Featured Case
-
Abstract
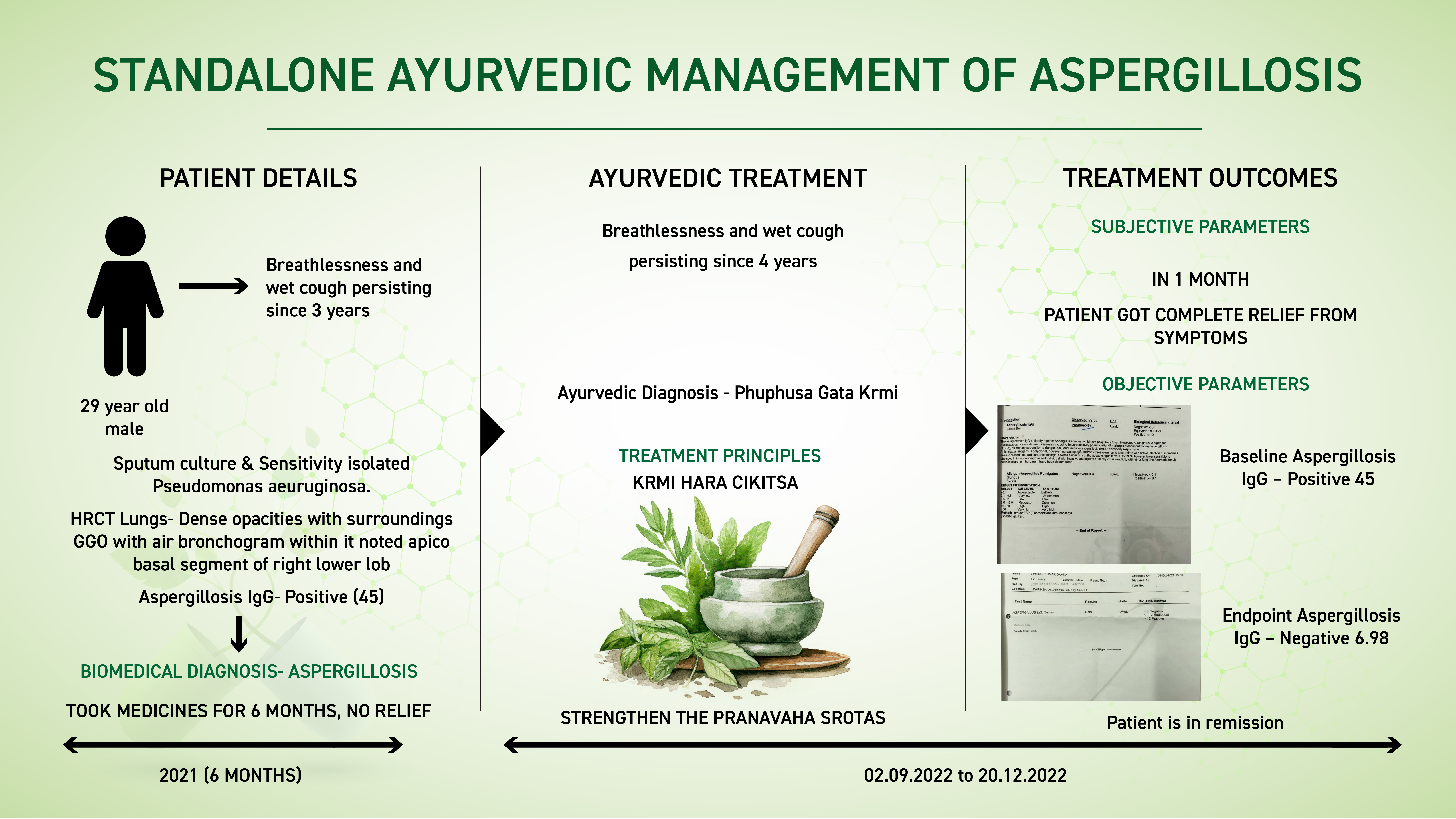
A 29 year old male patient presented with breathlessness and wet cough persisting since 4 years. It was only 1 year back that he consulted an allopathic doctor. Sputum culture and sensitivity test done isolated Pseudomonas aeruginosa. HRCT Lungs- Dense opacities with surroundings GGO with air bronchogram with in it noted apico basal segment of right lower lobe. Aspergillosis IgG was Positive with a reading of 45. Based on the clinical evaluation and the investigations, the biomedical diagnosis was made as Aspergillosis. He took conventional medicines for 6 months, but did not get relief. He now consulted Dr Rajnikanth for ayurvedic management. The ayurvedic diagnosis was Phuphusa gata krmi. The line of treatment followed was Krmi hara cikitsa. Strengthening the pranavaha srotas by including medicines indicated in shvasa roga was also a part of the treatment plan. With 1 month of Ayurvedic treatment, he got complete relief from all the symptoms. The Aspergillosis IgG became negative and the reading was 6.98U/ml. This case report demonstrates the standalone ayurvedic management of Aspergillosis in a patient who did not get relief despite taking conventional medicines.
