Featured Case
-
Abstract
A 70 year old female patient presented with a non-healing wound in the left flank region with severe pain since 15 days associated with a foul smell. The patient consulted allopathic doctor and the diagnosis was made as Necrotising cellulitis on the left flank. She was advised for plastic surgery for wound management. She was reluctant to go for surgical management and opted for Ayurvedic treatment and approached Dr Rajnikanth. Based on the previous treatment records and clinical examination, the biomedical diagnosis was made as Necrotising wound and the Ayurveda diagnosis as Nadi/ dushta vrana. The line of treatment followed was Vrana hara cikitsa. The medicines used were indicated in vrana, and visha cikitsa. With 2 months of Ayurvedic treatment, the wound healed completely. Bates- Jensen wound assessment score was 52 before treatment became 16 after treatment. This case report demonstrates the successful standalone ayurvedic management of necrotising wound in an elderly woman who was suggested plastic surgery as the best treatment option.
-
Summaries
-
Listen
-
Watch
-
View
-
Read
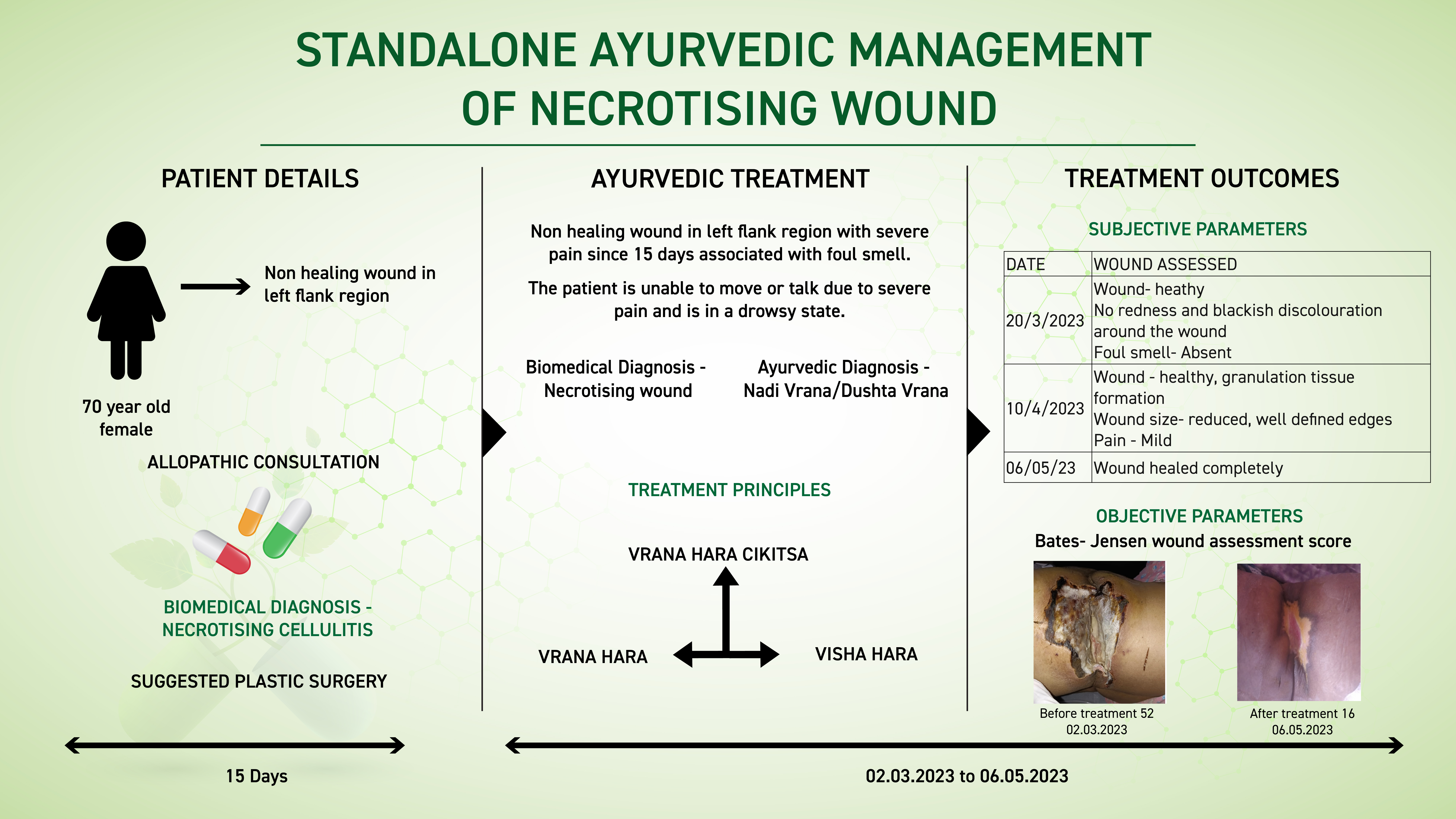
A 70 year old female patient presented with a non-healing wound in the left flank region with severe pain since 15 days associated with a foul smell. The patient consulted allopathic doctor and the diagnosis was made as Necrotising cellulitis on the left flank. She was advised for plastic surgery for wound management. She was reluctant to go for surgical management and opted for Ayurvedic treatment and approached Dr Rajnikanth. Based on the previous treatment records and clinical examination, the biomedical diagnosis was made as Necrotising wound and the Ayurveda diagnosis as Nadi/ dushta vrana. The line of treatment followed was Vrana hara cikitsa. The medicines used were indicated in vrana, and visha cikitsa. With 2 months of Ayurvedic treatment, the wound healed completely. Bates- Jensen wound assessment score was 52 before treatment became 16 after treatment. This case report demonstrates the successful standalone ayurvedic management of necrotising wound in an elderly woman who was suggested plastic surgery as the best treatment option.
