Featured Case
-
Abstract
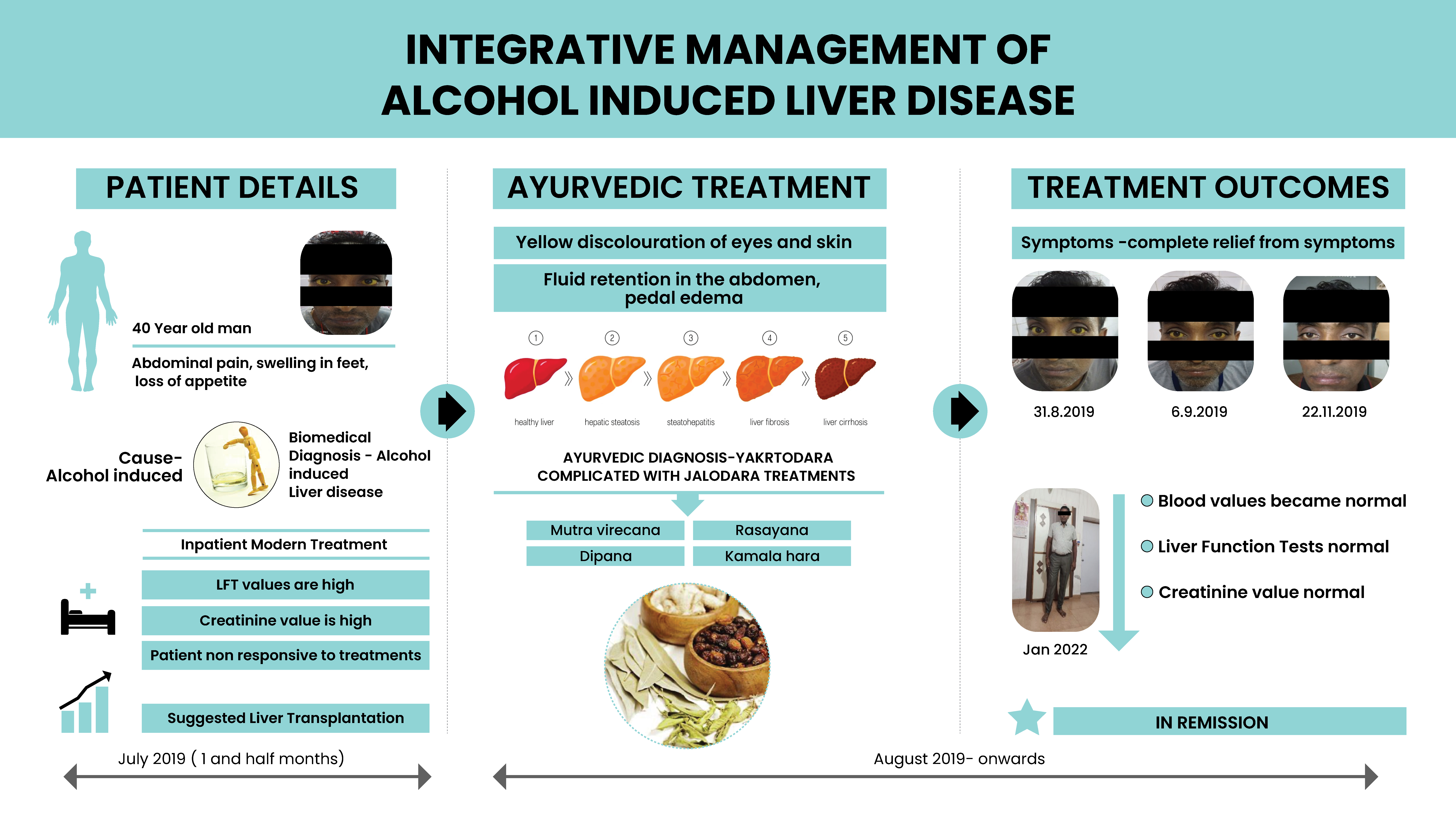
A 40-year-old male patient was diagnosed with alcohol-induced chronic liver disease. The biomedical diagnosis was based on the clinical presentation, Endoscopy, and blood investigations like Liver Function Tests and Kidney Function Tests. He was on conventional medicines since for one and a half months. The Liver Function tests revealed very high values of Bilirubin (Total, Direct and Indirect) and SGOT). The creatinine value was also elevated. The patient did not respond to the standard of care for protecting the Liver and was worsening clinically. Due to elevated blood parameters and aggravating symptoms, he was advised Liver transplantation, but the patient refused the treatment. He opted for Ayurveda and approached Dr S N Gupta. The presenting complaints were abdominal pain, loss of appetite, generalized weakness, itching, and swelling over the legs. On clinical examination, he had icterus, yellow discoloration of skin, mild distension of the abdomen and pedal edema. This condition was diagnosed as Yakrtodara with jalodara as a complication. The ayurvedic treatment target was Tridosha shamana, mutra virecana, yakrit samrakshana, dipana, pacana and rasayana. The patient was hospitalised and underwent treatment for two months. Most of his symptoms were relieved except for mild itching and mild yellow discolouration of sclera. The accumulation of abdominal fluid also reduced, resulting in the reduction of abdominal girth. In the first follow-up, the itching was relieved. In the second follow-up, the yellow discolouration of the sclera was relieved. Follow-up was done every month, and the patient is completely free of symptoms. The liver function tests, and the Creatinine became normal. The patient is now in remission and has been advised to strictly abstain strictly from alcohol, and tobacco. Diet and lifestyle modifications were also strongly recommended.
This case demonstrates that Ayurvedic treatments can successfully manage certain cases of Alcohol induced chronic liver disease with significant improvement in the subjective and objective parameters.