-
Summaries
-
Listen
-
Watch
-
View
-
Read
A 29 year old male patient presented with breathlessness and wet cough persisting since 4 years. It was only 1 year back that he consulted an allopathic doctor. Sputum culture and sensitivity test done isolated Pseudomonas aeruginosa. HRCT Lungs- Dense opacities with surroundings GGO with air bronchogram with in it noted apico basal segment of right lower lobe. Aspergillosis IgG was Positive with a reading of 45. Based on the clinical evaluation and the investigations, the biomedical diagnosis was made as Aspergillosis. He took conventional medicines for 6 months, but did not get relief. He now consulted Dr Rajnikanth for ayurvedic management. The ayurvedic diagnosis was Phuphusa gata krmi. The line of treatment followed was Krmi hara cikitsa. Strengthening the pranavaha srotas by including medicines indicated in shvasa roga was also a part of the treatment plan. With 1 month of Ayurvedic treatment, he got complete relief from all the symptoms. The Aspergillosis IgG became negative and the reading was 6.98U/ml. This case report demonstrates the standalone ayurvedic management of Aspergillosis in a patient who did not get relief despite taking conventional medicines.
-
-
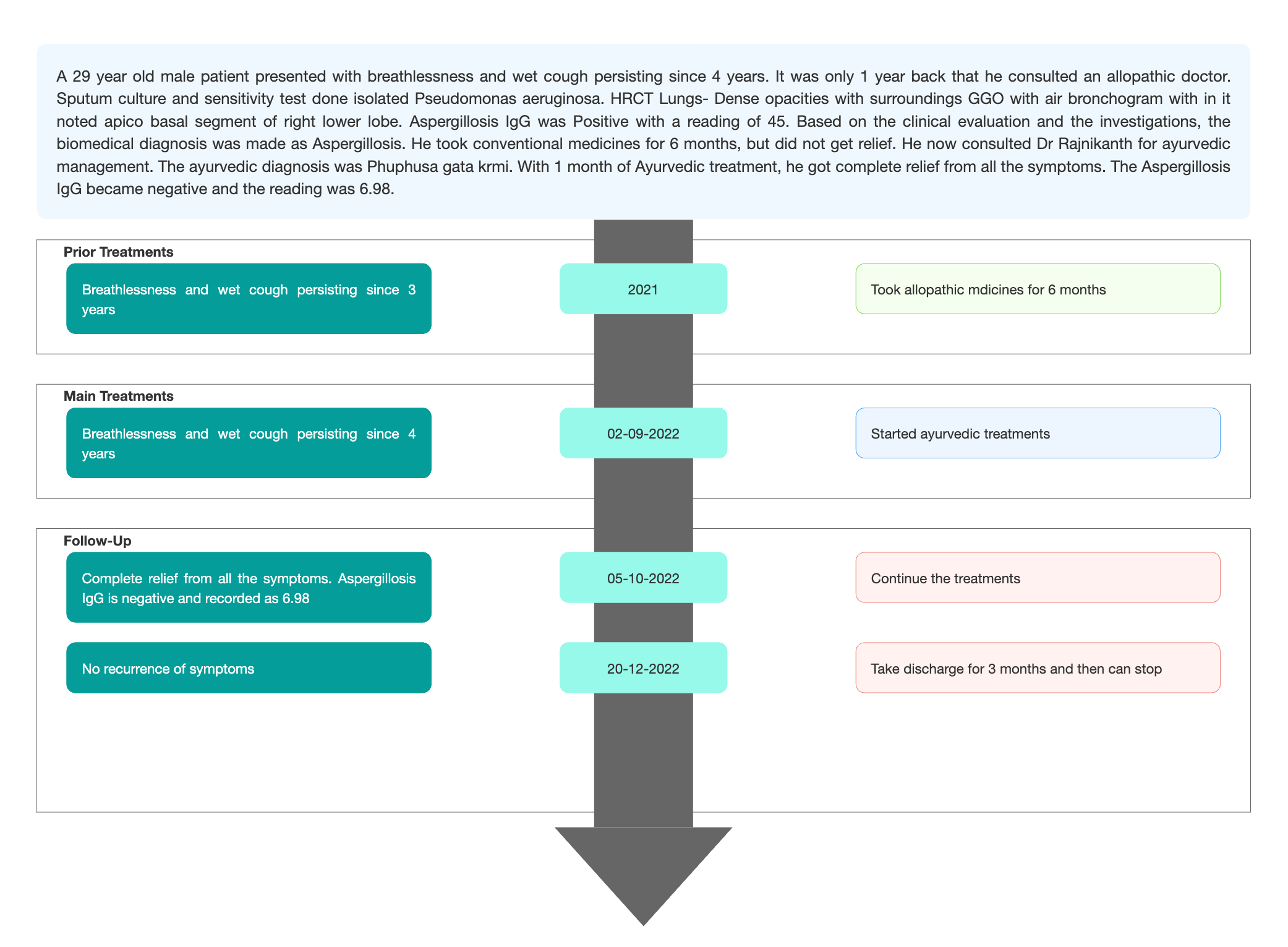
Timeline
-
Tabulated Summary
-
Narrative
TITLE OF CASE
Standalone successful ayurvedic management of Aspergillosis- A case report
Dr Rajnikanth Patel
ABSTRACT
A 29 year old male patient presented with breathlessness and wet cough persisting since 4 years. It was only 1 year back that he consulted an allopathic doctor. Sputum culture and sensitivity test done isolated Pseudomonas aeruginosa. HRCT Lungs- Dense opacities with surroundings GGO with air bronchogram with in it noted apico basal segment of right lower lobe. Aspergillosis IgG was Positive with a reading of 45. Based on the clinical evaluation and the investigations, the biomedical diagnosis