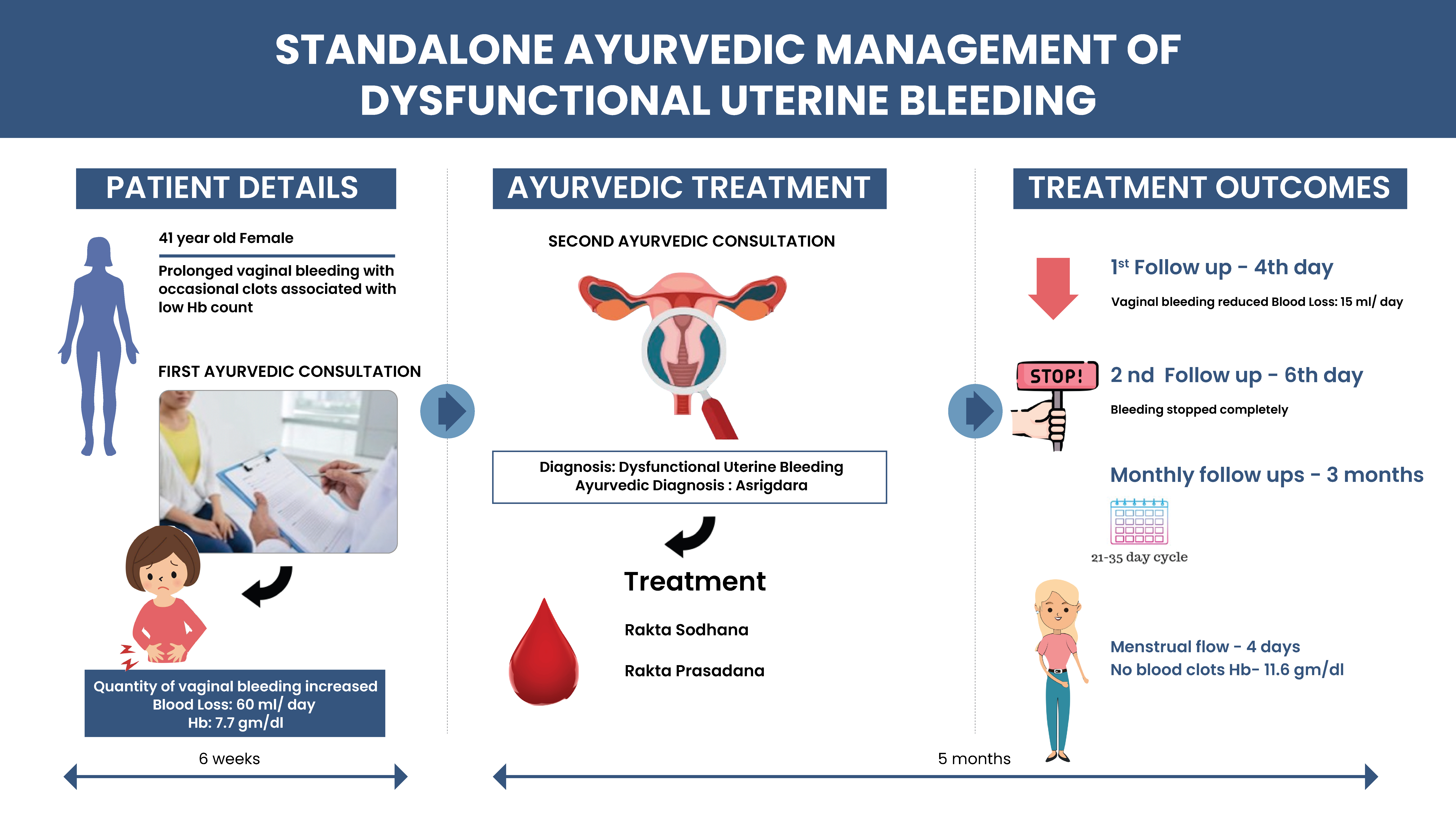
A 41-year-old female patient, a teacher by profession, presented with prolonged vaginal bleeding with occasional clots for two months associated with low Hemoglobin count and having a feeling of generalized body swelling. She had taken Ayurvedic medications for two months, the details of which she is unable to remember now. The patient did not respond well to the treatments, and the condition was found to be progressing. This time, she consulted Dr. Prajeesh Nath. Her blood loss was 60ml/day, which could be measured as she was using a menstrual cup, and in the blood routine examination, the Haemoglobin level was 8gm/dl. Dr Prajeesh Nath provisionally diagnosed the condition as Dysfunctional Uterine Bleeding and treated the condition as Asrigdara. Rakta shodhana and rakta prasadana were the line of treatments administered. After four days of Ayurvedic treatment, the blood loss reduced to 15ml/day, and after six days, the bleeding completely stopped. In the monthly follow-ups done for the next three months, the patient had a healthy menstrual cycle with menstrual flow lasting for four days with no blood clots. Hemoglobin checked after four months of treatment was 11.6gm/dl.
This case report highlights the need to explore the scope of Ayurveda as an alternative treatment approach to the management of dysfunctional uterine bleeding.