-
Summaries
-
Listen
-
Watch
-
View
-
Read
A 40-year-old male patient was diagnosed with alcohol-induced chronic liver disease. The biomedical diagnosis was based on the clinical presentation, Endoscopy, and blood investigations like Liver Function Tests and Kidney Function Tests. He was on conventional medicines since for one and a half months. The Liver Function tests revealed very high values of Bilirubin (Total, Direct and Indirect) and SGOT). The creatinine value was also elevated. The patient did not respond to the standard of care for protecting the Liver and was worsening clinically. Due to elevated blood parameters and aggravating symptoms, he was advised Liver transplantation, but the patient refused the treatment. He opted for Ayurveda and approached Dr S N Gupta. The presenting complaints were abdominal pain, loss of appetite, generalized weakness, itching, and swelling over the legs. On clinical examination, he had icterus, yellow discoloration of skin, mild distension of the abdomen and pedal edema. This condition was diagnosed as Yakrtodara with jalodara as a complication. The ayurvedic treatment target was Tridosha shamana, mutra virecana, yakrit samrakshana, dipana, pacana and rasayana. The patient was hospitalised and underwent treatment for two months. Most of his symptoms were relieved except for mild itching and mild yellow discolouration of sclera. The accumulation of abdominal fluid also reduced, resulting in the reduction of abdominal girth. In the first follow-up, the itching was relieved. In the second follow-up, the yellow discolouration of the sclera was relieved. Follow-up was done every month, and the patient is completely free of symptoms. The liver function tests, and the Creatinine became normal. The patient is now in remission and has been advised to strictly abstain strictly from alcohol, and tobacco. Diet and lifestyle modifications were also strongly recommended.
This case demonstrates that Ayurvedic treatments can successfully manage certain cases of Alcohol induced chronic liver disease with significant improvement in the subjective and objective parameters.
-
-
Timeline
-
Tabulated Summary
-
Narrative
TITLE OF CASE
Integrative management of Chronic liver disease (alcohol induced) in a male who was non-responsive to conventional medicines and suggested liver transplantation- A Case report
Prof. Dr S N Gupta
ABSTRACT
A 40-year-old male patient who suffered from alcohol-induced chronic liver disease [1] and was non-responsive to modern medicines was suggested liver transplantation. His presenting complaints were abdominal pain, loss of appetite, generalized weakness, itching, and swelling over the legs for the last 1 ½ months. He consulted Dr S N Gupta to seek Ayurvedic treatment. He was diagnosed as Yakrtodara[2] with Jalodara as a complication. The patient took IP treatment for 2 months (19.8.2020 to 18.10.2020), and his abdominal girth reduced to 86 cms from 89 cms, rest of the symptoms were relieved except for mild itching and mild yellow discolouration of sclera. Creatinine value is normal post ayurvedic treatments. In the first follow-up, the itching was relieved. In the second follow-up, the yellow discolouration of the sclera was relieved. Follow up done every month and the patient is completely free of symptoms and blood parameters are satisfactory. Even in patients where liver transplantation is suggested, Ayurveda can be considered as an option for treatment.
KEYWORDS
Ayurveda, chronic liver disease, yakrtodara, liver transplantation, rasayanam, liver disease, integrative
INTRODUCTION
Chronic liver disease (alcohol induced): ALD, accounts for a large portion of morbidity and mortality. In 2010, alcoholic cirrhosis caused half a million deaths worldwide, accounting for 50% of all cirrhosis-related mortality. Early diagnosis of ALD is important to encourage alcohol abstinence, minimize the progression of liver fibrosis, and manage cirrhosis-related complications including hepatocellular carcinoma. The overall incidence of hepatocellular carcinoma is increasing, and it is currently the main cause of death in patients with cirrhosis, including those with ALD. In such a scenario, Ayurveda can be considered as an option of treatment to help maintain the quality of life and be in remission.
PATIENT INFORMATION
A 40-year-old male patient suffered from abdominal pain, loss of appetite, generalized weakness, itching and swelling over legs since last 1 ½ months. There is no relevant family, or psychosocial history.
