Featured Case
-
Abstract
A 30-year-old female COVID positive patient was hospitalised on 7th May 2021 presenting with fever, body ache, and breathing difficulty since 1 week. On 10th May, her saturation was dropping to less than 90 even with 15 litres of NRBM. She was shifted to ICU. On 19th May, saturation dropped to 40 and she started gasping for breath. The patient also developed high grade fever and diarrhea. In spite of treatment with strong antibiotics and steroids, her condition rapidly deteriorated, and she presented with acute respiratory distress syndrome. The SpO2 dropped to 40, that demanded immediate intubation. Her blood parameters like TC, LFT, CRP, IL-6 were elevated, inspite of treatments. An emergency was declared, and the grave prognosis was explained to the family. The family did not want to intubate and requested to try Ayurvedic management. Dr Aswath Rao, who is a Junior resident, General Surgery- Bengaluru Medical college, under the guidance of his parents, Dr Ramesh and Dr Shobha Rao who are Ayurvedic Doctors, as per request of the family and with permission from the Hospital authorities, gave the Ayurvedic medicines. SpO2 normalized within 2 hours of starting the Ayurvedic treatment, and then remained stable throughout. The Liver Function Test, Total Count, CRP and IL-6 that were elevated normalized within 5 days. All Ayurvedic medicines were stopped after 20 days. The patient became stable and after the Respiratory distress was managed, she completed her course of modern medicine in the hospital and was discharged.
Take Away Message- This case report is an exapmle for the successful management of an emergency clinical condition like acute respiratory distress syndrome with Ayurvedic medicines. Here, an integrative approach helped the patient to come back to normal.
-
Summaries
-
Listen
-
Watch
-
View

-
Read
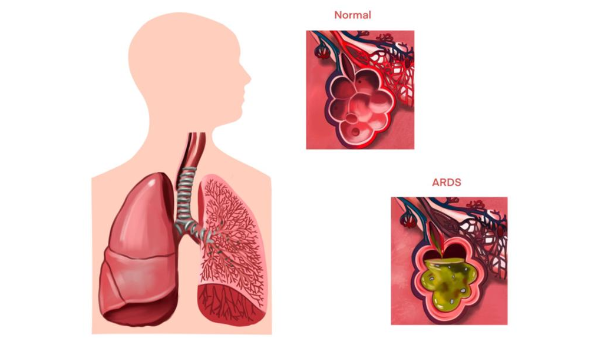
A 30-year-old female COVID positive patient was hospitalised on 7th May 2021 presenting with fever, body ache, and breathing difficulty since 1 week. On 10th May, her saturation was dropping to less than 90 even with 15 litres of NRBM. She was shifted to ICU. On 19th May, saturation dropped to 40 and she started gasping for breath. The patient also developed high grade fever and diarrhea. In spite of treatment with strong antibiotics and steroids, her condition rapidly deteriorated, and she presented with acute respiratory distress syndrome. The SpO2 dropped to 40, that demanded immediate intubation. Her blood parameters like TC, LFT, CRP, IL-6 were elevated, inspite of treatments. An emergency was declared, and the grave prognosis was explained to the family. The family did not want to intubate and requested to try Ayurvedic management. Dr Aswath Rao, who is a Junior resident, General Surgery- Bengaluru Medical college, under the guidance of his parents, Dr Ramesh and Dr Shobha Rao who are Ayurvedic Doctors, as per request of the family and with permission from the Hospital authorities, gave the Ayurvedic medicines. SpO2 normalized within 2 hours of starting the Ayurvedic treatment, and then remained stable throughout. The Liver Function Test, Total Count, CRP and IL-6 that were elevated normalized within 5 days. All Ayurvedic medicines were stopped after 20 days. The patient became stable and after the Respiratory distress was managed, she completed her course of modern medicine in the hospital and was discharged.
Take Away Message- This case report is an exapmle for the successful management of an emergency clinical condition like acute respiratory distress syndrome with Ayurvedic medicines. Here, an integrative approach helped the patient to come back to normal.
