Featured Case
-
Abstract
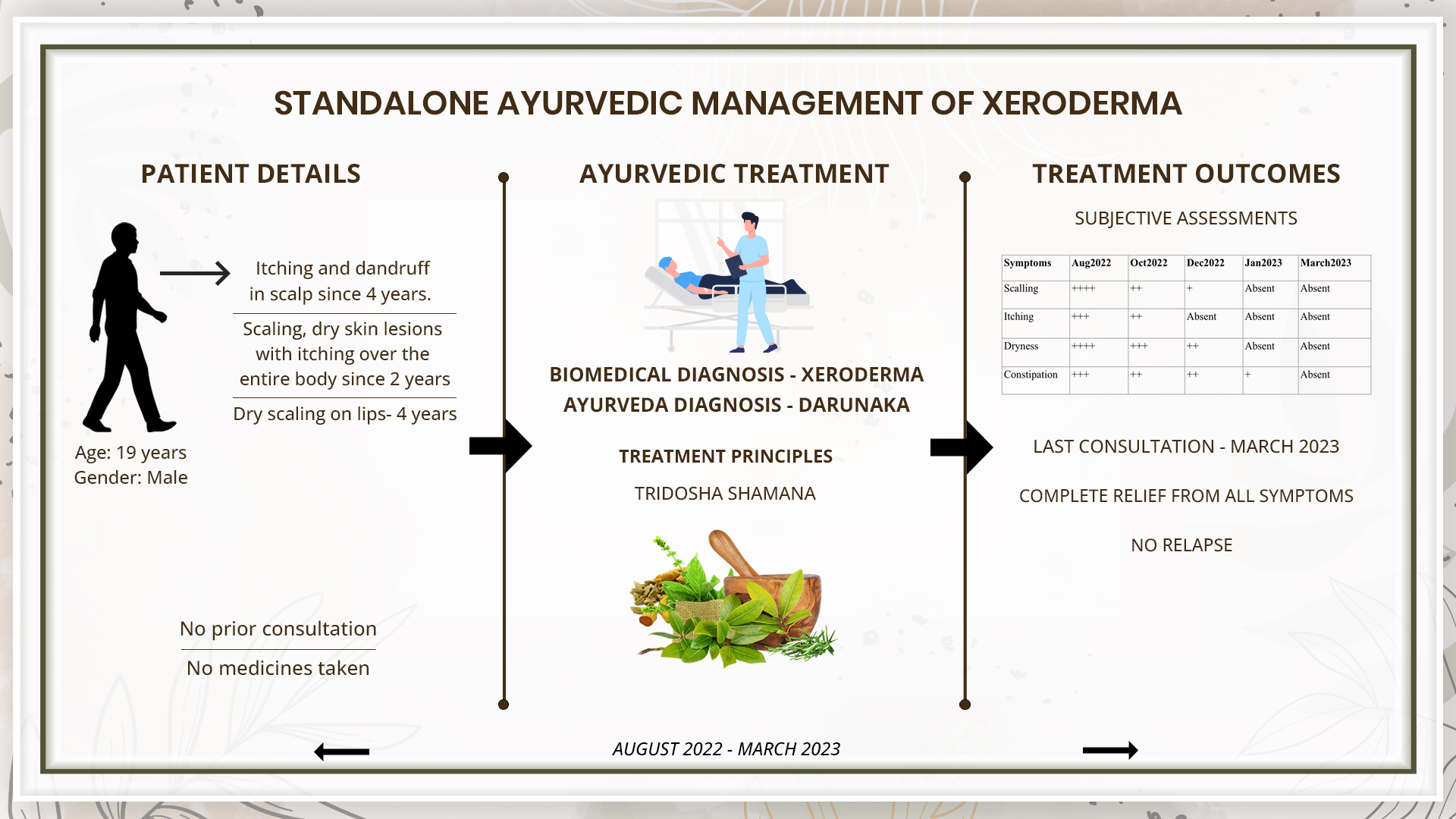
A 19-year-old male patient presented with itching and dandruff on the scalp for 4 years associated with scaling, dry skin lesions, and itching over the entire body for 2 years. There were no prior treatments. The patient consulted Dr Partap Chauhan for the management of this condition. Based on the clinical evaluation, the biomedical diagnosis was made as Xeroderma and the Ayurvedic diagnosis was Darunaka. The line of treatment was Vata-pitta, vata-kapha, tridosa shamana, sroto shodhana and rasayana cikitsa. With 7 months of Ayurvedic treatment, the patient got complete relief from symptoms. This case report is an example for the successful ayurvedic management of a case of Xeroderma in a patient with a chronic history.
