Featured Case
-
Abstract
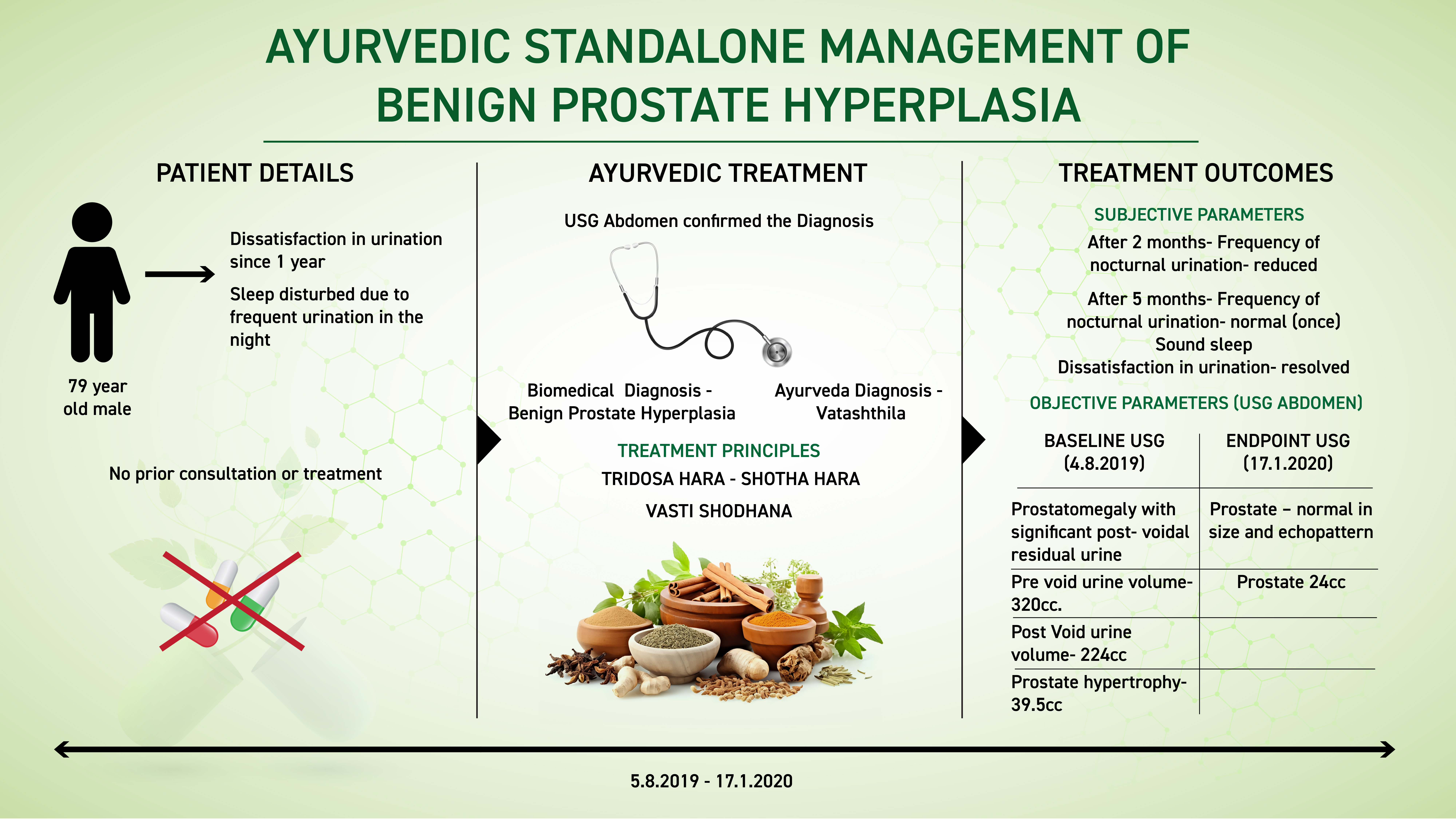
A 79 year old male patient complaints of dissatisfaction in urination since 1 year associated with frequent urination during the night. The sleep in the night is disturbed due to frequency of urination. There is no prior consultation or treatment. The patient opted for Ayurvedic management and approached Dr Tara. Based on the clinical examination and reports of USG abdomen, the biomedical diagnosis was made as Benign prostatic hyperplasia (BPH) and Ayurvedic diagnosis was Vatashtila. The line of treatment followed is Pitta hara and kapha hara, lekhana, rasayana, and mutrala. With 2 months of Ayurvedic treatment the patient noticed a significant reduction in symptoms. After 5 months, the patient attained complete relief from the symptoms and a repeat USG done revealed that the prostate was normal in size. This case report portrays the successful ayurvedic management of BPH, with simple oral medications.
