Featured Case
-
Abstract
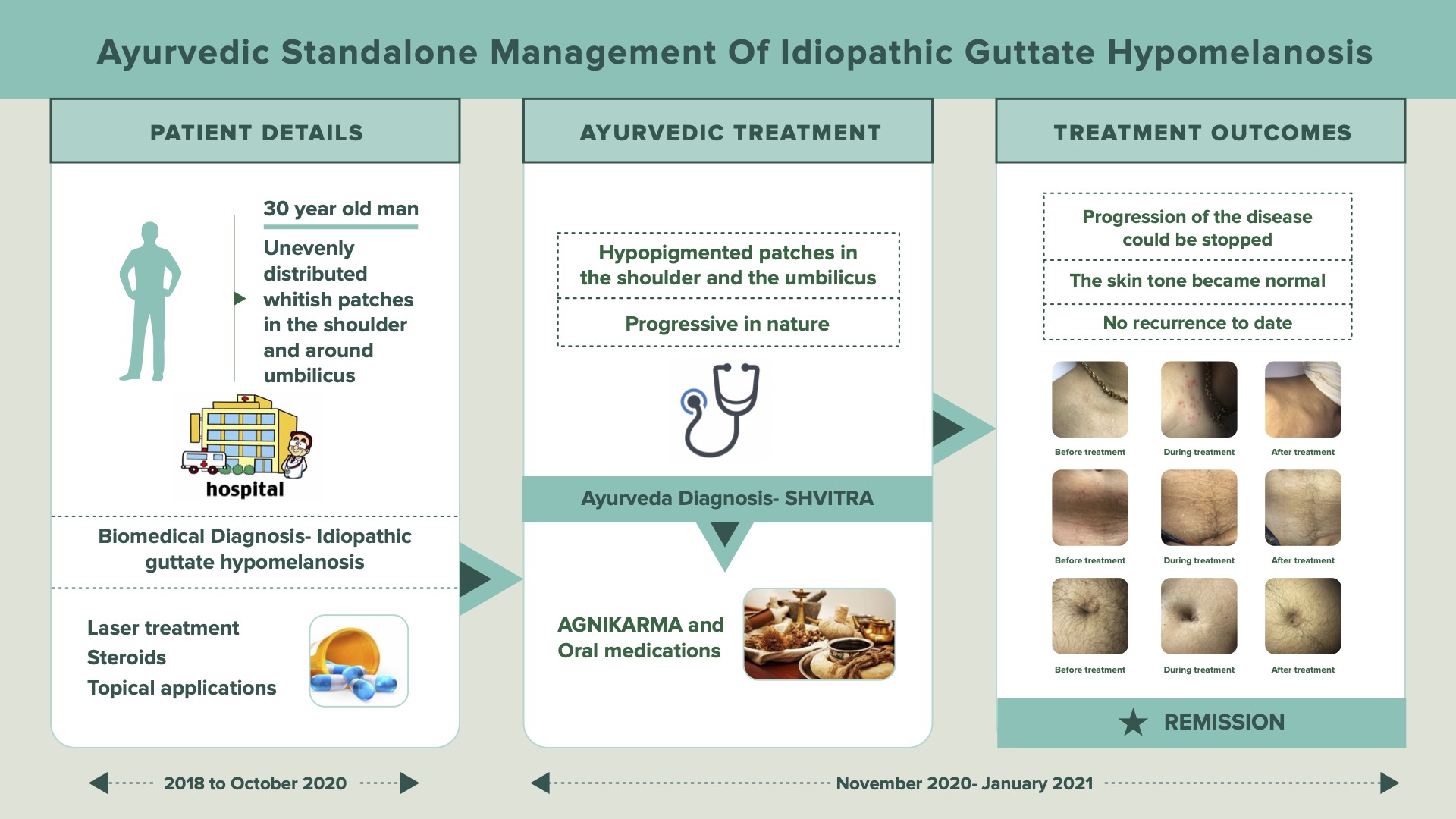
A 30-year-old male was suffering from whitish patches unevenly distributed over the skin in the shoulder region and around the umbilical region. He consulted a general practitioner, and a clinical diagnosis was made as Idiopathic Guttate Hypomelanosis. He underwent Laser treatment and the local application of steroids. After more than 1 year of treatment, there was only temporary relief. The patient now consulted Dr Jyoti Joshi, presenting with hypopigmented patches, progressive in nature, over the skin in the shoulder and umbilical region since 2018. This clinical condition was diagnosed as Shvitra. Agnikarma was the main line of treatment and oral medications were also given. Agnikarma were done once a week, for 3 weeks, with 22 number silver needle. Bakuci Tailam, was applied after this procedure at the spot of Agnikarma. A follow up done after 21 days revealed a significant reduction in hypopigmentation. After 1 month of treatment, the progression of the disease could be stopped entirely, and the hypopigmentation was seen diminishing by its colour and size. The patient started following a healthy diet and lifestyle that supported rapid recovery. There has been no recurrence to date.