-
-
Timeline
-
Tabulated Summary
-
Narrative
TITLE OF CASE
Successful Standalone Ayurvedic management of necrotising wound- a case report
Dr Rajnikanth
ABSTRACT
A 70-year-old female patient presented with a non-healing wound in the left flank region with severe pain since 15 days associated with a foul smell. The patient consulted allopathic doctor and the diagnosis was made as Necrotising cellulitis on the left flank. She was advised for plastic surgery for wound management. She was reluctant to go for surgical management and opted for Ayurvedic treatment and approached Dr Rajnikanth for better management of the condition. Based on the previous treatment records and clinical examination, the biomedical diagnosis was made as Necrotising wound and the Ayurveda diagnosis as Nadi/ dushta vrana. The line of treatment followed was Vrana hara cikitsa. The medicines used were indicated in vrana, and visha cikitsa. With 2 months of Ayurvedic treatment, the wound healed completely. Bates- Jensen wound assessment score was 52 before treatment became 16 after treatment. This case report demonstrates the successful standalone ayurvedic management of necrotising wound in an elderly woman who was suggested plastic surgery as the best treatment option.
KEYWORDS
Necrotising, wound, nadi vrana, dusta vrana, case report, standalone, cellulitis
INTRODUCTION
Necrosis is the death of cells in living tissue caused by external factors such as infection, trauma, or toxins. As opposed to apoptosis, which is naturally occurring and often beneficial planned cell death, necrosis is almost always detrimental to the health of the patient and can be fatal. Typically, cells that die as a result of necrosis do not signal nearby phagocytes to ingest said dead cells, which leads to a build up of dead tissue and cell debris.
Diagnosis; Diagnosis; Medical history and clinical evaluation are the 2 main diagnostic criteria. But additional investigations may be recommended to identify the intensity or severity of the wound, or to check for infections.
Symptoms: There are two main types of necrotic tissue present in wounds: eschar and slough. Eschar presents as dry, thick, leathery tissue that is often tan, brown or black. Slough is characterised as being yellow, tan, green or brown in color and may be moist, loose and stringy in appearance.
Causes: Necrosis can be caused by a number of external sources, including injury, infection, cancer, infarction, poisons, and inflammation. Black necrotic tissue is formed when healthy tissue dies and becomes dehydrated, typically as a result of local ischemia. Common causes of ischemia are diabetes or other metabolic disorders, or unrelieved local pressure that compresses soft tissue between a surface and underlying bony prominences (leading to the formation of pressure ulcers).
Treatment: The following precautions can help minimise the risk of developing necrotic wounds in at-risk patients and to minimise complications in patients already exhibiting symptoms:
Maintain moist wound environment to prevent dehydration and desiccation, and promote wound healing.
Treatment of necrosis typically involves two distinct steps. The underlying cause of the necrosis in wounds must be treated before the dead tissue itself can be dealt with. This can mean anything from administering antibiotics or anti-venom to relieving pressure on the wound area to restore perfusion. After the cause has been addressed, the necrotic tissue will need to be removed. Depending on the extent of necrosis, this can mean surgical, mechanical, or enzymatic debridement of the wound, or complete amputation of the affected area.
Prognosis: Depending on the depth of invasion, necrotising soft tissue infections can cause extensive local tissue destruction, tissue necrosis, systemic toxicity, and even death.
A necrotising infection causes patches of tissue to die. These infections are the result of bacteria invading the skin or the tissues under the skin. If untreated, they can cause death in a matter of hours. Fortunately, such infections are very rare. They can quickly spread from the original infection site, so it's important to know the symptoms.
PATIENT INFORMATION
In this case report, a 70-year-old female patient presented with a non-healing wound in the left flank region with severe pain since 15 days associated with a foul smell. The patient consulted allopathic doctor and the diagnosis was made as Necrotising cellulitis on the left flank. She was advised for plastic surgery for wound management. She was reluctant to go for surgical management and opted for Ayurvedic treatment and approached Dr Rajnikanth for better management of the condition. Based on the previous treatment records and clinical examination, the biomedical diagnosis was made as Necrotising wound and the Ayurvedic diagnosis as Nadi/ dushta vrana.
No relevant family/genetic/surgical or psychosocial history.
