Featured Case
-
Abstract
A 32-year-old female patient complaints of scanty and irregular periods associated with painful menstruation for 1 year. There were no prior consultations or treatments. She approached Dr Tara, for Ayurvedic management. Her USG reports revealed Bulky uterus with adenomyotic changes and Bilateral Polycystic ovaries. Based on the investigation report and clinical examination, the Biomedical diagnosis was made as Adenomyosis and the Ayurvedic diagnosis was Vataja Yonivyapat. The line of treatment followed was Vata- pitta shamana and initiate the vatanulomana. After 6 months of treatment, the patient got significant relief from all the symptoms with normal menstrual cycle. In the repeat USG, done at the endpoint, the uterus appears normal with homogenous myometrial echoes. This case report demonstrates the successful standalone ayurvedic management of Adenomyosis.
-
Summaries
-
Listen
-
Watch
-
View

-
Read
A 32-year-old female patient complaints of scanty and irregular periods associated with painful menstruation for 1 year. There were no prior consultations or treatments. She approached Dr Tara, for Ayurvedic management. Her USG reports revealed Bulky uterus with adenomyotic changes and Bilateral Polycystic ovaries. Based on the investigation report and clinical examination, the Biomedical diagnosis was made as Adenomyosis and the Ayurvedic diagnosis was Vataja Yonivyapat. The line of treatment followed was Vata- pitta shamana and initiate the vatanulomana. After 6 months of treatment, the patient got significant relief from all the symptoms with normal menstrual cycle. In the repeat USG, done at the endpoint, the uterus appears normal with homogenous myometrial echoes. This case report demonstrates the successful standalone ayurvedic management of Adenomyosis.
-
-
Timeline
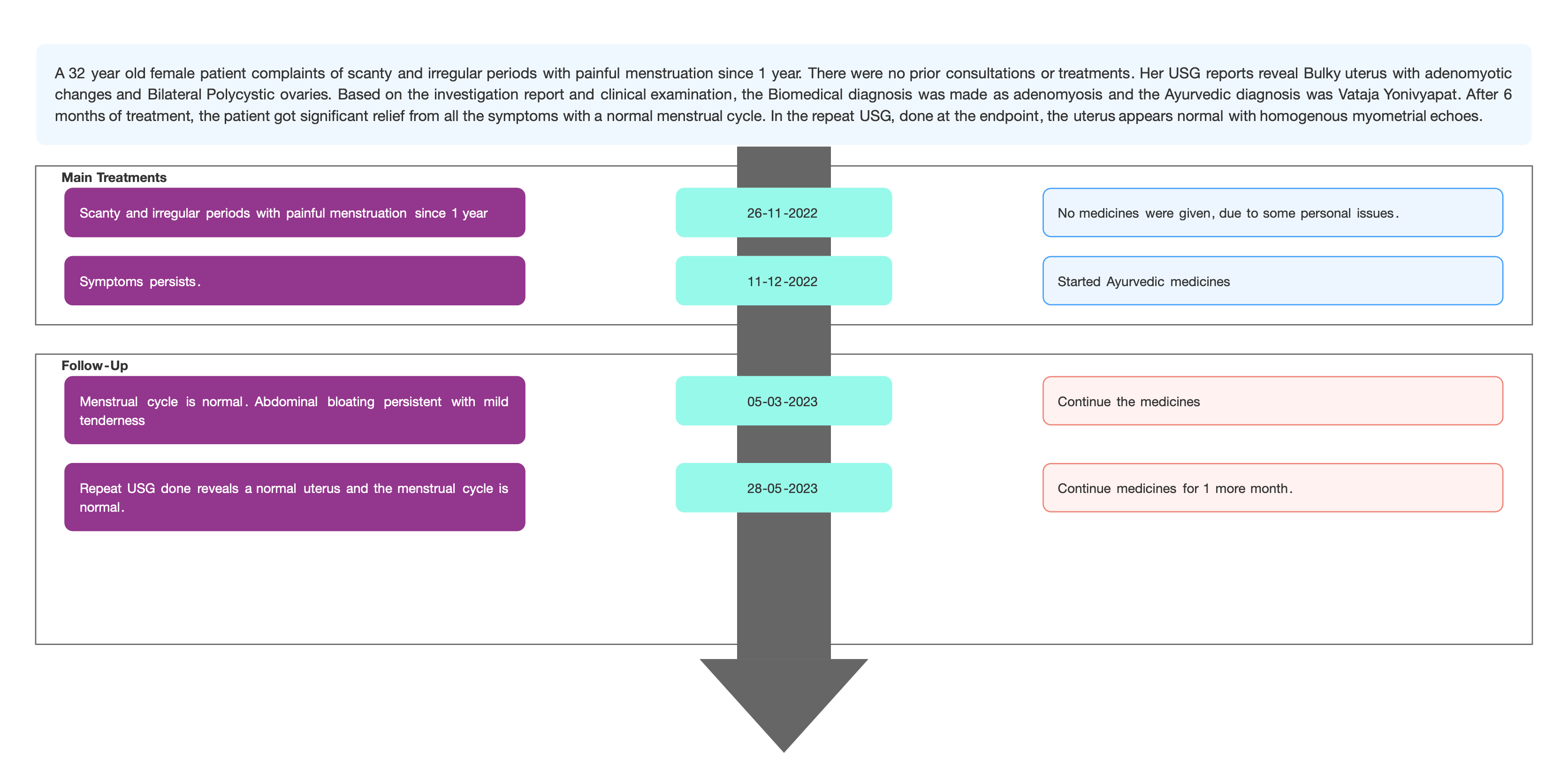
-
Tabulated Summary
-
Narrative
TITLE OF CASE
Standalone Ayurvedic management of Adenomyosis- A case report
Dr Tara
ABSTRACT
