Featured Case
-
Abstract
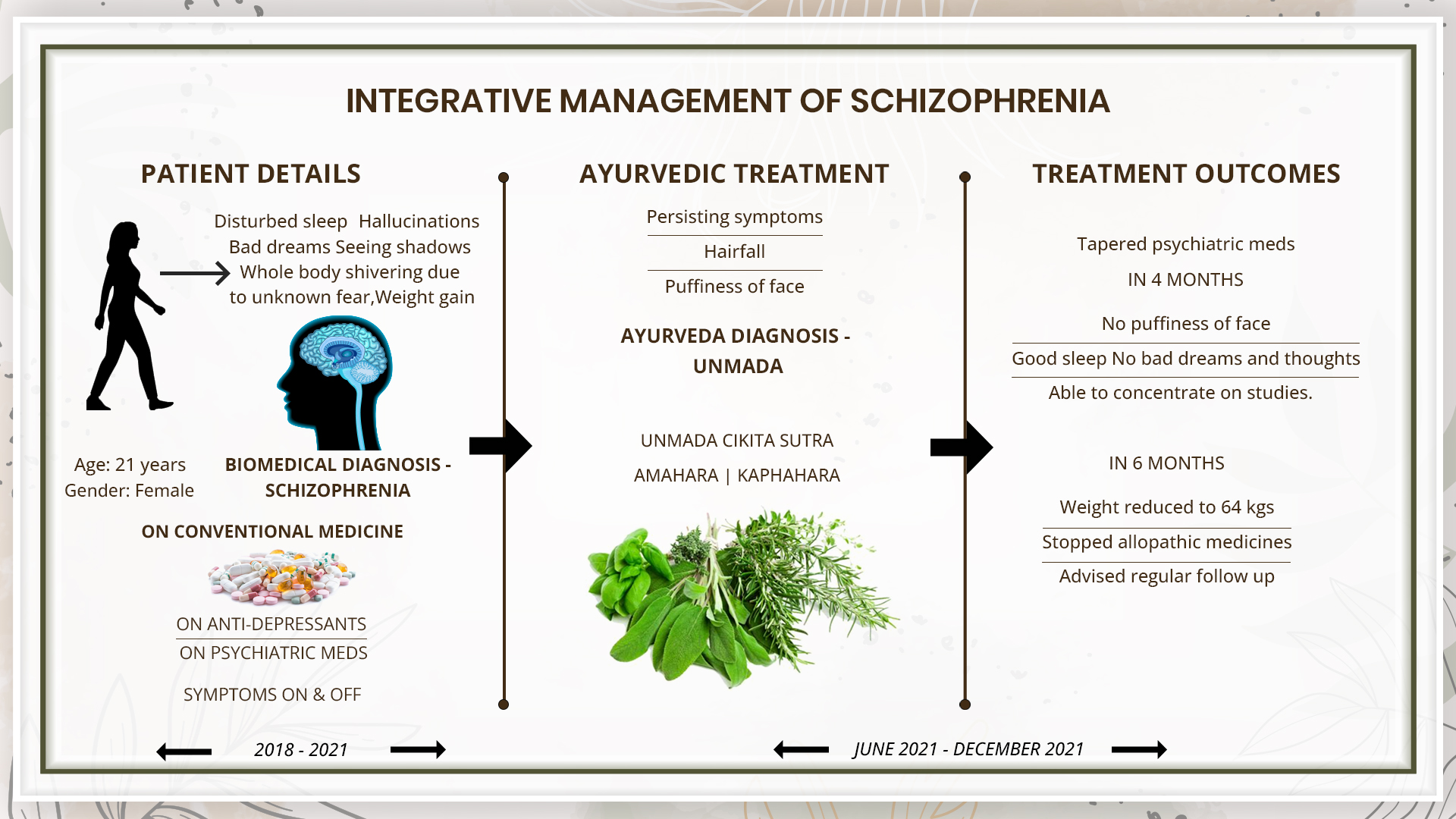
A 21-year-old female patient had an onset of hallucination and disturbed sleep with bad dreams in 2018. She immediately consulted a psychiatrist, and the provisional biomedical diagnosis made was schizophrenia. She started psychiatric drugs as prescribed by the doctor. She developed associated symptoms like whole body shivering due to unknown fear, hair fall, puffiness of the face and weight gain. Despite taking psychiatric drugs, over a period of 3 years, the symptoms were on and off. So, she approached Dr Jyoti Joshi for ayurvedic management. The ayurvedic diagnosis was unmada. The line of treatment followed was unmada cikitsa sutra, amahara and kapha shamana. With the Ayurveda treatment, the dose of psychiatric medicines could be tapered down in 4 months and completely stopped in 6 months. She got complete relief from her symptoms and all the ayurvedic medicines were stopped after 6 months. She is advised to come for regular follow ups.