-
-
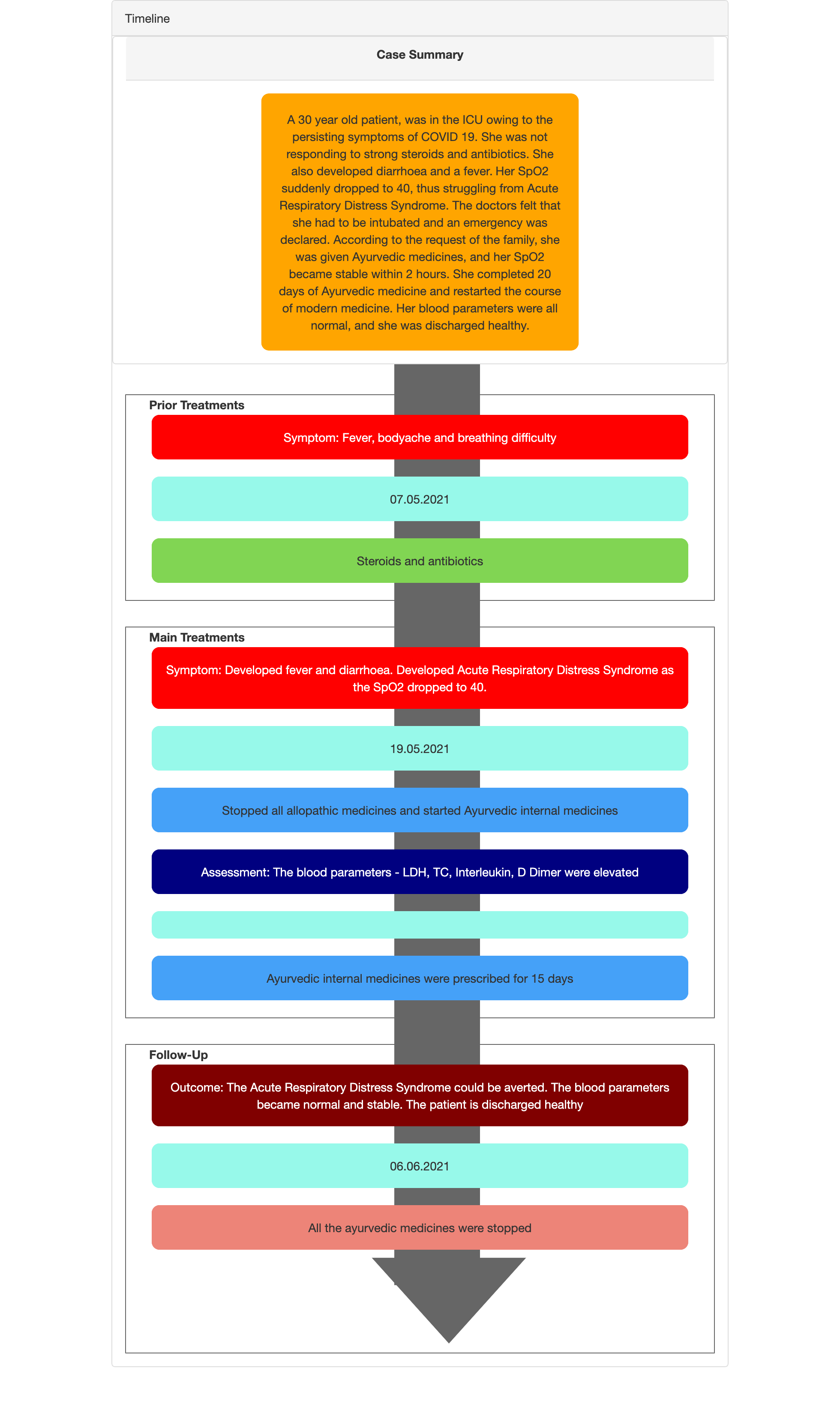
Timeline

-
Tabulated Summary
-
Narrative
TITLE OF CASE
Emergency management of Acute Respiratory Disorder Syndrome in a COVID positive patient on NIV (Non-Invasive Ventilation) with Ayurvedic-A Case report
Dr Aswath Rao, Dr Ramesh Rao, Dr Shobha Rao
ABSTRACT
A 30-year-old female was a confirmed case of COVID 19[1], was hospitalised to manage her symptoms. She was on non-invasive ventilation and developed acute respiratory distress syndrome (ARDS). Her SpO2 dropped down to 40. She was not responding to the antibiotics and steroids, her condition was rapidly deteriorating, she was suggested to be intubated. The family requested they try Ayurveda, and with permission from the Hospital, Dr Aswath Rao consulted his parents Dr Ramesh and Shobha Rao who were Ayurvedic Doctors and gave medicines. Within 2 hours, her SpO2 became normal, blood parameters improved gradually, and the patient became stable clinically. She took 20 days of Ayurvedic Medicines and was shifted back to room from ICU. She then had to continue modern medicines to complete the course and was discharged.
