Featured Case
-
Abstract
A 28-year-old female patient, presented with a three-month history of papules, pustules, redness, black spots, and overall dull skin on her forehead. She had tried Ayurvedic medicines for 15 days followed by Allopathic treatment for 10 days. But the symptoms persisted and so she opted for a second ayurvedic consultation. She consulted Dr Sushma, for better ayurvedic management. Based on clinical evaluation, the biomedical diagnosis was made as Acne vulgaris and the Ayurvedic diagnosis as Mukhadooshika. The line of treatment followed was to pacify the dushta rakta and pitta. Tvacya and dipana dravyas were included to address the condition. After 1 month- Papules healed, Redness absent, Dull skin on forehead- resolved. After 2 months- Black spots only a mild presentation persisted. After 3 months, there was complete relief from symptoms.
This case report demonstrates the successful standalone ayurvedic management of acne vulgaris, who did not get satisfactory response with conventional medicines.
-
Summaries
-
Listen
-
Watch
-
View
-
Read
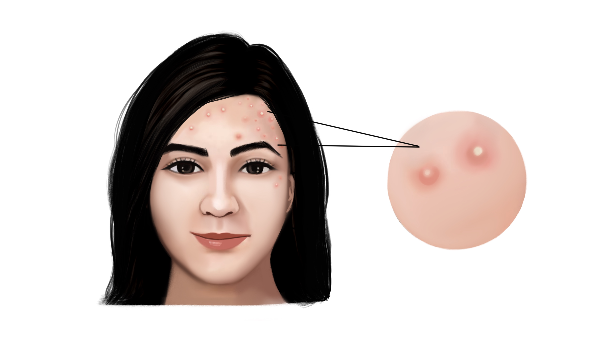
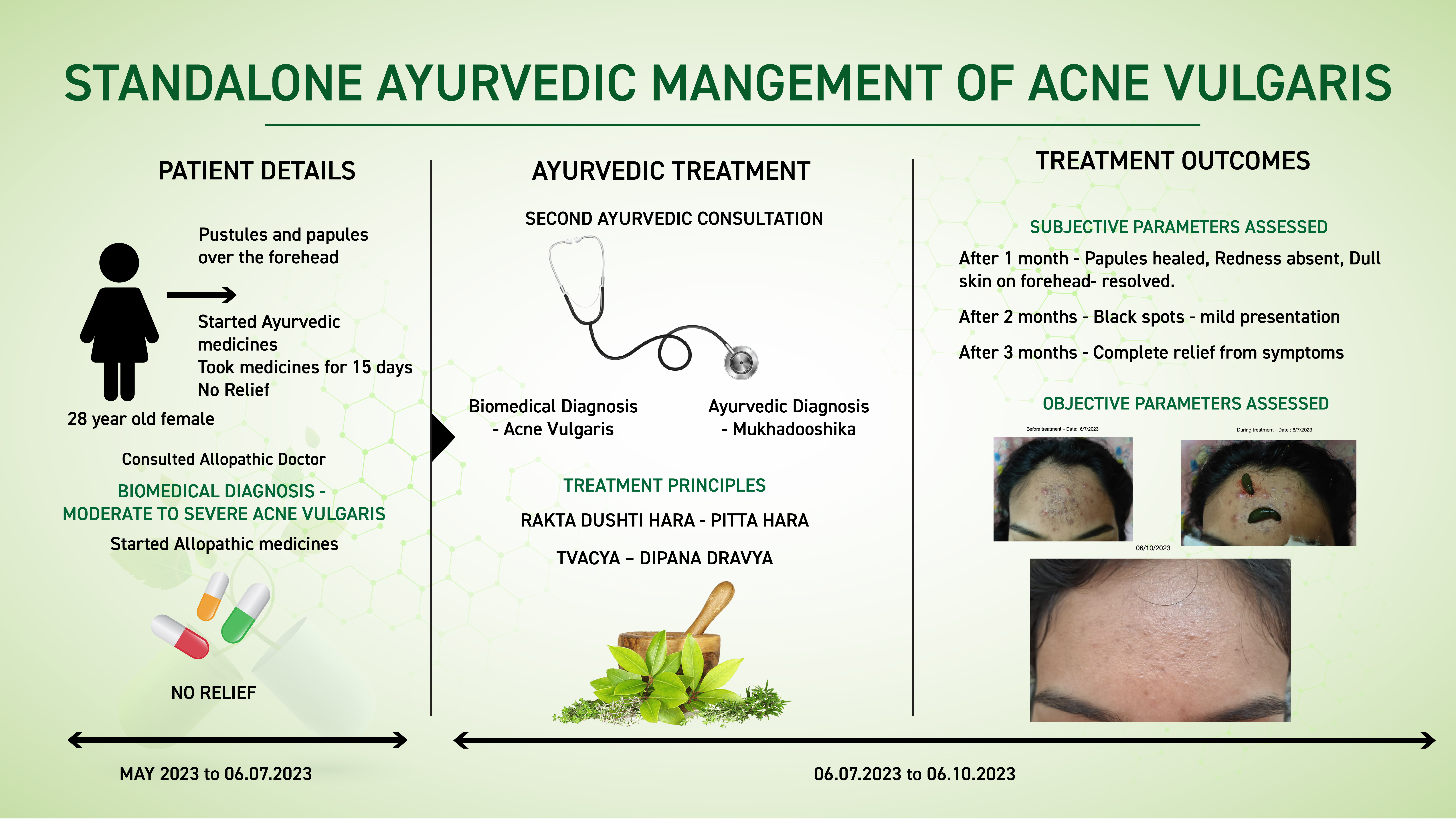
A 28-year-old female patient, presented with a three-month history of papules, pustules, redness, black spots, and overall dull skin on her forehead. She had tried Ayurvedic medicines for 15 days followed by Allopathic treatment for 10 days. But the symptoms persisted and so she opted for a second ayurvedic consultation. She consulted Dr Sushma, for better ayurvedic management. Based on clinical evaluation, the biomedical diagnosis was made as Acne vulgaris and the Ayurvedic diagnosis as Mukhadooshika. The line of treatment followed was to pacify the dushta rakta and pitta. Tvacya and dipana dravyas were included to address the condition. After 1 month- Papules healed, Redness absent, Dull skin on forehead- resolved. After 2 months- Black spots only a mild presentation persisted. After 3 months, there was complete relief from symptoms.