-
Summaries
-
Listen
-
Watch
-
View
-
Read

A 30-year-old male was suffering from whitish patches unevenly distributed over the skin in the shoulder region and around the umbilical region. He consulted a general practitioner, and a clinical diagnosis was made as Idiopathic Guttate Hypomelanosis. He underwent Laser treatment and the local application of steroids. After more than 1 year of treatment, there was only temporary relief. The patient now consulted Dr Jyoti Joshi, presenting with hypopigmented patches, progressive in nature, over the skin in the shoulder and umbilical region since 2018. This clinical condition was diagnosed as Shvitra. Agnikarma was the main line of treatment and oral medications were also given. Agnikarma were done once a week, for 3 weeks, with 22 number silver needle. Bakuci Tailam, was applied after this procedure at the spot of Agnikarma. A follow up done after 21 days revealed a significant reduction in hypopigmentation. After 1 month of treatment, the progression of the disease could be stopped entirely, and the hypopigmentation was seen diminishing by its colour and size. The patient started following a healthy diet and lifestyle that supported rapid recovery. There has been no recurrence to date.
-
-
Timeline
-
Tabulated Summary
-
Narrative
TITLE OF CASE
Standalone successful ayurvedic management of Idiopathic Guttate Hypomelanosis- A case report
Dr Jyoti Joshi
ABSTRACT
A 30-year-old male was suffering from whitish patches unevenly distributed over the skin in the shoulder region and around the umbilical region. He consulted a general practitioner, and a provisional diagnosis was made as Idiopathic Guttate Hypomelanosis. He underwent Laser treatment and the local application of steroids. After more than 1 year of treatment, there was no satisfactory relief. The patient now consulted Dr Jyoti Joshi, presenting with Hypopigmented patches, progressive in nature, over the skin in the shoulder and umbilical region since 2018. This clinical condition was diagnosed as Shvitra. Agnikarma was the main line of treatment and oral medications were also given. Agnikarma was done once a week, for 3 weeks, with 22 number silver needle. Bakuci Tailam was applied after this procedure at the spot of Agnikarma. A follow-up done after 21 days revealed a significant reduction in hypopigmentation. After 1 month of treatment, the progression of the disease could be stopped entirely, and the hypopigmentation was seen diminishing by its colour and size. The patient started following a healthy diet and lifestyle that supported rapid recovery. There has been no recurrence to date.
KEYWORDS
Idiopathic guttate hypomelanosis, standalone, skin disorder, case report, shvitra
INTRODUCTION
Idiopathic guttate hypomelanosis (IGH) is a benign, typically asymptomatic, leukodermic dermatosis of unclear aetiology that is classically seen in elderly, fair-skinned individuals, and often goes unrecognized or undiagnosed. Occasionally, IGH is aesthetically displeasing. However, it is not a dangerous process. Once present, lesions do not remit. Treatment is aimed at improving the cosmesis of lesions. This activity describes the clinical evaluation of idiopathic guttate hypomelanosis and explains the role of the health professional team in coordinating the care of this condition.
