Featured Case
-
Abstract
A 63-year-old female patient was a known case of Diabetes mellitus for 2 years and Hypertension for 17 years, and was on regular allopathic medicines. For the past 4-5 years, she has been suffering from low backache associated with stiffness. She tried painkillers but got no relief. She was advised to undergo surgery. The patient now consulted Dr Partap Chauhan for better ayurvedic management. Based on the clinical evaluation and MRI findings, the biomedical diagnosis was made as Lumbar spondylosis, and the Ayurvedic diagnosis was made as Kati shoola. The line of treatment planned was Vata kapha shamana, ama pacana, sroto shodhana and rasayana. Within 1 month of ayurvedic treatment, there was a significant reduction in pain and stiffness. In 2 months, there was only minimal pain on walking short distances. With 4 months of Ayurvedic treatment, the patient got complete relief from symptoms and the quality of life improved. At rest, VAS was recorded 8 before treatment and 2 after treatment. During activity, VAS recorded 10 before treatment became 2 after treatment. This case report demonstrates the successful ayurvedic management of chronic low backache, in a patient who was advised surgery as a remedy for her symptoms.
-
Summaries
-
Listen
-
Watch
-
View

-
Read
A 63-year-old female patient was a known case of Diabetes mellitus for 2 years and Hypertension for 17 years, and was on regular allopathic medicines. For the past 4-5 years, she has been suffering from low backache associated with stiffness. She tried painkillers but got no relief. She was advised to undergo surgery. The patient now consulted Dr Partap Chauhan for better ayurvedic management.
Based on the clinical evaluation and X Ray findings, the biomedical diagnosis was made as Lumbar spondylosis, and the Ayurvedic diagnosis was made as Kati shoola. The line of treatment planned was Vata kapha shamana, ama pacana, sroto shodhana and rasayana. Within 1 month of ayurvedic treatment, there was a significant reduction in pain and stiffness. In 2 months, there was only minimal pain on walking short distances. With 4 months of Ayurvedic treatment, the patient got complete relief from symptoms and the quality of life improved. At rest, VAS was recorded 8 before treatment and 2 after treatment. During activity, VAS recorded 10 before treatment became 2 after treatment. This case report demonstrates the successful ayurvedic management of chronic low backache, in a patient who was advised surgery as a remedy for her symptoms.
-
-
Timeline
-
Tabulated Summary
-
Narrative
TITLE OF CASE
Ayurvedic management of Lumbar Spondylosis- A case report
Dr Partap Chauhan
ABSTRACT
A 63-year-old female patient was a known case of Diabetes mellitus for 2 years and Hypertension for 17 years, and was on regular allopathic medicines. For the past 4-5 years, she is suffering from low backache associated with stiffness. She tried painkillers but got no relief. She was advised to undergo surgery. The patient now consulted Jiva Ayurveda.
Based on the clinical evaluation and X Ray findings, the biomedical diagnosis was made as Lumbar spondylosis, and the Ayurvedic diagnosis was made as Kati shoola. The line of treatment planned was Vata kapha shamana, ama pacana, sroto shodhana and rasayana. Within 1 month of ayurvedic treatment, there was a significant reduction in pain and stiffness. In 2 months, there was only minimal pain on walking short distances. With 5 months of Āyurvedic treatment, the patient got complete relief from symptoms and the quality of life improved. At rest, VAS was recorded 8 before treatment and 2 after treatment. During the activity, VAS recorded 10 before treatment became 2 after treatment.
KEYWORDS
Lumbar spondylosis, katishoola, spondylosis, case report
INTRODUCTION
“Spondylolysis” is the medical term for a small crack (fracture) between two vertebrae in your spine. When this affects the Lumbar vertebrae, then it is called as Lumbar spondylosis.
Lumbar spondylosis is an age-related degeneration of the vertebrae and disks of the lower back. These changes are often called degenerative disk disease and osteoarthritis. The common condition is marked by the breakdown of one or more of the disks that separate the bones of the spine. The disks provide cushioning between the vertebrae and absorb pressure put on the spine. Although most people experience some degeneration of the spine as they age, not everyone experiences back pain.