-
Summaries
-
Listen
-
Watch
-
View
-
Read
Standalone Ayurvedic management of Dysfunctional Uterine Bleeding
A 41-year-old female patient, a teacher by profession, presented with prolonged vaginal bleeding with occasional clots for two months associated with low Hemoglobin count and having a feeling of generalized body swelling. She had taken Ayurvedic medications for two months, the details of which she is unable to remember now. The patient did not respond well to the treatments, and the condition was found to be progressing. This time, she consulted Dr. Prajeesh Nath. Her blood loss was 60ml/day, which could be measured as she was using a menstrual cup, and in the blood routine examination, the Haemoglobin level was 8gm/dl. Dr Prajeesh Nath provisionally diagnosed the condition as Dysfunctional Uterine Bleeding and treated the condition as Asrigdara. Rakta shodhana and rakta prasadana were the line of treatments administered. After four days of Ayurvedic treatment, the blood loss reduced to 15ml/day, and after six days, the bleeding completely stopped. In the monthly follow-ups done for the next three months, the patient had a healthy menstrual cycle with menstrual flow lasting for four days with no blood clots. Hemoglobin checked after four months of treatment was 11.6gm/dl.
This case report highlights the need to explore the scope of Ayurveda as an alternative treatment approach to the management of dysfunctional uterine bleeding.
-
-
Timeline
-
Tabulated Summary
-
Narrative
TITLE OF CASE:
Standalone Ayurvedic management of Dysfunctional Uterine Bleeding - A case report
Dr Prajeesh Nath
ABSTRACT
A 41-year-old female patient, a teacher by profession, presented with prolonged vaginal bleeding with occasional clots for two months associated with low Hemoglobin count and having a feeling of generalized body swelling. She had taken some unknown Ayurvedic medications for two months. The patient did not respond well to the treatments, and the condition was found to be progressing. She opted for a second Ayurvedic consultation. Her blood loss was 60 ml/day, which could be measured as she was using a menstrual cup, and in the blood routine examination, the Hemoglobin level was 8gm/dl. The condition was provisionally diagnosed as Dysfunctional Uterine Bleeding and treated the condition as Asrgdara. Rakta shodhana and rakta prasadana were the line of treatments administered. After four days of Ayurvedic treatment, the blood loss reduced to 15ml/day, and after six days, the bleeding completely stopped. In the monthly follow-ups done for the next three months, the patient had a healthy menstrual cycle with menstrual flow lasting for four days with no blood clots. Hemoglobin checked after four months of treatment was 11.6gm/dl. So, Ayurveda can be adopted as an alternate way of managing complex dysfunctional uterine bleeding.
KEYWORDS
Dysfunctional uterine bleeding, Asrgdara, Case report, Ayurveda, Standalone
INTRODUCTION
Dysfunctional uterine bleeding or Abnormal uterine bleeding is a broad term that describes irregularities in the menstrual cycle involving frequency, regularity, duration, and volume of flow outside of pregnancy. Up to one-third of women will experience abnormal uterine bleeding in their life, with irregularities most commonly occurring at menarche and perimenopause. A normal menstrual cycle has a frequency of 24 to 38 days and lasts 2 to 7, with 5 to 80 milliliters of blood loss. Variations in any of these 4 parameters constitute abnormal uterine bleeding.
PATIENT INFORMATION
41year old female patient, a teacher by profession, complained of prolonged vaginal bleeding with occasional clots since 2 months associated with low Hb and a feeling of having a generalized body swelling.
Medical history: The onset of symptoms started about 2 months ago. The patient had missed periods on February 2021, and on 12th March, bleeding started, which was very scanty. Later from 18th March 2021, she experienced heavy bleeding with occasional clots. The patient did not have any other co-morbidities or any previous history of menstrual irregularity apart from a simple ovarian cyst in the right ovary. The quantity of vaginal bleeding was increasing day by day. The blood loss at the time of consultation was approximately 60 ml/day. The patient was not willing to take up the modern line of management. She previously consulted an Ayurvedic doctor, who advised her some oral medications, the details she doesn't remember. She took them for a short while but did not get much relief. So, she approached for a second Ayurvedic consultation.
CLINICAL FINDINGS
- Not done as the patient had consulted online. Body weight recorded by the patient - 74kg
TIMELINE
Image 1. Attached
DIAGNOSTIC ASSESSMENT
Modern Diagnosis: Based on the presenting symptoms and medical history, the condition was diagnosed as Dysfunctional Uterine Bleeding.
Image 2. Blood investigation report before treatment
Ayurvedic diagnosis: Asrigdara was the diagnosis confirmed by the physician
Differential diagnosis: The differential diagnosis for genital tract bleeding based on anatomic location or system:
• Vulva: Benign growths or malignancy
• Vagina: Benign growths, sexually transmitted infections, vaginitis, malignancy, trauma, foreign bodies
• Cervix: Benign growths, sexually transmitted infections, malignancy
• Fallopian tubes and ovaries: Pelvic inflammatory disease, malignancy.
These were ruled out by the physician, based on the clinical examination and the investigations done.
Prognosis: In the conventional line of management, non-steroidal anti-inflammatory drugs (NSAIDs) or ant prostaglandins are used but with side effects like headaches, and gastrointestinal symptoms such as nausea, vomiting, diarrhoea and dyspepsia. In this case, the patient opted for Ayurvedic treatment. With standalone Ayurvedic treatment, prolonged vaginal bleeding for 2 months, completely stopped with 6 days of treatment and the Hb level has almost reached the normal range after 5 months of treatment.