This case report demonstrates the successful standalone ayurvedic management of acne vulgaris, who did not get satisfactory response with conventional medicines.
-
-
Timeline
-
Tabulated Summary
-
Narrative
TITLE OF CASE
Standalone successful Ayurvedic management of Acne Vulgaris- a case report
Dr Sushma NS
ABSTRACT
A 28-year-old female patient, presented with a three-month history of papules, pustules, redness, black spots, and overall dull skin on her forehead. She had tried Ayurvedic medicines for 15 days followed by Allopathic treatment for 10 days. But the symptoms persisted and so she opted for a second ayurvedic consultation. She consulted Dr Sushma, for better ayurvedic management. Based on clinical evaluation, the biomedical diagnosis was made as Acne vulgaris and the Ayurvedic diagnosis as Mukhadooshika. The line of treatment followed was to pacify the dushta rakta and pitta. Tvacya and dipana dravyas were included to address the condition. After 1 month- Papules healed, Redness absent, Dull skin on forehead- resolved. After 2 months- Black spots only a mild presentation persisted. After 3 months, there was complete relief from symptoms.
This case report demonstrates the successful standalone ayurvedic management of acne vulgaris, who did not get satisfactory response with conventional medicines.
KEYWORDS
Mukhadooshika, Acne vulgaris, Ayurveda, Case report, Standalone
INTRODUCTION
Acne, or acne vulgaris, is a common skin condition that develops when dead skin cells, sebum (skin oil), and bacteria plug the pores, leading to skin lesions commonly known as pimples or zits. Acne outbreaks can develop on the face, back, shoulders, and chest. A range of acne treatments—from over-the-counter products to prescription medications to specialist procedures—can help clear the skin and prevent scarring. The specific treatment depends on the type and severity of acne.
Types of Acne Vulgaris; There are several types of acne. They have similar causes but vary in appearance and severity. The different types of acne include White heads, Black heads, Pustules and Papules, Nodules and cysts.
Symptoms-
- Small, red bumps
- Small, red bumps containing yellow or white pus
- Whiteheads
- Blackheads
- Crusting over the bumps
- Redness and swelling on the skin surrounding the blemishes
- Pain or tenderness, especially with cysts and nodules
Risk Factors: Age, hormonal changes, diet, skin type, family history, personal care products, medication and smoking can cause acne.
Diagnostic criteria: Medical history, clinical evaluation are the basic diagnostic criteria. Tests may be suggested if the doctor suspects any underlying medical condition.
Treatment options & prognosis; There are many treatment options for acne. Treatment can help control acne breakouts and may prevent long-term scarring. Your healthcare provider can recommend specific treatments based on the severity of your acne. This may include topical treatments applied to the skin, oral prescription medications, or procedures performed as an out patient. Dermatological procedures can address stubborn or severe acne. This might include laser therapy and corticosteroid injections. Laser therapy and light devices, when combined with other acne treatments, can reduce inflammation, clear acne, and help prevent scarring. Corticosteroid injections work quickly to reduce pain and inflammation. The injections help treat severe acne breakouts that are causing painful cysts and nodules. However, if acne are not managed well, it can cause complications like scarring, hyper pigmentation, infections and emotional distress.
PATIENT INFORMATION
In this case report, a 28-year-old female patient, presented with a three-month history of papules, pustules, redness, black spots, and overall dull skin on her forehead. She had tried Ayurvedic medicines for a month and Allopathic treatment for 10 days. But the symptoms persisted and so she opted for a second ayurvedic consultation. She consulted Dr Sushma, who made the biomedical diagnosis as Acne vulgaris and the Ayurvedic diagnosis as Mukhadooshika.
No relevant family, genetic, psychosocial or surgical history.