KEYWORDS
COVID, ARDS, Non-invasive ventilation, SpO2, Intubation
INTRODUCTION
The coronavirus disease 19 (COVID-19) is very contagious and also a pathogenic viral infection by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), believed to have originated in Wuhan, China and later became a pandemic. Unfortunately, there is no clinically approved antiviral drug or vaccine that is directly proven to be effective against COVID-19. Now very effective vaccines have been developed to combat the Covid Virus.
Diagnostic Criteria: Initially an Antigen test is used to test for COVID, then a confirmatory test is done with real-time fluorescence (RT- PCR) to detect SARS-CoV-2 positive nucleic acid in sputum, throat swabs, and lower respiratory tract sample secretions. Further tests and imaging are done, if the symptoms are severe or if the patient is deteriorating.
PATIENT INFORMATION
A 30-year-old female, a confirmed case of COVID positive was hospitalised on 7th May 2021 presenting with fever, body ache, and breathing difficulty for 1 week. On 10th May, her saturation was dropping to less than 90 even with 15 litres of NRBM. So, on 10th May she was shifted to ICU. Her condition was deteriorating day by day. The patient did not respond to medicines like Remdesivir, Tocilizumab and even antibiotics like Teicoplanin, colistin, Meropenam. The Total WBC counts reached up to 25500. Now she developed high grade fever and diarrhoea. On 19th May, on ventilator (NIV), fio2 100, by the end of the day- saturation started dropping down to 40. The Doctors in charge of the ICU believed she has to be intubated immediately. The patient was critical, and emergency was declared. But the family requested to try Ayurveda, and so obtaining permission from the Hospital authorities, and guided by Dr Ramesh and Dr Shobha who were Ayurvedic Physicians, medicines were prescribed.
PHYSICAL EXAMINATION & CLINICAL FINDINGS
Patient is conscious, tachypnic. HR- 90bpm; BP- 106/46mm Hg: SpO2- 40. ABG (19/5/2021) - pH- 7.2. pCO2- 38.1. pO2- 38.4. HCO3- 24.2. On NIV, prone position.24/16; F1O2- 100 %. At baseline SpO2- 40.
TIMELINE
Image 1. Attached below
DIAGNOSTIC ASSESSMENT
Modern Diagnostic parameter: The records available from the modern hospital confirm the diagnosis as COVID positive and ARDS was induced by COVID.
Image 2. Diagnosis proof- Hopsital Record and the coneventional medicines prescribed
Image 3. Blood parameters at Baseline- Before starting Ayurvedic Treatments
Image 4. ICU monitor depicting the drop of SpO2
Ayurvedic Assessment was done by Dr Ramesh and Dr Shobha based on the inputs given.
Differential Diagnosis- This does not apply as the patient came in with a definite diagnosis.
Prognosis- There was no vaccine or medicine that was proved to be effective for COVID-19 at that point of time. The treatment was symptomatic and the patients with severe infection were given oxygen therapy. In cases of respiratory failure mechanical ventilation is required whereas hemodynamic support is important for septic shock management[1]. In this patient, even the strong antibiotics administered could not reverse the symptoms.
THERAPEUTIC INTERVENTION
See the Tab 'Treatment Details'
FOLLOW-UP AND OUTCOMES
Not relevant. The patient was discharged after her complete course of treatment, and she became stable.
Clinician-based assessment; Within 24 hours of starting the Ayurvedic medicines- IL-6 decreased from 380 to 14 (Normal range 5-7). CRP became normal. TC reduced significantly.
High value of LFT was corrected within 3 days. The patient became comfortable and now had smooth breathing. Endpoint vitals: After 1 hour of Ayurvedic medicines SpO2- crossed 76: After 2 hours of Ayurvedic treatment- SpO2 crossed 90.