CLINICAL FINDINGS
General examination
Patient is in a drowsy state
Clinical FindingsWound examination was done
-- large blackish-coloured patch on the left gluteal region
-- redness surrounding the patch
-- no sensation
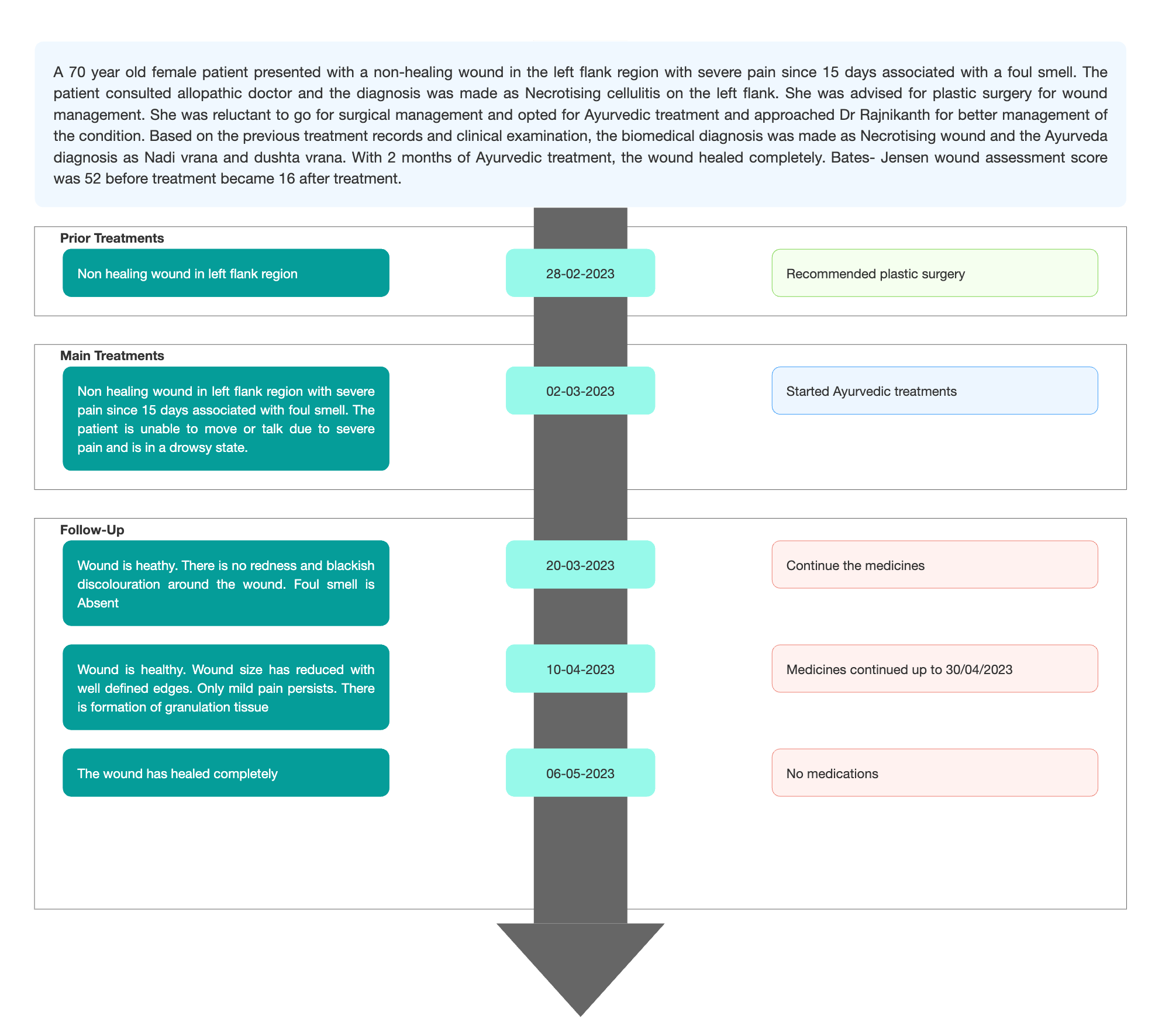
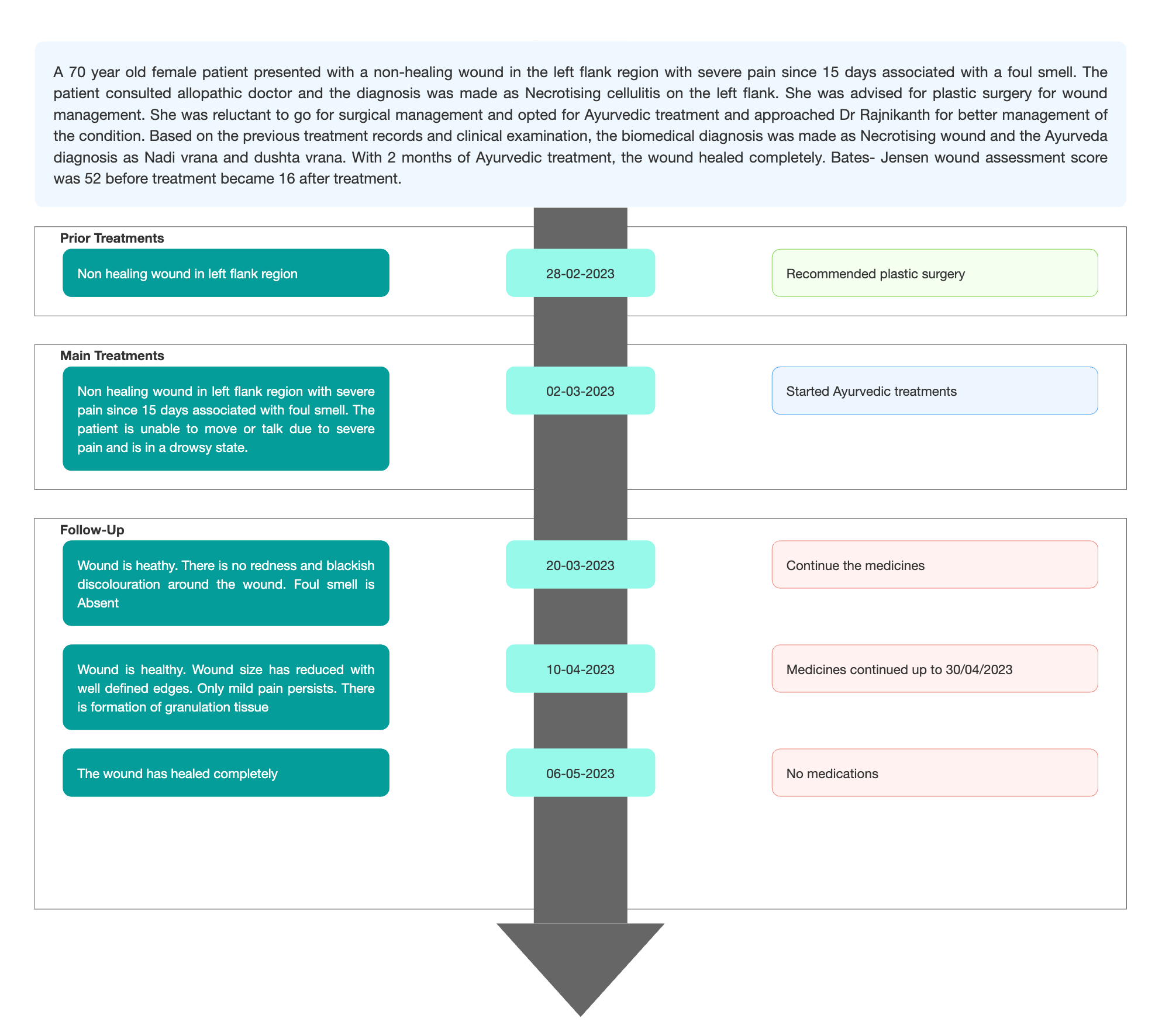
TIMELINE
Image 1. Timeline of events added below
DIAGNOSTIC ASSESSMENT
Modern Diagnostic parameter; Based on the clinical examination and previous treatment