-
Summaries
-
Listen
-
Watch
-
View
-
Read
A 79 year old male patient complaints of dissatisfaction in urination since 1 year associated with frequent urination during the night. The sleep in the night is disturbed due to frequency of urination. There is no prior consultation or treatment. The patient opted for Ayurvedic management and approached Dr Tara. Based on the clinical examination and reports of USG abdomen, the biomedical diagnosis was made as Benign prostatic hyperplasia (BPH) and Ayurvedic diagnosis was Vatashtila. The line of treatment followed is Pitta hara and kapha hara, lekhana, rasayana, and mutrala. With 2 months of Ayurvedic treatment the patient noticed a significant reduction in symptoms. After 5 months, the patient attained complete relief from the symptoms and a repeat USG done revealed that the prostate was normal in size. This case report portrays the successful ayurvedic management of BPH, with simple oral medications.
-
-
Timeline
-
Tabulated Summary
-
Narrative
TITLE OF CASE
Standalone Ayurvedic management of Benign Prostatic Hyperplasia- a case report
Dr Tara
ABSTRACT
A 79 year old male patient complaints of dissatisfaction in urination since 1 year associated with frequent urination during the night. The sleep in the night is disturbed due to frequency of urination. There is no prior consultation or treatment. The patient opted for Ayurvedic management and approached Dr Tara. Based on the clinical examination and reports of USG abdomen, the biomedical diagnosis was made as Benign prostatic hyperplasia (BPH) and Ayurvedic diagnosis was Vatashtila. The line of treatment followed is Pitta hara and kapha hara, lekhana, rasayana, and mutrala. With 2 months of Ayurvedic treatment the patient noticed a significant reduction in symptoms. After 5 months, the patient attained complete relief from the symptoms and a repeat USG done revealed that the prostate was normal in size. This case report portrays the successful ayurvedic management of BPH, with simple oral medications.
KEYWORDS
BPH, vatasthila, case report, ayurveda, standalone
INTRODUCTION
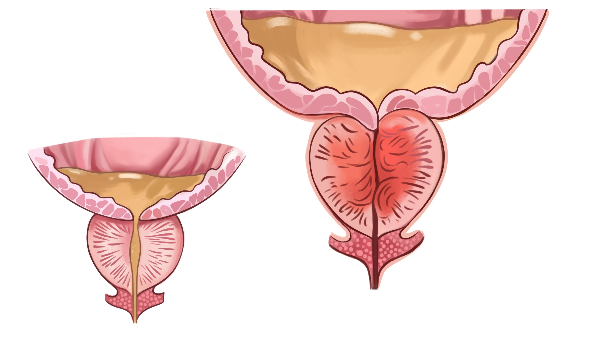
Benign prostatic hyperplasia (BPH) is a health issue that becomes more common with age. It's also called an enlarged prostate. The prostate is a small gland that helps make semen. It's found just below the bladder. And it often gets bigger as you get older. An enlarged prostate can cause symptoms that may bother you, such as blocking the flow of urine out of the bladder. It also can cause bladder, urinary tract or kidney problems.
Symptoms: Common symptoms of BPH include:
- Frequent or urgent need to pee, also called urination.
- Peeing more often at night.
- Trouble starting to pee.
- Weak urine stream, or a stream that stops and starts.
- Dribbling at the end of urination.
- Not being able to fully empty the bladder.
- Less common symptoms include: Urinary tract infection. Not being able to pee. Blood in the urine.
The symptoms of BPH tend to slowly get worse. But sometimes they stay the same or even improve over time.
Causes: The exact cause is not known. It may be because of the changes in the balance of sex or the changes in the hormones as they grow older. The risk factors are aging, family history, diabetes and heart disease, and the lifestyle adapted.
Complications:
The common complications seen are not able to pee, urinary tract infections, bladder stones, bladder damage, and kidney damage.