As a disk degenerates, bone spurs may form at the edges of the vertebrae. Bone spurs may also compress the spinal nerves, leading to weakness or numbness in the arms or legs. If bone spurs compress the spinal cord, you may develop problems with walking and bladder and bowel control. Over time, a degenerating disc may break down completely, leaving no space between two vertebrae, which can result in impaired movement, pain, and nerve damage. The pressure can cause pain, weakness, and numbness in the back and the legs.
Causes: The most common causes of pars fractures include:
Overuse, Repetitive motions that put stress on your low back cause wear and tear on your vertebrae. Over time, this damage can add up to cause a pars fracture. Doing physical work for your job, playing contact sports and repeatedly injuring your low back can all damage your vertebrae.
- Growth spurts: Some kids and teens develop spondylolysis when they’re going through a growth spurt — a period when their bodies are physically growing and changing quickly.
- Genetics: Some people are born with thinner vertebrae. This can make you more likely to experience a pars fracture.
Symptoms and Diagnosis: Symptoms of spondylosis may vary from none to mild to severe. The most common symptom is low back pain. The specialists diagnose spondylosis based on the history of symptoms, a physical exam, and imaging tests that may include X-rays, CT scan, or MRI.
Prognosis: The management of the condition depends on the extent of damage. As this is age related degeneration, this cannot be completely cured. But the symptoms can be addressed and the deterioration can be prevented. When the damage is severe, then surgery is recommended.