records, the biomedical diagnosis was made by the treating physician as Necrotising wound.
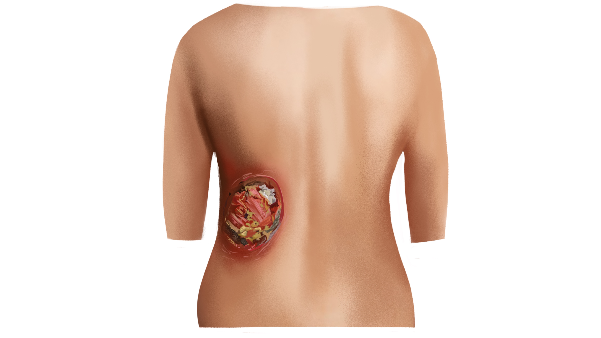
Image 2. Image of the wound taken at baseline dated 2.3.2023
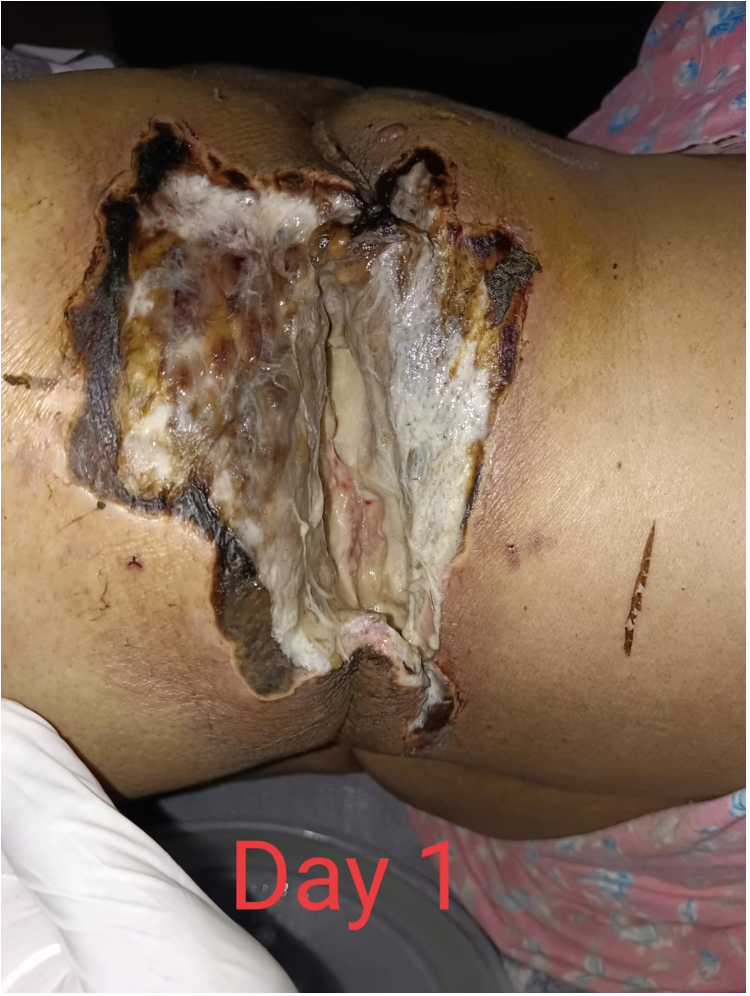
Image 3. Diagnosis proof document at baseline

Ayurvedic Assessment was done based on the presenting complaints and clinical evaluation. The treating physician confirmed the Ayurvedic diagnosis as Dushta vrana/Nadi vrana.