-
Summaries
-
Listen
-
Watch
-
View
-
Read

A 21-year-old female patient had an onset of hallucination and disturbed sleep with bad dreams in 2018. She immediately consulted a psychiatrist, and the provisional biomedical diagnosis made was schizophrenia. She started psychiatric drugs as prescribed by the doctor. She developed associated symptoms like whole body shivering due to unknown fear, hair fall, puffiness of the face and weight gain. Despite taking psychiatric drugs, over a period of 3 years, the symptoms were on and off. So, she approached Dr Jyoti Joshi for ayurvedic management. The ayurvedic diagnosis was unmada. The line of treatment followed was unmada cikitsa sutra, amahara and kapha shamana. With the Ayurveda treatment, the dose of psychiatric medicines could be tapered down in 4 months and completely stopped in 6 months. She got complete relief from her symptoms and all the ayurvedic medicines were stopped after 6 months. She is advised to come for regular follow ups.
-
-
Timeline
-
Tabulated Summary
-
Narrative
TITLE OF CASE
Integrative management of Schizophrenia- a case report
Dr Jyoti Joshi
ABSTRACT
A 21-year-old female patient had an onset of hallucination and disturbed sleep with bad dreams in 2018. She immediately consulted a psychiatrist, and the provisional biomedical diagnosis made was schizophrenia. She started psychiatric drugs as prescribed by the doctor. She developed associated symptoms like whole body shivering due to unknown fear, hair fall, puffiness of the face and weight gain. Despite taking psychiatric drugs, over a period of 3 years, the symptoms were on and off. So, she approached Dr Jyoti Joshi. The ayurvedic diagnosis was unmada. The line of treatment followed was unmada cikitsa sutra, amahara and kapha shamana. With the Ayurveda treatment, the dose of psychiatric medicines could be tapered down in 4 months and completely stopped in 6 months. She got complete relief from her symptoms and all the ayurvedic medicines were stopped after 6 months. She is in remission.
KEYWORDS
Schizophrenia, unmada, case report, integrative
INTRODUCTION
Schizophrenia is a serious mental illness that affects how a person thinks, feels, and behaves. People with schizophrenia may seem like they have lost touch with reality, which can be distressing for them and for all surrounding them. The symptoms of schizophrenia can make it difficult to participate in usual, everyday activities, but effective treatments are available. Many people who receive treatment can engage in school or work, achieve independence, and enjoy personal relationships.
Schizophrenia symptoms can differ from person to person, but they generally fall into three main categories: psychotic, negative, and cognitive.
Hallucinations, delusions, thought and mood disorder are the common symptoms of schizophrenia. There can also be negative and cognitive symptoms.
Treatment strategy: Current treatments for schizophrenia focus on helping individuals manage their symptoms, improve day-to-day functioning, and achieve personal life goals, such as completing education, pursuing a career, and having fulfilling relationships. Anti-psychotic medications, psychosocial treatment, counselling, family and friends education and support, Coordinated Specialty Care, and Assertive Community Treatment are some treatment options.
Prognosis: There is no cure for schizophrenia. But with medical intervention, the quality of life can be maintained.
PATIENT INFORMATION
A 21-year-old female patient had an onset of hallucination and disturbed sleep with bad dreams in 2018. Associated complaints- whole body shivering due to unknown fear, hair fall, puffiness of the face and weight gain developed over a period of 3 years.
Medical History: She immediately consulted a psychiatrist, and the provisional biomedical diagnosis made was schizophrenia. She started psychiatric drugs as prescribed by the doctor. She developed associated symptoms like whole body shivering due to unknown fear, hair fall, puffiness of the face and weight gain. Despite taking psychiatric drugs, over a period of 3 years, the symptoms were on and off.
CLINICAL FINDINGS/PHYSICAL EXAMINATION
A general examination was done. No specific anomalies were detected. Vitals are normal.