Aetiology: The aetiology of IGH remains unknown. Several hypotheses exist, including the notion that this is a manifestation of the skin's normal ageing process, occurs secondary to cumulative chronic sun exposure, or occurs as a result of repeated microtrauma to the skin
Diagnostic criteria: Medical history taking and clinical examination are the basic diagnostic criteria. Given the benign course of IGH, no laboratory, radiographic, or other tests are typically necessary to investigate these patients. Dermoscopy can be a valuable tool in the evaluation of lesions of IGH.
Treatment:
Patients should be reassured that lesions of IGH are benign and that no treatment is necessary. There are no universally accepted efficacious treatments for this condition.
In general, as sunlight is most likely a contributing or potentially even precipitating factor, the use of sunscreens and physical barriers should be recommended for all patients. In addition to photoprotection, treatment for cosmetic purposes are available and have shown promise used alone or in combination. These include cryotherapy, superficial abrasion, topical steroids, topical retinoids, topical calcineurin inhibitors, dermabrasion, topical 88% phenol, fractional carbon dioxide lasers, non-ablative fractional photothermolysis via fractional 1550-nm ytterbium/erbium fiber laser, and excimer light treatment.
PATIENT INFORMATION
A 30-year-old male was suffering from whitish patches unevenly distributed over the skin in the shoulder region and around the umbilical region. He consulted a general practitioner, and a clinical diagnosis was made as Idiopathic Guttate Hypomelanosis
Medical History: He underwent Laser treatment and the local application of steroids. After more than 1 year of treatment, there was no significant relief. The patient now consulted Dr Jyoti Joshi, presenting with Hypopigmented patches, progressive in nature, over the skin in the shoulder and umbilical region since 2018. This was diagnosed as Shvitra.
CLINICAL FINDINGS/PHYSICAL EXAMINATION