-
Summaries
-
Listen
-
Watch
-
View
-
Read

A 19-year-old male patient presented with itching and dandruff on the scalp for 4 years associated with scaling, dry skin lesions, and itching over the entire body for 2 years. There were no prior treatments. The patient consulted Dr Partap Chauhan for the management of this condition. Based on the clinical evaluation, the biomedical diagnosis was made as Xeroderma and the Ayurvedic diagnosis was Darunaka. The line of treatment was Vata-pitta, vata-kapha, tridosa shamana, sroto shodhana and rasayana cikitsa. With 7 months of Ayurvedic treatment, the patient got complete relief from symptoms. This case report is an example for the successful ayurvedic management of a case of Xeroderma in a patient with a chronic history.
-
-
Timeline
-
Tabulated Summary
-
Narrative
TITLE OF CASE
Standalone ayurvedic management of xeroderma- A case report
Dr Partap Chauhan
ABSTRACT
A 19-year-old male patient presented with itching and dandruff on the scalp for 4 years associated with scaling, dry skin lesions, and itching over the entire body for 2 years. There were no prior treatments. The patient consulted Dr Partap Chauhan for the management of this condition. Based on the clinical evaluation, the biomedical diagnosis was made as Xeroderma and the Ayurvedic diagnosis was Darunaka. The line of treatment was Vata-pitta, vata-kapha, tridosa shamana, sroto shodhana and rasayana cikitsa. With 7 months of Ayurvedic treatment, the patient got complete relief from symptoms. This case report is an example for the successful ayurvedic management of a case of Xeroderma in a patient with a chronic history.
KEYWORDS
Ayurveda, xeroderma, darunaka, case report, dermatitis
INTRODUCTION
Xeroderma, xerosis or xerosis cutis, or simply dry skin, is a skin condition characterised by excessively dry skin.
The medical term xeroderma, meaning 'dry skin', derives from Greek (xeros) 'dry' (derma) ‘skin'.
Causes: Xeroderma is a very common condition. It happens more often in the winter when the cold air outside and the hot air inside create a low relative humidity. This causes the skin to lose moisture and it may crack and peel. Bathing or hand washing too frequently, especially if one is using harsh soaps, can contribute to xeroderma. Xeroderma can be caused by a deficiency of vitamin A, vitamin D, zinc, systemic illness, severe sunburn, or some medication. Xeroderma can be caused by choline inhibitors. Detergents such as washing powder and dishwashing liquid can cause xeroderma.
Prevention: Many creams and lotions, commonly based on vegetable oils/butters, petroleum oils/jellies, and lanolin are widely available. As a preventive measure, such products may be rubbed onto the affected area as needed (often every other day) to prevent dry skin. The skin is then patted dry to prevent the removal of natural lipids from the skin. Taking a shower or washing hands with special moisturising soaps or body washes can protect the skin from drying out further.
Diagnostic criteria: Diagnosis of xeroderma is based on clinical evaluation. Xeroderma can usually be differentiated by inflammatory disorders such as atopic dermatitis and psoriasis by the absence of erythema in xeroderma. Unlike the fine white scales of xeroderma, ichthyosis is characterised by fish-like scales.
Prognosis: Xeroderma is generally benign and may persist for years. The prognosis is favorable with avoidance of triggers and incorporating a skincare regimen focused on gentle cleansing and adequate moisturising. Many people with the condition have a shortened lifespan from developing skin cancer at a very young age. Taking steps to prevent sun damage early in life can increase the chances of living longer.
PATIENT INFORMATION
The patient is a 19 year old male who complained of itching and dandruff in scalp since 4 years associated with scaling, dry skin lesions, and itching over the entire body for 2 years. There were no prior consultation or treatment. Based on the clinical evaluation, the ayurvedic physician made the biomedical diagnosis as Xeroderma and ayurvedic diagnosis as Darunaka. This was a chronic condition, with no prior medical intervention.