General line of treatment: Most people with lumbar spondylosis can be treated with nonsteroidal anti-inflammatory drugs or pain relievers, heat or ice applications, and physical therapy. People who still experience pain or are significantly restricted in their daily movements after trying more conservative treatments may consider surgery to remove the deteriorated disk and fuse the two vertebrae. Surgery may be recommended for patients who have severe or high-grade slippage of the vertebra, such as when more than 50% of the fractured vertebra slips forward on the vertebra below it.
PATIENT INFORMATION
The patient is a 63 year old female, known case of Diabetes mellitus and Hypertension, who presented with low backache with stiffness for last 4 to 5 years. She consulted an Allopathic doctor and was prescribed pain killers. She was recommended surgical management. The patient was not willing to undergo surgery, and so opted for Ayurveda.
No relevant family/genetic/surgical history.
Psychosocial history- Stressed
CLINICAL FINDINGS
Only general examination was done.
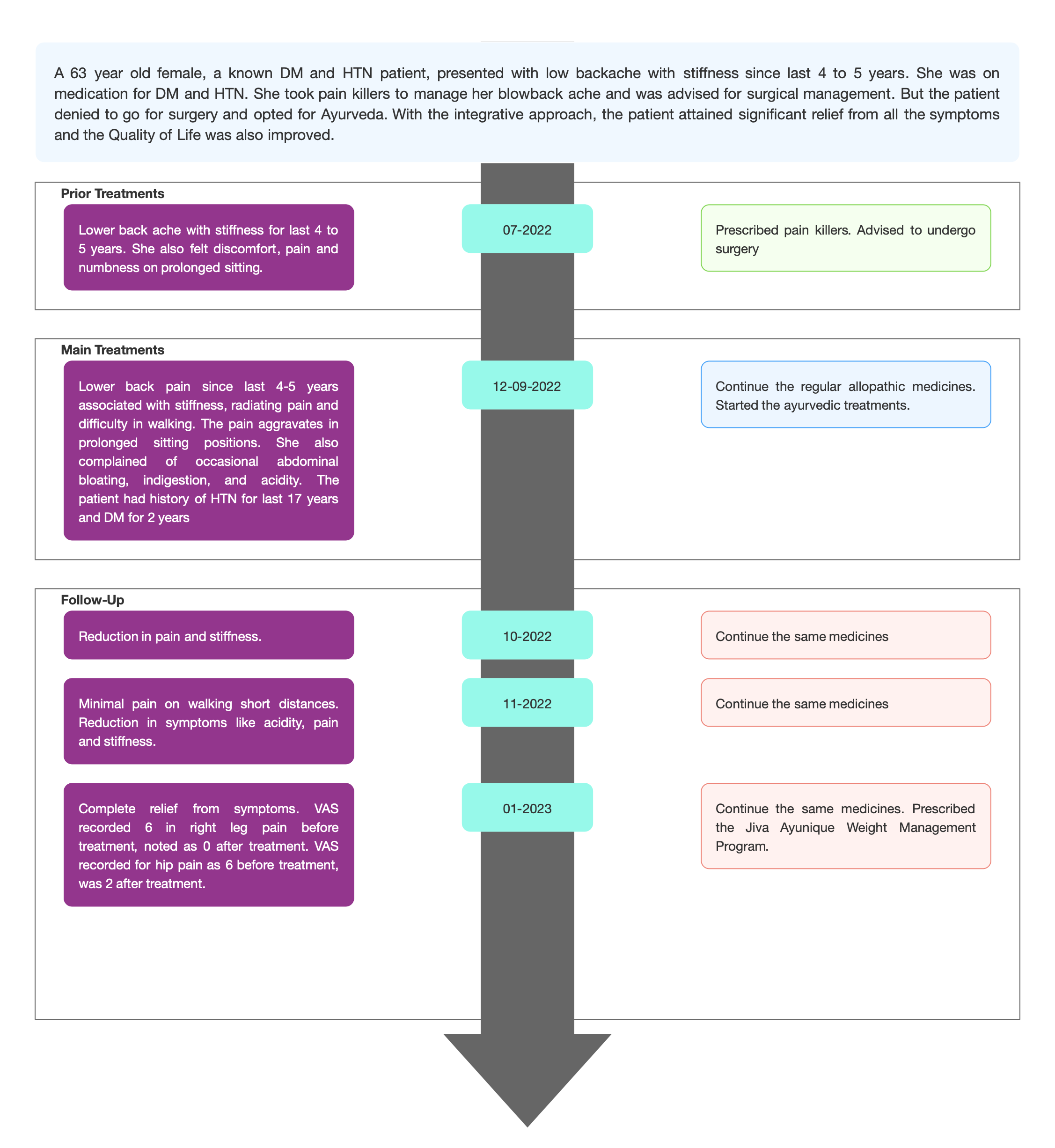
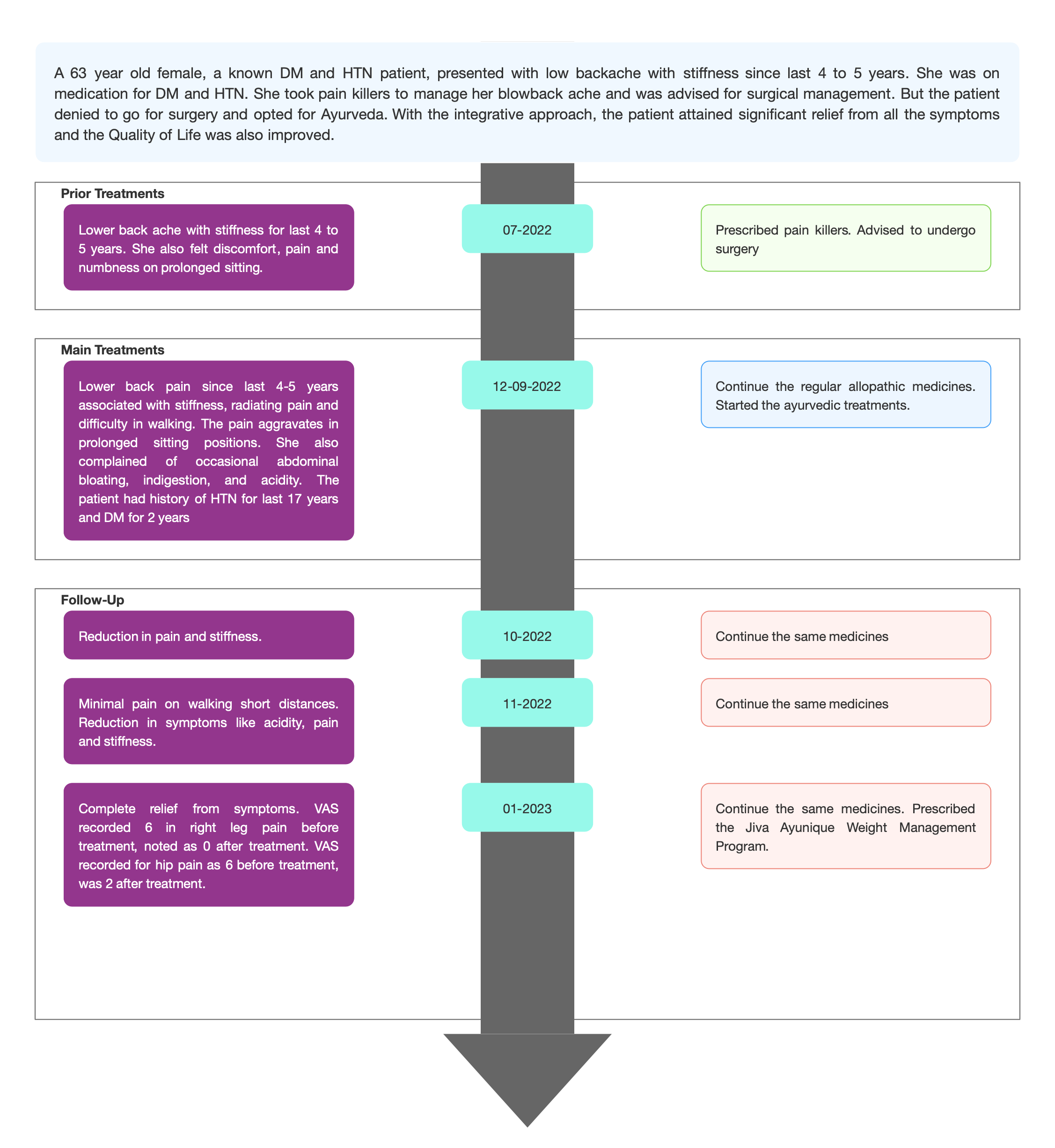
TIMELINE
Image 1. Timeline of events added below
DIAGNOSTIC ASSESSMENT
Modern Diagnostic parameter; The biomedical diagnosis was confirmed by the Ayurvedic physician based on the clinical evaluation and the X Ray done at the baseline.
Table 1. Assessment of symptoms at baseline
Complaints
Matrix
Rest - Before
Activity Before
Lower back pain
VAS
8/10
10/10
Stiffness over Lower back region
H/M/L
H
H
Pain over R leg
VAS
6/10
7/10
Pain over Hip
VAS
6/10
8/10
Acidity
H/M/L
H
Controlled well
Image 1. Baseline X Ray of the lumbar spine dated 12.9.2022

Ayurvedic Assessment was done based on the presenting complaints and clinical evaluation. The treating physician confirmed the Ayurvedic diagnosis as Kati shoola.
Differential Diagnosis-
Lumbosacral disc injuries
Lumbosacral discogenic pain syndrome
Lumbosacral facet syndrome
Lumbosacral spine acute bony injuries
Lumbosacral spine sprain/strain injuries
Lumbosacral spondylolisthesis.
Based on the clinical examination and the X Ray available, the above mentioned diseases were ruled out.