A 32-year-old female patient complaints of scanty and irregular periods associated with painful menstruation for 1 year. There were no prior consultations or treatments. She approached Dr Tara, for Ayurvedic management. Her USG reports revealed Bulky uterus with adenomyotic changes and Bilateral Polycystic ovaries. Based on the investigation report and clinical examination, the Biomedical diagnosis was made as Adenomyosis and the Ayurvedic diagnosis was Vataja Yonivyapat. The line of treatment followed was Vata- pitta shamana and initiate the vatanulomana. After 25 days of treatment, the patient got significant relief from all the symptoms with normal menstrual cycle. In the repeat USG, done at the endpoint, the uterus appears normal with homogenous myometrial echoes. This case report demonstrates the successful standalone ayurvedic management of Adenomyosis.
KEYWORDS
Adenomyosis, Case report, Yonivyapat, Yoniroga, Irregular menstruation, Ayurveda, Scanty menstruation
INTRODUCTION
Adenomyosis (ad-uh-no-my-O-sis) occurs when the tissue that normally lines the uterus (endometrial tissue) grows into the muscular wall of the uterus. The displaced tissue continues to act normally — thickening, breaking down and bleeding — during each menstrual cycle. An enlarged uterus and painful, heavy periods can result.
Causes and treatment approach: The exact cause is not known, but the disease usually resolves after menopause. For women who have severe discomfort from adenomyosis, hormonal treatments can help. Removal of the uterus (hysterectomy) cures adenomyosis. The general causes that are attributed are invasive tissue growth, developmental origins, uterine inflammation related to child birth, and stem cell origins. The risk factors include prior uterine surgeries, child birth and middle age. Generally women in the age group between 40 and 50 get affected.
Symptoms: Sometimes, adenomyosis causes no signs or symptoms or only mild discomfort. However, adenomyosis may present with Heavy or prolonged menstrual bleeding, Severe cramping or sharp, knifelike pelvic pain during menstruation (dysmenorrhea), Chronic pelvic pain, Painful intercourse (dyspareunia). The uterus might get bigger. Tenderness or pressure is experienced in the lower abdomen.
Complications:
If you often have prolonged, heavy bleeding during your periods, you can develop chronic anemia, which causes fatigue and other health problems. Although not harmful, the pain and excessive bleeding associated with adenomyosis can disrupt your lifestyle. The normal and regular activities may have to be changed owing to the discomforts of the condition.