No relevant family/genetic/surgical history.
Psychosocial history- Is stressed
CLINICAL FINDINGS
On examination: Rough , Itchy and Flaky skin from the scalp.
Scaling ++++
Itching +++
Dryness ++++TIMELINE
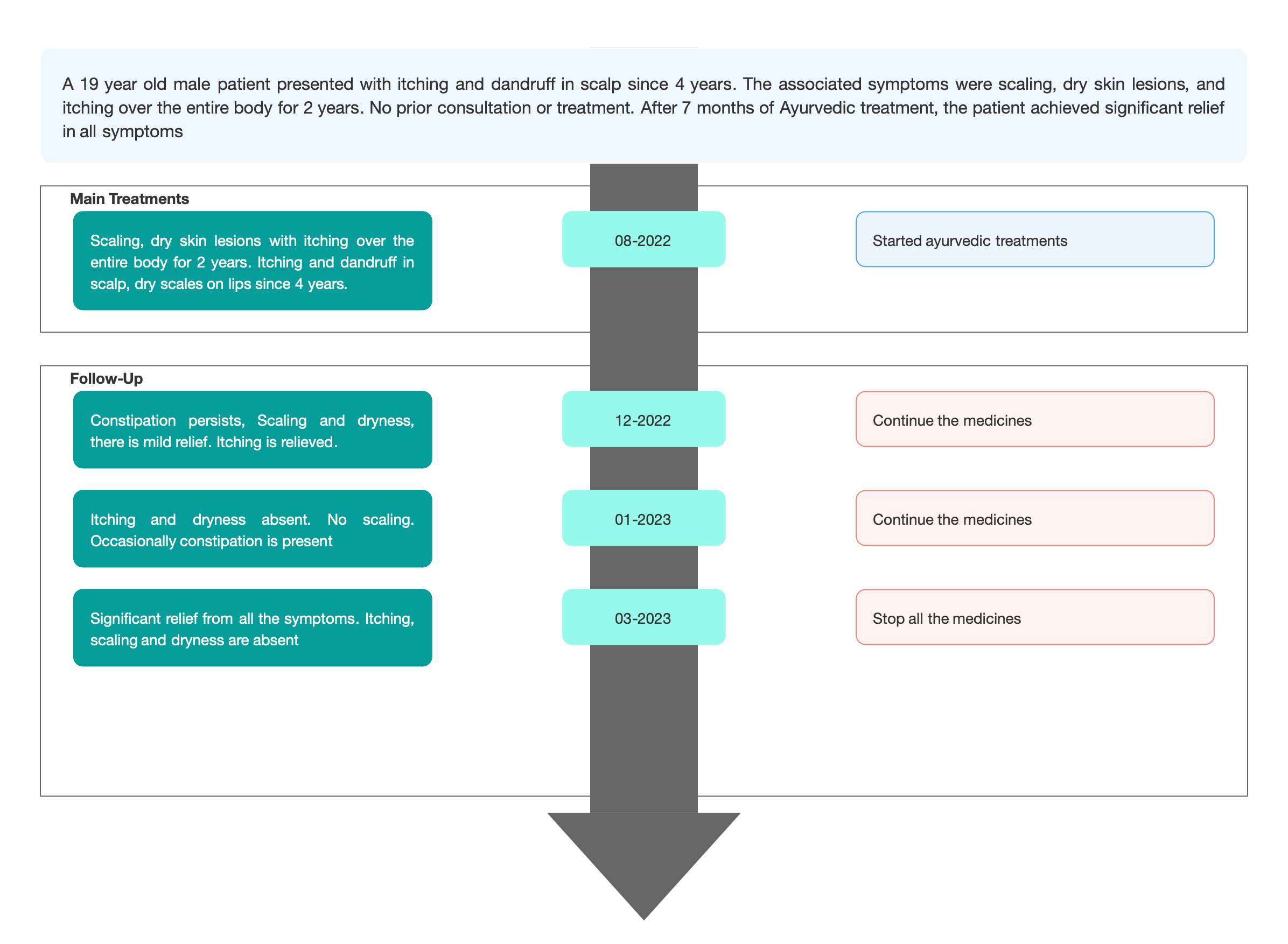
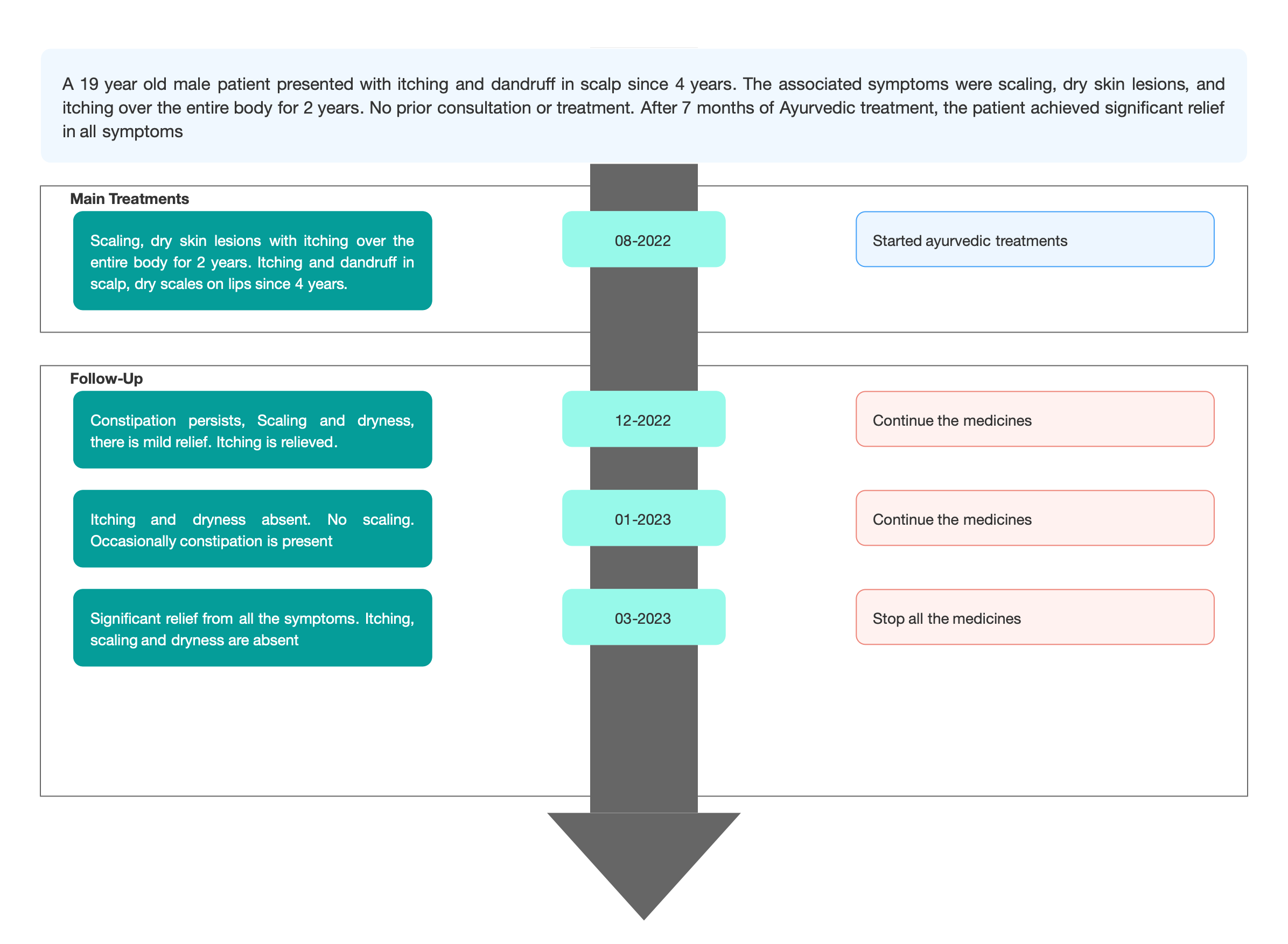
Image 1. Timeline of events added below
DIAGNOSTIC ASSESSMENT
Modern Diagnostic parameter; The biomedical diagnosis was confirmed by the Ayurvedic physician based on the clinical evaluation.
Ayurvedic Assessment was done based on the presenting complaints and clinical evaluation. The treating physician confirmed the Ayurvedic diagnosis as Darunaka.