Prognosis- The prognosis of the patients with conservative management is good. If the patient does not respond to conservative management, surgical intervention is advised. In this case, considering its chronicity, surgical management was advised by the allopathic doctor. With the integrative approach, the patient attained significant relief from all the symptoms and the quality of life was also improved.
THERAPEUTIC INTERVENTION
Refer the tab ‘Treatment’ in the Portal.
FOLLOW-UP AND OUTCOMES
The patient had 4 follow ups in total. Each follow up, the symptoms of pain, stiffness, difficulty in movement and acidity were observed and documented.
Clinician-based assessment; After 8 months of treatment, patient is free from itching and pus discharge. Swelling and pain reduced. After 1 and a half years of treatment, the patient got relief from all the symptoms. The abscess has completely healed.
Table 2. Physician’s assessment of symptoms
Symptoms
Sep 2022
Oct 2022
Nov 2022
Dec 2022
Jan 2023
Pain
++++
++
+
Absent
Absent
Stiffness
++++
+
++
Absent
Absent
Difficulty in walking
++++
+++
++
+
Absent
Acidity
++++
++
+
Absent
Absent
Table 3. Patient’s assessment of symptoms
Complaints
Matrix
Rest
Before After
Activity
Before After
Lower back pain
VAS
8/10 2/10
10/10 2/10
Stiffness over Lower back region
H/M/L
H Nil
H Nil
Pain over R leg
VAS
6/10 No pain
7/10 No pain
Pain over Hip
VAS
6/10 2/10
8/10 2/10
Acidity
H/M/L
H
Controlled well Absent
After 1 month of treatment, there was a reduction in pain and stiffness. After 2 months, significant reduction in pain, stiffness and acidity, reduced pain while walking for short distance. After 3 months, no pain and stiffness, no pain while walking for short distances: Acidity- absent;
Pain - present after stepping/ walking for long distance. The patient got complete relief from symptoms in 5 months.Intervention adherence and tolerability – The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment- Subjective parameters were the main assessment tools.