Image 5. ICU Monitor after 2 hours of starting Ayurvedic medicines:
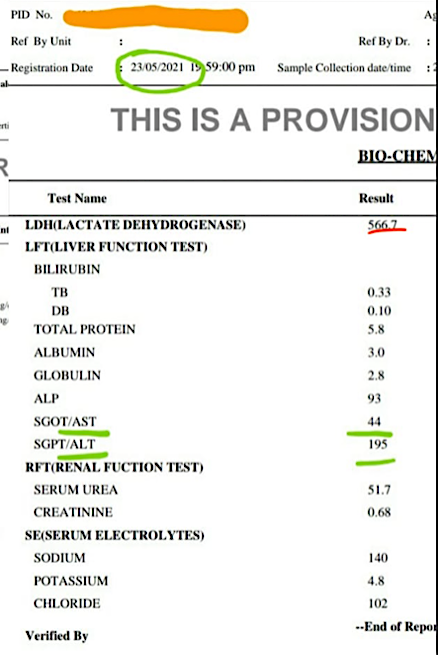
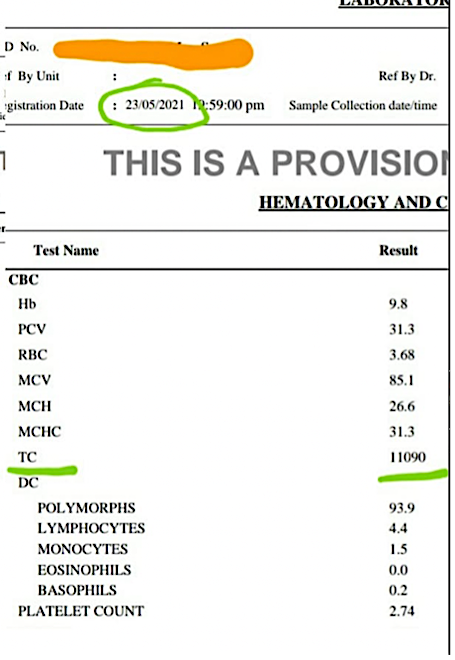
Image 6. Blood Parameters after starting Ayurvedic Treatments: (23/5/2021)
Patient-assessment: Not relevant
Intervention adherence and tolerability – The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment- By monitoring the patient.
Adverse and unanticipated events; None reported
DISCUSSION
This case report is of a patient who was in the ICU department of a Modern Hospital. When the prognosis was declared as grave, and the clinical condition of the patient was critical, the family requested to try Ayurveda. As per this request, Dr Aswath Rao, who oversaw the patient in the ICU at that time, sought the help of his parents Dr Ramesh and Dr Shobha Rao, who were Ayurvedic physicians to prescribe the medicines. With the permission from the family and the Hospital, the oral medicines were administered, and the patient became stable within 2 hours. An exact Ayurvedic correlation was not given here, but the target was to address the inflammation and to protect the heart and the lungs.
PATIENT’S PERSPECTIVE
Not available.
LEARNING POINTS/TAKE-HOME MESSAGES
When this case was being documented, there were no exact protocols being brought into practice for the treatment of COVID. This patient was rapidly sinking and was nonresponsive to the antibiotics and steroids that were administered to her. With a wise decision made by the Doctor and the family, they tried Ayurveda as an alternative that could stabilize her. She completed her entire course of modern medicines also before getting discharged from the hospital in a healthy condition.
INFORMED CONSENT
Written consent obtained from patient.
ACKNOWLEDGEMENTS
Dr Ramesh Rao and Dr Shobha Rao
CONFLICT OF INTEREST
None declared.
FUNDING
None
REFERENCE
- Mousavizadeh L, Ghasemi S. Genotype and phenotype of COVID-19: Their roles in pathogenesis. J Microbiol Immunol Infect. 2021 Apr;54(2):159-163. doi: 10.1016/j.jmii.2020.03.022. Epub 2020 Mar 31. PMID: 32265180; PMCID: PMC7138183.
- Sharma A, Ahmad Farouk I, Lal SK. COVID-19: A Review on the Novel Coronavirus Disease Evolution, Transmission, Detection, Control and Prevention. Viruses. 2021 Jan 29;13(2):202. doi: 10.3390/v13020202. PMID: 33572857; PMCID: PMC7911532.