CLINICAL FINDINGS
General examination was done. Soft tissue enlargement with swelling (appr. 1x 1 cm)
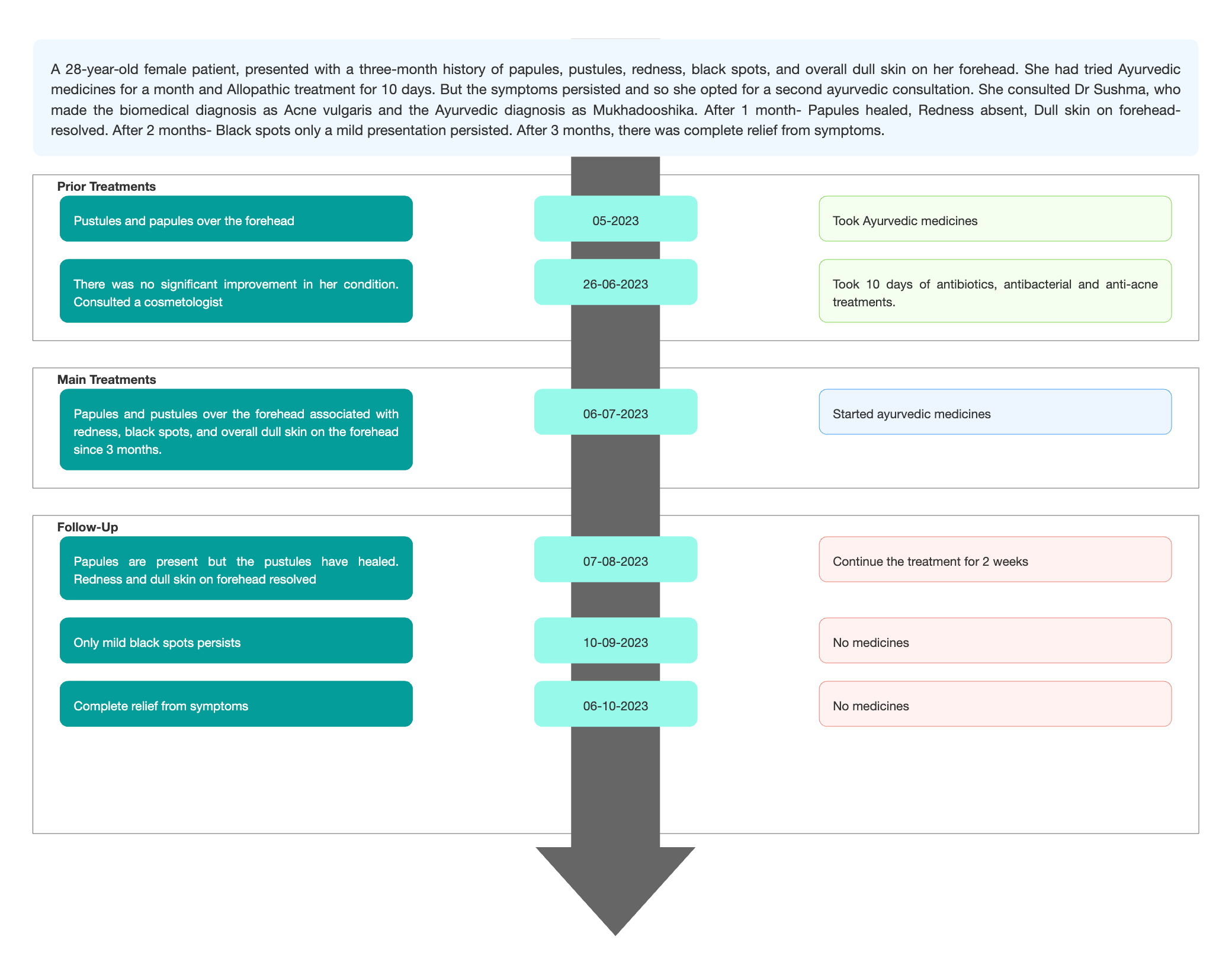
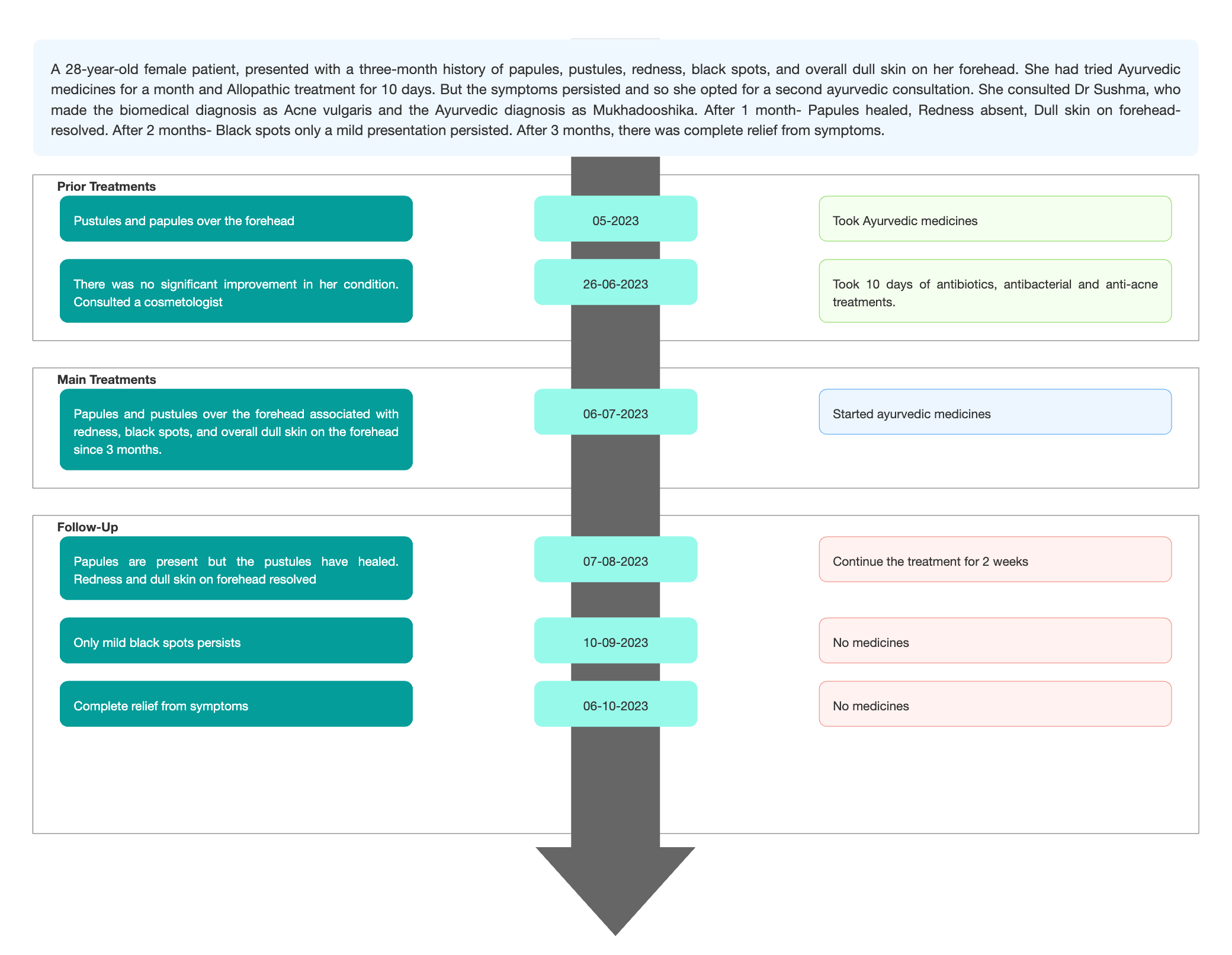
TIMELINE
Image 1. Timeline of events added below
DIAGNOSTIC ASSESSMENT
Modern Diagnostic parameter; Based on the medical history and clinical evaluation, the biomedical diagnosis was made as Acne vulgaris.
Image 2. Image of the symptom taken at baseline
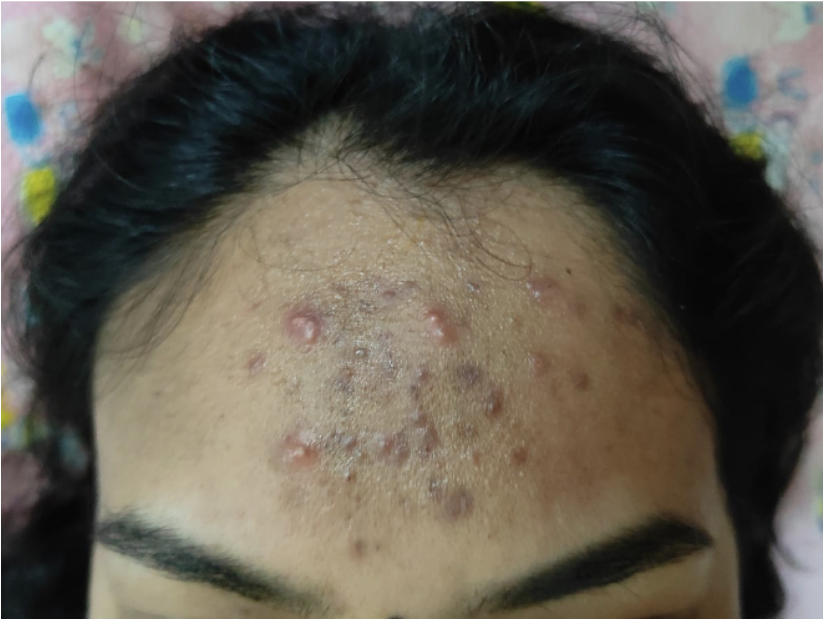
Ayurvedic Assessment was done based on the presenting complaints, and clinical evaluation and the diagnosis was confirmed as Mukhadooshika.
Differential Diagnosis- Cellulitis, rosacea, perioral dermatitis, necrotising fasciitis.
Based on the physical examination and previous treatment history this condition was diagnosed as Acne Vulgaris
Prognosis & Treatment available: The overall prognosis of acne is generally good with appropriate treatment. In this case report, the patient presented with pustules and papules over the forehead with occasional discharge since 3 months. The condition persisted in spite of taking both Ayurvedic and Allopathic treatments including antibiotic tablets, and antibacterial and anti-acne creams. But with 3 months of Ayurvedic treatment as prescribed by Dr Sushma, the patient was relieved from all the symptoms.