Differential Diagnosis-
Ichthyosis Vulgaris
Atopic dermatitis
Stasis dermatitis
Irritant contact dermatitis
Allergic contact dermatitis
Nummular dermatitis
Scabies. The physician ruled out these conditions based on clinical evaluation
Prognosis- Xeroderma is generally benign and may persist for years. The prognosis is favorable with avoidance of triggers and incorporating a skincare regimen focused on gentle cleansing and adequate moisturising. In this case, the patient got complete relief from symptoms in 7 months.
THERAPEUTIC INTERVENTION
Refer the tab ‘Treatment’ in the Portal.
FOLLOW-UP AND OUTCOMES
The patient had 4 follow ups in total. Each follow up, the symptoms of itching, scaling, dryness and constipation were documented.
Table 1. Symptoms improvement -date wise observation
Symptoms
Aug 2022
Oct 2022
Dec 2022
Jan 2023
March 2023
Scaling
++++
++
+
Absent
Absent
Itching
+++
++
Absent
Absent
Absent
Dryness
++++
+++
++
Absent
Absent
Constipation
+++
++
++
+
Absent
Clinician-based assessment; Complete relief from all the symptoms at the end of 7 months.
Patient-assessed; Not relevant
Intervention adherence and tolerability – The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment- Subjective parameters were the main assessment tools.
Adverse and unanticipated events; None reported
DISCUSSION:
Rheumatoid arthritis has no cure and is a progressive disease associated with morbidity and increased mortality. All individuals will experience multiple exacerbations and, without treatment, tend to have poor outcomes with disability and increased mortality. Here, the ayurvedic diagnosis was made as Amavata and the line of treatment followed was tridosa shamana, sroto shodhana, ama pacana, balya and rasayana.
PATIENT’S PERSPECTIVE
Not available.
LEARNING POINTS/TAKE HOME MESSAGES
Xeroderma is generally benign and may persist for years. The prognosis is favourable with avoidance of triggers and incorporating a skincare regimen focused on gentle cleansing and adequate moisturising. In this patient, with 7 months of ayurvedic treatment, he got complete relief from symptoms. The medicines mainly targeted at addressing the symptoms and all teak roga cikitsa sutra was followed.
INFORMED CONSENT
Written consent obtained from patient for publishing of the case report in the Portal
ACKNOWLEDGEMENTS
None
CONFLICT OF INTEREST
None declared.
FUNDING
None
REFERENCE
- Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 978-1-4160-2999-1.[page needed]
- "Medical Definition of Xeroderma". MedTerms. 29 March 2021. Retrieved 17 May 2022.
- "Dry Skin (Xeroderma)". Merck Manuals. May 2021. Retrieved 17 May 2022.
- "Managing Dry Skin". US Pharmacist. 30 (3). 2005. Retrieved 17 May 2022.
- R. Wolf (1996). "The Lanolin Paradox". Dermatology. 192 (3): 198–202.
- Zirwas MJ; Stechschulte SA (2008). "Moisturizer allergy: diagnosis and management". J Clin Aesthet Dermatol. 1 (4): 38–44.
- my.clevelandclinic.org › health › diseases
-
Immersive Learning
-
Modern Diagnosis
MODERN DIAGNOSIS: Xeroderma
ABOUT THE DISEASE:
Xeroderma, xerosis or xerosis cutis, or simply dry skin, is a skin condition characterised by excessively dry skin.
The medical term xeroderma, meaning 'dry skin', derives from Greek (xeros) 'dry' (derma) ‘skin'.
Causes: Xeroderma is a very common condition. It happens more often in the winter when the cold air outside and the hot air inside create a low relative humidity. This causes the skin to lose moisture and it may crack and peel. Bathing or hand washing too frequently, especially if one is using harsh soaps, can contribute to xeroderma. Xeroderma can be caused by a deficiency of vitamin A, vitamin D, zinc, systemic illness, severe sunburn, or some medication. Xeroderma can be caused by choline inhibitors. Detergents such as washing powder and dishwashing liquid can cause xeroderma.
Prevention: Many creams and lotions, commonly based on vegetable oils/butters, petroleum oils/jellies, and lanolin are widely available. As a preventive measure, such products may be rubbed onto the affected area as needed (often every other day) to prevent dry skin. The skin is then patted dry to prevent the removal of natural lipids from the skin. Taking a shower or washing hands with special moisturising soaps or body washes can protect the skin from drying out further.