Differential Diagnosis-
Pressure ulcers
diabetic ulcers
Ischemic ulcers
Venous ulcersCellulitis
Superficial abscesses
Pyoderma gangrenosum
Arterial insufficiency and compartment syndrome.
Based on the previous treatment records and clinical findings, the condition is diagnosed as necrotising wound.Prognosis- Depending on the depth of invasion, necrotising soft tissue infections can cause extensive local tissue destruction, tissue necrosis, systemic toxicity, and even death. A necrotising infection causes patches of tissue to die. These infections are the result of bacteria invading the skin or the tissues under the skin. If untreated, they can cause death in a matter of hours. Fortunately, such infections are very rare. They can quickly spread from the original infection site, so it's important to know the symptoms. The patient had been suffering from the wound since 15 days. Her condition was diagnosed as a necrotizing wound and she was recommended plastic surgery by the allopathic physician. Necrotising wounds typically result in a prolonged recovery and functional deficits. In this case, with standalone ayurveda treatment the patient attained a complete recovery in 2 months.
THERAPEUTIC INTERVENTION
Refer the tab ‘Treatment’ in the Portal.
FOLLOW-UP AND OUTCOMES
The patient had 3 follow ups in total. Each follow up, the wound was assessed and documented.
Subjective parameters: Photographs of the wound were taken throughout the treatment.
Image 4. Photographs of the wound taken throughout the treatment
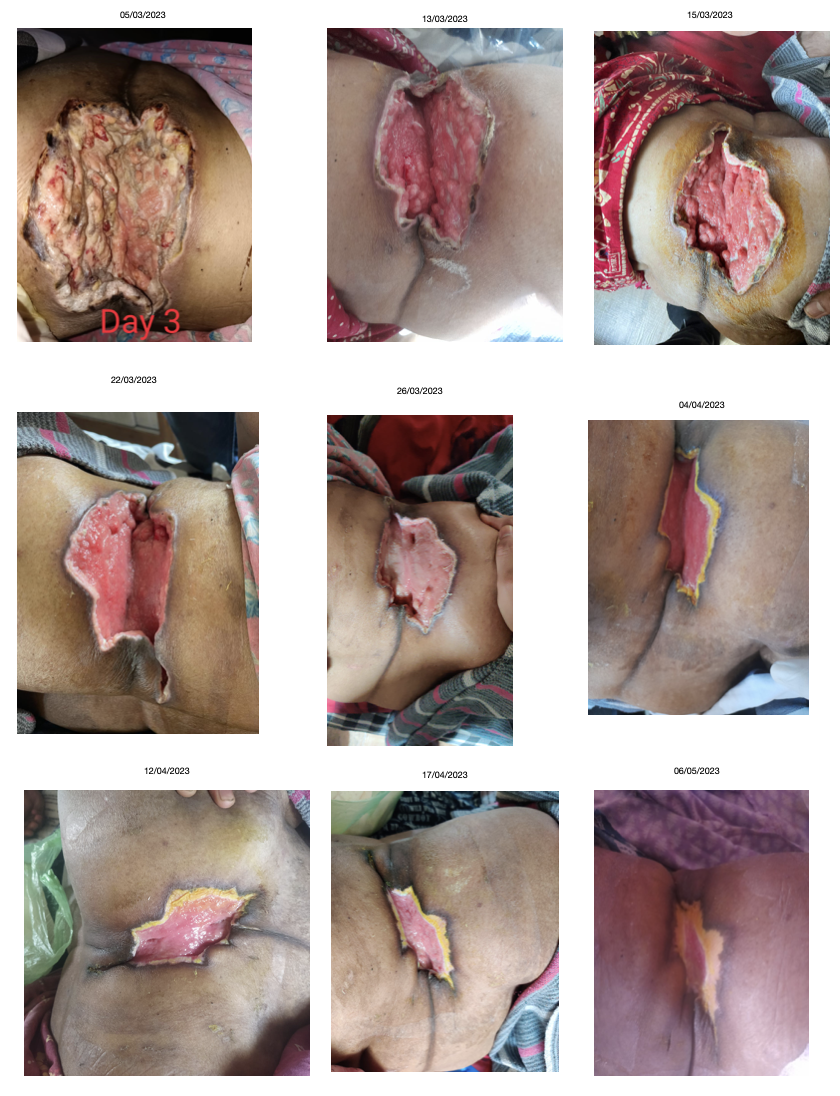
Clinician-based assessment; Wound examination and photographs were taken in each follow-up. The patient was in a drowsy state due to pain before treatment. After 4 days of treatment, her drowsiness was relieved. After 2 weeks of treatment, the wound became healthy. There was no foul smell, red or blackish discolouration around the wound. With 2 months of Ayurvedic treatment, the wound healed completely. Bates- Jensen wound assessment score was 52 before treatment became 16 after treatment.