Diagnosis; Medical history and clinical evaluation are the main diagnostic criteria. Digital rectal exam, Urine test and Blood test are the basic diagnostic tools used by the doctors. Apart form this, the doctor may recommend PSA test, Urine flow test, Postvoid residual volume, and 24 hour voiding is also adopted to help diagnosis the condition. If the health problem is more complex, then a transrectal ultrasound, Prostate biopsy, urodynamic and pressure flow studies, cystoscopy are also adopted in the diagnosis.
Treatment: There are different types of treatment mentioned for BPH. The treatment will be decided depending upon the age, size of the prostate, overall health and the intensity of the symptoms. If the symptoms do not interfere with the quality of life, then treatment is generally not done. If the symptoms get worse or increase then treatments are given. The medicines given are alpha blockers, 5- alpha reductase inhibitors, combination therapy and Tadalafil. As the last resort, surgery may be suggested. Transurethral resection of the prostate, Transurethral incision of the prostate, Transurethral microwave thermotherapy, Laser therapy are some of the surgical procedures that are suggested to treat an enlarged prostate.
Prognosis: The outlook for people with BPH is very good. BPH doesn’t have a cure, but treatments can help alleviate your symptoms.
PATIENT INFORMATION
In this case report, a 79 year old male patient complaints of dissatisfaction in urination since 1 year associated with frequent urination during the night and disturbed sleep due to waking often to urinate. There were no prior consultations or treatments. He consulted Dr Ramkumar for ayurvedic management.
No relevant family/genetic/surgical history.
Psycosocial History- Sleeps during day time and disturbed sleep in night
CLINICAL FINDINGS
General physical examination was done.
Ayurvedic examination:
Prakruti- Kapha pradhana vata dosha
Vikruti- kapha pradhana tridosha
Dushya- mamsa, meda, mutra
Srotodushti- mutravaha and mamsavaha srotas
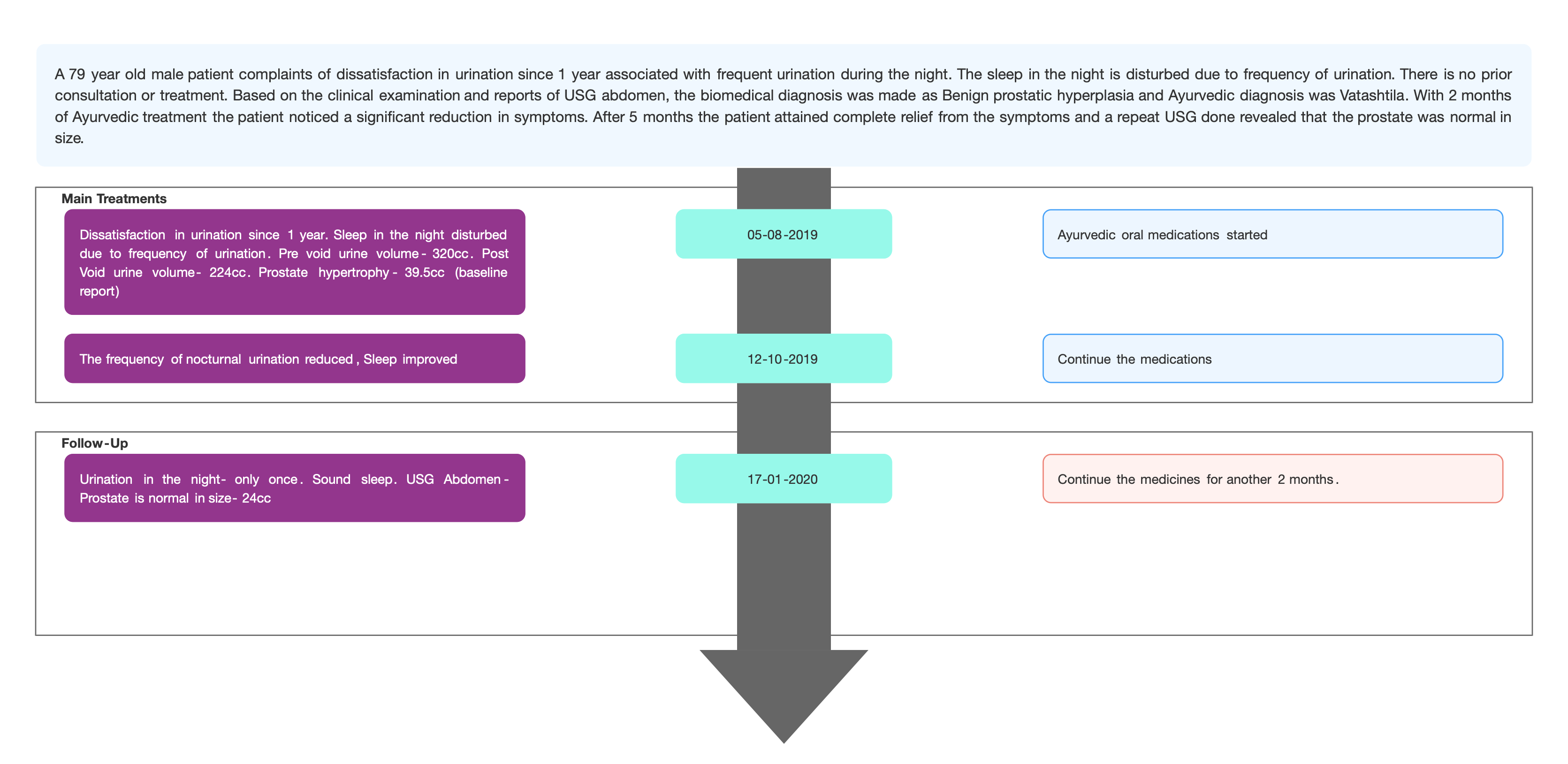
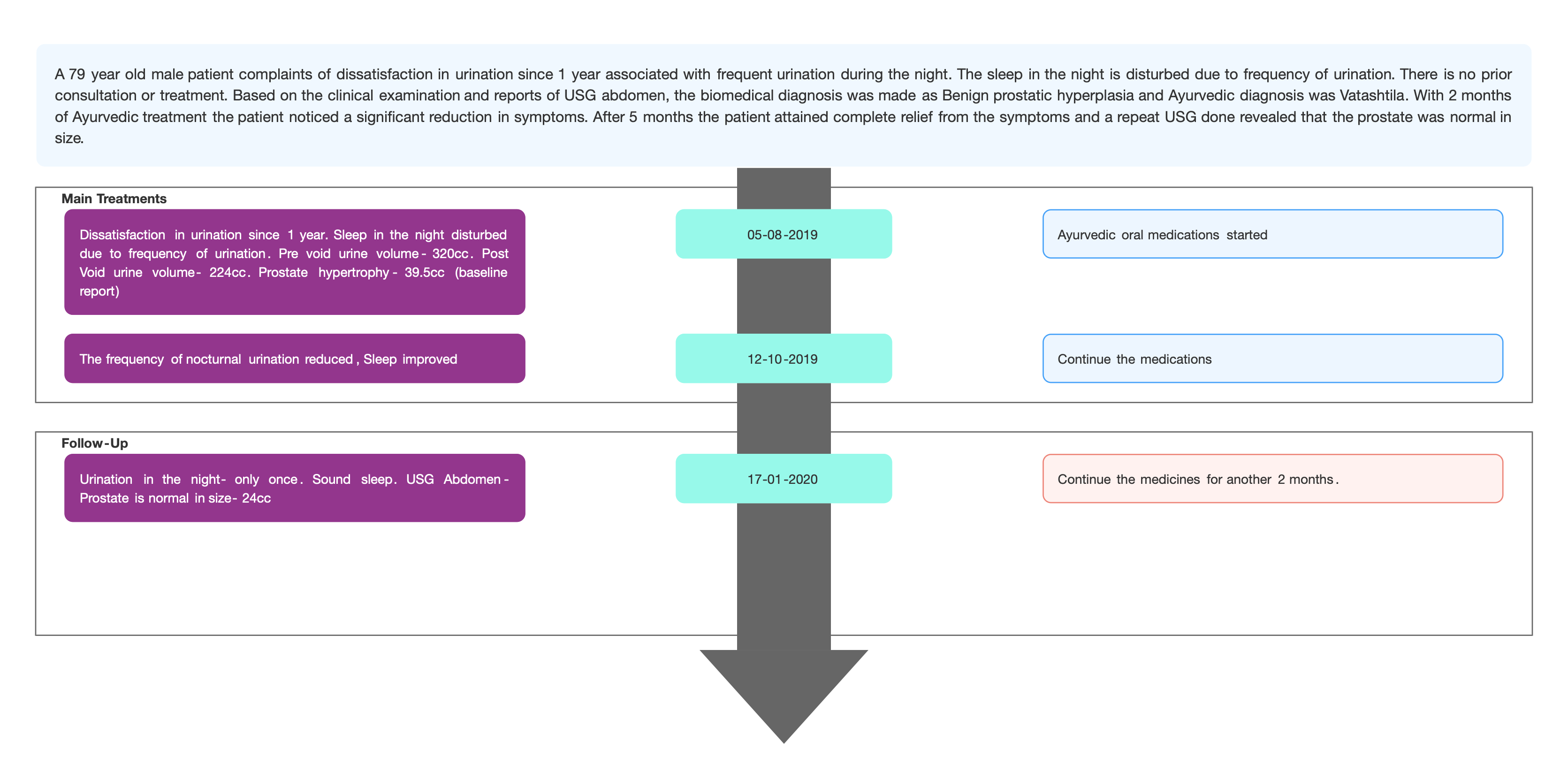
TIMELINE
Image 1. Timeline of events added below
DIAGNOSTIC ASSESSMENT
Modern Diagnostic parameter; Based on the clinical examination and USG reports, the biomedical diagnosis was made as BPH.