Adverse and unanticipated events; None reported
DISCUSSION:
The patient had been suffering from the condition since 4-5 years, and there was no relief inspite of taking pain killers. The prognosis of the patients with conservative management is good. If the patient does not respond to conservative management, surgical intervention is advised. In this case, considering its chronicity, surgical management was advised by the allopathic doctor. With the integrative approach, the patient attained significant relief from all the symptoms and the quality of life was also improved.
PATIENT’S PERSPECTIVE
Not available.
LEARNING POINTS/TAKE HOME MESSAGES
This case report demonstrates the successful Ayurvedic management of Lumbar Spondylosis in a female patient, who was suffering from the condition since 4-5 years. She had tried painkillers and was advised surgery for better management. With 5 months of Ayurvedic treatment, the patient got complete relief from symptoms and the quality of life improved.
INFORMED CONSENT
Written consent obtained from patient for publishing of the case report in the Portal
ACKNOWLEDGEMENTS
None
CONFLICT OF INTEREST
None declared.
FUNDING
None
REFERENCE
-
Immersive Learning
-
Modern Diagnosis
MODERN DIAGNOSIS: Lumbar spondylosis
ABOUT THE DISEASE:
“Spondylolysis” is the medical term for a small crack (fracture) between two vertebrae in your spine. When this affects the Lumbar vertebrae, then it is called as Lumbar spondylosis.
Lumbar spondylosis is an age-related degeneration of the vertebrae and disks of the lower back. These changes are often called degenerative disk disease and osteoarthritis. The common condition is marked by the breakdown of one or more of the disks that separate the bones of the spine. The disks provide cushioning between the vertebrae and absorb pressure put on the spine. Although most people experience some degeneration of the spine as they age, not everyone experiences back pain.
As a disk degenerates, bone spurs may form at the edges of the vertebrae. Bone spurs may also compress the spinal nerves, leading to weakness or numbness in the arms or legs. If bone spurs compress the spinal cord, you may develop problems with walking and bladder and bowel control. Over time, a degenerating disc may break down completely, leaving no space between two vertebrae, which can result in impaired movement, pain, and nerve damage. The pressure can cause pain, weakness, and numbness in the back and the legs.
Causes: The most common causes of pars fractures include:
Overuse, Repetitive motions that put stress on your low back cause wear and tear on your vertebrae. Over time, this damage can add up to cause a pars fracture. Doing physical work for your job, playing contact sports and repeatedly injuring your low back can all damage your vertebrae.
- Growth spurts: Some kids and teens develop spondylolysis when they’re going through a growth spurt — a period when their bodies are physically growing and changing quickly.
- Genetics: Some people are born with thinner vertebrae. This can make you more likely to experience a pars fracture.
Symptoms and Diagnosis: Symptoms of spondylosis may vary from none to mild to severe. The most common symptom is low back pain. The specialists diagnose spondylosis based on the history of symptoms, a physical exam, and imaging tests that may include X-rays, CT scan, or MRI.
In this case report, the patient is a 63 year old female, known case of Diabetes mellitus and Hypertension, who presented with low backache with stiffness for last 4 to 5 years. She consulted an Allopathic doctor and was prescribed pain killers. She was recommended surgical management. The patient was not willing to undergo surgery, and so opted for Ayurveda. The diagnosis was confirmed as Lumbar Spondylosis based on the X Ray done at baseline. MRI was suggested, but the reports were not submitted.