On examination of the skin- hypo-pigmented round patches over the skin distributed unevenly around the right side of the chest-shoulder regions and around the umbilical region. There was no pain, itching, burning sensation, or tenderness.
TIMELINE
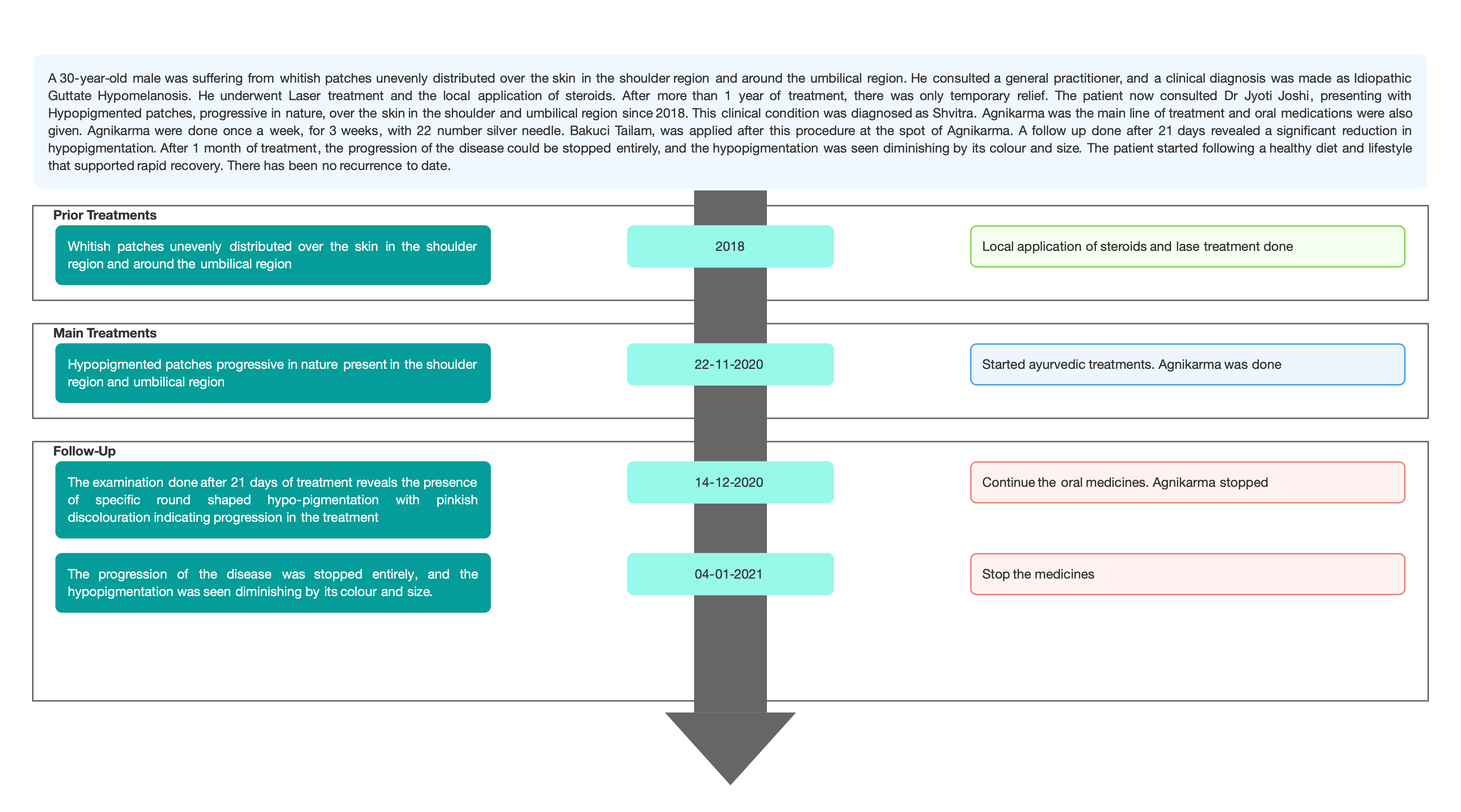
Image 1. Timeline of events added as an attachment.
DIAGNOSTIC ASSESSMENT
Modern Diagnostic parameter: The biomedical diagnosis was made based on the clinical presentation and evaluation.
Image 2. An image of the hypopigmented patches before treatment was added below
Ayurvedic Assessment was done based on the clinical evaluation by the ayurvedic physician.
Differential Diagnosis- This does not apply as the patient came in with a definite diagnosis.
Prognosis- Idiopathic guttate hypomelanosis is a benign condition with a good prognosis; however, once present, lesions do not remit without treatment. In this case, the patient underwent laser treatment and local steroid application. But he was not satisfied with the outcomes, and he discontinued the treatment. After 1 month of Ayurvedic treatment, the progression of the disease could be arrested entirely, and the hypopigmentation was seen diminishing by its colour and size.
THERAPEUTIC INTERVENTION
See the tab ‘Treatment details’
FOLLOW-UP AND OUTCOMES
Follow up done after 21 days, observed a reduction in the hypo-pigmentation
Image 3. The image during treatment is added below
Image 4. The image taken after treatment is added below
Clinician-based assessment; After 1 month of treatment, the progression of the disease was stopped entirely, and the hypopigmentation was seen diminishing by its colour and size. As the patient started following a regular healthy diet, habit and sleep pattern, the clinical features were consistently reducing.
Patient-assessed: Not relevant.
Intervention adherence and tolerability – The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment- By monitoring the patient.
Adverse and unanticipated events; None reported.
DISCUSSION ;
Agnikarma gives the exact application of the required quantity of heat, to heal the affected parts of the skin. After agnikarma, when Bakuci tailam is applied, it helps fasten the process.
PATIENT’S PERSPECTIVE
Not available.