THERAPEUTIC INTERVENTION
See Tab ‘Treatment Details’
FOLLOW-UP AND OUTCOMES
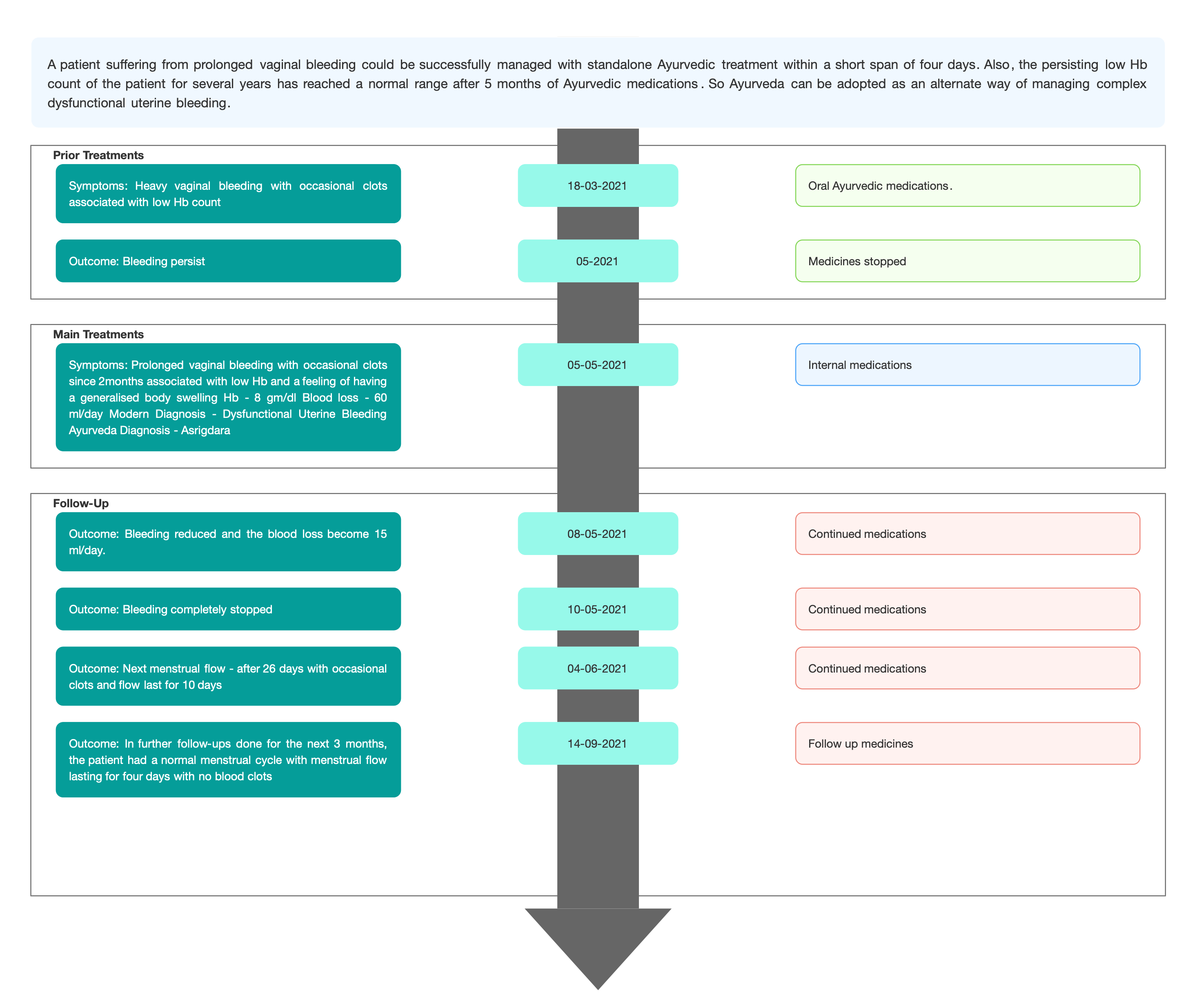
First follow-up (8/5/21)- Bleeding reduced and the blood loss become 15 ml/day.