was made as Aspergillosis. He took conventional medicines for 6 months, but did not get relief. He now consulted Dr Rajnikanth for ayurvedic management. The ayurvedic diagnosis was Phuphusa gata krmi. The line of treatment followed was Krmi hara cikitsa. Strengthening the pranavaha srotas by including medicines indicated in shvasa roga was also a part of the treatment plan. With 1 month of Ayurvedic treatment, he got complete relief from all the symptoms. The Aspergillosis IgG became negative and the reading was 6.98U/ml. This case report demonstrates the standalone ayurvedic management of Aspergillosis in a patient who did not get relief despite taking conventional medicines.
KEYWORDS
Aspergillosis, cough, case report, krmi, phuphusa, phuphusa gata, lungs
INTRODUCTION
Aspergillosis is a term for an infection caused by several types of Aspergillus fungi (plural of fungus). Aspergillus is usually found outdoors, in dead leaves, plants, soil or compost. It’s occasionally found in moist environments indoors. Most people breathe in Aspergillus spores every day without getting sick. But in certain people, Aspergillus can cause allergic reactions, chronic lung conditions and invasive disease that spreads to your brain, kidneys, lungs or other organs.
Types of aspergillosis
- Allergic bronchopulmonary aspergillosis (APPA).
- Aspergilloma (“fungus ball”).
- Chronic pulmonary aspergillosis.
- Invasive aspergillosis. Fever is a common symptom.
Symptoms: Symptoms of aspergillosis vary depending on the type and location in your body. Symptoms of infections or allergic reactions in your lungs are the most common.
They include:
- Coughing (sometimes coughing up blood).
- Shortness of breath (dyspnea).
- Noisy breathing (wheezing).
- Chest pain.
- Fever.
Fatigue and weight loss can be symptoms of chronic pulmonary aspergillosis.
Additional symptoms may be present depending upon the part of the body affected.