Diagnosis; Medical history and clinical evaluation are the main diagnostic criteria. A pelvic exam that reveals an enlarged tender uterus, Ultrasound imaging of the uterus, and Magnetic resonance imaging (MRI) of the uterus are some other diagnostic tools that are used. If serious pathologies are suspected, then an endometrial biopsy may be done also, mostly to rule out malignancies.
Treatment: Adenomyosis often goes away after menopause, so treatment might depend on how close you are to that stage of life.
Other options include:
Anti-inflammatory drugs: Drugs like ibuprofen (Advil, Motrin IB, others), helps control the pain. By starting an anti-inflammatory medicine one to two days before your period begins and taking it during your period, you can reduce menstrual blood flow and help relieve pain.
Hormone medications. Combined estrogen-progestin birth control pills or hormone-containing patches or vaginal rings will help controlling the bleeding and also reduce the pain associated with adenomyosis.
Hysterectomy. This is the last resort of treatment, when no other treatments are working.
The consensus to treatment is a stepwise approach with medical therapy to include anti-inflammatory and hormonal agents with progression to minimally invasive procedures such as endometrial ablation/myomectomy or uterine artery embolisation. The best treatment option is hysterectomy.
PATIENT INFORMATION
The patient is a 32 year old female patient complaints of scanty and irregular periods with painful menstruation since 1 year. There were no prior consultations or medications.
No relevant family/genetic/psycosocial history.
Surgical History- Underwent 2 C- Sections
CLINICAL FINDINGS
On examination, Abdomen bloated with mild tenderness in hypogastric region
TIMELINE
Image 1. Timeline of events added below
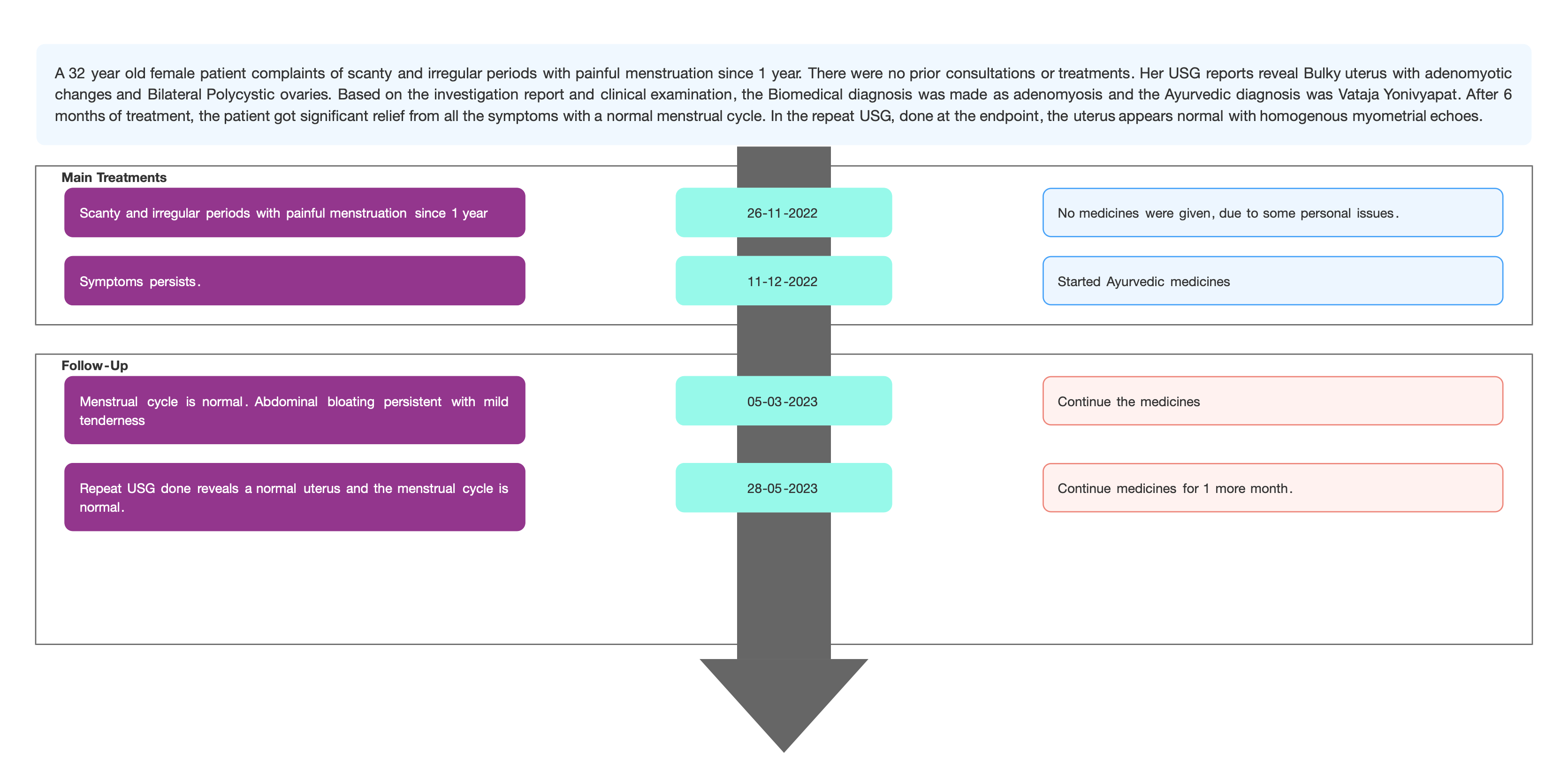
DIAGNOSTIC ASSESSMENT
Modern Diagnostic parameter; Based on the clinical examination and USG reports, the biomedical diagnosis was made as Adenomyosis.
Image 2. USG taken at baseline dated 26.11.2022

The reports revealed Bulky uterus with adenomyotic changes: Bilateral Polycystic ovaries
Ayurvedic Assessment was done based on the presenting complaints and clinical evaluation. The treating physician confirmed the Ayurvedic diagnosis as Vataja Yoniroga.