Diagnostic criteria: Diagnosis of xeroderma is based on clinical evaluation. Xeroderma can usually be differentiated by inflammatory disorders such as atopic dermatitis and psoriasis by the absence of erythema in xeroderma. Unlike the fine white scales of xeroderma, ichthyosis is characterised by fish-like scales.
Prognosis: Xeroderma is generally benign and may persist for years. The prognosis is favorable with avoidance of triggers and incorporating a skincare regimen focused on gentle cleansing and adequate moisturising. Many people with the condition have a shortened lifespan from developing skin cancer at a very young age. Taking steps to prevent sun damage early in life can increase the chances of living longer.
In this case report, the patient is a 19 year old male who complained of itching and dandruff in scalp since 4 years associated with scaling, dry skin lesions, and itching over the entire body for 2 years. There were no prior consultation or treatment. Based on the clinical evaluation, the ayurvedic physician made the biomedical diagnosis as Xeroderma and ayurvedic diagnosis as Darunaka. This was a chronic condition, with no prior medical intervention.
Treatment: Repeated application (typically over a few days) of emollients or skin lotions/creams to the affected area will likely result in quick alleviation of xeroderma. In particular, the application of highly occlusive barriers to moisture, such as petrolatum, vegetable oils/butters, and mineral oil have been shown to provide excellent results. Many individuals find specific commercial skin creams and lotions (often comprising oils, butters, and or waxes emulsified in water) quite effective (although individual preferences and results vary among the wide array of commercially available creams).
Lanolin, a natural mixture of lipids derived from sheep's wool, helps replace natural lipids in human skin and has been used since ancient times (and in modern medicine) as among the most powerful treatments for xeroderma. Some people may, however, have allergies to lanolin, producing the opposite of the desired effect.[5] Also, pure lanolin is a thick waxy substance which, for many individuals, proves difficult and inconvenient for general use on dry skin (especially over large areas of the body).
Reference
- Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 978-1-4160-2999-1.[page needed]
- "Medical Definition of Xeroderma". MedTerms. 29 March 2021. Retrieved 17 May 2022.
- "Dry Skin (Xeroderma)". Merck Manuals. May 2021. Retrieved 17 May 2022.
- "Managing Dry Skin". US Pharmacist. 30 (3). 2005. Retrieved 17 May 2022.
- R. Wolf (1996). "The Lanolin Paradox". Dermatology. 192 (3): 198–202.
- Zirwas MJ; Stechschulte SA (2008). "Moisturizer allergy: diagnosis and management". J Clin Aesthet Dermatol. 1 (4): 38–44.
- my.clevelandclinic.org › health › diseases
-
Ayurveda Diagnosis
AYURVEDA DIAGNOSIS: Darunaka
ABOUT THE DISEASE:
The ayurvedic physician has correlated Xeroderma to darunaka. Darunaka means difficult to bear or tolerate. This is commonly referred to as dandruff, a disorder that affects the scalp. It has been reported that Darunaka (Seborrhoeic Dermatitis) affect about 4% of the population, and dandruff (which is mild seborrhoeic dermatitis of the scalp) can affect almost half of all adults. It can start at any time after puberty and is slightly commoner in men. It can result in social or self-esteem problems.
The primary symptoms in this patient, were itching and dandruff in the scalp for 4 years. Though the symptoms also affected the entire body, the treating physician connects it to darunaka. Dandruff causes white, dry flakes of dead skin cells to shed from the scalp. Although dandruff rarely causes baldness and hair loss, the itchiness of this condition may most certainly be a cause of concern. If white flakes persist for a long time, the person may experience symptoms of seborrhea, psoriasis, or eczema.
Darunaka is a Kapalagataroga but Acharya Sushruta has described this disease as a Kshudraroga due to the vitiation of Vata and Kapha Doshas with symptoms like Kandu (itching on scalp), Keshachyuti (falling of hair), Swapa(abnormalities of touch sensation on scalp), Rookshata (roughness or dryness of the scalp) and Twaksphutana (breaking or cracking of the scalp skin). Seborrhoeic Dermatitis, an irritative disease of the scalp in which shedding of dead tissue from the scalp with itching sensation is the cardinal feature which can be correlated with Darunaka.