Diagnostic criteria: Medical history and clinical evaluation are the basic diagnostic criteria used. This method used will depends on the symptoms and health history. Imaging like X-rays or CT scans, biopsy, tests of fluid or tissue, and allergy tests all help to diagnose various forms of aspergillosis. Its symptoms look similar to many other illnesses, so additional tests may be required to rule out other conditions.
Treatment: Surgery, antifungal medications and corticosteroids are the most common treatment options. The treatment chosen will depend on the part affected.
Prognosis: Surgery or antifungals can cure some types of noninvasive aspergillosis. In some cases, it may go away and come back again (recur). Invasive aspergillosis can be very hard to cure.
PATIENT INFORMATION
A 29 year old male patient presented with breathlessness and wet cough persisting since 4 years. It was only 1 year back that he consulted an allopathic doctor. Sputum culture and sensitivity test done isolated Pseudomonas aeruginosa. HRCT Lungs- Dense opacities with surroundings GGO with air bronchogram with in it noted apico basal segment of right lower lobe. Aspergillosis IgG was Positive with a reading of 45. Based on the clinical evaluation and the investigations, the biomedical diagnosis was made as Aspergillosis.
No significant family/surgical/psychosocial or genetic history.
CLINICAL FINDINGS
Pain in chest and epigastric area
Respiratory system examination:
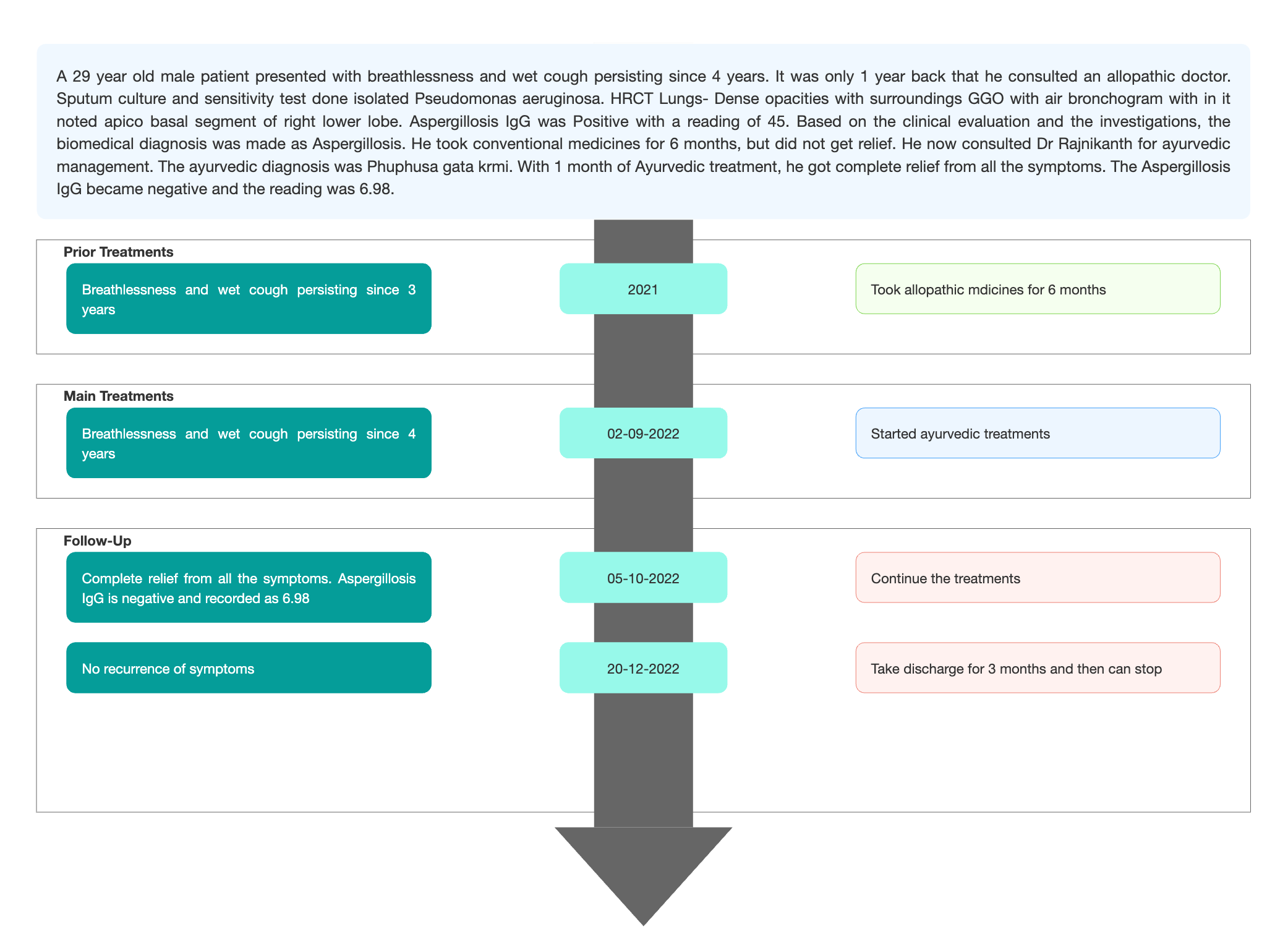
Auscultation- Wheeze + (right)TIMELINE
Image 1. Timeline of events added below
DIAGNOSTIC ASSESSMENT
Modern Diagnostic parameter; The biomedical diagnosis was confirmed based on the clinical evaluation, sputum culture and sensitivity test, and Aspergillosis IgG (Serum EIA) test as Aspergillosis.