Medical History: The patient developed pain in the abdomen and loss of appetite on 2nd July 2019. He consulted a general physician and took treatment for 10 days. Provisional diagnosis was made as Hepatitis with Cirrhosis (?), and treatment was given. In August 2019, endoscopy done diagnosed with Mild oesophagitis, pan gastritis and PHG. He tried conventional medicines but did not get relief. Moreover, there was an increase in general weakness and pedal oedema. Thereafter he was referred to a gastroenterologist in Ahmedabad city. He got a one-month treatment with no improvement. His condition was continuously deteriorating. His blood parameters (liver profile) were continuously increasing. As he was not responding to the treatment, and the symptoms were worsening, he was advised to undergo liver transplantation. At this stage, he was referred to Ayurveda, by his friends, and thus came to the Ayurvedic hospital on 19.8.2019.
CLINICAL FINDINGS
Abdominal girth- 89 cms. Weight 72.9kgs; Height 176cms; BMI- 23.53kg/m2
Icterus, yellow discoloration of skin, mild distension of abdomen and pedal oedema. The patient was fully conscious and oriented. His mental status was normal.
TIMELINE
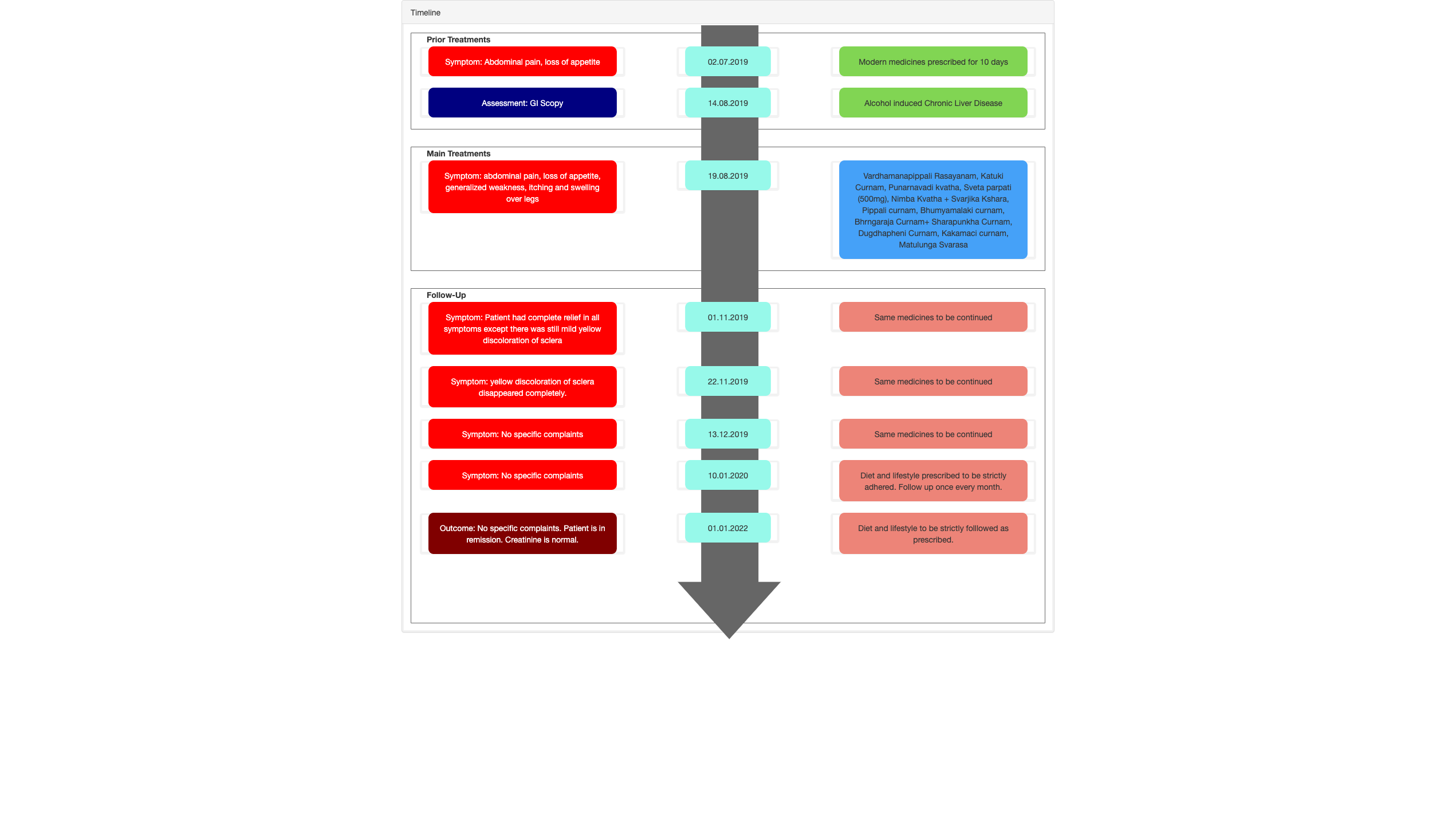
Image 1. Timeline of events attached below
DIAGNOSTIC ASSESSMENT
Modern Diagnostic parameter: The records available from the modern hospital confirm the diagnosis as Chronic liver disease – alcohol induced.
Image 2. Diagnosis proof document. Hospital records attached here.
Image 3. Blood parameters showing a high LFT values before Ayurvedic treatment attached below
Ayurvedic Assessment was done based on the clinical evaluation by the ayurvedic physician, and the confirmed biomedical diagnosis from the modern hospital.
Differential Diagnosis- This does not apply as the patient came in with a definite diagnosis.
Prognosis- The pathology of the alcohol-induced liver disease consists of three major lesions with progressive injury rarely existing in a pure form: (1) fatty liver, (2) alcoholic hepatitis, and (3) cirrhosis. The prognosis of severe alcoholic liver disease is dismal. Liver transplantation is indicated for chronic hepatitis with cirrhosis. This patient opted out of liver transplantation and sought Ayurvedic treatment. Post Ayurvedic treatments, he got complete relief and is in remission now. He was on tab.rifaximine, tab.rabeprazole, tab.ursodeoxycholicacid, tab.niacinamide, tab.ondesatron, tab.fexofinamide, tab.predmet (corticosteroid), vitamin E and frusemide. All his medicines except Ursodeoxycholic acid and frusemide were stopped, after starting the Ayurvedic treatment.
THERAPEUTIC INTERVENTION
See the tab ' Treatment Details'
FOLLOW-UP AND OUTCOMES
First follow up (01/11/2019)
The patient had complete relief in all symptoms except there was still mild yellow discolouration of sclera.
Second follow up (22/11/2019)
In clinical examination, yellow discolouration of the sclera disappeared completely.
Third follow up (13/12/2019)
No specific complaints.
Fourth follow up (10/01/2020)
No specific complaints. Creatinine value has significantly reduced. The patient comes for follow-up every month. The biochemistry investigations are normal.
Clinician-based assessment; At the baseline the abdominal girth was 89 cms, during treatment, his abdominal girth was 83cms and after treatment it was 86 cms. At the time of discharge there was mild itching and rest of symptoms were relieved. On clinical examination, there was mild yellow discoloration of sclera.
Patient-assessed: Not relevant
Follow up test results: Blood parameters like Creatinine, Bilirubin, SGPT, SGOT, Serum Proteins, Albumin, Globulin are satisfactory.
Image 4. Midpoint and Endpoint Blood parameters attached below
Intervention adherence and tolerability: The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment: By monitoring the patient.
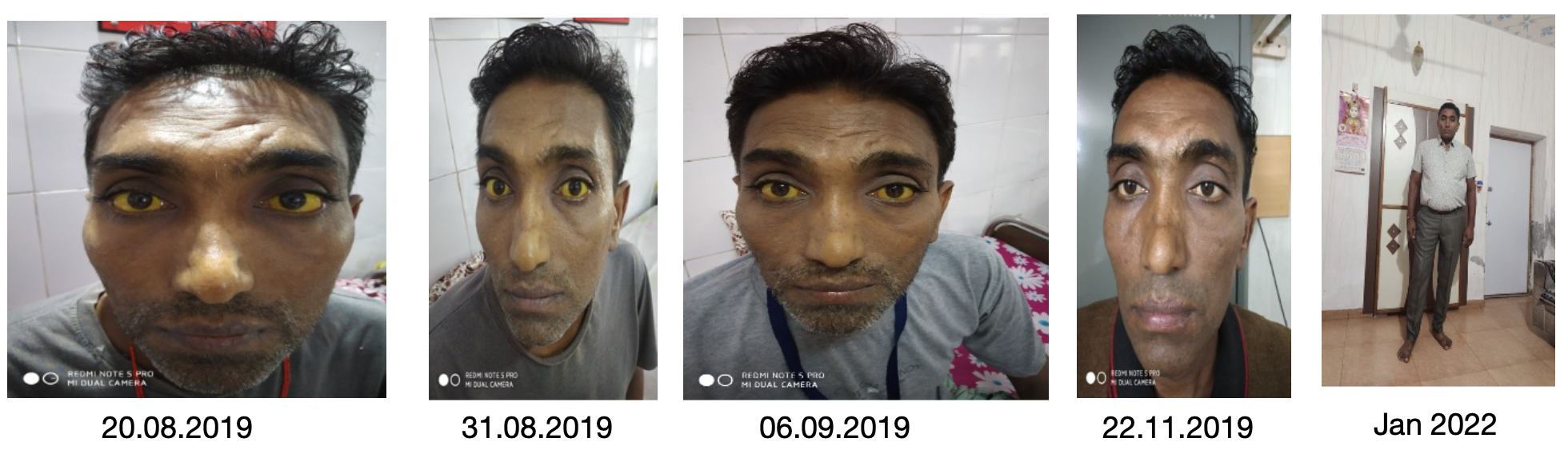
Image 5. Patient images from baseline to endpoint attached below
Adverse and unanticipated events: None reported
DISCUSSION:
In Ayurveda, dipana and rasayana treatments are recommended for udararoga. If there is ascites or pedal oedema, then mutravirecana is recommended. The patient is advised to avoid taking water in case of ascites. Camel milk is recommended for food. Bhumyamalaki, bhrngaraja, katuki, sharapunkha are hepatoprotective and widely used in liver diseases. Dugdhapheni is given for mutravirecana. Kakamaci is rasayana, tridosa samaka and useful in shotha. Matulunga is specifically useful in shakhashrita kamala. Even after getting complete symptomatic relief, and the blood parameters being satisfactory, it is necessary to follow wholesome regimens to prevent a recurrence.