In this case report, the patient is a 19 year old male who complained of itching and dandruff in scalp since 4 years associated with scaling, dry skin lesions, and itching over the entire body for 2 years. There were no prior consultation or treatment. Based on the clinical evaluation, the ayurvedic physician made the biomedical diagnosis as Xeroderma and ayurvedic diagnosis as Darunaka. This was a chronic condition, with no prior medical intervention.
Causative factors: Madhava Nidana in Kshudra roga adhyaya explains that non-application of Kesha Taila (oiling of head), improper cleaning, sleeping during day time, night vigil, exposure to dust, hot weather etc. are causative factors for Darunaka.
Prognosis: This being categorised as Kshudra roga, the management can be done easily. Vaghbhata specifically mentions that it is sadhya in nature.
Rationale of Treatment: The general line of treatment for Tvak roga was followed. The symptoms like itching, scaling and dry skin lesions were also addressed.
Table 1. The medicines and the specific rationale for choosing them are being tabulated as explained by the treating physician
MEDICINE
RATIONALE Arogyadayini ras Vata-pitta shamana, pitta rechana, srotoshodhana Tikatras guggulu Vatakapha shamana, rakta shodhana, sroto shodhana Nimbadi vati Vatakapha shamana, raktashodhana, kandudgha, krimighna Saaf Saaf tab Srotoshodhana, Amapacana Kumari asav Tridosha shamana, srotoshodhana, rasayana Panchtikta Ghrta Vatakapha shamana, raktashodhana, srotoshodhana, rasayana, snehana Reference
1. Kumari Archana et.al. An ayurvedic approach in the management of darunaka (seborrhoeic dermatitis): a case study. Vol.10; Issue: 4; April 2020
-
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Arogyadayini ras Tablet 1 Oral- with warm water twice daily after food 2022-08-29 - 2023-01-03 Patent and Proprietary Medicine Tikatras guggulu Tablet 1 Oral- with warm water twice daily after food 2022-08-29 - 2023-01-03 Patent and Proprietary Medicine Nimbadi Vati Tablet 1 Oral- with warm water twice daily after food 2022-08-29 - 2023-01-03 Patent and Proprietary Medicine Saaf Saaf tab Tablet 2 Oral- with warm water at bedtime 2022-11-25 - 2022-12-30 Patent and Proprietary Medicine Kumari Asav Asava 20 ml Oral, After Dinner 2022-08-29 - 2023-01-03 Sarangadhara Samhita.Madhyamakhanda. 10.18- 27 Pancatikta Ghrta Ghrtam 1 tablespoon Oral- on empty stomach in the morning 2022-08-29 - 2023-01-03 Bhaishajya Ratnavali - Visphotacikitsa Prakarana Neem shampoo Sira snana Required Quantity For hairwash 2022-08-29 - 2023-01-03 Patent and Proprietary Medicine -
Outcome Measures
OUTCOME MEASURES
The patient is a 19 year old male who complained of itching and dandruff in scalp since 4 years associated with scaling, dry skin lesions, and itching over the entire body for 2 years. There were no prior consultation or treatment. Based on the clinical evaluation, the ayurvedic physician made the biomedical diagnosis as Xeroderma and ayurvedic diagnosis as Darunaka. This was a chronic condition, with no prior medical intervention.
Assessment: Subjective parameters were assessed to analyse the outcome of the treatment.
Subjective parameters: The symptoms as proceeding through the treatment were tabulated. Itching, Scaling, Dryness and Constipation were recorded.
Table 1. Symptoms assessed and documented date wise
Symptoms
Aug 2022
Oct 2022
Dec 2022
Jan 2023
March 2023
Scaling
++++
++
+
Absent
Absent
Itching
+++
++
Absent
Absent
Absent
Dryness
++++
+++
++
Absent
Absent
Constipation
+++
++
++
+
Absent
After 2 months of treatment, there was a significant reduction in symptoms. After 4 months, itching completely relieved. Mild dryness and scaling persists. After 5 months, only constipation persists. He got complete relief from itching, scaling and dryness. After 6 months, complete relief from all the symptoms.
Objective parameters: None
-