Image 2. HRCT Lungs dated 6.9.2021

Image 3. Sputum culture and sensitivity test dated 7.9.2021

Image 4. Cartridge based nucleic acid amplification test dated 7.9.2021

Image 5. Aspergillosis IgG (Serum EIA) report dated 9.9.2021

Image 6. Treatment history. Prescription of the conventional medicine

Ayurvedic Assessment was done based on the presenting complaints and clinical evaluation. The treating physician made the Ayurvedic diagnosis as Phuphusagata krmi.
Differential Diagnosis-
Asthma
Atypical mycobacterial infection
Bacterial pneumonia
Bacterial sinusitis with abscess
Blastomycosis
The patient was confirmed to have Aspergillosis based on the previous treatment records and the investigations done.Prognosis- The prognosis of aspergillosis is good in patients with mild alterations in function. However, many patients may require steroids for a prolonged time if the diagnosis is delayed. Delay in diagnosis may lead to steroid resistance and the development of lung fibrosis. In this case report, the patient had a long history of symptoms which was only diagnosed 1 year back. By that time the condition had worsened and even with the standard of care, the symptoms persisted. With one month of ayurvedic treatments, he attained significant relief.
THERAPEUTIC INTERVENTION
Refer the tab ‘Treatment’ in the Portal.
FOLLOW-UP AND OUTCOMES
The patient had 4 follow ups in total. Both subjective and objective assessments were done.
Clinician-based assessment; Patient presented with breathlessness and wet cough persisting since 4 years. With 1 month of Ayurvedic treatment, the patient got significant relief from the persisting cough and breathing difficulty.
Image 7. Lab reports of Aspergillosis IgG dated 5.10.2022

Intervention adherence and tolerability– The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment- Images were taken before and after treatment.
Adverse and unanticipated events; None reported
DISCUSSION ;
The patient had been suffering from the symptoms since 4 years. It was not attended to, but only 1 year back the patient consulted allopathic doctor and started conventional medicines. But the symptoms till persisted. The ayurvedic diagnosis was Phuphusagata krmi, and the line of treatment followed was basically krmi hara cikitsa. Strengthening the Pranavaha srotas was also a part of the treatment plan. With 1 month of ayurvedic treatments, the patient got complete relief from all the symptoms.
PATIENT’S PERSPECTIVE
Not available.
LEARNING POINTS/TAKE HOME MESSAGES
This case highlights the efficacy of ayurveda in successfully treating a chronic condition of aspergillosis in a patient who had persistent symptoms since 4 years and was diagnosed and took medical care only 1 year back, but did not get relief.
INFORMED CONSENT
Written consent obtained from patient for publishing the case report.
ACKNOWLEDGEMENTS
None
CONFLICT OF INTEREST
None declared.