Image 5. Bates Jensen Wound Assessment score at baseline and endpoint

The wound assessment score at baseline was 52, and it became 16 at endpoint
Intervention adherence and tolerability – The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment- Subjective and objective parameters were the main assessment tools.
Adverse and unanticipated events; None reported
DISCUSSION:
The patient had been suffering from the wound since 15 days. Her condition was diagnosed as a necrotising wound and she was recommended plastic surgery by the allopathic physician. Necrotising wounds typically result in a prolonged recovery and functional deficits. In this case report, the ayurvedic diagnosis was Dushta vrana- Nadi vrana. The line of treatment mainly followed was Vrana cikitsa. The wound healed completely with 2 months of treatment.
PATIENT’S PERSPECTIVE
Not available.
LEARNING POINTS/TAKE HOME MESSAGES
This case underscores the effectiveness of Ayurveda in successfully treating a necrotising wound, which was recommended for plastic surgery under standard of care. The patient experienced full recovery and improved quality of life through Ayurvedic treatment.
INFORMED CONSENT
Written consent obtained from patient for publishing of the case report in the Portal
ACKNOWLEDGEMENTS
None
CONFLICT OF INTEREST
None declared.
FUNDING
None
REFERENCE
1. https://www.woundsource.com/patientcondition/necrotic-wounds
-
Immersive Learning
-
Modern Diagnosis
MODERN DIAGNOSIS: Necrotising wound
ABOUT THE DISEASE:
Necrosis is the death of cells in living tissue caused by external factors such as infection, trauma, or toxins. As opposed to apoptosis, which is naturally occurring and often beneficial planned cell death, necrosis is almost always detrimental to the health of the patient and can be fatal. Typically, cells that die as a result of necrosis do not signal nearby phagocytes to ingest said dead cells, which leads to a build up of dead tissue and cell debris.
Diagnosis; Medical history and clinical evaluation are the 2 main diagnostic criteria. But additional investigations may be recommended to identify the intensity or severity of the wound, or to check for infections.
In this case report, a 70-year-old female patient presented with a non-healing wound in the left flank region with severe pain since 15 days associated with a foul smell. The patient consulted allopathic doctor and the diagnosis was made as Necrotising cellulitis on the left flank. She was advised for plastic surgery for wound management. She was reluctant to go for surgical management and opted for Ayurvedic treatment and approached Dr Rajnikanth for better management of the condition. Based on the previous treatment records and clinical examination, the biomedical diagnosis was made as Necrotising wound and the Ayurvedic diagnosis as Nadi/ dushta vrana.
Symptoms: There are two main types of necrotic tissue present in wounds: eschar and slough. Eschar presents as dry, thick, leathery tissue that is often tan, brown or black. Slough is characterised as being yellow, tan, green or brown in color and may be moist, loose and stringy in appearance.
Causes: Necrosis can be caused by a number of external sources, including injury, infection, cancer, infarction, poisons, and inflammation. Black necrotic tissue is formed when healthy tissue dies and becomes dehydrated, typically as a result of local ischemia. Common causes of ischemia are diabetes or other metabolic disorders, or unrelieved local pressure that compresses soft tissue between a surface and underlying bony prominences (leading to the formation of pressure ulcers).
Image 1. Image of the wound taken at baseline dated 2.3.2023

Image 2. Diagnosis proof document at baseline

Image 3. Bates- Jensen wound assessment score at baseline
Treatment: The following precautions can help minimise the risk of developing necrotic wounds in at-risk patients and to minimise complications in patients already exhibiting symptoms:
Maintain moist wound environment to prevent dehydration and desiccation, and promote wound healing.
Treatment of necrosis typically involves two distinct steps. The underlying cause of the necrosis in wounds must be treated before the dead tissue itself can be dealt with. This can mean anything from administering antibiotics or anti-venom to relieving pressure on the wound area to restore perfusion. After the cause has been addressed, the necrotic tissue will need to be removed. Depending on the extent of necrosis, this can mean surgical, mechanical, or enzymatic debridement of the wound, or complete amputation of the affected area.
Prognosis: Depending on the depth of invasion, necrotising soft tissue infections can cause extensive local tissue destruction, tissue necrosis, systemic toxicity, and even death.
A necrotising infection causes patches of tissue to die. These infections are the result of bacteria invading the skin or the tissues under the skin. If untreated, they can cause death in a matter of hours. Fortunately, such infections are very rare. They can quickly spread from the original infection site, so it's important to know the symptoms.
Reference
-
Ayurveda Diagnosis
AYURVEDA DIAGNOSIS: Dushta vrana- Nadi vrana
ABOUT THE DISEASE:
There are two disease entities mentioned in this case report as the Biomedical diagnosis Necrotising wound cannot be directly correlated to any specific condition in the classical textbooks of Ayurveda. Necrotising wound has been explained as Dushta Vrana and Nadi Vrana.