LEARNING POINTS/TAKE-HOME MESSAGES
The 30-year-old male patient diagnosed with Idiopathic guttate hypomelanosis tried allopathic medicines over a period of more than 1 year but did not get satisfactory relief. Moreover, the condition was progressing. A follow-up done after 21 days of treatment, revealed the presence of specific round-shaped hypopigmentation with pinkish discolouration indicating significant outcomes in the treatment With 1 month of Ayurveda treatment, the progressive nature of the disease could be stopped. The hypopigmented patches were seen diminishing in size and shape. This case report demonstrates the successful ayurvedic management of Idiopathic guttate hypomelanosis.
INFORMED CONSENT
Written consent was obtained from the patient to publish the case report.
CONFLICT OF INTEREST
None declared.
FUNDING
None
REFERENCE
- Brown F, Crane JS. Idiopathic Guttate Hypomelanosis. In: Stat Pearls. Treasure Island (FL): Stat Pearls Publishing; September 12, 2022.
- Narahari SR, Aggithaya MG, Suraj KR. A protocol for systematic reviews of Ayurveda treatments. Int J Ayurveda Res. 2010 Oct;1(4):254-67. doi: 10.4103/0974-7788.76791. PMID: 21455455; PMCID: PMC3059450.
Image 1. Timeline of events added below
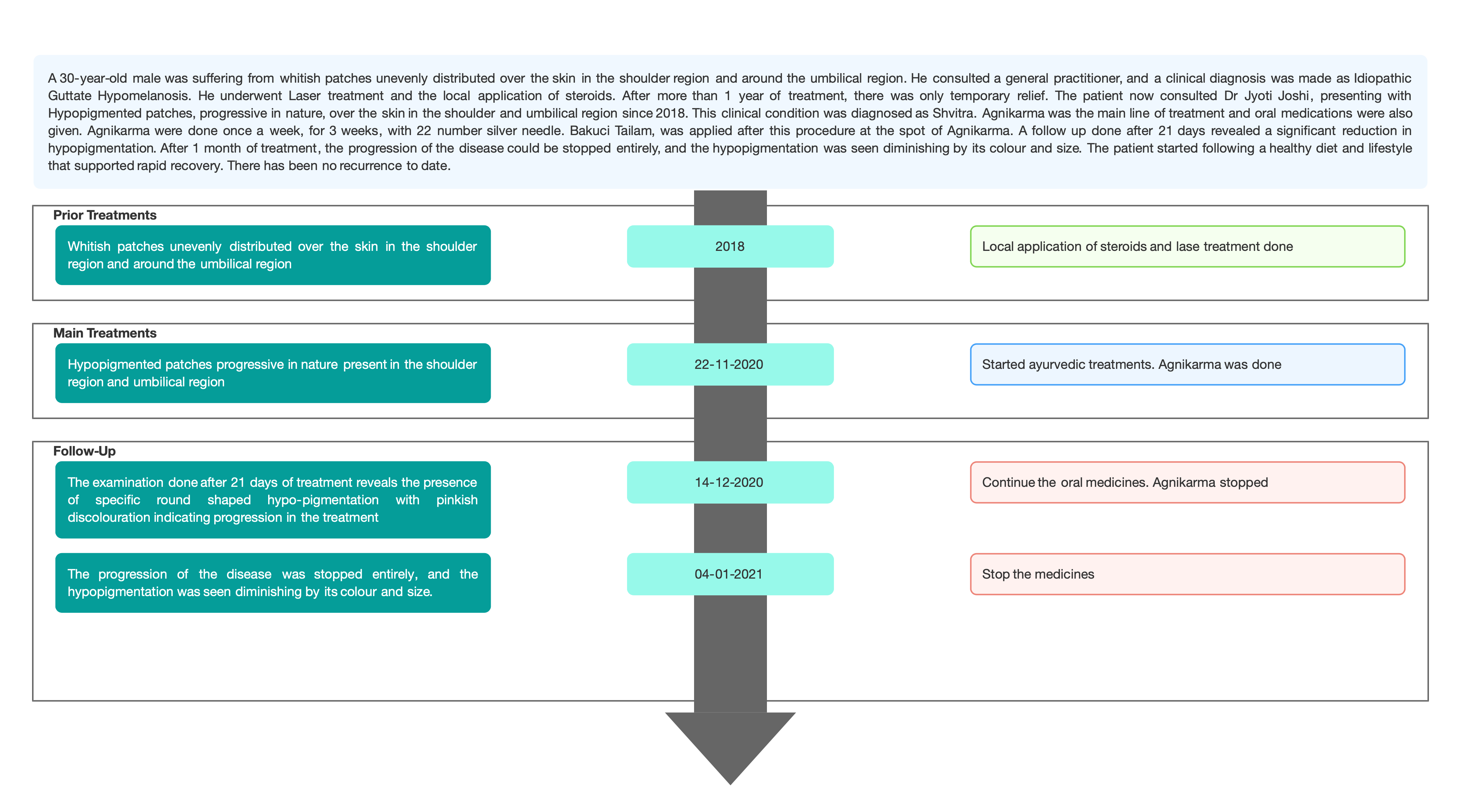
Image 2. Images taken before treatment
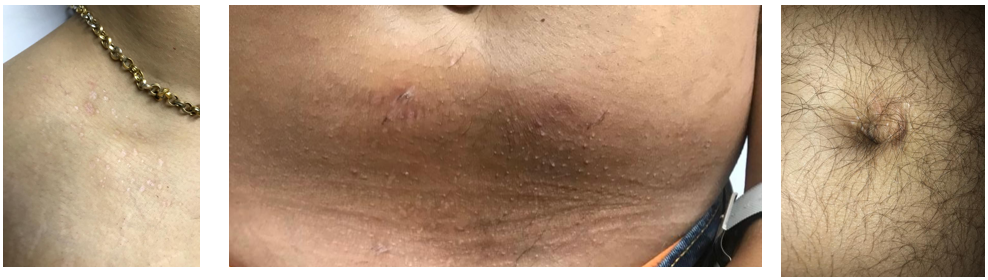
Image 3. Images taken during treatment
t
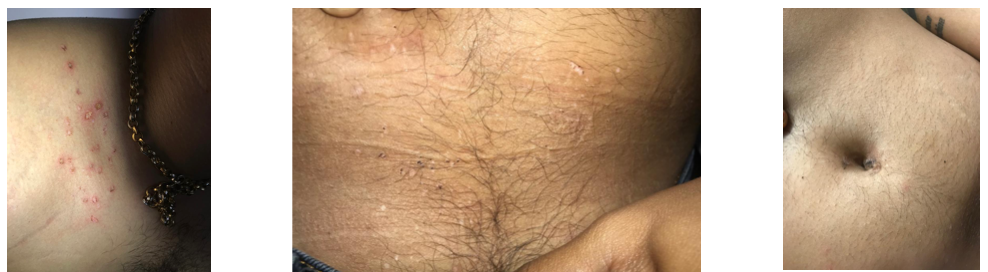
Image 4. Images taken after treatment
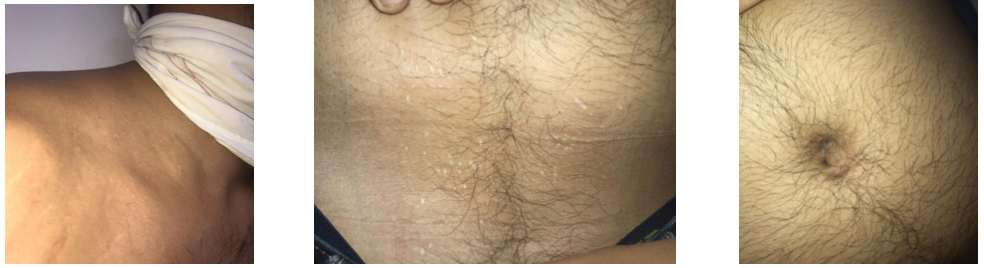
-
Immersive Learning
-
Modern Diagnosis
BIOMEDICAL DIAGNOSIS: Idiopathic guttate hypomelanosis
ABOUT THE DISEASE:
Idiopathic guttate hypomelanosis (IGH) is a benign, typically asymptomatic, leucodermic dermatosis of unclear aetiology that is classically seen in elderly, fair-skinned individuals, and often goes unrecognized or undiagnosed. Occasionally, IGH is aesthetically displeasing. However, it is not a dangerous process. Once present, lesions do not remit. Treatment is aimed at improving the cosmesis of lesions. This activity describes the clinical evaluation of idiopathic guttate hypo melanosis and explains the role of the health professional team in coordinating the care of this condition.