Differential Diagnosis-
Polyps
Leiomyoma
Malignancy/hyperplasia
Coagulopathy
Ovulatory dysfunction
Based on the investigation report and clinical examination, the condition was diagnosed as AdenomyosisPrognosis- The consensus to treatment is a stepwise approach with medical therapy to include anti-inflammatory and hormonal agents with progression to minimally invasive procedures such as endometrial ablation/myomectomy or uterine artery embolisation. The best treatment option is hysterectomy. In this case report, with 25 days of Ayurvedic treatment, the patient had normal menstrual cycle. After 3 months of treatment, the patient got significant relief from all the symptoms with normal menstrual cycle. In the repeated USG, done at endpoint, the uterus appears normal with homogenous myometrial echoes.
THERAPEUTIC INTERVENTION
Refer the tab ‘Treatment’ in the Portal.
FOLLOW-UP AND OUTCOMES
The patient had 2 follow ups in total.
Subjective parameters:
Clinician-based assessment; After 25 days of treatment, the menstrual cycle became normal. After 3 months, the menstrual cycle was still stable and regular.
Image 3. USG taken at endpoint dated 27.5.2023

Patient-assessed; Not relevant.
Intervention adherence and tolerability – The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment- Subjective and objective parameters were the main assessment tools.
Adverse and unanticipated events; None reported
DISCUSSION:
Adenomyosis (ad-uh-no-my-O-sis) occurs when the tissue that normally lines the uterus (endometrial tissue) grows into the muscular wall of the uterus. The displaced tissue continues to act normally — thickening, breaking down and bleeding — during each menstrual cycle. An enlarged uterus and painful, heavy periods can result. In this patient, though the presenting symptoms did not match with the exact presentation of adenomyosis, the treating physician relied on the USG report to confirm the biomedical diagnosis as Adenomyosis. The ayurvedic diagnosis was Vataja yoniroga, and the line of treatment followed was Vata- pitta shamana and initiate the vatanulomana. The rationale of medicines chosen was as follows:
Drakshadi kashayam - The main ingredient in Drakshadi kashayam is draksha which has vata and pitta shamana properties can be used in bleeding disorders as well in case of Adenomyosis.