FUNDING
None
REFERENCE
- https://my.clevelandclinic.org/health/diseases/14770-aspergillosis
-
Immersive Learning
-
Modern Diagnosis
MODERN DIAGNOSIS: Aspergillosis
ABOUT THE DISEASE:
Aspergillosis is a term for an infection caused by several types of Aspergillus fungi (plural of fungus). Aspergillus is usually found outdoors, in dead leaves, plants, soil or compost. It’s occasionally found in moist environments indoors. Most people breathe in Aspergillus spores every day without getting sick. But in certain people, Aspergillus can cause allergic reactions, chronic lung conditions and invasive disease that spreads to your brain, kidneys, lungs or other organs.
Types of aspergillosis
- Allergic bronchopulmonary aspergillosis (APPA).
- Aspergilloma (“fungus ball”).
- Chronic pulmonary aspergillosis.
- Invasive aspergillosis. Fever is a common symptom.
Symptoms: Symptoms of aspergillosis vary depending on the type and location in your body. Symptoms of infections or allergic reactions in your lungs are the most common.
They include:
- Coughing (sometimes coughing up blood)
- Shortness of breath
- Noisy breathing (wheezing)
- Chest pain.
- Fever.
Fatigue and weight loss can be symptoms of chronic pulmonary aspergillosis.
Additional symptoms may be present depending upon the part of the body affected.
A 29 year old male patient presented with breathlessness and wet cough persisting since 4 years. It was only 1 year back that he consulted an allopathic doctor. Sputum culture and sensitivity test done isolated Pseudomonas aeruginosa. HRCT Lungs- Dense opacities with surroundings GGO with air bronchogram with in it noted apico basal segment of right lower lobe. Aspergillosis IgG was Positive with a reading of 45. Based on the clinical evaluation and the investigations, the biomedical diagnosis was made as Aspergillosis. He took conventional medicines for 6 months, but did not get relief. He now consulted Dr Rajnikanth for ayurvedic management. The ayurvedic diagnosis was Phuphusa gata krmi.
In this case report, the lungs were affected.
Image 1. HRCT of Lungs dated 6.9.2021

Image 2. Sputum culture and sensitivity test dated 7.9.2021

Image 3. Cartridge based nucleic acid amplification test dated 7.9.2021

Image 4. Aspergillosis IgG (Serum EIA) report dated 9.9.2021

Image 5. Treatment history. Prescription of the conventional medicine

Diagnostic criteria: Medical history and clinical evaluation are the basic diagnostic criteria used. This method used will depends on the symptoms and health history. Imaging like X-rays or CT scans, biopsy, tests of fluid or tissue, and allergy tests all help to diagnose various forms of aspergillosis. Its symptoms look similar to many other illnesses, so additional tests may be required to rule out other conditions.
Treatment: Surgery, antifungal medications and corticosteroids are the most common treatment options. The treatment chosen will depend on the part affected.
Prognosis: Surgery or antifungals can cure some types of noninvasive aspergillosis. In some cases, it may go away and come back again (recur). Invasive aspergillosis can be very hard to cure.
Reference
-
Ayurveda Diagnosis
AYURVEDA DIAGNOSIS: Phuphusa gata kimi
ABOUT THE DISEASE:
The word Krmi is derived from dhatu ‘kunya himsAyAm’ (Siddhantakaumudi) which means ‘to kill' or to ‘yield harmful effect’. Ashtanga Hrdaya mentions that krimi are present all over the biosphere. Their Utpatti Sthanas are told as parvata (mountain), vana (forest), oushadhi (plants), pashu (animals), apsu (water).
After the Vedic period, the description of Krimi is found in Samhita Kala, where Caraka has mentioned Krimiroga in the Vimana sthana of Caraka Samhita, in the parlance of Krimija Hridroga & Sirasula, and an indirect reference in Janapadodhvamsa. The Susruta Samhita on the other hand has described Krimiroga in Nidana and Cikitsa sthana. Susruta mentions that Kushtha is a Upasargika Roga indicating that it is contagious, which in turn implies the role of the microbes. Acaryas have described Krimi roga as a primary disease and also as a causative factor for other diseases e.g. siroroga, and hridroga.
Nidana- Factors responsible for the growth of Krimi are intake of food in indigested state, excess use of madhura and amla rasa, pishtanajaggery, milk, kusumba oil, til oil, fish, anoopmamsa, sedentary life style, excess day sleeping and use of dietetic incompatibilities.