PATIENT’S PERSPECTIVE
Not available.
LEARNING POINTS/TAKE-HOME MESSAGES
Even in patients of Chronic Liver Disease (alcohol induced) where liver transplantation is suggested as the best treatment option, Ayurvedic treatments can be recommended as an alternative treatment. Diet and lifestyle to be strictly adhered to along with complete abstinence from alcohol. Medicines should be continued, and regular follow-ups are required.
INFORMED CONSENT
Written consent obtained from patient.
ACKNOWLEDGEMENTS
Dr Pankaj Chayyani.
CONFLICT OF INTEREST
None declared.
FUNDING
None
REFERENCE
- Fan J, Shi Y, Peng Y. Autophagy and Liver Diseases. Adv Exp Med Biol. 2020;1207:497-528. doi: 10.1007/978-981-15-4272-5_37. PMID: 32671772.
- Kiran et al. Analytical review of Yakrit vikara mentioned in Ayurveda and contemporary medicine. World Journal of Pharmacy and Pharmaceutical Sciences. Vol 11, Issue 8, 2022.
Image 1. Timeline of events
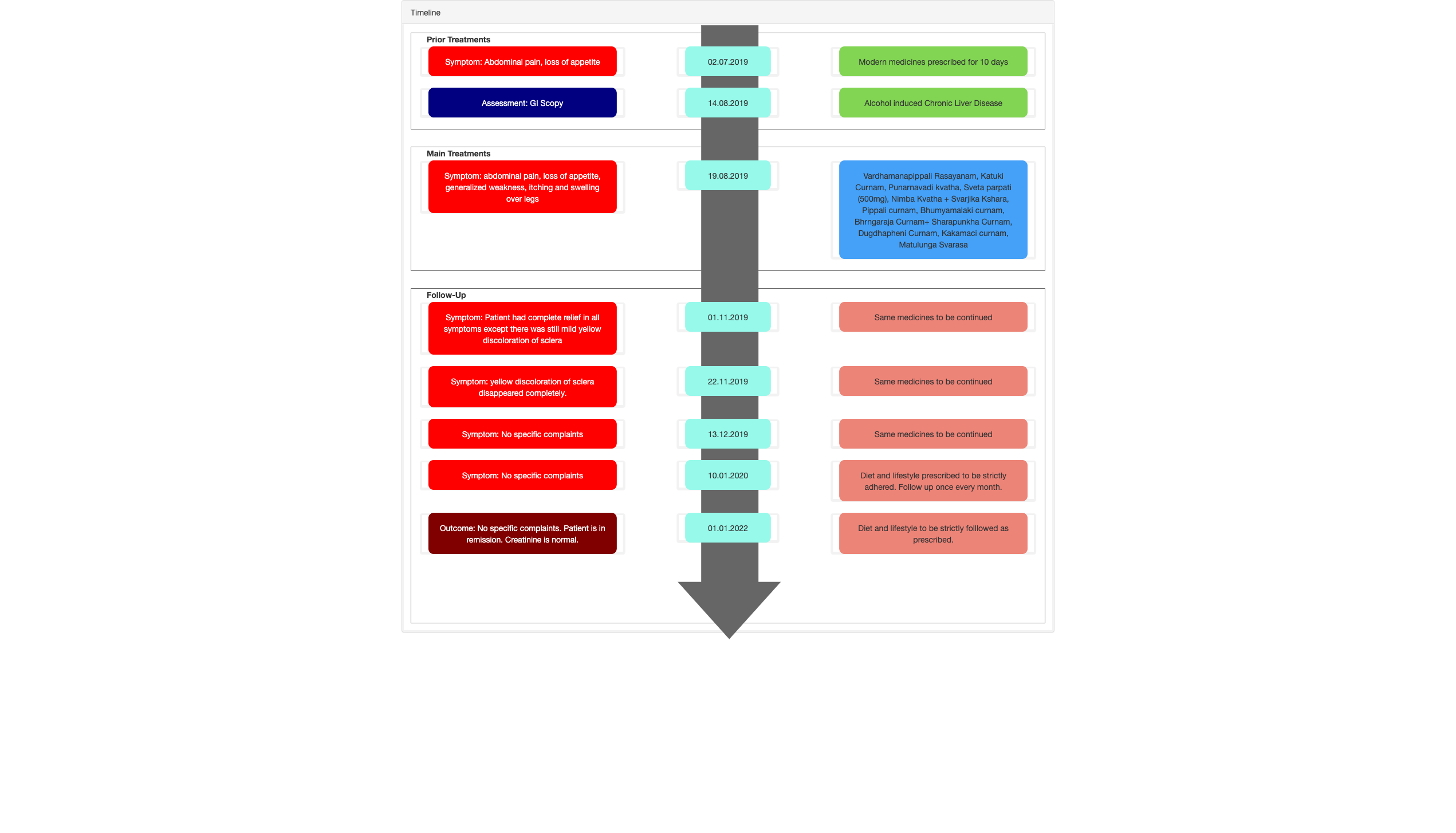
Image 2. Diagnosis proof document. Hospital records

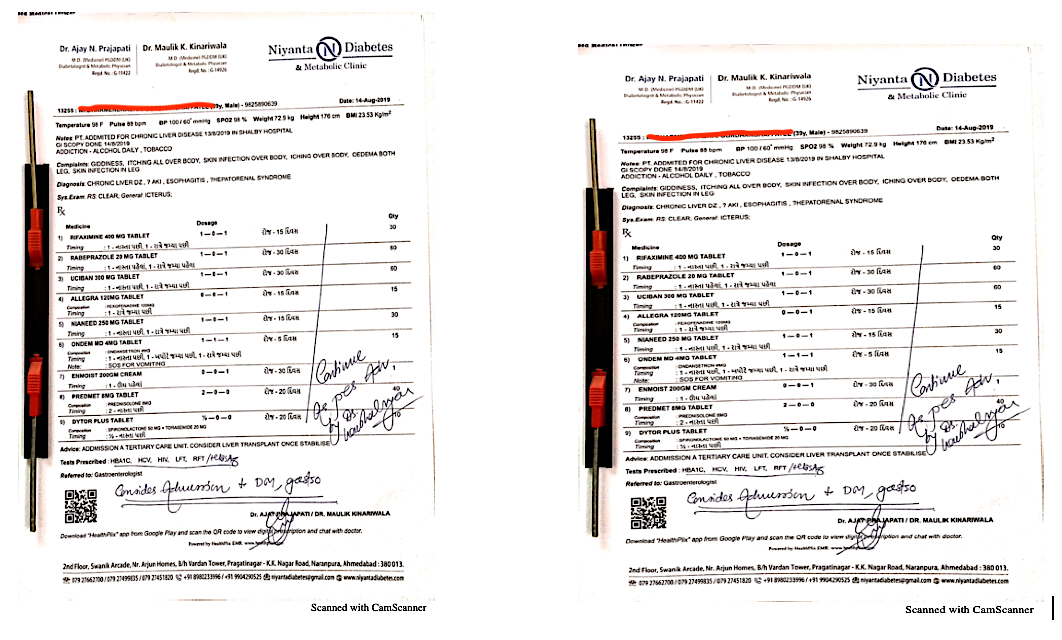
Image 3. Blood parameters showing a high LFT values before Ayurvedic treatment
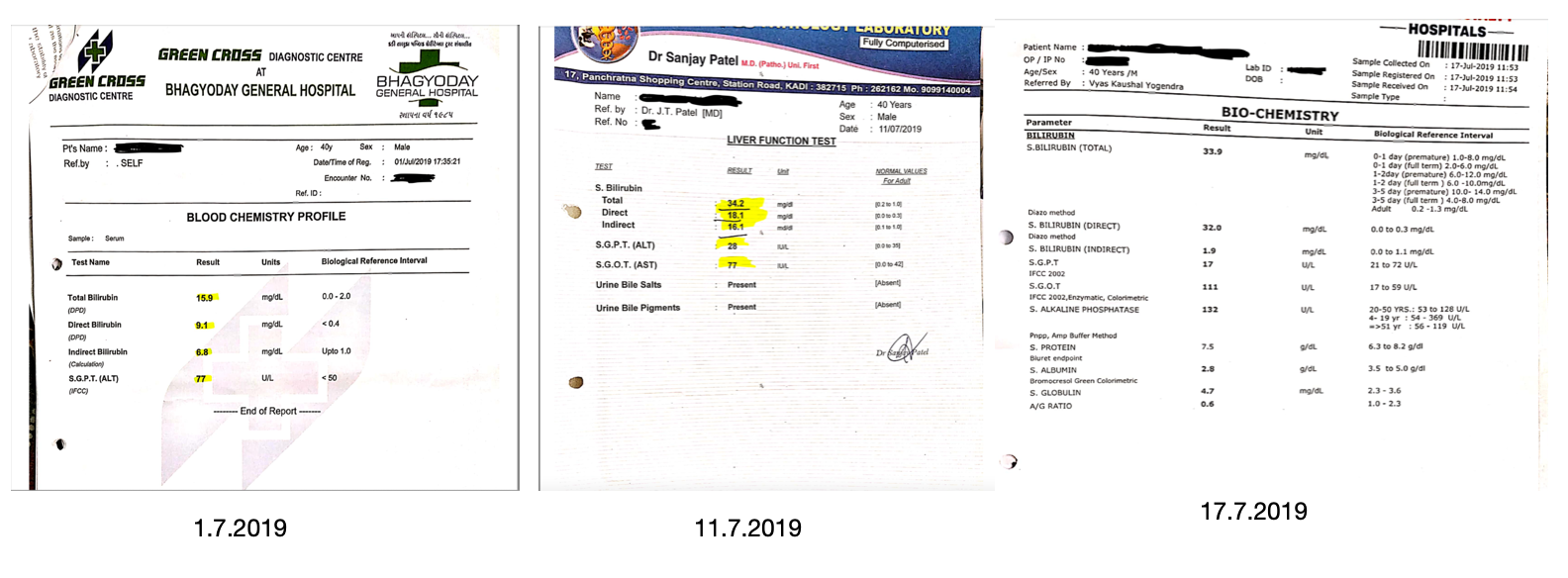

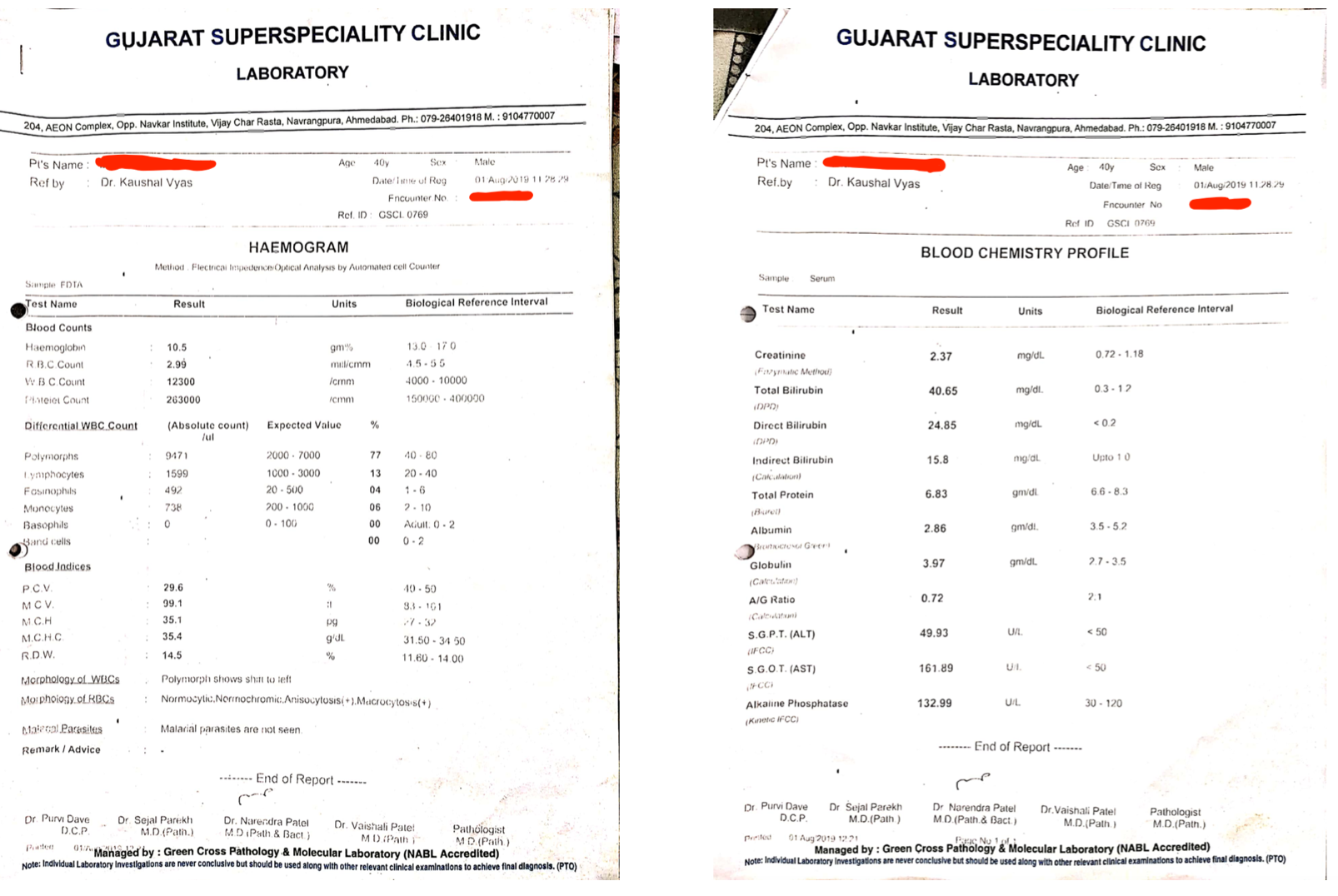