In this patient, at baseline pain, stiffness, difficulty in walking and acidity were ++++
Table 1. Assessment of symptoms at baseline
Complaints
Matrix
Rest - Before
Activity Before
Lower back pain
VAS
8/10
10/10
Stiffness over Lower back region
H/M/L
H
H
Pain over R leg
VAS
6/10
7/10
Pain over Hip
VAS
6/10
8/10
Acidity
H/M/L
H
Controlled well
Image 1. Baseline X Ray of the lumbar spine dated 12.9.2022

Prognosis: The management of the condition depends on the extent of damage. As this is age related degeneration, this cannot be completely cured. But the symptoms can be addressed and the deterioration can be prevented. When the damage is severe, then surgery is recommended.
General line of treatment: Most people with lumbar spondylosis can be treated with nonsteroidal anti-inflammatory drugs or pain relievers, heat or ice applications, and physical therapy. People who still experience pain or are significantly restricted in their daily movements after trying more conservative treatments may consider surgery to remove the deteriorated disk and fuse the two vertebrae. Surgery may be recommended for patients who have severe or high-grade slippage of the vertebra, such as when more than 50% of the fractured vertebra slips forward on the vertebra below it.
Reference
-
Ayurveda Diagnosis
AYURVEDA DIAGNOSIS: Kati shoola
ABOUT THE DISEASE:
In this case report, the patient is a 63 year old female, known case of Diabetes mellitus and Hypertension, who presented with low backache with stiffness for last 4 to 5 years. The biomedical diagnosis was Lumbar spondylosis based on the X Ray at baseline. The ayurvedic diagnosis is Kati shoola.
Kati refers to ‘low back’ (hip) and shoola refers ‘pain’. The other terms that are generally used to explain this condition are ‘katigraha’, ‘prishtagraha’etc, which are included under Vata pradosaja vyadhi. This is mostly expressed as a symptom in many diseases. In the classical textbooks of ayurveda, this is not being handled as a major or separate disease entity. But assessing the presentation, the nidana can be proposed and the cikitsa can be formulated.
Causative factors:
. Intake of dry, light, bitter, pungent and cold food
. Less food intake
. Fasting or less nutritive food
. Intake of mudga (green gram), masura (red lentil), kalaya (peanut) etc
. Over-exercise
. Long walk
. Fall or injury to the back
. Injury to the vital points
. Weight lifting
. Improper lying
. Brisk walk
. Excess sexual indulgence
. Suppression of the urges
. Work exhaustion
. Stress
. Grief
. Fear
. Dissatisfaction
. Emaciation
Clinical features:
Low back ache may be a pre-monitory (prodromal) symptom in fistula in ano, sciatica, gouty arthritis, hernia, emaciation disorder etc. Pain is concned to lower part of the spine (back bone) especially lumbar region or lumbo-sacral area (rarely sacro-iliac region also). If it is secondary, earlier history of fall or injury may be associated. Rarely, radiating pain may be complained by the patient towards lower limbs. But it is quite common in low back aches if the defect is in the discs between vertebrae (back bones). Often the movements of lumbo-sacral region like eexion and rotation are hampered either partially or completely.
Low back pain may be found in mild form in case of anemia, sciatica, rheumatoid arthritis, hemorrhoids, urinary calculi, uterine disorders etc also.Line of treatment
The general principles of treatment of vata dosha are adopted in case of katishoola (low back pain). It includes various measures to suit its varied clinical entities, stages and associated complaints.. Snehana (oleation) – by sneha dhara (pouring oil), abhyanga (oil massage), avagaha (tub bath with oil or oleaginous medicaments), kati basti (retaining medicaments on the back) etc.
. Swedana (sudation) –avagaha sweda (sweating treatment with tub bath), pizichil (kayaseka), nadi sweda (sudation through a tubular device – local sudation), panda sweda (sudation through medicated paste or powder) etc.
. Mridu Samshodhana -mild purgation
. Basti (medicated enema) like eranda basti, vaitarana basti, pippalyadianuvasana basti
etc.Sadhyasadhyata: In this patient, the symptoms have a chronic history of 4-5 years. The medical history has been recorded only from July 2022. The prior treatment history is not available. Being ‘cirottha’, this can be declared as Kricchrasadhya.
Rationale of treatment as explained by the Treating physician: The rationale for choosing each medicine has been tabulated and presented.