THERAPEUTIC INTERVENTION
Please refer the tab ‘Treatment’ in the Portal.
FOLLOW-UP AND OUTCOMES
Both objective and subjective parameters were assessed to analyse the outcome of the ayurvedic treatment.
Subjective parameters: The symptoms were assessed through out the treatment.
Table 1. Date wise assessment of symptoms
Date
Clinical findings
Papules
Pustules
Redness
Black spots
Dull skin on the forehead
7/8/23
+
Cured
Cured
++
Cured
10/9/23
Cured
Cured
Cured
+
Cured
6/10/23
Cured
Cured
Cured
Cured
Cured
Objective parameters: Images were taken through out the treatment, and documented to assess the changes.
Image 1. Jalaukavacaranam dated 6.7.2023
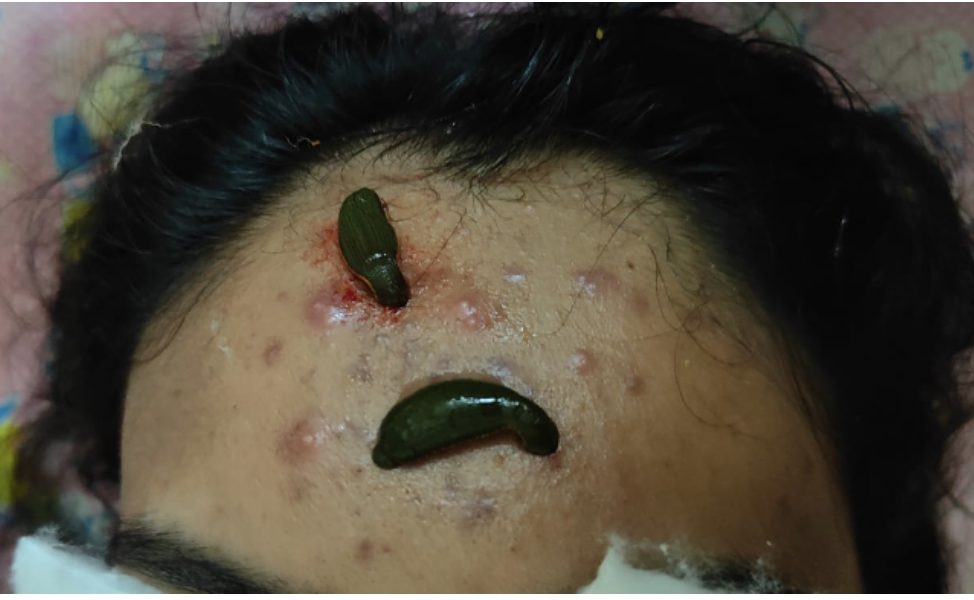
Image 2. Image dated 7.8.2023
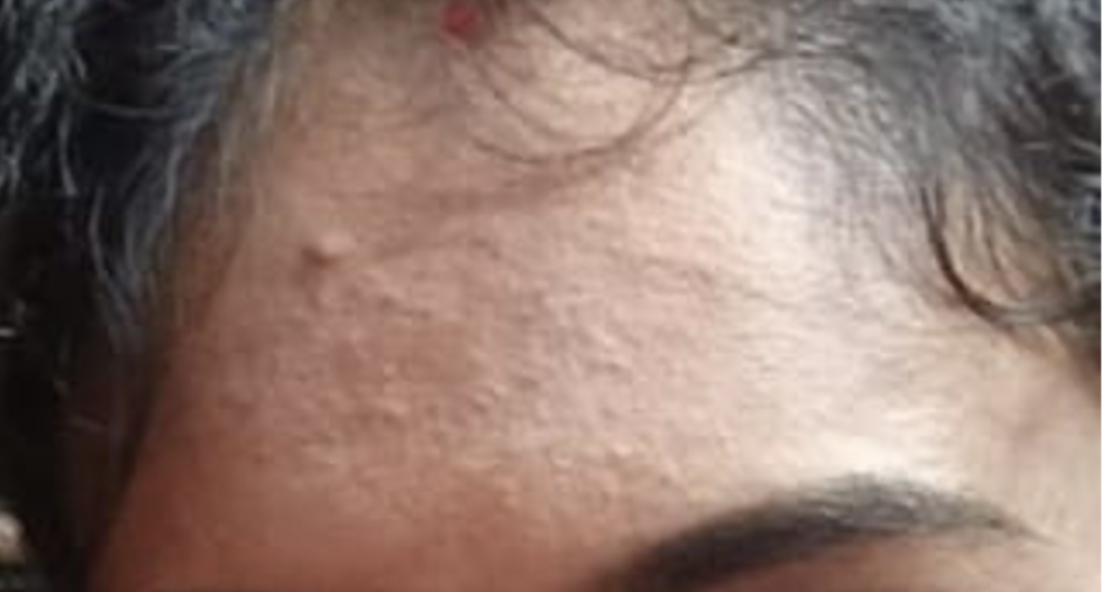
Image 3. Image dated 10.9.2023
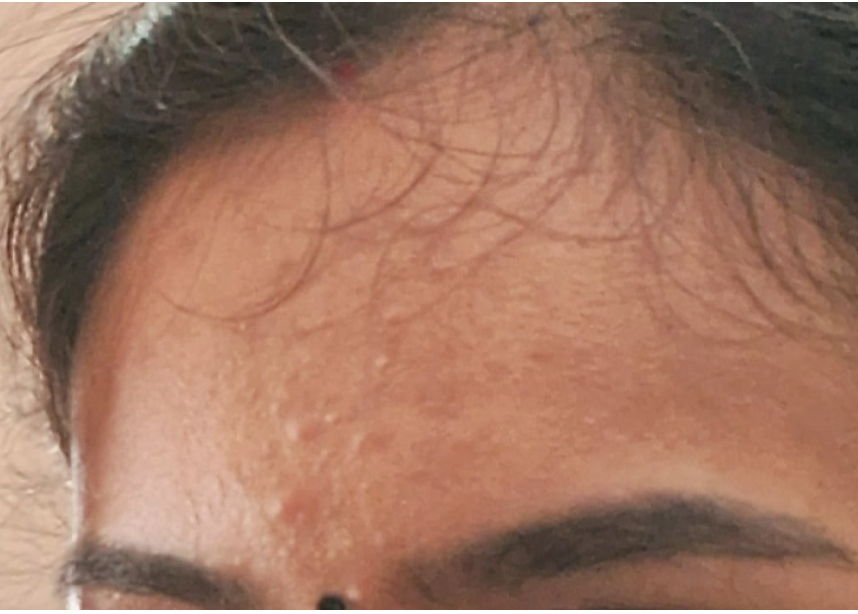
Image 4. Image at endpoint dated 6.10.2023
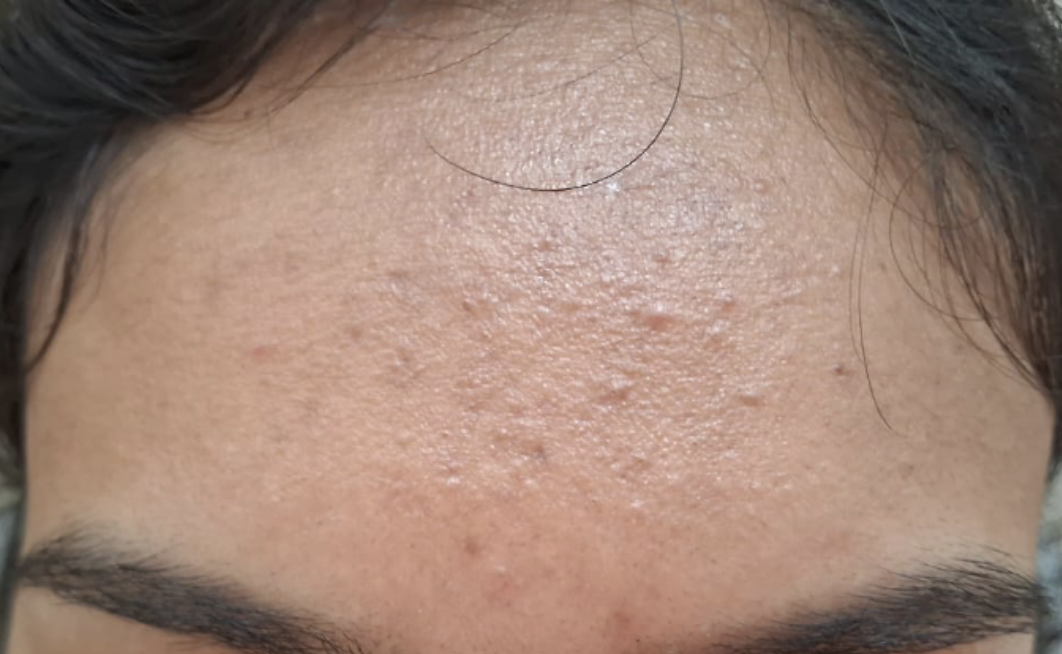
Clinician-based assessment; After 1 month- Papules healed, Redness absent, Dull skin on forehead- resolved. After 2 months- Black spots only a mild presentation persisted. After 3 months, there was complete relief from symptoms.
Patient-assessed; Not relevant
Intervention adherence and tolerability – The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment- By monitoring the patient.
Adverse and unanticipated events; None reported
DISCUSSION ;
The patient had tried ayurvedic medicines for a period of 1 month, but the symptoms persisted. She then tried antibiotics and anti-bacterial and anti-acne creams for 10 days, but there was no relief. But on following Dr Sushma’s prescription, she got complete relief from the symptoms. The treatments targeted at pacifying rakta dushti and vitiated pitta. Tvacya and dipana dravya were selected specifically to address the condition.
PATIENT’S PERSPECTIVE
Not available.
LEARNING POINTS/TAKE HOME MESSAGES
This case highlights the effectiveness of Ayurvedic treatment for acne vulgaris, as the patient, who had been struggling with the condition for three months without any relief from biomedical treatments, experienced positive results.