Second 10/5/21- Bleeding completely stopped
4/6/2021- Next menstrual flow - after 26 days with occasional clots and flow last for 10days
In further follow ups done for next 3 months, the patient had normal menstrual cycle with menstrual flow lasting for four days with no blood clots
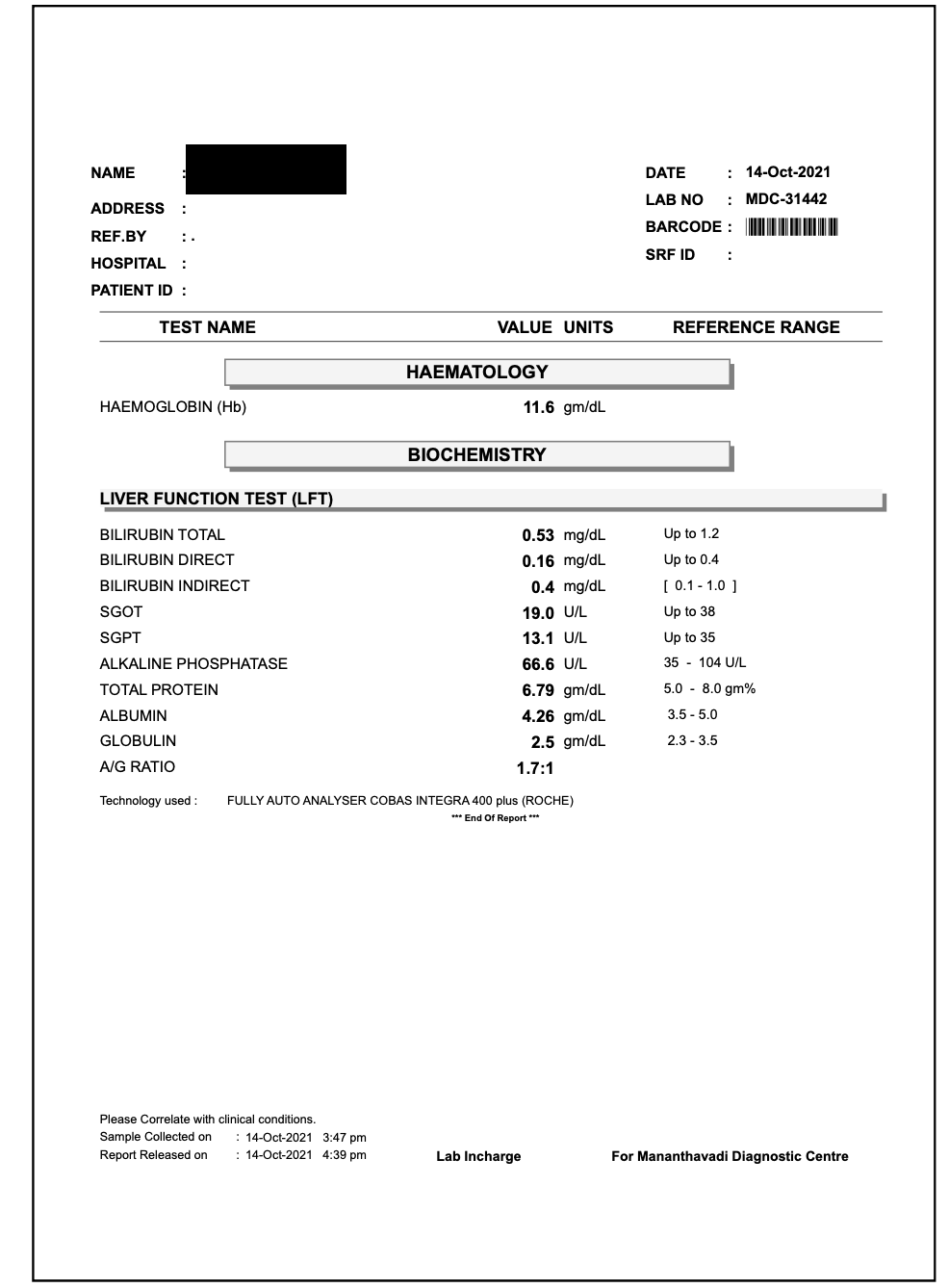
14/10/21- Hb - 11.6 gm/dl
Clinician-based assessment: The patient had prolonged vaginal bleeding for 2 months soaking 7-8 pads / 4 cups per day (blood loss - 60 ml/day) associated with low Hb count. 4 days after the initiation of treatment the bleeding reduced, and the blood loss become 15 ml/day. After 6 days of treatment, the bleeding completely stopped. Hb count before the treatment was 8gm/dl which has become 11.6gm/dl after 4 months of treatment.
Image 3. Blood investigation report after treatment
Body weight recorded by the patient before treatment- 74kg, which becomes 68kg after treatment.
Patient assessed: Not relevant
Intervention adherence and tolerability: The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment- By monitoring the patient.
Adverse and unanticipated events: None reported
DISCUSSION
Excessive flow and prolonged duration of menses during menstrual cycle or inter-menstrual bleeding known as Asrigdara. Acharya Charaka has described four types of Asrigdara i.e., Vataja, Pittaja, Kaphaja and Sannipataja Asrigdara. Acharya Sushruta has mentioned all types of Asrigdara along with general clinical features of Asrigdara but has not described any classification. Different types of Samprapti, Dosanubandha and Anubandhita Lakshana are seen in every patient of Asrgdara. So, the treatment depends based on doshanubandha and Samprapti Vighatana. In this case, the clinician treated the condition as Asrigdara and followed rakta prasadana and rakta sodhana line of management. Guluchyadi Kashayam was advised for Rakta prasadana and Rakta Sthambana . Punarnavadi was given, focussing on sarvanga sopha with Pandu and also as Rakta prasadana. Avipathi Churnam was advised for samana and sodhana of Pitta. Chandraprabha Vati was given to reduce the Sarvanga Sopha. It also acts as Granthi vilayana, vatanaulomana, and srotosodhana. Lodhradi kashayami is Yoni dosha hara. Drakshadi has Brihmana, Rakta prasadana
PATIENT’S PERSPECTIVE:
Not available
LEARNING POINTS:
A case of prolonged vaginal bleeding could be successfully managed with standalone Ayurvedic treatment within few days. Also, the persisting low Hb count of the patient for several years has reached to normal range after 5 months of Ayurvedic medications. So, Ayurveda can be opted as an alternative treatment dysfunctional uterine bleeding.