Image 1. Timeline of events
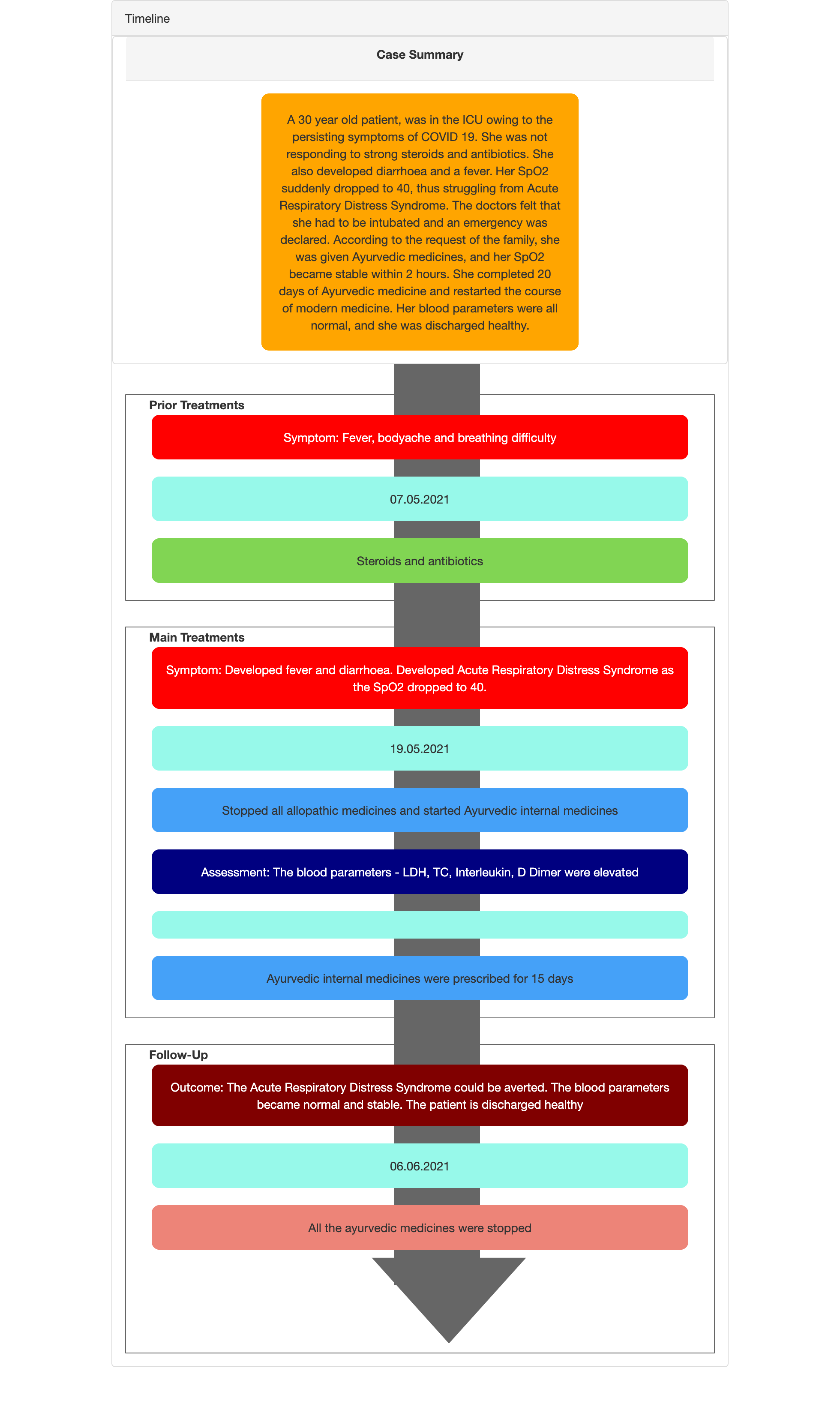

Image 2. Diagnosis proof- Hopsital Record and the conevntional medicines prescribed (7.5.2021). Grave Prognosis declared on 19.5.2021.
 .
. 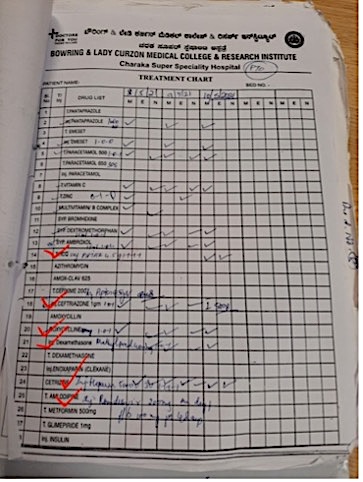

Image 3. Baseline blood parameters in order 15.5.2021, 19.5.2021, and 20.5.2021
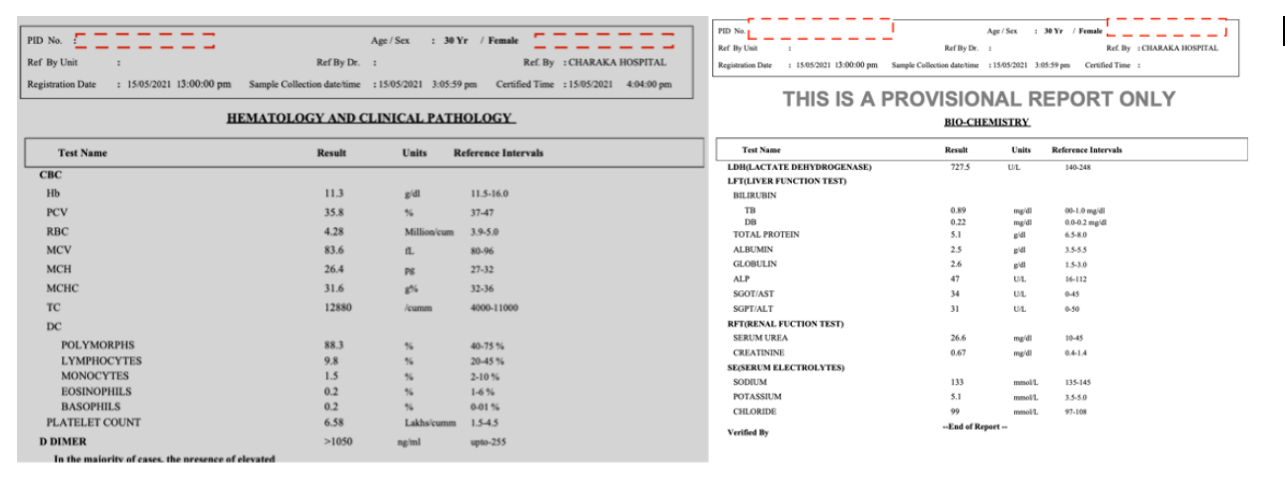
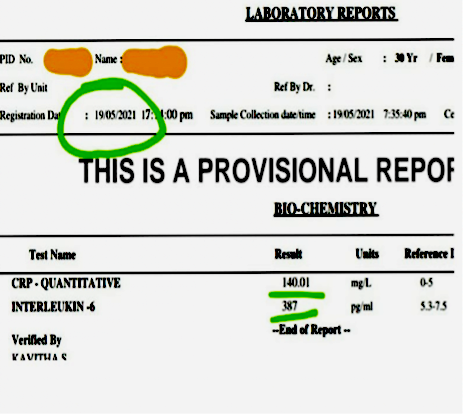
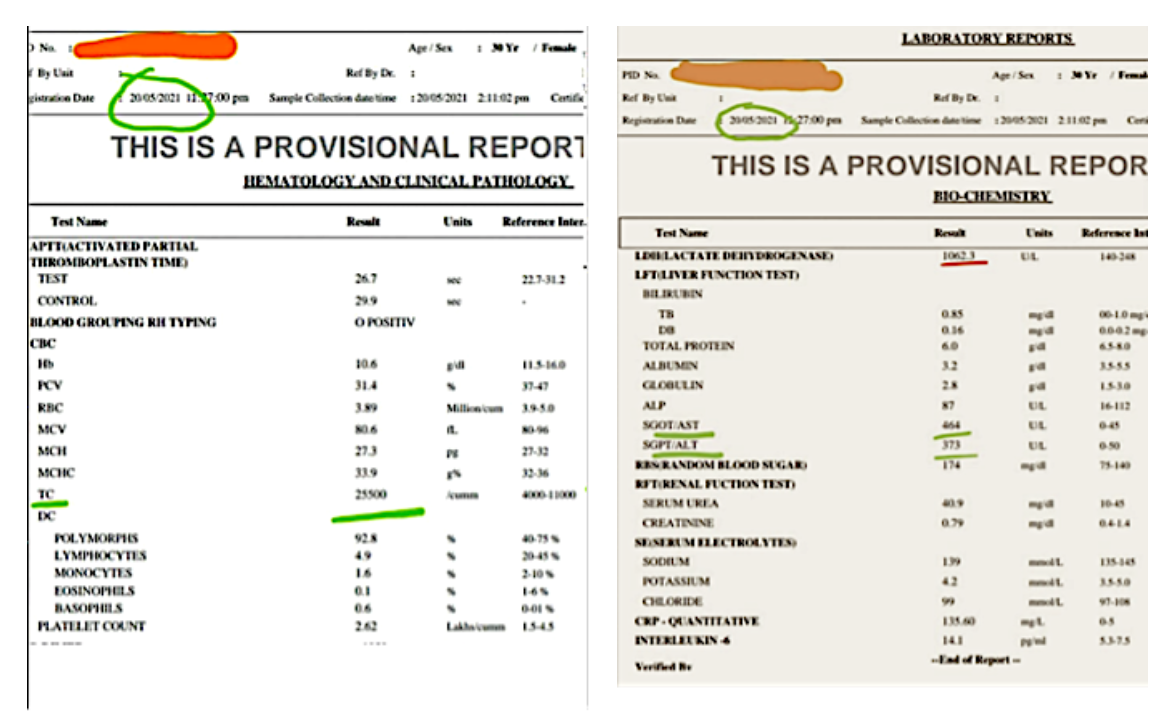
Image 4. ICU monitor depicting the drop of SpO2. 19.5.2021
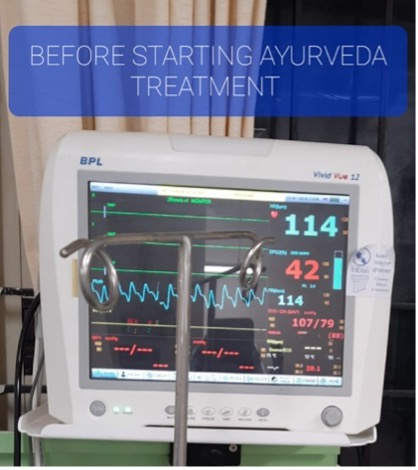
Image 5. ICU Monitor after 2 hours of starting Ayurvedic medicines:
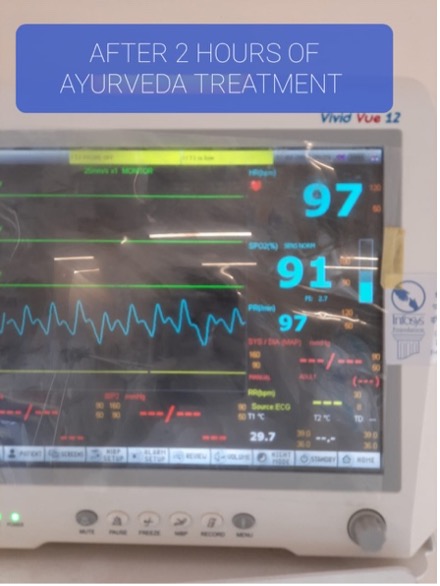
Image 6. Blood Parameters after starting Ayurvedic Treatments: (23/5/2021)
-
Immersive Learning
-
Modern Diagnosis
MODERN DIAGNOSIS: Acute Respiratory Disorder Syndrome in a COVID 19
ABOUT THE DISEASE:
The coronavirus disease 19 (COVID-19) is very contagious and also a pathogenic viral infection by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), became a pandemic within a short span of time. Unfortunately, there is no clinically approved antiviral drug or vaccine that is proven to be effective against COVID-19. There are a few broad-spectrum antiviral drugs studied for its efficacy to counteract the COVID-19.