In this case report, a 70-year-old female patient presented with a non-healing wound in the left flank region with severe pain since 15 days associated with a foul smell. The patient consulted allopathic doctor and the diagnosis was made as Necrotising cellulitis on the left flank. She was advised for plastic surgery for wound management. She was reluctant to go for surgical management and opted for Ayurvedic treatment and approached Dr Rajnikanth for better management of the condition. Based on the previous treatment records and clinical examination, the biomedical diagnosis was made as Necrotising wound and the Ayurveda diagnosis as Nadi/ dushta vrana.
ABOUT VRANA
The definition of Vrana is:
व्रण गात्र विचूर्णने व्रणयति इति व्रणह….(AH.Utt.25.22)
There is a destruction, break, rupture or discontinuity in the body tissue, it is called as Vrana.
वृणोति यस्मात् रूढे'अपि व्रनवस्तु न नश्यति ।आदेह धारणात्तस्मत्व्रणैत्युच्च्यते ॥
Susruta explains Vrana as that which retains the scar even after complete healing of the wound, and the imprint remains the entire life. (Su.Ci.1.6)
DUSHTA VRANA
दोषैरधिष्ठितो दुष्टः…..
When it becomes the seat of the vitiated dosa then it is called as Dushta Vrana.
In Dushta Vrana, there is severe pain, profuse discharge having putrified smell, and irregular base and margin.
पूतिगन्धान् विवर्णाञ्च बहुस्रावान्महारुजः॥८३॥
Dushta Vrana is difficult to heal and heals very slowly in spite of the best efforts by Cikitsa Chatuspada.
Lakshanas of Dushta Vrana
तत्रातिसंवृतोऽतिविवृतोऽतिकठिनोऽतिमृदुरुत्सन्नोऽवसन्नोऽतिशीतोऽत्युष्णः
नगन्धात्यर्थदाहपाकरागवेदनावानिति पित्तेन, शेषाः कफेन; उन्मार्गी मुखात् मुखान्तरवान्, उत्सङ्गः कोटरः’ इति चक्रः; कृष्णरक्तपीतशुक्लादीनांवर्णानामन्यतमवर्णो भैरवः पूतिपूयमांससिरास्नायुप्रभृतिभिः पूर्णःपूतिपूयास्राव्युन्मार्ग्युत्सङ्ग्यमनोज्ञदर्शनगन्धोऽत्यर्थंवेदनावान्दाहपाकरागकण्डूशोफपिडकोपद्रुतोऽत्यर्थं दुष्टशोणितास्रावी दीर्घकालानुबन्धी चेतिदुष्टव्रणलिङ्गानि | (Su.Su 22/7)Management of Vrana
Treatment varies depending on the type of vrana and the management is given till the complete removal of scar tissue. In the treatment of nija vrana, i.e., those ulcers which recur due to aggravation of doshas, Sushruta explained the 60 upakrama, Charaka explained 36 upakrama and Vagbhata mentioned 26 upakramas. Seven modalities of Vrana Vimlapana, Avasecana, Upanaha, Patana kriya, Shodhana, Ropana, Vaikritapaham are explained by Acarya Sushruta. Sapta upkrama are a principal line of treatment which is explained in detail as Shashti upakrama.
NADI VRANA:
नाडी नालश्च ।।
Nadi refers to Srotas, according to Amarakosha.नाडी संलर्गनो व्रणः || (Shabdakalpadruma)
Nadi Vrana is the ulcer having a track. “Nadi’ refers to the channel of the abscess, and ‘vrana’ refers to the ulcer cause. Fistula in ano can also be included under Nadi Vrana (though Bhagandara is a name given for Ayurvedic term correlated with anal fistula).
Causes: Causes of Nadi vrana:
Shopha upeksha – Due to the miss-diagnosis from the part of physician, when a formed and ripe pus cavity or abscess or swelling is considered to be unripe one and neglected or when pus filled wounds or ulcers are neglected, the pus (infected and contaminated material) on not finding the exit, traverses in a reverse direction and penetrates the deeper tissues and organs. The pus makes its own tract to travel deep into the body and the tract or pathway through which the pus travels deep into the tissues is called Nadi. The ulcers causing such nadi are called Nadi Vranas. These are compared to Sinus explained in modern science.
Types (According to Sushruta) –
Vataja Nadi – Sinus associated with vitiated Vata: rough on touch, narrow opening and associated with pain, foamy discharges at night
Pittaja Nadivran – Sinus associated with vitiated Pitta: associated with thirst, rise in body temperature, pricking pain, body fatigue, fever and splitting pain, hot and yellow discharges during day time
Kaphaja Nadivranam – Sinus associated with vitiated Kapha: hard, itchy, associated with mild pain, thick, viscous, white coloured unctous discharges during day time
Vata-Pittaja Nadi – Sinus associated with vitiated Vata and pitta: presents with mixed symptoms of Vataja and Pittaja Nadi
Pitta-Kaphaja Nadi – Sinus associated with vitiated Pitta and Kapha: presents with mixed symptoms of Pittaja and Kaphaja Nadi
Kapha-Vataja Nadi – Sinus associated with vitiated Kapha and Vata: presents with mixed symptoms of Kaphaja and Vataja Nadi
Tridoshaja Nadi – Sinus caused or associated with vitiation of all 3 doshas: presents with burning sensation, fever, dyspnoea, fainting, dryness of mouth and other mixed symptoms of vitiation of all 3 doshas. This is a dangerous and life threatening condition which had crossed the limitations of treatment.