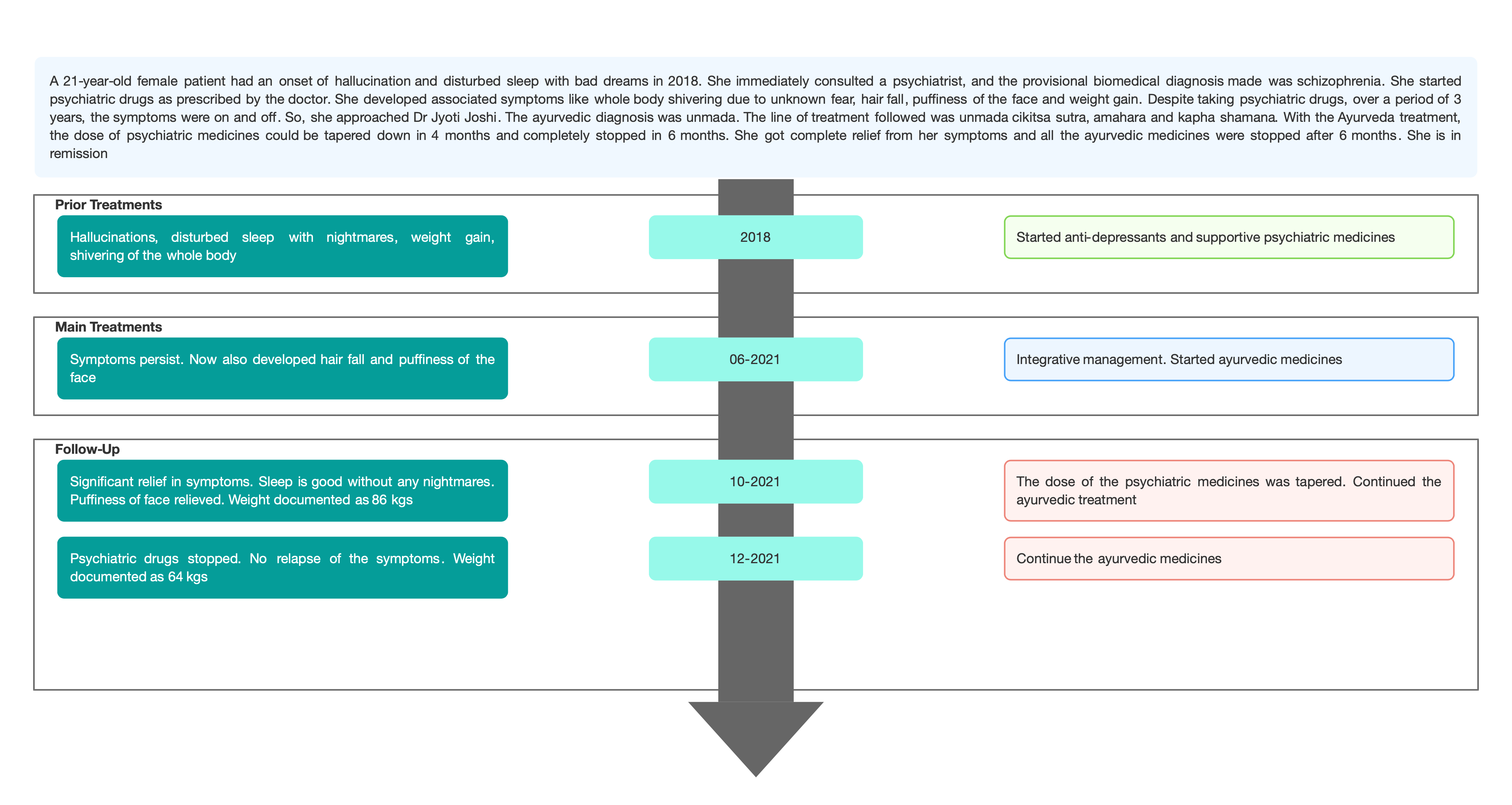
TIMELINE
Image 1. Timeline of events attached below
DIAGNOSTIC ASSESSMENT
Modern Diagnostic parameter: Biomedical diagnosis was made based on the clinical presentation and evaluation.
Image 2. Prescriptions of regular psychiatric medicines taken by the patient added below.
Ayurvedic Assessment was done based on the clinical evaluation by the ayurvedic physician.
Differential Diagnosis- This does not apply as the patient came in with a definite diagnosis.