Aetiology: The aetiology of IGH remains unknown. Several hypotheses exist, including the notion that this is a manifestation of the skin's normal ageing process, occurs secondary to cumulative chronic sun exposure, or occurs as a result of repeated microtrauma to the skin
Diagnostic criteria: Medical history taking and clinical examination are the basic diagnostic criteria. Given the benign course of IGH, no laboratory, radiographic, or other tests are typically necessary to investigate these patients. Dermoscopy can be a valuable tool in the evaluation of lesions of IGH. In this case report, the patient is a 30-year-old male suffering from whitish patches unevenly distributed over the skin in the shoulder region and around the umbilical region. He consulted a general practitioner, and a clinical diagnosis was made as Idiopathic Guttate Hypomelanosis. He underwent Laser treatment and the local application of steroids. After more than 1 year of treatment, there was only temporary relief. The symptoms were progressing.
Image 1. Image of the hypopigmented patches before treatment added below

Patients should be reassured that lesions of IGH are benign and that no treatment is necessary. There are no universally accepted efficacious treatments for this condition.
In general, as sunlight is most likely a contributing or potentially even precipitating factor, the use of sunscreens and physical barriers should be recommended for all patients. In addition to photoprotection, treatment for cosmetic purposes are available and have shown variable promise used alone or in combination. These include cryotherapy, superficial abrasion, topical steroids, topical retinoids, topical calcineurin inhibitors, dermabrasion, topical 88% phenol, fractional carbon dioxide lasers, non-ablative fractional photothermolysis via fractional 1550-nm ytterbium/erbium fiber laser, and excimer light treatment.
Reference
- Brown F, Crane JS. Idiopathic Guttate Hypomelanosis. In: Stat Pearls. Treasure Island (FL): Stat Pearls Publishing; September 12, 2022.
-
Ayurveda Diagnosis
AYURVEDA DIAGNOSIS: Shvitra
ABOUT THE DISEASE:
Shvitra is correlated to Vitiligo in biomedicine bearing similarity in the presentation of symptoms. This is a common problem associated with an intense social stigma in the society.
According to Ayurveda, the skin is an essential sense organ. Basic energy principles like vata and one of the five heat-producing activities similar to metabolism (bhrajaka pitta) reside in the skin (called twak in sanskrit). As the skin covers the whole body bhrajaka pitta should be maintained in a proper state and it needs continuous care.
Shvitra and Kilasa are synonymous. But there are opinions that there are two subtypes. Sushruta explains that Kilasa is a variety that affects only the skin. Supporting his opinion, Madhava and Vagbhata view that Kilasa is nirdista as it remains at skin level (called the twakgata condition in Ayurveda). Caraka explains that Shvitra becomes firmly established when the dosha enters different levels of dhatu, indicated by a change in the colour of the lesions. When dosha enters dhatu, the disease shows a poor prognosis (asadhya). Bhoja identified more subcategories on the basis of nidana; originating from the dosha and from vrana. Sub-classifications in the doshaja variety are Daruna, Aruna, and Kilasa. Depending on the presentation of symptoms, shvitra can be classified as vata, pitta and kapha type. In this case report, the patient is 30-year-old male who suffered from whitish patches unevenly distributed over the skin in the shoulder region and around the umbilical region for 2 years, without getting satisfactory outcomes with conventional medicines. The subtype of Shvitra has not been specified by the treating physician.