Shalya janya nadi – Sinus caused due to foreign substances is called shalya janya nadi. In Shalyaja Nadi Vrana, hair can be considered as shalya (Foreign body) because hair follicles have never been demonstrated in the walls of the sinus. The hairs projecting from the sinus are dead hairs, with their painted ends directed towards the blind end of the sinus. While describing the “shalya” Acharya Sushruta has
Treatment: This primarily depends upon the type of Nadi Vrana. Basically, the Nadi has to be cut open and then medicines to initiate the healing have to be administered either internally or externally. Acharya Sushruta has mentioned Nadi Vrana in Chhedya & Bhedya Vyadhi. In chikitsa sthana he mentioned vidarana karma which indicates to chhedana and bhedana karma.
Treatment rationale: As the Ayurvedic diagnosis is a combination of 2 disease conditions namely dushta and nadi vrana, the basic chikitsa sutra followed was Vrana cikitsa. Tab kaishora guggulu is indicated in nadi vrana, Tab shiva gulika was given for rasayana and avrana cikitsartham, vyadhiharan rasa is indiacted for dushta vrana, Shirisha panchanga ghrita was given to nullify the effect of visha.
Reference
- Vagabhata, Astangasangraha, Atridev Gupta,Krishnadas Academy, Varanasi UP Ed., 1993; 846:225.35.
- Madhavakara, Madhavanidan With MadhukoshaCommentary By Vijayarakshita And Srikant Data,Vinal Madhukar Hindi Commentary By Dr.Brahmanand Tripathi Choukhamba SanskritSansthan, Varanasi, 520:
- Traditional and contemporary appraisal of dushta vrana w.s.r to venous ulcers. Available from: https://www.researchgate.net/publication/324156242_traditional_and_contemporary_appraisal_of_dushta_vrana_wsr_to_venous_ulcers#fulltextfilecontent [accessed apr 01 2023].
- https://www.easyayurveda.com/2017/03/06/nadivrana-sinus-ayurvedic-treatment/
5. Sushruta Samhita -Vol I & II Ayuveda Tatwasandipika by AmbikaDutta Shastri, Chaukhamba Subharti Prakshan.
6. Sushruta Samhita -Vol I-II translated by Prof.K.R.Srikantha Murthy, Chaukhambha orientelia.
-
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Tab Kaishora guggulu Tablet 2-2-2 Oral, with warm water before food 2023-03-02 - 2023-04-30 Sharangdhara Samhita Madhyama Khanda 7. 70-81 Tab Shiva gulika Tablet 1-1-1 Oral, with warm water after food 2023-03-02 - 2023-04-30 Bhaishajya Ratnavali. Rasayana Prakarana. 73.151-173 Vyadhiharan rasa Curna 2 gms/15 days Oral 2023-03-02 - 2023-04-30 Ayurvedic Patent & Proprietary Medicine Shirisha panchanga ghrita Ghrta 5 gms Oral, twice daily 2023-03-02 - 2023-04-30 Ayurvedic Patent & Proprietary Medicine Panca valkala kwatha Kvatha Required quantity Vrana prakshalana, twice a day 2023-03-02 - 2023-04-30 Sahasrayogam. Kashaya prakarana Nimba, Khadira, Shirisha and Vidanga Curna Required quantity Vrana dhoopna twice daily 2023-03-02 - 2023-04-30 Nimba churna- Bhaishajya Ratnavali Vatarakta adhikara 31-38?Khadira churna- Bhavaprakasha nighantu Vatadi varga?Shirisha churna- Bhavaprakasha nighantu Asanadi varga?Vidanga churna- Bhavaprakasha nighantu Haritakyadi varga WH5 gel Ointment Required quantity Vrana lepana 2023-03-02 - 2023-04-30 Ayurvedic Patent & Proprietary Medicine -
Outcome Measures
OUTCOME MEASURES
In this case report, a 70-year-old female patient presented with a non-healing wound in the left flank region with severe pain since 15 days associated with a foul smell. The patient consulted allopathic doctor and the diagnosis was made as Necrotising cellulitis on the left flank. She was advised for plastic surgery for wound management. She was reluctant to go for surgical management and opted for Ayurvedic treatment and approached Dr Rajnikanth for better management of the condition. Based on the previous treatment records and clinical examination, the biomedical diagnosis was made as Necrotising wound and the Ayurvedic diagnosis as Nadi/ dushta vrana.
Assessment: Subjective and objective parameters were assessed to analyse the outcome of the treatment.
Subjective parameters: The changes observed in the symptoms were noted date wise, and tabulated.
Table 1. Symptoms tabulated throughout the treatment
DATE
WOUND ASSESSED
20/3/2023
Wound- heathy
No redness and blackish discolouration around the wound
Foul smell- Absent10/4/2023
Wound - healthy, granulation tissue formation
Wound size- reduced, well defined edges
Pain - Mild06/05/23
Wound healed completely
Objective parameters:
Images were taken throughout the treatment and documented date wise.
Image 1.Images taken throughout the treatment date wise.

Bates- Jensen Wound assessment score was documented at baseline and endpoint. The value was 52 at baseline that reduced to 16 at endpoint, indicating that the wound regeneration is happening.
Image 2. Bates- Jensen wound assessment score sheet

-