Due to causative aggravating factors, Kapha and Pitta get aggravated. It generates different types of Krimi. These Krimi reside at various places in the body like amasaya, pakvasaya, dhamani and rakta etc.विंशतिविधाः क्रिमयः पूर्वमुद्दिष्टा नानाविधेन प्रविभागेनान्यत्र सहजेभ्यः; ते पुनः प्रकृतिभिर्विभज्यमानाच्चतुर्विधा भवन्ति; तद्यथा- पुरीषजाः, श्लेष्मजाः, शोणितजा, मलजाश्चेति॥९॥ (CS.Vi.7)
There are 20 types of Krimi, which can be generally classified as Bahya and Abhyantara. The main four types of krmi are purishaja, shleshmaja, shonitaja and malaja, that can be categorised into bahya and abhyantara. Another type of classification is Drishya and Adrishya. The chikitsa sutra for krimi is Apakarshaṇa (Extraction measures), Prakriti Vighata (Antagonistic measures) and Nidana Parivarjana (Avoidance of causative factors).
A 29 year old male patient presented with breathlessness and wet cough persisting since 4 years. It was only 1 year back that he consulted an allopathic doctor. Sputum culture and sensitivity test done isolated Pseudomonas aeruginosa. HRCT Lungs- Dense opacities with surroundings GGO with air bronchogram with in it noted apico basal segment of right lower lobe. Aspergillosis IgG was Positive with a reading of 45. Based on the clinical evaluation and the investigations, the biomedical diagnosis was made as Aspergillosis. He took conventional medicines for 6 months, but did not get relief. He now consulted Dr Rajnikanth for ayurvedic management. The ayurvedic diagnosis was Phuphusa gata krmi.
Rationale of treatment as explained by the treating physician:
Table 1. The medicines/therapies and the rationale behind choosing them
Medicine
Rationale
Kabasura Kashaya
To strengthen pranavaha srotas
Swasanandam gulika
Indicated in shwasa roga
Krimighna vatika
To reduce and kill the colony of fungus in the lungs
Adhatodai kudiner
Indicated in ardra kasa chikitsa
Pushkarmoola curna and vidanga churna siddha jala
Pushkaramoola to strengthen the pranavaha srotas and vidanga for krmi cikitsa
Reference
1. CRITICAL REVIEW OF AYURVEDA DRUGS USED FOR KRIMI ROGA. WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES · January 2017 DOI: 10.20959/wjpps201711-10404 ).
2. Caraka Samhita. Vimansthana. 7.12-14
3. Sushruta Samhita Uttartantra. 54.8
-
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Kabasura Kashaya Kashaya 10 ml Oral, thrice a day 2022-09-02 - 2023-03-15 Siddha Medicine Swasanandam gulika Tablet 1 Oral, twice daily after food 2022-09-02 - 2022-12-20 Arogyakalpadrumam. Krimighna vatika Tablet 2 Oral, thrice daily after food 2022-09-02 - 2022-12-20 Ayurvedic Patent & Proprietary Medicine Adhatodai kudiner Panam 10 ml Oral, twice a day 2022-10-10 - 2022-12-20 Siddha Formulary of India, Part-1 Pushkaramoola curna + Vidanga curna Siddha jala panam Required quantity Oral 2022-09-02 - 2023-03-15 Anubhuta Yoga -
Outcome Measures
OUTCOME MEASURES
In this case report, a 29 year old male patient presented with breathlessness and wet cough persisting since 4 years. It was only 1 year back that he consulted an allopathic doctor. Sputum culture and sensitivity test done isolated Pseudomonas aeruginosa. HRCT Lungs- Dense opacities with surroundings GGO with air bronchogram with in it noted apico basal segment of right lower lobe. Aspergillosis IgG was Positive with a reading of 45. Based on the clinical evaluation and the investigations, the biomedical diagnosis was made as Aspergillosis. He took conventional medicines for 6 months, but did not get relief. He now consulted Dr Rajnikanth for ayurvedic management. The ayurvedic diagnosis was Phuphusa gata krmi.
Assessment: Both subjective and objective assessments were done.
Subjective assessment- With 1 month of ayurvedic treatment, patient got complete relief from the symptoms.
Objective assessment- Aspergillosis IgG (Serum IEA) was checked after 1 month of treatment and the value was recorded as 6.98 and marked negative.
Image 1. Lab reports of Aspergillosis IgG dated 5.10.2022

-