Prognosis- In schizophrenia, the prognosis is dependent on several factors. Insidious onset, childhood or adolescent onset, poor premorbid adjustment, and cognitive impairment are indicative of a poor prognostic outcome, whereas acute onset, and living in a developed country signal comparatively better prognostic factors. However, suicide is the most common cause of premature death in schizophrenia, with two-thirds of patients reporting at least one episode of suicidal ideation. Treatment-resistant schizophrenia is when the condition fails to respond to at least two antipsychotic medications for at least six weeks. In this case, the patient is 21 years old, which indicates a poor prognosis and was also under psychiatric treatment. In spite of taking medicines, the symptoms persisted, and hence they opted for Ayurveda care; Her psychiatric drugs could be tapered gradually and completely stopped in 6 months.
THERAPEUTIC INTERVENTION
See the tab ‘Treatment details’
FOLLOW-UP AND OUTCOMES
Clinician-based assessment; After 4 months of treatment:
No puffiness of the face
Good sleep
No bad dreams and thoughts
Able to concentrate on studies.
With the Ayurveda treatment, the dose of psychiatric medicines could be tapered in 4 months and the patient could completely stop the medicines in 6 months.
Objective parameters: None
Patient-assessed; Not relevant.
Intervention adherence and tolerability – The patient adhered to the prescribed treatments and tolerated the treatments well.
Method of assessment- By monitoring the patient.
Adverse and unanticipated events; None reported.
DISCUSSION ;
In this case report, the ayurvedic diagnosis was unmada. The treatment administered was Chitrakadi vati as a part of amahara cikitsa and panchagavya ghrita- indicated in unmada and is kapha shamana.
PATIENT’S PERSPECTIVE
Video of the patient's narrative is available with the patient’s consent. The identity is masked.
LEARNING POINTS/TAKE-HOME MESSAGES
This case report demonstrates how ayurvedic intervention could help manage the symptoms, and taper the dose of psychiatric drugs and stop them altogether in a 21-year-old female patient, who was responding satisfactorily to conventional medicines.
INFORMED CONSENT
Written consent was obtained from the patient with the family’s knowledge to publish the case report.
CONFLICT OF INTEREST
None declared.
FUNDING
None
REFERENCE
Image 1. Timeline of events added below
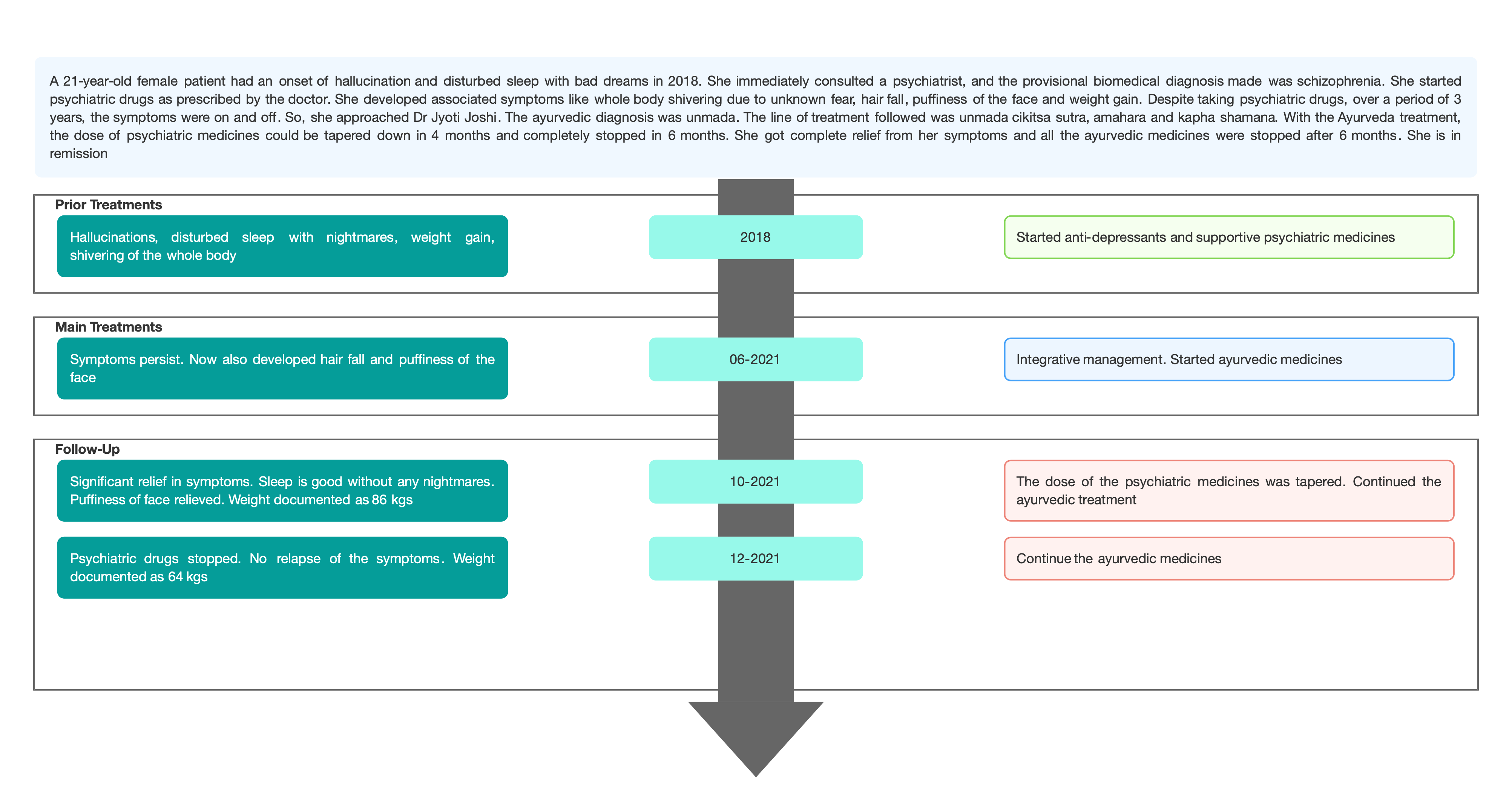
Image 2. Prescription medicines the patient was taking

-
Immersive Learning
-
Modern Diagnosis
MODERN DIAGNOSIS: Schizophrenia
ABOUT THE DISEASE:
Schizophrenia is a serious mental illness that affects how a person thinks, feels, and behaves. People with schizophrenia may seem like they have lost touch with reality, which can be distressing for them and for all surrounding them. The symptoms of schizophrenia can make it difficult to participate in usual, everyday activities, but effective treatments are available. Many people who receive treatment can engage in school or work, achieve independence, and enjoy personal relationships.