Gandharvahasthadi Kashaya – it mainly has vatahara and anulomana properties due to which can act remarkably on bloating issues as well as yonivyapat.
Sukumaram Kashayam has vata and pitta shamana properties and has antispasmodic action, which gives relief from menstrual cramps, severe throbbing pain or severe lower abdominal cramps that occur just before or during menstrual periods.
Shringa bhasma: Due to its action on vata and pitta doshas balancing, it can be used in adenomyosis.
Hinguvacadi Curna- Vatahara and anulomana karma
Sukumara Lehya- Due to vata and pitta shamana properties it can be given in irregular periods and helps to bring menstrual cycle to normalcy.
Kanasthahwadi Kashayam:- Due to vatahara and kaphahara properties it can be used in ama condition which gives relief from abdominal bloating and scanty menstrual flow.
Kanchanar guggulu:- Kanchanar guggulu helps balance kapha and reduces medha dhatu.
PATIENT’S PERSPECTIVE
Not available.
LEARNING POINTS/TAKE HOME MESSAGES
This case report highlights the efficacy of standalone ayurveda treatment for the management of adenomyosis within a short span of 3 months.
INFORMED CONSENT
Written consent obtained from patient for publishing of the case report in the Portal
ACKNOWLEDGEMENTS
None
CONFLICT OF INTEREST
None declared.
FUNDING
None
REFERENCE
-
Immersive Learning
-
Modern Diagnosis
MODERN DIAGNOSIS: Adenomyosis
ABOUT THE DISEASE:
Adenomyosis (ad-uh-no-my-O-sis) occurs when the tissue that normally lines the uterus (endometrial tissue) grows into the muscular wall of the uterus. The displaced tissue continues to act normally — thickening, breaking down and bleeding — during each menstrual cycle. An enlarged uterus and painful, heavy periods can result.
Causes and treatment approach: The exact cause is not known, but the disease usually resolves after menopause. For women who have severe discomfort from adenomyosis, hormonal treatments can help. Removal of the uterus (hysterectomy) cures adenomyosis. The general causes that are attributed are invasive tissue growth, developmental origins, uterine inflammation related to child birth, and stem cell origins. The risk factors include prior uterine surgeries, child birth and middle age. Generally women in the age group between 40 and 50 get affected.
Symptoms: Sometimes, adenomyosis causes no signs or symptoms or only mild discomfort. However, adenomyosis may present with
Heavy or prolonged menstrual bleeding
Severe cramping or sharp, knifelike pelvic pain during menstruation (dysmenorrhea)
Chronic pelvic pain
Painful intercourse (dyspareunia)
Your uterus might get bigger. Although you might not know if your uterus is bigger, you may notice tenderness or pressure in your lower abdomen.
Complications:
If you often have prolonged, heavy bleeding during your periods, you can develop chronic anemia, which causes fatigue and other health problems. Although not harmful, the pain and excessive bleeding associated with adenomyosis can disrupt your lifestyle. The normal and regular activities may have to be changed owing to the discomforts of the condition.
Diagnosis; Medical history and clinical evaluation are the main diagnostic criteria. A pelvic exam that reveals an enlarged tender uterus, Ultrasound imaging of the uterus, and Magnetic resonance imaging (MRI) of the uterus are some other diagnostic tools that are used. If serious pathologies are suspected, then an endometrial biopsy may be done also, mostly to rule out malignancies.
In this case report, a 32 year old female patient complaints of scanty and irregular periods with painful menstruation since 1 year. There were no prior consultations or medications. Dr Tara suggested to take a USG scan which revealed Bulky uterus with adenomyotic changes and Bilateral Polycystic ovaries. Based on the investigation report and clinical examination, the Biomedical diagnosis was adenomyosis and the Ayurvedic diagnosis was Vataja Yonivyapat. Though the symptoms do not primarily match the adenomyosis symptoms, the treating physician decided to go with the USG findings in confirming the biomedical diagnosis. The symptoms correlate more with her presenting complaints of PCOS.