Symptoms: The common symptoms are cough, fatigue, and fever, fewer common symptoms are headache, haemoptysis, lymphopenia, sputum and gastrointestinal disorders. The chest CT scan reveals pneumonia, but grave presentations like acute cardiac injury, or respiratory distress syndrome also manifest. Patients with mild symptoms recover within a week usually, whereas in severe cases, there occurs progressive respiratory failure caused by alveolar damage, and this is life-threatening.
ARDS in COVID 19- In this case report, the patient is confirmed case of COVID 19, and was hospitalised and on Non-invasive ventilation. But her condition worsened and SpO2 dropped to 40. She was in Acute Respiratory Distress Syndrome and ventilator was advised. She was not responding to the spectrum of antibiotics and steroids that were prescribed. She also developed associated symptoms like diarrhoea and temperature. Emergency was declared and the grave prognosis was explained to her family. Her LDH, SGOT, SGPT, CRP, Interleukin, D DIMER were all very high and WBC was also increasing. The family wanted to try Ayurveda. Dr Aswath Rao was on duty in the ICU, so as requested by the patient’s family, with the permission from the hospital authorities, he sought guidance from his parents who were ayurvedic physicians, started the ayurvedic medicines. Within 2 hours of starting Ayurvedic treatments, her SpO2 normalised and remained stable. Repeat blood tests showed significant reduction in the abnormal blood values.
Diagnostic Criteria- conducting real-time fluorescence (RT- PCR) to detect SARS-CoV-2 positive nucleic acid in sputum, throat swabs, and lower respiratory tract sample secretions .
Image 1. Hospital Records. Attached below
Image 2. Medications prescribed Attached below
Image 3. ARDS Emergency with Low SpO2 and Grave Prognosis declared
Previous medicines; Remdesivir, Tocilizumab and even antibiotics like Teicoplanin, colistin, Meropenam. She was not responding to the treatments and the condition was worsening day by day.
Treatment- At present, there are vaccinations available for COVID, and it is not as terrorising as it was 2 years back. But during the outbreak in 2020, there was a lot of confusion due to lack of diagnostics and proper treatment parameters. The death toll was very high, and the doctors were also at a loss, not knowing exactly how the grave presentations had to be handled. But at the time, the patient was admitted, there were no treatment protocols to manage the condition. The treatment is symptomatic and the patients with severe infection are given oxygen therapy. In cases of respiratory failure mechanical ventilation is required whereas hemodynamic support is important for septic shock management. In this patient, even the strong antibiotics administered could not reverse the symptoms.