Etiology
The causative factors for Kusta and Shvitra are the same and affect the same dhatu. Shvitra differs from other skin disorders by the normal functioning of all but the twak resulting in discolouration of the skin (twak vaivarnyata), without discharge (aparisravi). The dietary factors are also discussed in the causation of vitiligo. Seventeen ways of dietary intake are labelled as virudha diet. Excessive consumption of food that takes a longer time to digest (guru) and non-vegetarian and spicy foods are also associated with etiology.
Sadhyasadhyata
Good prognosis (sadhya) patients have lesions of recent onset (nava), are not thickened (thanu), and show pigmented hairs (ashukla roma). Patients who are likely to have poor prognosis exhibit lesions on the external genitalia, lips, and tips of fingers (Anthejatam), coalescing (samslista), and/or covering large areas of the body (bahala) or those that appears like burn wounds (agnidagdhaja).
Treatment: Classical textbooks of Ayurveda recommend four steps of treatment. The first step is shodhana karma using Psoralia corylifolia (bakuci kwatha) and Eurphorbia nerifolia (snuhi). This medicine is expected to induce multiple bouts of purgation. In the next step oil massage is advocated. The next step is the exposure of lesions to the sun rays as long as the patient can tolerate them (Soorya pada santhapam. The patient receives peya for the following three days. If bullae arise after a sun bath they must be punctured using a sterile needle. On these days, diet regulations should be strictly followed.
Ayurveda recommends several medicines alone or in combination, following the four steps of initial therapy mentioned earlier.
The rationale of treatment: Agnikarma was chosen as the main treatment, to induce the exact amount of heat required to initiate the healing process. This would help pacify the dosa and also prevent remission.
Reference
- Narahari SR, Aggithaya MG, Suraj KR. A protocol for systematic reviews of Ayurveda treatments. Int J Ayurveda Res. 2010 Oct;1(4):254-67. doi: 10.4103/0974-7788.76791. PMID: 21455455; PMCID: PMC3059450.
-
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Rasamanikya + Tamra basma + Bakuci curna + Kanchanara curna + Punarnava curna + Vijaysar Powder Rasamanikya 15mg + Tamra basma 10mg + Bakuci curna 500mg + Kanchanara curna 500mg + Punarnava curna 1 mg BD after food 2020-11-22 - 2021-01-02 Rasamanikya- Siddha Bheshaja Manimala. Jvara prakarana.66. Bakuci taila Taila Required quantity Apply on the spots of Agnikarma after the procedure 2020-11-22 - 2021-01-02 Anubhuta dravya prayoga -
Outcome Measures
OUTCOME MEASURES
ABOUT THE DISEASE:
A 30-year-old male was suffering from whitish patches unevenly distributed over the skin in the shoulder region and around the umbilical region. He consulted a general practitioner, and a clinical diagnosis was made as Idiopathic Guttate Hypomelanosis. He underwent Laser treatment and the local application of steroids. After more than 1 year of treatment, there was only temporary relief. The patient now consulted Dr Jyoti Joshi, presenting with Hypopigmented patches, progressive in nature, over the skin in the shoulder and umbilical region since 2018. This clinical condition was diagnosed as Shvitra.
Assessment criteria: Subjective parameters were the main criteria followed for assessing the outcomes.
A follow-up was done after 21 days and revealed a significant reduction in hypopigmentation. After 1 month of treatment, the progression of the disease could be stopped entirely, and the hypopigmentation was seen diminishing by its colour and size. The patient started following a healthy diet and lifestyle that supported rapid recovery. There has been no recurrence to date.
Image 1. The hypopigmented patches during treatment were added below

Image 2. The image was taken of the skin after the treatment

-