Image 1. USG Abdomen at baseline dated 26.11.2022

Treatment: Adenomyosis often goes away after menopause, so treatment might depend on how close you are to that stage of life.
Other options include:
Anti-inflammatory drugs: Drugs like ibuprofen (Advil, Motrin IB, others), helps control the pain. By starting an anti-inflammatory medicine one to two days before your period begins and taking it during your period, you can reduce menstrual blood flow and help relieve pain.
Hormone medications. Combined estrogen-progestin birth control pills or hormone-containing patches or vaginal rings will help controlling the bleeding and also reduce the pain associated with adenomyosis.
Hysterectomy. This is the last resort of treatment, when no other treatments are working.
Prognosis: The consensus to treatment is a stepwise approach with medical therapy to include anti-inflammatory and hormonal agents with progression to minimally invasive procedures such as endometrial ablation/myomectomy or uterine artery embolisation. The best treatment option is hysterectomy.
Reference
-
Ayurveda Diagnosis
AYURVEDA DIAGNOSIS: Vataja Yonivyapat
ABOUT THE DISEASE:
The word ‘yoni’ stands for Vagina or female reproductive systems and ‘vyapat’ stands for diseases. It can also be referred to as Yoniroga. There are 20 yonirogas that have been explained in detail in the classical textbooks.
Nidana: The causative factors are as follows:
मिथ्याचारेण ताः स्त्रीणां प्रदुष्टेनार्तवेन च|
जायन्ते बीजदोषाच्च दैवाच्च शृणु ताः पृथक्॥८॥(CS.Ci.30)
Mithyachara – wrong regime: Pradushta Arthava – menstrual morbidities: Beeja Dosha – defective genes, or gametes: Daiva or Karma- due to the divine interception or due to karma.
Symptoms: When the yoni roga is caused by vitiation of vata predominantly, then it is called as Vataja yonivyapat.
Causes and symptoms of vataja yoniroga are If a woman having Vata body type, resorts to Vata increasing food and regimen, it causes Vata increase. The aggravated Vata gets located in the reproductive organs to produce below symptoms –
Stambha – stiffness, Pipilika – a sensation as if ants are crawling, Stambha – numbness, Supti – numbness and such other ailments caused by Vata in that place (reproductive organs). Because of aggravated Vata, the patient gets untimely menstrual bleeding which is phena, tanu, ruksha,
sa syat sa shabda.वातलाहारचेष्टाया वातलायाः समीरणः। विवृद्धो योनिमाश्रित्य योनेस्तोदं सवेदनम्॥९॥
स्तम्भं पिपीलिकासृप्तिमिव कर्कशतां तथा। करोति सुप्तिमायासं वातजांश्चापरान् गदान्॥१०॥
सा स्यात् सशब्दरुक्फेनतनुरूक्षार्तवा/निलात्। व्यापत्कट्वम्ललवणक्षाराद्यैः पित्तजा भवेत्॥११॥ (CS.Ci.30)
Complications: When afflicted with Yoniroga, then patient can be affected with gulma, arshas and pradara.
Treatment for Yonirogas: Sneha, Sveda and Vasti are the main treatment procedures followed for Yonirogas in general.
स्नेहनस्वेदबस्त्यादि वातजास्वनिलापहम्॥४१॥ (CS.Ci.30)
Specific treatment for vataja yoniroga:
वातव्याधिहरं कर्म वातार्तानां सदा हितम्।
औदकानूपजैर्मांसैः क्षीरैः सतिलतण्डुलैः॥४७॥
सवातघ्नौषधैर्नाडीकुम्भीस्वेदैरुपाचरेत्।
अक्तां लवणतैलेन साश्मप्रस्तरसङ्करैः॥४८॥
स्विन्नां कोष्णाम्बुसिक्ताङ्गीं वातघ्नैर्भोजयेद्रसैः।४९। (CS.Ci.30)
The body is smeared with oil mixed with rock- salt and thereafter, nadi, kumbhi, ashma, prastara and sankara types of sweda karmas are administered with the medicines containing meat of aquatic (audaka) and marshy land- inhabiting animals (anupamamsa), milk, dehusked tila – sesame and vayu- alleviating herbs. After swedana, she is sprinkled with warm water, and given mamsarasa prepared by boiling with vatahara dravyas.