Image 4. Baseline blood parameters Attached Below
Image 1. Hospital Records confirming diagnosis

Image 2. Conventional medicines prescribed

Image 3. Low level SpO2 monitored. Grave Prognosis declared


Image 4. Blood parameters in order- 15.5.2021, 19.5.2021 and 20.5.2021



-
Ayurveda Diagnosis
Ayurvedic Assessment was done by Dr Ramesh and Dr Shobha based on the inputs given. An Ayurvedic Diagnosis was not given by the team.
-
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Jayamangala Rasa Rasa 1-0-1 Sublingual 2021-05-19 - 2021-06-17 Proprietary Medicine Swasa Kasa Cintamani rasa Rasa 1-0-1 Oral 2021-05-19 - 2021-06-17 Rasayogaratnakara.2.213 Makaradhwaja Gutika Gutiks 1-0-1 Oral 2021-05-19 - 2021-06-17 Proprietary Medicine Hemagarbha Potali Rasa 1-0-1 Sublingual 2021-05-19 - 2021-06-17 Yogaratnakara.Kasa Mallagarbha Potali Rasa 1-0-1 Sublingual 2021-05-19 - 2021-06-19 Rasayoga Sagara Rasa Sindhoora Rasa 0-1-0 Sublingual 2021-05-19 - 2021-06-17 Rasatarangini.6.162-176 Trailokyachintamani Rasa Rasa 0-1-0 Oral 2021-05-19 - 2021-06-17 Bhaishajya Ratnavali. Rasayana prakarana. 136-143 Swasakutar Rasa Rasa 1-0-1 Oral 2021-05-19 - 2021-05-28 Bhaishajya Ratnavali. Shavasa Rogadhikara Abraka bhasma Bhasma 1-0-1 Sublingual 2021-05-19 - 2021-05-23 Rasatarangini.10.39-42 Abraka bhasma Bhasma 1-0-1 Sublingual 2021-05-24 - 2021-06-28 Rasatarangini.10.39-42 Choushashta pippali Tablet 1-1-1 Oral 2021-05-19 - 2021-05-23 Ayurveda Sarasangraha Choushashta pippali Tablet 1-0-1 Oral 2021-05-24 - 2021-06-28 Ayurveda Sarasangraha Chandramrita rasa Tablet 1-1-1 Oral 2021-05-19 - 2021-05-23 Bhaishajyaratnavali. Kasarogadhikara.121-126 Chandramrita rasa Tablet 1-0-1 Oral 2021-05-24 - 2021-05-28 Bhaishajyaratnavali. Kasarogadhikara.121-126 Sitopaladi Curnam Curnam 1 tsp Oral, with warm water 2021-05-19 - 2021-05-23 Ayurved Sar Sangrah, Churna Prakarna -
Outcome Measures
OUTCOME MEASURES
The 30 year old female patient was a confirmed case of COVID positive and hospitalised for management of symptoms. But she was deteriorating and shifted to ICU within 3 days. Despite strong antibiotics to manage her fever and diarrhoea, she developed ARDS induced by COVID 19, and SpO2 suddenly dropped to 40. As allopathic medicines were not helping her, the condition was managed with Ayurvedic medicines. An emergency was declared, and ventilator was suggested. The relatives requested Ayurvedic medicine be tried out. Within 2 hours of starting the Ayurvedic medicines, the SpO2 became normal and remained stable throughout.
Image 1. After 2 hours of starting Ayurvedic medicines- ICU Monitor
Blood parameters checked on the next day and after 2 days showed a significant reduction in the abnormal values. The patient was becoming stable. After 20 days, the ayurvedic medicines were discontinued, and supportive allopathic medicines were given until discharge to complete her course of treatment. In this case report, the initial crisis of ARDS due to COVID, was averted with Ayurvedic medicines.
Image 2. Blood Parameters showing a significant improvement after 3 days of Ayurvedic Treatment.
DISEASE MODIFYING EFFECT- ARDS resolved. The SpO2 is stable, and the patient has no respiratory distress. The Blood parameters were showing a significant reduction within 2 days of treatment. Ayurvedic medicines were continued for another 20 days and then stopped.
Image 1. After 2 hours of starting Ayurvedic medicines- ICU Monitor

Image 2. Blood Parameters after 3 days of Ayurvedic Treatment

-