Image 1. USG Abdomen at baseline dated 04.08.2019

The reports revealed Prostatomegaly with significant post void residual urine (vol 39.5 cc)
Ayurvedic Assessment was done based on the presenting complaints and clinical evaluation. The treating physician confirmed the Ayurvedic diagnosis as Vatashtila
Differential Diagnosis- Bladder/prostate cancer
Cauda equina (can present with acute retention)
High-pressure chronic retention (presentation insidious or with acute renal failure)
Urinary tract infections/sexually transmitted infections
Prostatitis
Neurogenic bladder (can be secondary to Parkinson's, Multiple sclerosis, etc.)
Urinary tract stones (bladder stones)
Urethral stricture
Based on the investigation reports and presenting symptoms, the physician clinically diagnosed the condition as Benign Prostatic Hyperplasia.
Prognosis- The risk of acute urinary retention also increased with age, as reported in a study, the incidence of retention in men increased over ten-fold, from 3/1000 (40-49yrs) to 34.7/1000 (70-79yrs). Left untreated, BPH, therefore, has a significant risk of progression and presentation. Indeed, up to 42% of men who presented with retention, went on to have surgery. Men with significantly enlarged prostates (>30ml) have also been shown to be at an increased risk of disease progression.
In this case report, with 5 months of ayurvedic treatment, the patient got a significant relief in the symptoms. The repeat USG done at endpoint did not detect BPHTHERAPEUTIC INTERVENTION
Refer the tab ‘Treatment’ in the Portal.
FOLLOW-UP AND OUTCOMES
The patient had 2 follow ups in total.
Subjective parameters:
Clinician-based assessment; There were 2 follow ups with a time gap of 2 months each. After 2 months of treatment, the frequency of nocturnal urination reduced and sleep improved. After 5 months, the patient got complete relief from the symptoms The USG done at endpoint, reveals no prostatomegaly. Prostate size is normal.
Image 2. USG taken at endpoint dated 17.1.2020

Patient-assessed; Not relevant.
Intervention adherence and tolerability – The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment- Subjective and objective parameters were the main assessment tools.
Adverse and unanticipated events; None reported
DISCUSSION:
Benign prostatic hyperplasia (BPH) is a health issue that becomes more common with age. It's also called an enlarged prostate. The prostate is a small gland that helps make semen. It's found just below the bladder. And it often gets bigger as you get older. An enlarged prostate can cause symptoms that may bother you, such as blocking the flow of urine out of the bladder. It also can cause bladder, urinary tract or kidney problems. In this case report, the patient first choice of treatment was Ayurveda. The line of treatment followed is Pitta hara and kapha hara, lekhana, rasayana, and mutrala. With the help of ayurvedic treatments, in 5 months the patient got complete relief from symptoms.
PATIENT’S PERSPECTIVE
Not available.
LEARNING POINTS/TAKE HOME MESSAGES
This case report highlights the efficacy of standalone Ayurveda treatment in an old man who was suffering from Benign Prostatic Hyperplasia, preventing its progression and also achieved remission in 5 months.
INFORMED CONSENT
Written consent obtained from patient for publishing of the case report in the Portal
ACKNOWLEDGEMENTS
None
CONFLICT OF INTEREST
None declared.