INFORMED CONSENT
Written consent was obtained from the patient.
ACKNOWLEDGEMENTS
None
CONFLICT OF INTEREST
None declared
FUNDING
None
REFERENCE
- Davis E, Sparzak PB. Abnormal Uterine Bleeding. [Updated 2022 Sep 9]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK532913/
- Acharya Priyavrat Sharma(ed), Sushruta Samhita with Dalhana virachita Nibandha Sangraha vyakhya, published by Chaukhamba samskrita Samsthana, Varanasi, 8th edition 2005, Sharira Sthana 2/18
Image 1. Timeline
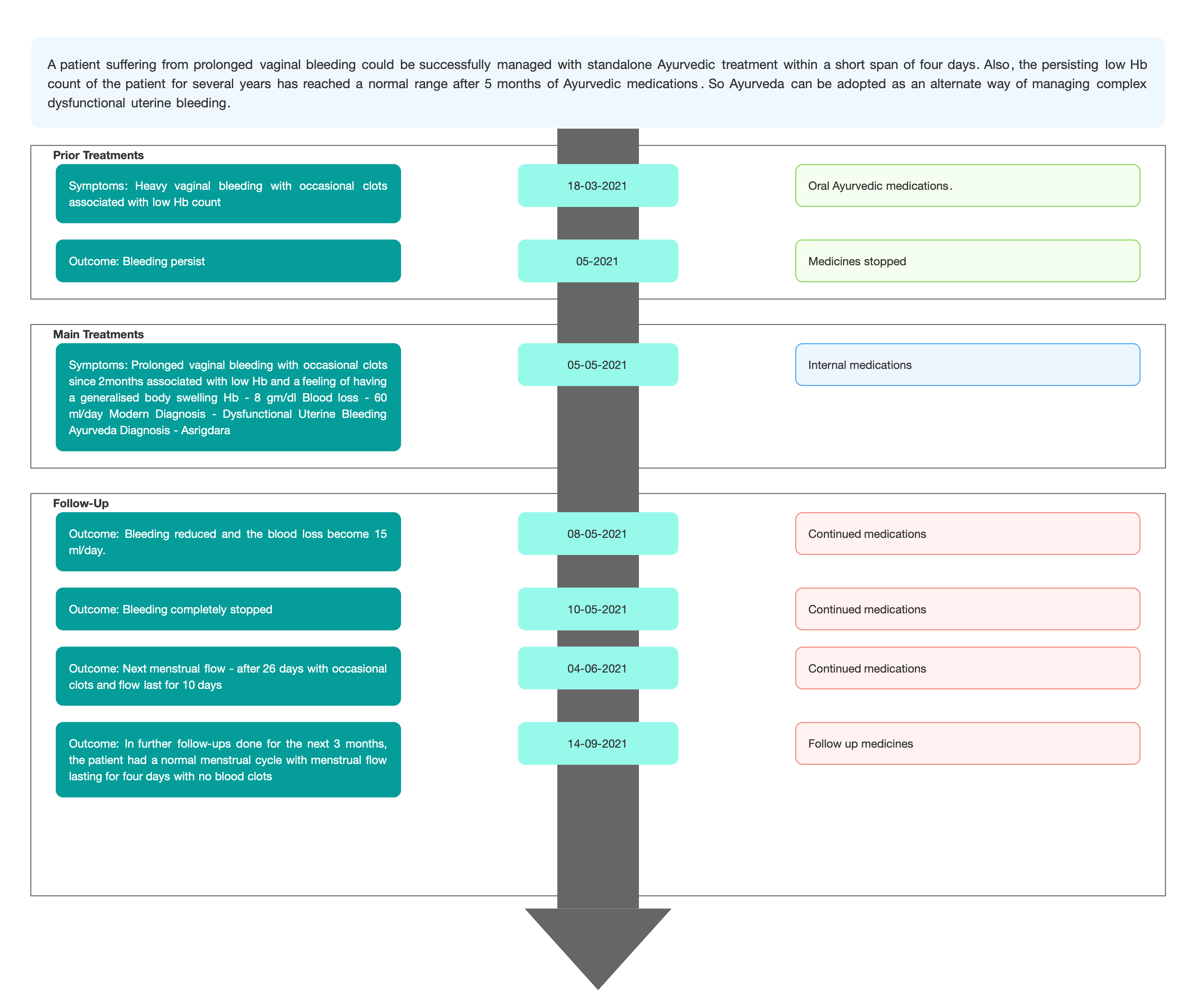
Image 2. Blood investigation report before treatment
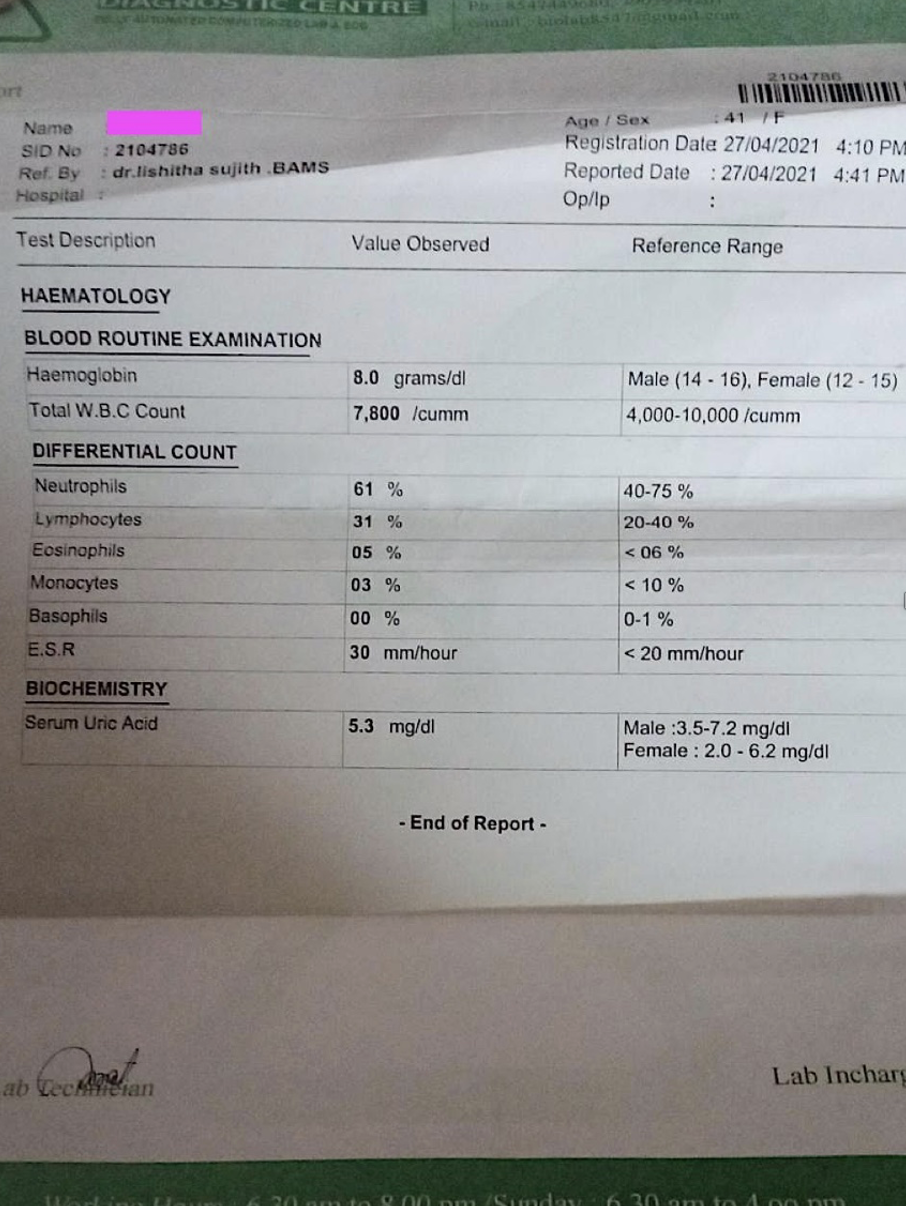
Image 3. Blood investigation reports after treatment

-
Immersive Learning
-
Modern Diagnosis
Modern diagnosis:
Dysfunctional uterine bleeding (DUB)
About the disease:
Dysfunctional uterine bleeding (DUB) is defined as excessively heavy, prolonged or frequent bleeding of uterine origin that is not due to pregnancy or any recognizable pelvic or systemic disease.
Signs and symptoms of DUB:
Unusual increase in blood loss
More than 7 days of bleeding
Bleeding not contained within pads or tampons (particularly if wearing the largest size)
Clots greater than 3 cm, and
Presence of signs of anaemia or iron deficiency on blood testing.
Diagnostic Criteria:
• Routine Pap test
• Full blood examination - if anemia is suspected /serum ferritin to detect iron deficiency
• Coagulation screen or platelet function tests – if a coagulopathy is suspected
• Thyroid function tests, renal investigations, or auto-antibodies such as lupus coagulant - if the organic disease is suspected.
• Transvaginal ultrasound- for excluding pelvic causes. Hysteroscopy with dilation and curettage or endometrial biopsy, or laparoscopy if there is associated pain
Treatment:
In the conventional line of management, non-steroidal anti-inflammatory drugs (NSAIDs) or antiprostaglandins are used but with side effects like headaches, and gastrointestinal symptoms such as nausea, vomiting, diarrhoea and dyspepsia appear. If other treatments are proven to be ineffective, in such cases hysterectomy is suggested. Hysterectomy can lead to amenorrhea but does have a significant morbidity rate.
Diagnosis of this case:
In this case report, blood investigation showed, the patient had a low Hb count. Old reports confirmed the persistent low hemoglobin level. Based on the presenting symptoms and laboratory findings, the clinician diagnosed the condition as Dysfunctional Uterine Bleeding.