INFORMED CONSENT
Written consent obtained from patient for publishing of the case report in the Portal
ACKNOWLEDGEMENTS
None specified
CONFLICT OF INTEREST
None declared.
FUNDING
None
REFERENCE
-
Immersive Learning
-
Modern Diagnosis
BIOMEDICAL DIAGNOSIS: Acne vulgaris
ABOUT THE DISEASE:
Acne, or acne vulgaris, is a common skin condition that develops when dead skin cells, sebum (skin oil), and bacteria plug the pores, leading to skin lesions commonly known as pimples or zits. Acne outbreaks can develop on the face, back, shoulders, and chest. A range of acne treatments—from over-the-counter products to prescription medications to specialist procedures—can help clear the skin and prevent scarring. The specific treatment depends on the type and severity of acne.
Types of Acne Vulgaris; There are several types of acne. They have similar causes but vary in appearance and severity. The different types of acne include White heads, Black heads, Pustules and Papules, Nodules and cysts.
Symptoms-
- Small, red bumps
- Small, red bumps containing yellow or white pus
- Whiteheads
- Blackheads
- Crusting over the bumps
- Redness and swelling on the skin surrounding the blemishes
- Pain or tenderness, especially with cysts and nodules
Risk Factors: Age, hormonal changes, diet, skin type, family history, personal care products, medication and smoking can cause acne.
Diagnostic criteria: Medical history, clinical evaluation are the basic diagnostic criteria. Tests may be suggested if the doctor suspects any underlying medical condition.
Treatment options & prognosis; There are many treatment options for acne. Treatment can help control acne breakouts and may prevent long-term scarring. Your healthcare provider can recommend specific treatments based on the severity of your acne. This may include topical treatments applied to the skin, oral prescription medications, or procedures performed as an out patient. Dermatological procedures can address stubborn or severe acne. This might include laser therapy and corticosteroid injections. Laser therapy and light devices, when combined with other acne treatments, can reduce inflammation, clear acne, and help prevent scarring. Corticosteroid injections work quickly to reduce pain and inflammation. The injections help treat severe acne breakouts that are causing painful cysts and nodules. However, if acne are not managed well, it can cause complications like scarring, hyper pigmentation, infections and emotional distress.
In this case report, a 28-year-old female patient, presented with a three-month history of papules, pustules, redness, black spots, and overall dull skin on her forehead. She had tried Ayurvedic medicines for 15 days followed by Allopathic treatment for 10 days. But the symptoms persisted and so she opted for a second ayurvedic consultation. She consulted Dr Sushma, who made the biomedical diagnosis as Acne vulgaris and the Ayurvedic diagnosis as Mukhadooshika.
Image 1. Baseline image taken of the symptoms

Reference
-
Ayurveda Diagnosis
AYURVEDIC DIAGNOSIS: Mukhadooshika
ABOUT THE DISEASE:
The Biomedical diagnosis in this case report is Acne vulgaris and the ayurvedic correlation given by the treating physician is Mukhadooshika.
In Ayurvedic texts the disease, Mukhadooshika has not been mentioned independently. It has been described with some minor diseases. This group of minor diseases is known as ‘Kshudra roga.’ According to Sushruta, 44 diseases have been described under this group; Mukhadooshika is one of the kshudra roga.
शाल्मलीकण्टकप्रख्याः कफमारुतशोणितैः। जायन्ते पिडका यूनां वक्त्रे या मुखदूषिकाः॥३९॥(SS.Ni.13)
The Shalmali thorn like eruptions on the face of adults due to vitiation of Kapha, Vata and Rakta are known as “Yuvanapidaka” or “Mukhadooshika.” Acharya Vagbhata has mentioned the role of Meda in the pathology of Mukhadooshika which resembles the modern theory of sebum involvement in the pathogenesis of acne.
Causes: The causative factors of acne are mainly divided into 4 types
- Kalaja- Vasanta Ritu, Grishma Ritu, Sharad Ritu, Tarunya
- Aharaja; Excess intake of Katu, Tikta, Amla, Lavana Rasa, Snigdha, Guru, Picchila, Abhishyandi Aharasevana, Ushna Tikshna Ahara.
- Viharaja; Divaswapa, Excess Atapasevana, Ratri jagarana, Vegavarodha.
- Manasika; Atichinta, Atikrodha, Atibhaya, Udvega, Svabhava.
Lakshana of Mukhadooshika:
………..सरुजो घनाः।
मेदोगर्भा मुखे यूनां ताभ्यां च मुखदूषिकाः॥५॥(AH.Utt.31)
- Pidika – means eruption. The disease is in the form of eruptions.
- Saruja – The eruptions are painful. The pain may be mild or acute in nature.
- Ghana – means thick, hard or indurate. So, the eruptions of the disease are hard and thick.
- Medogarbha – The eruptions are impregnated with Meda. Meda is known as comedone.
- Yuna Mukha – This disease occurs on the face of adults.