Image 4. Endpoint and follow up blood parameters
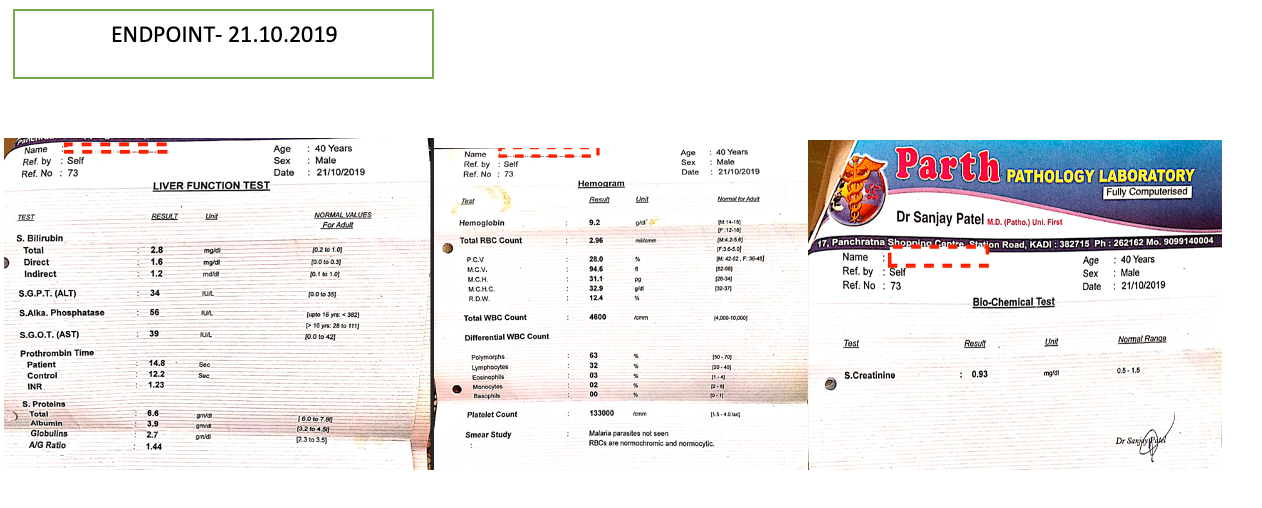

Image 5. Patient images from baseline to endpoint
-
Immersive Learning
-
Modern Diagnosis
MODERN DIAGNOSIS: Chronic Liver Disease (Alcoholic induced)
About the disease:
About 35 % of the alcohol drinkers, are affected with advanced liver disease, while the rest handle the clinical condition with medical help. There are still no pharmacological or nutritional therapies that are FDA-approved to be used in the treatment of alcoholic liver disease. Excessive and chronic consumption of alcohol results in a range of hepatic lesions, like steatosis, hepatitis, and fibrosis/cirrhosis. This is a progressive disorder and requires medical intervention immediately. Cessation of drinking (i.e., abstinence) is an integral part of therapy. Liver transplantation remains the life-saving strategy for patients with end-stage alcoholic liver disease (Osna NA, Donohue TM Jr, Kharbanda KK. Alcoholic Liver Disease: Pathogenesis and Current Management. Alcohol Res. 2017;38(2):147-161. PMID: 28988570; PMCID: PMC5513682)
Prognosis: In the initial stages, like fatty changes the condition can be reversed. But when fibrosis and cirrhosis set in, it becomes irreversible. Alcohol abstinence is a mandatory rule as a part of therapy. The target of the treatment is to try and normalise the blood parameters and help maintain the quality of life. If the patient is nonresponsive to treatment and the condition worsens, then liver transplantation is suggested.
In this patient, the symptoms started in July 2019. He started allopathic medicines immediately. The diagnosis was confirmed by the conventional medicine expert: GI Scope done on 14/8/2019– Mild oesophagitis, Pangastritis PHG. The symptoms like pedal oedema, yellow discolouration of the skin, icterus and abdominal distention were worsening and there was no change in the abnormal blood values of the liver profile, in spite of taking conventional medicine for 1 and half months. He was suggested Liver transplantation due to the elevated blood values and the deteriorating clinical condition. When he came for ayurvedic consultation in August 2019, he was on tab. rifaximine, tab. rabeprazole, tab. ursodeoxycholic acid, tab. niacinamide, tab. ondesatron, tab. fexofinamide, tab. predmet (corticosteroid), vitamin E and frusemide, and was suggested Liver transplantation.