In this case report, a 32 year old female patient complaints of scanty and irregular periods with painful menstruation since 1 year. There were no prior consultations or medications. Dr Tara suggested to take a USG scan which revealed Bulky uterus with adenomyotic changes and Bilateral Polycystic ovaries. Based on the investigation report and clinical examination, the Biomedical diagnosis was adenomyosis and the Ayurvedic diagnosis was Vataja Yonivyapat.
Rationale of treatment as explained by the physician is tabulated below.
Drakshadi kashayam - The main ingredient in Drakshadi kashayam is draksha which has vata and pitta shamana properties can be used in bleeding disorders as well in case of Adenomyosis.
Gandharvahasthadi Kashaya – it mainly has vatahara and anulomana properties due to which can act remarkably on bloating issues as well as yonivyapat.
Sukumaram Kashayam has vata and pitta shamana properties and has antispasmodic action, which gives relief from menstrual cramps, severe throbbing pain or severe lower abdominal cramps that occur just before or during menstrual periods.
Shringa bhasma: Due to its action on vata and pitta doshas balancing, it can be used in adenomyosis.
Hinguvacadi Curna- Vatahara and anulomana karma
Sukumara Lehya- Due to vata and pitta shamana properties it can be given in irregular periods and helps to bring menstrual cycle to normalcy.
Kanasthahwadi Kashayam:- Due to vatahara and kaphahara properties it can be used in ama condition which gives relief from abdominal bloating and scanty menstrual flow.
Kanchanar guggulu:- Kanchanar guggulu helps balance kapha and reduces medha dhatu.
Reference
- Caraka Samhita.Cikitsa.30
- https://www.easyayurveda.com/2016/02/02/charaka-chikitsa-sthana-30th-chapter-yoni-vyapat/
-
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Drakshadi Kashayam + Gandharvahasthadi Kashayam + Sukumaram Kashayam + Shringa bhasma Samyoga 15ml kashayam + 1 pinch bhasma Oral, Kashayam with 60ml warm water + 1 pinch bhasma twice daily before food 2022-02-11 - 2023-05-27 Sukumara kashayam, ?Drakshyadi kashayam, Gandharvahasthadi kashayam- Sahasrayogam Kashaya prakaranam: ?Shringa bhasma - Rasatarangini 12.105-107 Hinguvachadi Curnam Curna 1 tsp With warm water before lunch 2022-12-11 - 2023-05-27 AH.Ci.14.31- 33 Sukumara Lehyam Lehyam 1 tsp At bedtime 2022-12-11 - 2023-06-27 AH.Ci.13.41- 47 Gandharvahasthadi Kashayam + Sukumaram Kashayam + Kanasathahwadi Kashayam + Kanchanara guggulu Samyoga 15ml kashayam + 1 tablet Oral, kashayam with 45 ml warm water + 1 tablet twice daily before food 2023-05-28 - 2023-06-27 Kanchanara guggulu- Sh. sam Madyama khanda 7. 94-100. Kanasathahwadi Kashayam- Sahasrayogam Kashaya prakaranam -
Outcome Measures
In this case report, a 32 year old female patient complaints of scanty and irregular periods with painful menstruation since 1 year. There were no prior consultations or medications. Dr Tara suggested to take a USG scan which revealed Bulky uterus with adenomyotic changes and Bilateral Polycystic ovaries. Based on the investigation report and clinical examination, the Biomedical diagnosis was adenomyosis and the Ayurvedic diagnosis was Vataja Yonivyapat.
Assessment: Subjective and objective parameters were assessed to analyse the outcome of the treatment.
Subjective parameters: After 25 days, significant improvement was seen in patient. The menstrual cycle was normal. After 3 months of treatment, the menstrual cycle became normal.
Objective parameters:
At endpoint, a repeat USG was done to assess the outcome of the treatment.
Image 1. USG at endpoint dated 27.5.2023

-