Image 1. Blood Investigation reports before treatment
Prognosis
The prognosis is favourable but also depends on the aetiology. The main goal of evaluating and treating chronic Abnormal Uterine Bleeding is to rule out serious conditions such as malignancy and improve the patient's quality of life, keeping in mind current and future fertility goals and other comorbid medical conditions that may impact treatment or symptoms. Prognosis also differs based on conservative medical versus surgical treatment. With standalone Ayurvedic treatment, prolonged vaginal bleeding for 2 months, completely stopped within 4 days of treatment and Hb level has almost reached the normal range after 5 months of treatment
Image 1.
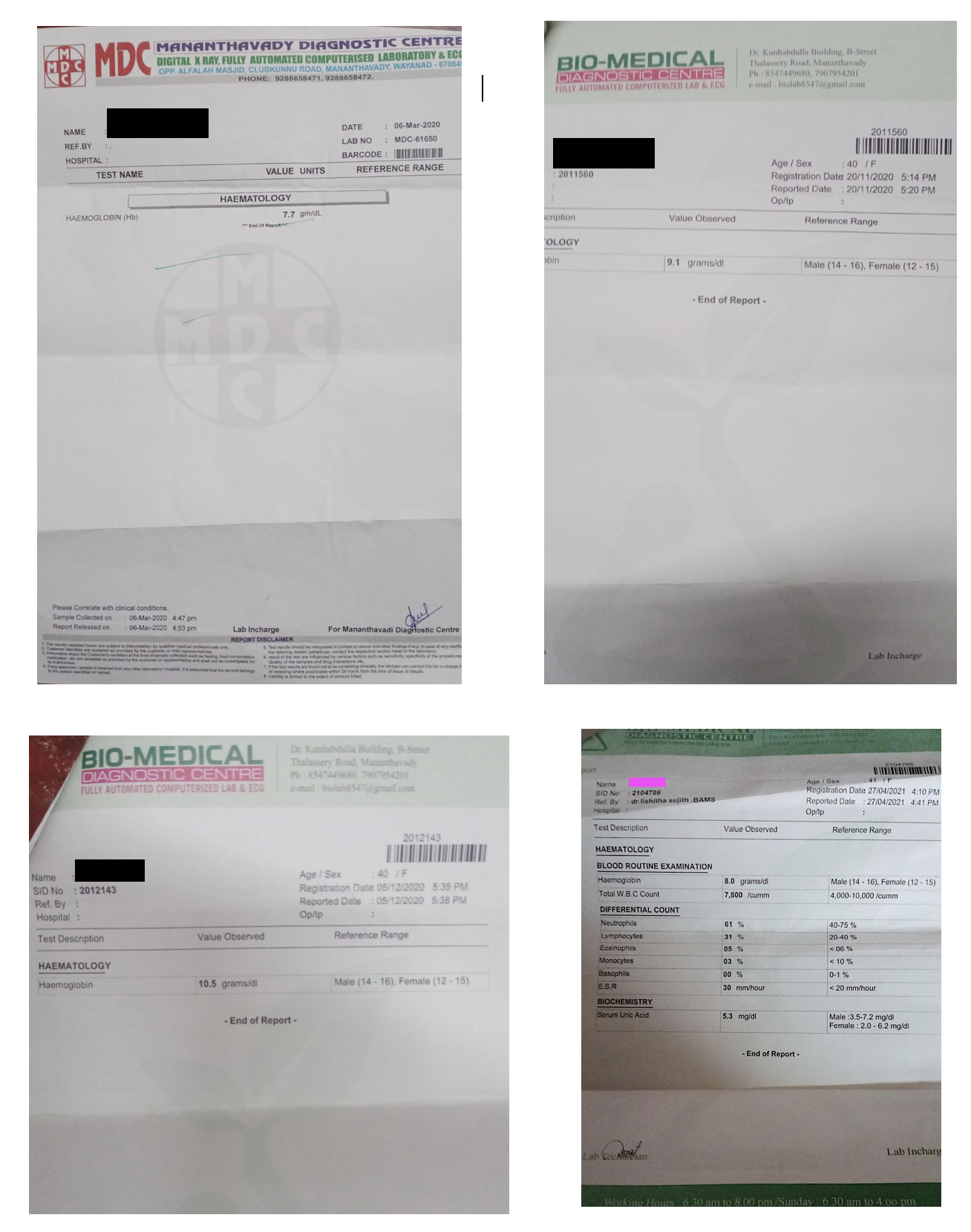

-
Ayurveda Diagnosis
Ayurveda Diagnosis: Asrigdara
तदेवातिप्रसग़्गेन प्रव्ऱ्त्तमन्ऱ्तावपि॥१८॥
अस्ऱ्ग्दरं विजानीयादतोऽअन्यद्रक्तलक्षणात्॥(Su.sa 2/18)
Excessive flow and prolonged duration of menses during menstrual cycle or inter-menstrual bleeding known as Asrigdara
Pathogenesis
According to AcharyaCharaka, aggravated Vata affects uterine vessels and boosts amount of blood and this increase in blood volume thus causes increase in menstrual blood and creates Rakta-pradara.