Treatment options: Medical and surgical interventions are available depending upon the extent of liver damage. Liver transplantation is the last option suggested if the patient is nonresponsive to the treatments, causing a clinical deterioration. In this patient, the ayurvedic physician targeted at pacifying the aggravated dosas and protecting the liver at the same time. The Agni had to be pacified and medicines were given to relieve the oedema.
Diagnostic Criteria: The diagnosis was made based on the reports obtained from the Modern hospital. The blood chemistry reports and the modern prescription copy was submitted. The reports of the modern doctor suggest Liver transplantation is also available.
Image 1. July Provisional Diagnosis- Hepatitis and Liver Cirrhosis?/ August 2019- Diagnosed as Chronic Liver Disease attached below
Blood investigations dated July 2019: The Liver profile values are high.
Image 2. Liver Function Tests July 2019. Attached below
The patient was recommended for Liver transplantation from a Modern hospital: 19.7.2019
Image 3. Recommendation for Liver Transplantation attached below
Image 4. The conventional medicines the patient had tried August 2019 attached below
Baseline Blood parameters dated 1.8.2019, prior to starting the Ayurvedic treatment.
Image 5. Baseline blood parameters attached below
Continuous monitoring of the liver profile showed abnormal values despite taking conventional medicine for 1 and half months.
Image 1. July Provisional Diagnosis- Hepatitis and Liver Cirrhosis?/ August 2019- Diagnosed as Chronic Liver Disease

Image 2. Liver Function Tests July 2019


Image 3. Recommendation for Liver Transplantation

Image 4. The conventional medicines the patient had tried August 2019

-
Ayurveda Diagnosis
AYURVEDA DIAGNOSIS: Yakrtodaram
About the Disease:
The term ‘Yakrt Vikara’ was first expounded by Bhavamishra in his treatise along with a detailed classification. ‘Ya’ stands for activity and ‘krt’ indicates disintegration or breaking down. So ‘Yakrt’ can be defined as an organ that breaks down various factors inside the body. The term ‘Vikara’ means disease. Yakrit is very important because it is the raktavaha srotas mulam.It is the ashaya of pitta and agni. When the yakrt is affected, the metabolism of rasa and rakta dhatu are affected, thus manifesting in Kamala. This also matches with the modern concept of derangement of bile pigments thus causing the yellow discolouration. Udara is generally used to indicate abnormal enlargement of the organ due to accumulation of fluid. Yakrtodara can be correlated to Ascites. Madhava Nidana mentions 13 different types of udara, and yakrtodara is one among them. Mala sancaya and Vata vrddhi can be considered as the main causative factors. Mala sancaya is the main causative factor for all the udara rogas.
Samprapti- This is basically a tridoshaja vyadhi, but pitta is the main aggravated dosa, as yakrit is pittasthana. Rasa, Rakta and Medas are the dushyas involved. The srotas affected are rasavaha, raktavaha, medovaha, annavaha, and purishavaha. Vyaktasthana is udara and it is a krcchra sadhya vyadhi.
In this patient, the addiction to alcoholism can be considered as the nidana for causing the yakrtodaram. He is also addicted to tobacco. The disease has been diagnosed as a chronic liver disease- alcohol-induced, but the symptoms manifested only one and half months back. The patient was clinically deteriorating and the blood parameters like Liver Function Tests and Creatinine were very high.
Caraka in Cikitsa sthana , 13th chapter explains in detail about the lakshana of Yakrtodara.
Acarya mentions that the symptoms of plihodara and yakrtodara are identical in features and can be managed in a similar way. Daurbalya, arocaka, avipaka, varcamutraghatam, pipasa, angamarda, chardi, murccha, angasada, kasa, shvasa etc are the symptoms. All or some of the symptoms may manifest in a patient suffering from this condition. In this patient, the symptoms were icterus, yellow discolouration of the skin, pedal oedema, and abdominal distention.
Prognosis- Kricchrasadhya vyadhi
Treatment- Vatanulomana is the main target in udara rogas. In pittadhishthana rogas, like yakrit, virecana is the best treatment option to pacify the aggravated pitta. Virecana is also indicated in bahudoshavastha and srotorodha. As pitta gets pacified, there is also a direct pacifying effect on rakta. (CS. Si.6.9).
In this patient, the physician targeted pacifying the tridoshas to address the samprapti, yakrt samrakshana to protect the affected organ, dipana and pacana to correct the metabolism, and mutra virecana to give relief from oedema.
Ayurvedic Assessment and Diagnosis: This patient is a confirmed case of Acute Liver Disease. Based on the lakshanas, clinical evaluation and the confirmed biomedical diagnosis, the Ayurvedic diagnosis was made.
The Physician’s rationale for treatment: In Ayurveda, dipana and rasayana treatments are recommended for udararoga. If there is ascites or pedal oedema, then mutravirecana is recommended. The patient is advised to avoid taking water in case of ascites. Camel milk is recommended for food. Bhumyamalaki, bhringaraja, katuki, and sharapunkha are hepatoprotective and widely used in liver diseases. Dugdhapheni is given for mutravirecana. Kakamaci is rasayana, tridosa samana and is indicated in shotha. Matulunga is specifically useful in shakhashrita kamala. Even after getting complete relief, it is necessary to follow wholesome regimens to prevent a recurrence. As this condition is alcohol induced, it is mandatory that the abstinence from alcohol also must be followed along with treatment advice.