Samprapti of Mukhadushika
According to Sushruta, the disease Mukhadooshika is due to vitiated Kapha, and Vata dosa and Rakta Dhatu. The exact description about the disease process is not available and the involvement of Pitta Dosa is also not explained in any of the Ayurvedic text. But when Rakta is involved, Pitta will automatically be vitiated, because the aggravating factors for both Rakta and Pitta are similar. According to Acharya Charaka Pitta plays a significant role in the formation of Pidaka. Though Vyaktisthana of the Pidaka is on the skin, involvement of Rasa Dhatu can also be considered here.
Samprapti Ghataka
• Dosha – Kapha, Vata, Rakta
• Dushya – Rasa, Rakta, Meda, Shukra
• Srotas – Svedavaha, Rasavaha, Raktavaha • Mala – Sweda, Tvaka Sneha
• Srotodusti – Sanga, Atipravritti
• Agni – Jatharangimandya
• Udbhavasthana – Amashayasamuttha
• Roga Marga – BahyaCikitsa: Chikitsa of Mukhadushika
Line of treatment prescribed by different Acharya can be summarised as follows.
Sushruta – Vamana, Lepana
Ashtanga Hridaya – Lepana, Vamana, Nasya, ShiravyadhaBhavaprakash - Lepa, Vamana, Abhyanga
Yoga Ratnakara - Siravedha, Pralepa, Abhyanga
Sharangadhara Samhita - Lepa
Bhaishajjya Ratnavali - Siravedha, Pralepa, AbhyangaIn this case report, a 28-year-old female patient, presented with a three-month history of papules, pustules, redness, black spots, and overall dull skin on her forehead. She had tried Ayurvedic medicines for 15 days followed by Allopathic treatment for 10 days. But the symptoms persisted and so she opted for a second ayurvedic consultation. She consulted Dr Sushma, who made the biomedical diagnosis as Acne vulgaris and the Ayurvedic diagnosis as Mukhadooshika.
Rationale of treatment explained by the Physician: The logic of using medicines and their targets as explained is tabulated below.
Table 1. The medicines, therapies and the rationale for choosing them
Name of the medicine/ Procedure
Rationale
Rakta mokshana (Jalauka)
Dusta rakta hara and pitta hara
Trivrit Lehyam
Virechana
Tikthakam kashayam
Pitta hara, Dipana, Tvacya, Dusta rakta hara
Patolakaturohinyadi Kashayam
Indicated in Kapha pitta kushta, jwara, visha, kamala, arochaka
Arogyavardhini vati
Kapha pitta hara, dipana, tvacya
Clarina cream
Kapha pitta hara, dipana, tvacya
Reference
1. Vidhya’Bharti, Sharma et al. A SHORT REVIEW ON MUKHADUSHIKA WITH SPECIAL REFERENCE TO ACNE VULGARIS. Int.J.Res.Ayurveda Pharm.11(3). 2020
-
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Jalaukavacaranam NA Single sitting External application on the affected site 2023-07-06 - 2023-07-06 SS.Su.13.11 Trivrit Lehyam + Draksa Svarasa Samyoga 10 gms lehyam + Required quantity Draksha Svarasa At bedtime 2023-07-09 - 2023-07-09 AH.Ka.2.9 Tiktakam Kashayam Kashayam 15 ml With 45 ml of luke warm water on empty stomach twice daily 2023-07-12 - 2023-07-31 Sahasra yogam - Kashaya Prakarana Patolakaturohinyadi Kashayam Kashayam 15 ml With 45 ml of luke warm water on empty stomach twice daily 2023-07-12 - 2023-07-31 Sahasra yogam - Kashaya Prakarana Arogyavardhini vati Tablet 1 Tablet With warm water after food twice daily 2023-07-12 - 2023-07-27 Rasendrasarasangraha. Jwara Rogadhikara. 13. 105 Clarina cream Ointment Required Quantity External application on the affected site 2023-07-25 - 2023-08-20 Patent and Proprietary Medicine -
Outcome Measures
OUTCOME MEASURES
In this case report, a 28-year-old female patient, presented with a three-month history of papules, pustules, redness, black spots, and overall dull skin on her forehead. She had tried Ayurvedic medicines for 15 days followed by Allopathic treatment for 10 days. But the symptoms persisted and so she opted for a second ayurvedic consultation. She consulted Dr Sushma, who made the biomedical diagnosis as Acne vulgaris and the Ayurvedic diagnosis as Mukhadooshika.
Assessment: Both objective and subjective parameters were assessed to analyse the outcome of the ayurvedic treatment.
Subjective parameters: The symptoms were tabulated date wise to assess the outcome.
Table 1. Date wise assessment of symptoms
Date
Clinical findings
Papules
Pustules
Redness
Black spots
Dull skin on the forehead
7/8/23
+
Cured
Cured
++
Cured
10/9/23
Cured
Cured
Cured
+
Cured
6/10/23
Cured
Cured
Cured
Cured
Cured
Objective parameters: Images were taken through out the treatment, and documented to assess the changes.
Image 1. Jalaukavacaranam dated 6.7.2023

Image 2. Image dated 7.8.2023

Image 3. Image dated 10.9.2023

Image 4. Image at endpoint dated 6.10.2023

-