Table 1. The list of medicines/therapy and the specific rationale
Medicines/ Procedure
Rationale of choosing the medicine
Pedantak churna
Vata-kapha shamana, ama pacana, vedana shamana
Balamoola churna
Vata-kapha shamans, vedana shamana, balya, rasayana
Erandmoola churna
Vata shamana, amapacana, srotoshodhana,recana
Go amrit bhasma
Pitta shamana, vedana shamana
Muktashukti pisti
Pitta shamana, rasayana
Sandhiroghar guggulu
Vata-kapha shaman, pachan, vedana shaman, srotoshodhan
Ekangveer ras
Vata shamana, vedana shamana, rasayana , srotoshodhana
Arogyadayini tab.
Vata-pitta shamana, recana, srotoshodhana, rasayana
Ksheerbala oil
Vata shamana, vedana sthapana, snehana, balya, rasayana.
Maha yograj guggulu
Vata shamana, vedana shamana, srotoshodhana
Reference:
-
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Peedantak Curna Curna 0.75gm Oral- with warm water twice daily 2022-09-12 - 2023-09-17 Patent and Proprietary Medicine Balamoola curna Curna 0.75gm Oral- with warm water twice daily 2022-09-12 - 2023-09-17 Ayurveda Sara Sangraha Erandmoola Curna Curna 0.75gm Oral- with warm water twice daily 2022-09-12 - 2023-09-17 Ayurveda Sara Sangraha Go amrit bhasma Curna 0.125 mg Oral- with warm water twice daily 2022-09-12 - 2023-09-17 Ayurveda Sara Sangraha Muktashukti pisti Curna 0.125 mg Oral- with warm water twice daily 2022-09-12 - 2023-09-17 Ayurveda Sara Sangraha Sandhiroghar guggulu Tablet 1 Oral- with warm water twice daily 2022-09-12 - 2023-09-17 Patent and Proprietary Medicine Sandhiroghar guggulu Tablet 1 Oral- with warm water twice daily 2022-09-12 - 2023-09-17 Patent and Proprietary Medicine Ekangveer ras Tablet 1 Oral- with warm water twice daily 2022-09-12 - 2023-09-17 Patent and Proprietary Medicine Arogyadayini tab. Tablet 1 Oral- with warm water twice daily 2022-09-12 - 2023-09-17 Patent and Proprietary Medicine Ksheerbala Taila Taila 10 drops With milk, at bedtime 2022-09-12 - 2023-09-17 Sahasrayogam. Taila Prakaranam Maha yograj guggulu Tablet 1 Oral- with warm water twice daily 2022-09-12 - 2023-09-17 Ayurveda Sara Sangraha -
Outcome Measures
OUTCOME MEASURES
In this case report, the patient is a 63 year old female, known case of Diabetes mellitus and Hypertension, who presented with low backache with stiffness for last 4 to 5 years. She consulted an Allopathic doctor and was prescribed pain killers. She was recommended surgical management. The patient was not willing to undergo surgery, and so opted for Ayurveda. The diagnosis was confirmed as Lumbar Spondylosis based on the X Ray done at baseline. MRI was suggested, but the reports were not submitted.
Assessment: Subjective parameters were assessed to analyse the outcome of the treatment. Subjective parameters: The patient and the physician assessment, of the symptoms were done before and after treatment, to assess the outcome of the treatment.
Table 1. Patient’s assessment of symptoms
Complaints
Matrix
Rest
Before After
Activity
Before After
Lower back pain
VAS
8/10 2/10
10/10 2/10
Stiffness over Lower back region
H/M/L
H Nil
H Nil
Pain over R leg
VAS
6/10 No pain
7/10 No pain
Pain over Hip
VAS
6/10 2/10
8/10 2/10
Acidity
H/M/L
H
Controlled well Absent
Table 2. Physician’s assessment of symptoms
Symptoms
Sep 2022
Oct 2022
Nov 2022
Dec 2022
Jan 2023
Pain
++++
++
+
Absent
Absent
Stiffness
++++
+
++
Absent
Absent
Difficulty in walking
++++
+++
++
+
Absent
Acidity
++++
++
+
Absent
Absent
After 1 month of treatment, there was a reduction in pain and stiffness. After 2 months, significant reduction in pain, stiffness and acidity, reduced pain while walking for short distance. After 3 months, no pain and stiffness, no pain while walking for short distances: Acidity- absent;
Pain - present after stepping/ walking for long distance. The patient got complete relief from symptoms in 5 months.
-