-
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Vardhamanapippali Rasayanam Curnam Started with one gram twice a day on first day and increased 1 gm twice every day to reach five gram Oral with milk 2019-08-19 - 2019-08-30 CS.Ci.1.3 Katuki Curnam Curnam 5 gms Virecanam- Oral, with warm water on empty stomach 2019-08-31 - 2019-08-31 Anubhuta Yogam Punarnavadi Kvatha Kasayam 40 ml Oral, with warm water twice daily 2019-08-19 - 2022-12-31 Sahasrayogam, Kasaya Prakaranam Sveta Parpati Parpati 500 mg Oral, with warm water twice daily 2019-09-01 - 2022-12-31 Sidha yoga sangraha; Mutrakricchra Adhikara. Nimba Kvatha + Svarjika Kshara Snana drava Required quantity To be used for bathing in a luke warm form 2019-09-01 - 2022-12-31 Anubhuta Yogam Pippali curnam Curnam 1 gm Oral with warm water twice daily 2019-09-01 - 2022-12-31 Anubhuta Yogam Bhumyamalaki curnam Curnam 3 gms Oral, with warm water twice daily 2019-09-01 - 2022-12-31 Anubhuta Yogam Bhrngaraja curnam + Sharapunkha curnam Curnam 2 gms each Oral, with warm water twice daily 2019-09-01 - 2022-12-31 Anubhuta Yogam Dugdhapheni curnam Curnam 2 gms Oral, with warm water twice daily 2019-09-01 - 2022-12-31 Anubhuta Yogam Kakamaci curnam Curnam 3 gms Oral, with warm water twice daily 2019-09-01 - 2022-12-31 Anubhuta Yogam Matulunga svarasa Svarasa 20 ml Oral, twice a day 2019-09-01 - 2022-12-31 Anubhuta Yogam -
Outcome Measures
OUTCOME MEASURE:
The 40-year-old male patient, diagnosed with Chronic Liver Disease – alcohol-induced, presented with very high Bilirubin (Direct & Indirect), SGOT and SGPT values and symptoms like icterus, yellow discolouration of the skin, abdominal distention and pedal oedema. The symptoms were worsening in spite of taking conventional medicines since 1 and half months. When the modern medicine expert suggested Liver transplantation, he opted for Ayurveda. At the time of admission for ayurvedic treatment, he was also taking conventional medicines- tab. rifaximine, tab. rabeprazole, tab. ursodeoxycholic acid, tab. niacinamide, tab. ondesatron, tab. fexofinamide, tab. predmet (corticosteroid), vitamin E and frusemide. But after treatment, only ursodeoxycholic acid and frusemide were continued, and the rest of the modern medicine was stopped. He got complete relief from his symptoms. The abdominal girth reduced from 89 cms to 86 cms. His liver profile was satisfactory.
The blood parameters at the endpoint and in follow-up were satisfactory. Repeat blood tests done after 9 months, showed satisfactory values, and the patient is leading a normal life.
Image 1. Endpoint Blood tests dated 21.10.2019 attached below.
Image 2. Follow up Blood test dated May 2020 attached below
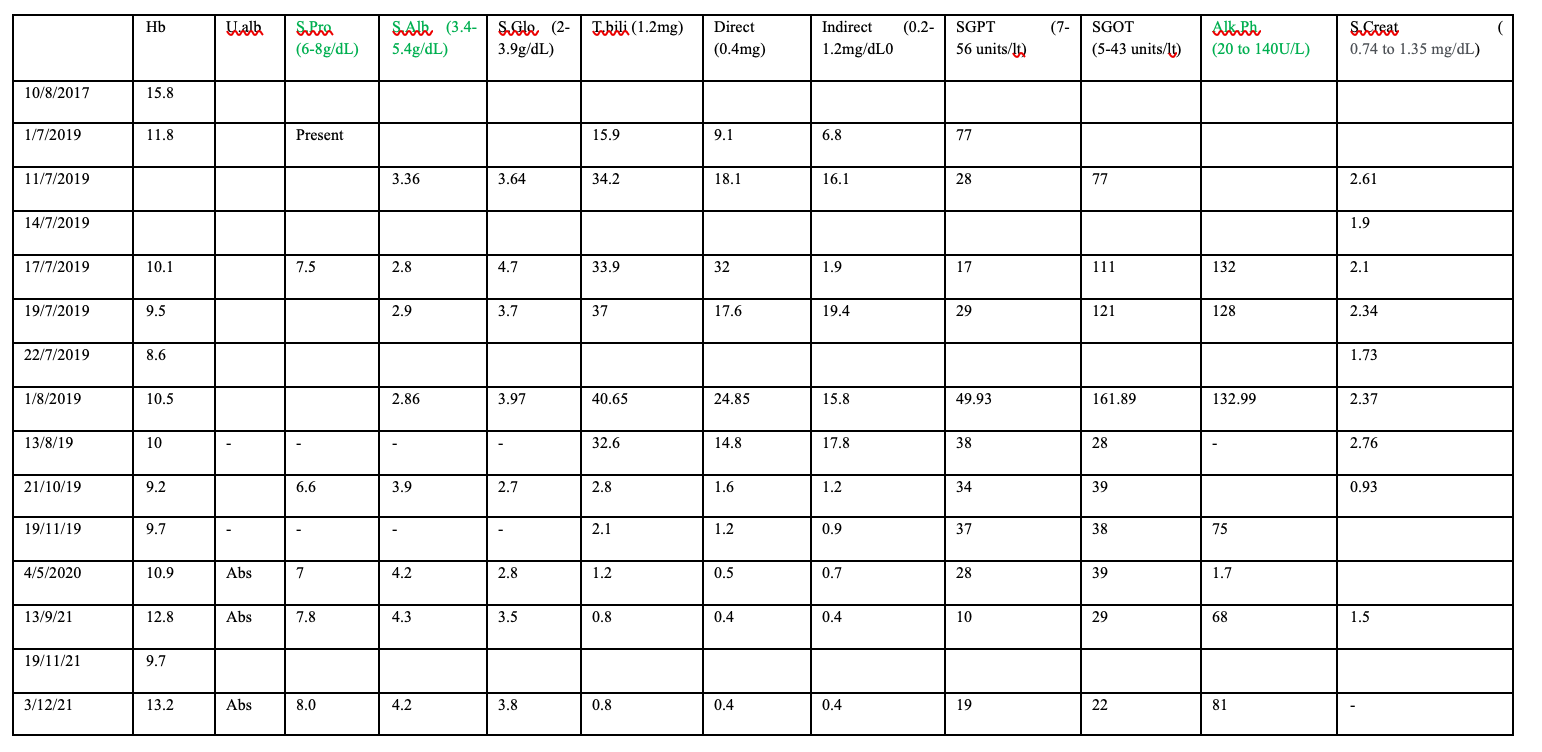
Image 3. Blood parameters tabulated datewise (From the treating physician's notes) attached below.
Disease-modifying effect: Complete relief from symptoms and blood parameters are satisfactory. Patient was advised to strictly abstain from alcohol and follow diet and lifestyle recommendations.
Image 4. Images of the patient taken at baseline, midpoint, endpoint and follow up attached below.
Image 1. Endpoint Blood tests dated 21.10.2019

Image 2. Follow up Blood test dated May 2020

Image 3. Blood parameters tabulated datewise documented by the treating physician

Image 4. Images of the patient taken at baseline, midpoint, endpoint and follow up

-