FUNDING
None
REFERENCE
-
Immersive Learning
-
Modern Diagnosis
MODERN DIAGNOSIS: Benign prostatic hyperplasia
ABOUT THE DISEASE:
Benign prostatic hyperplasia (BPH) is a health issue that becomes more common with age. It's also called an enlarged prostate. The prostate is a small gland that helps make semen. It's found just below the bladder. And it often gets bigger as you get older. An enlarged prostate can cause symptoms that may bother you, such as blocking the flow of urine out of the bladder. It also can cause bladder, urinary tract or kidney problems.
Symptoms: Common symptoms of BPH include:
- Frequent or urgent need to pee, also called urination.
- Peeing more often at night.
- Trouble starting to pee.
- Weak urine stream, or a stream that stops and starts.
- Dribbling at the end of urination.
- Not being able to fully empty the bladder.
- Less common symptoms include: Urinary tract infection. Not being able to pee. Blood in the urine.
The symptoms of BPH tend to slowly get worse. But sometimes they stay the same or even improve over time.
Causes: The exact cause is not known. It may be because of the changes in the balance of sex or the changes in the hormones as they grow older. The risk factors are aging, family history, diabetes and heart disease, and the lifestyle adapted.
Complications:
The common complications seen are not able to pee, urinary tract infections, bladder stones, bladder damage, and kidney damage.
Diagnosis; Medical history and clinical evaluation are the main diagnostic criteria. Digital rectal exam, Urine test and Blood test are the basic diagnostic tools used by the doctors. Apart form this, the doctor may recommend PSA test, Urine flow test, Postvoid residual volume, and 24 hour voiding is also adopted to help diagnosis the condition. If the health problem is more complex, then a transrectal ultrasound, Prostate biopsy, urodynamic and pressure flow studies, cystoscopy are also adopted in the diagnosis.
In this case report, a 79 year old male patient complaints of dissatisfaction in urination since 1 year associated with frequent urination during the night and disturbed sleep due to waking often to urinate. There were no prior consultations or treatments. He consulted Dr Tara for ayurvedic management. Based on clinical examination and USG abdomen reports the physician diagnosed the condition as Benign prostatic hyperplasia and Ayurvedic diagnosis as vatasthila.
Image 1. USG Abdomen at baseline dated 04.08.2019

Treatment: There are different types of treatment mentioned for BPH. The treatment will be decided depending upon the age, size of the prostate, overall health and the intensity of the symptoms. If the symptoms do not interfere with the quality of life, then treatment is generally not done. If the symptoms get worse or increase then treatments are given. The medicines given are alpha blockers, 5- alpha reductase inhibitors, combination therapy and Tadalafil. As the last resort, surgery may be suggested. Transurethral resection of the prostate, Transurethral incision of the prostate, Transurethral microwave thermotherapy, Laser therapy are some of the surgical procedures that are suggested to treat an enlarged prostate.
Prognosis: The outlook for people with BPH is very good. BPH doesn’t have a cure, but treatments can help alleviate your symptoms.
Reference
-
Ayurveda Diagnosis
AYURVEDA DIAGNOSIS: Vatashtila
ABOUT THE DISEASE:
The term mutraghata is made up of two words i.e.; mutra (i.e.; urine) and aghata means obstruction of urinary passage. Vatashtila is a type of Mutraghata. Mutraghata is correlated to obstructive neuropathy owing to the similarity in symptoms.
Causes: Sushruta has mentioned various etiological factors like suppression of natural urges vegavarodha), excessive exercise (i.e.; ativyayam), excessive sexual intercourse (i.e.; ativyavyav), too much intake of astringent, bitter, and pungent foods (i.e.; katu and teekshna rasa ahara), excess use of wine and fleshy meat leads to vatashtila.
The general symptoms for all types of mutraghata are:
सामान्यलिङ्गं रुङ्नाभिसेवनीबस्तिमूर्धसु।
विशीर्णधारं मूत्रं स्यात्तया मार्गनिरोधने॥९॥
तद्व्यपायात्सुखं मेहेदच्चं गोमेदकोपमम्।
तत्सङ्क्षोभात्क्षते सास्रमायासाच्चातिरुग्भवेत्॥१०॥
There is pain in the nabhi, sevani and the vasti. There is an obstruction to the normal flow of the urine. Once the urination happens, then the patient gets relief from pain. When there is a complete obstruction in the tract, then there will be blood in the urine.