Classification
Acharya Charaka has described four types of Asrigdara i.e., Vataja, Pittaja, Kaphaja and Sannipataja Asrigdara. Acharya Sushruta has mentioned all types of Asrigdara along with general clinical features of Asrigdara but has not described any classification. Mostly Acharyas have mentioned four types of Asrigdara.
Chikitsa
Different types of Samprapti, Dosanubandha and Anubandhita Lakshana are seen in every patient of Asrgdara. So, the treatment depends based on doshanubandha and Samprapti Vighatana.
Management- Raktasthambhaka, Raktasthapaka, Dipana, Pachana, Bruhaniya ,Balya Chikitsa using Madhur Tikta Kashaya rasa pradhana dravyas
Ayurvedic diagnosis of the case:
41yr old female patient complaints of prolonged vaginal bleeding with occasional clots for 2months associated with low Hb count. The condition started about 2months before consultation as prolonged vaginal bleeding with a blood loss of 60ml/day. The patient was unwilling to go for any modern line of management and opted for Ayurvedic treatment. Laboratory investigation revealed low Hb count. The clinician diagnosed the case as Dysfunctional uterine Bleeding. Based on the patient symptoms and medical history, the clinician correlated the condition as Asrigdara in Ayurveda.
Treatment rationale:
The clinician followed rakta prasadana and rakta sodhana line of management.
Guluchyadi Kashayam -given for Rakta prasadana and Rakta Sthambana
Punarnavadi - given focussing on sarvanga sopha with Pandu and also as Rakta prasadana
Avipathi Churnam was advised for samana and sodhana of Pitta.
Chandraprabha Vati- For Sarvanga Sopha and Granthi vilayana, also as vatanaulomana, and srotosodhana
Lodhradi kashayam - Yoni dosha hara & for granthi
Drakshadi - Brihmana, Rakta prasadana and is indicated in Pandu
Tapyadi - To increase Hb count (Pandu)
Sukumara Kashayam & ghritam has lekhana guna that can be helpful in effective management of simple ovarian cyst. -
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Guluchyadi + Punarnavadi kashayam Kashaya 15 ml twice daily Oral, with 45ml boiled and cooled water 1and 1/2 hr before food 2021-05-05 - 2021-06-24 Ashtanga Hrudaya Sahasra Yogam Avipathi choornam Choornam 1 tsp Oral, with 1 glass hot water 2021-05-05 - 2021-06-24 Sahasra yoga -Choorna yoga prakarana Chandraprabha tab Tablet 2-0-2 Oral, with kashayam 2021-05-05 - 2021-07-22 Bhaishajyaratnavali-Prameha Lodhradi Kashaya 15ml, Oral, 2021-06-25 - 2021-07-22 Ashtangahrudayam Tab. Tapyadi loham Tablet 1-0-0 Oral, after breakfast 2021-06-25 - 2021-07-27 Ayurveda sara sangraha Sukumaram ghritam Ghritam 1tsp-0-1tsp 7am-0-6pm Oral, after melting add 1pinch of salt 2021-06-25 - 2021-07-27 Ashtangahrudayam Musalikhadiradi kashayam Kashaya 15ml, twice daily Oral, with 45ml boiled and cooled water 1and 1/2 hr before food 2021-07-23 - 2021-08-01 Sahasrayogam Kashayaprakaranam Chandraprabha tab Tablet 1-0-1 Oral 2021-08-02 - 2021-09-14 Bhaishajyaratnavali-Prameha Lodhradi kashayam + Drakshadi kashayam Kashaya 15ml, twice daily 7am-0-6pm Oral, with with 45ml boiled and cooled water 2021-08-02 - 2021-09-14 Ashtangahrudayam Tab. Tapyadi loham Tablet 1-0-0 Oral, after breakfast 2021-08-02 - 2021-08-29 Ayurveda sara sangraha Sukumaram ghritam Ghritam 0-0-1tsp Oral, after melting add 1pinch of salt 2021-08-02 - 2022-02-16 Ashtangahrudayam Sukumaram Kashayam Kashaya 15ml, twice daily Oral, with 45ml boiled and cooled water 1and 1/2 hr before food 2021-09-14 - 2022-02-16 Sahasra yoga -
Outcome Measures
OUTCOME MEASURES
A 41-year-old female patient complained of prolonged vaginal bleeding with occasional clots for 2 months associated with low Hb count. Ayurveda was the first choice of treatment for the patient. She had prolonged vaginal bleeding with a blood loss of 60 ml/day. Laboratory investigation revealed a low Hb count. Based on the presenting complaint and persisting low Hb count, the condition was clinically diagnosed as Dysfunctional Uterine Bleeding. The outcome was assessed based on the daily blood loss and the Haemoglobin count.The patient had prolonged vaginal bleeding since 2 months soaking 7-8 pads / 4 cups per day (blood loss - 60 ml/day) associated with low Hb count. 4 days after treatment initiation, the bleeding reduced and the blood loss became 15 ml/day. After 6 days of treatment, the bleeding completely stopped. The Hb count before the treatment on 27/4/21 was 8 gm/ dl, which became 11.6 gm /dl after the treatment.
Body weight recorded by the patient before treatment- 74 kg, which becomes 68 kg after 4 months.
Image 1. Blood investigation report after treatment

-