The samprapti and specific lakshana of Vatashtila are:
शकृन्मार्गस्य बस्तेश्च वायुरन्तरमाश्रितः॥२३॥
अष्ठीलाभं घनं ग्रन्थिं करोत्यचलमुन्नतम्। वाताष्ठीलेति साऽऽआध्मानविण्मूत्रानिलसङ्गकृत्॥२४॥ (AH.Ni.9)
Vayu vitiation produces an elevated, mobile and glandular swelling that obstructs the passage of faeces and urine. This presents with adhmana, and sanga of vit, mutra, and anila.
Treatment: Sushruta has described general guideline for management of all type of mutraghata (i.e.; obstructive uropathy) with use of kashaya, kalka, avaleha, kshar, madya, aasava, snehana, swedana, basti and uttarbasti. Uttarbasti in urological disorders, it is the best treatment modality for vitiated vata dosha and various decoction, kalka, ghee, avaleha, milk, kshara, alcohol, upanaha sweda, is also indicated. Sneha virechana should be used in all types of urinary disorders.
In this case report, a 79 year old male patient complaints of dissatisfaction in urination since 1 year associated with frequent urination during the night and disturbed sleep due to waking often to urinate. There were no prior consultations or treatments. He consulted Dr Tara for ayurvedic management. Based on clinical examination and USG abdomen reports the physician diagnosed the condition as Benign prostatic hyperplasia and Ayurvedic diagnosis as vatasthila.
Rationale for specific selection of medicines as explained by the physician is mentioned below.
Varunadi Kashayam for lekhana
Amritaashwagandhadi for rejuvenation purpose
Punarnavadi for Mutrala karma
Chandraprabha vati for mutrakrichcha
Elaganadi to support the urinary system function
Brihatyadi kashayam for Kaphahara
And Drakshadi for Pittahara property
Reference
- Caraka Samhita.Cikitsa.30
- Susruta Samhita. Uttara tantra. 58.
-
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Amritashwagandhadi Kashaya + Elakanadi Kashayam + Varunadi Kashaya + Chandraprabha Vati Samyoga 15 ml of Kasaya + 1 tablet Oral, with 60ml warm water- daily morning before food. 2019-08-05 - 2020-03-15 Amritashwagandhadi Kashaya - Patent & proprietary. Elakanadi Kashaya - Sahasrayogam Kashaya prakarana. Varunadi Kashaya - Sahasrayogam Kashaya prakarana. Chandraprabha Vati- Sharangadhara Samhita. Madhyama Khanda 7.40 - 49 Punarnavadi Kashaya + Brihathyadi Kashaya + Drakshadi Kashaya + Chandraprabha Vati Samyoga 15 ml of Kasaya + 2 tablet Oral, with 60ml warm water- daily evening before food. 2019-08-05 - 2020-03-15 Punarnavadi Kashaya- Sahasrayogam Kashaya prakarana. Brihatyadi Kashaya- AH. Ci. 11.35. Drakshadi Kashaya- Sahasrayogam Kashaya prakarana. Chandraprabha vati- Sharangadhara Samhita. Madhyama Khanda 7.40 - 49 Dhanwantaram Ghrta + Vasthyamayantaka Ghrta Ghrta 1 tsp Oral at bedtime 2019-08-05 - 2020-03-15 Dhanwantaram Ghrta - AH. Ci.12.19-24. Vasthyamayantaka Ghrta - Sahasrayogam. Ghrta Prakarana -
Outcome Measures
In this case report, a 79 year old male patient complaints of dissatisfaction in urination since 1 year associated with frequent urination during the night and disturbed sleep due to waking often to urinate. There were no prior consultations or treatments. He consulted Dr Ramkumar for ayurvedic management. Based on clinical examination and USG abdomen reports the physician diagnosed the condition as Benign prostatic hyperplasia and Ayurvedic diagnosis as vatasthila.
Assessment: Subjective and objective parameters were assessed to analyse the outcome of the treatment.
Subjective parameters: After 2 months of starting ayurvedic treatments, the frequency of nocturnal urination reduced. Sleep improved. After 5 months, dissatisfaction in urination- absent:
frequency of urination in night- reduced to 1 (Normal) and patient has a sound sleep.Objective parameters:
At endpoint, a repeat USG was done to assess the outcome of the treatment.
Image 1. USG at endpoint dated 17.1.2020

-