It’s important to recognize the symptoms of schizophrenia and seek help as early as possible. People with schizophrenia are usually diagnosed between the ages of 16 and 30, after the first episode of psychosis. Starting treatment as soon as possible following the first episode of psychosis is an important step toward recovery. However, research shows that gradual changes in thinking, mood, and social functioning often appear before the first episode of psychosis. Schizophrenia is rare in younger children.
Schizophrenia symptoms can differ from person to person, but they generally fall into three main categories: psychotic, negative, and cognitive.
Hallucinations, delusions, thought and mood disorder are the common symptoms of schizophrenia. There can also be negative and cognitive symptoms.
In this case report, a 21-year-old female patient had an onset of hallucination and disturbed sleep with bad dreams in 2018. She immediately consulted a psychiatrist, and the provisional biomedical diagnosis made was schizophrenia. She started psychiatric drugs as prescribed by the doctor. She developed associated symptoms like whole body shivering due to unknown fear, hair fall, puffiness of the face and weight gain. Despite taking psychiatric drugs, over a period of 3 years, the symptoms were on and off.
Image 1. Prescriptions of regular psychiatric medicine taken by the patient added below

References from:
-
Ayurveda Diagnosis
AYURVEDA DIAGNOSIS: Unmada
ABOUT THE DISEASE:
Unmada covers a wide range of major mental disorders and is considered synonymous with madness and mental derangement, in which a person loses his/her contact with reality and loses the ability to regulate his/her actions and conduct according to norms of the society.
In unmada there is an upward movement of doshas leading to disturbance in the functions of manas causing mada in an individual. The factual clinical picture of the mental status of psychotic patients is vividly described. This description suggests that a patient of unmada develops derangement of all the activities of manas, buddhi, ahamkara, and indriyas. He develops thought disturbances in the form of abnormalities of chintana, vichara and uhya, derangement of memory in the form of smriti nasha, and smriti bramsha; behavioural, social and emotional disturbances in the form of abnormalities of achara, dharma and bhavas along with functional derangement of indriyas causing abaddha vakya, and hridaya shunyata.
Thus, unmada is not a lone clinical entity comparable to a single modern diagnostic category, rather it is a syndrome describing a group of psychotic disorders. It is a common and broader entity, which provides guidance to the line of management for almost all psychiatric disorders from an Ayurvedic perspective. As psychotic disorders cover almost all the major mental illnesses, the different types and sub-types of unmada can be separately correlated with different psychotic disorders. The clinical features of the different types of unmada resemble various types of schizophrenia, manic psychosis, psychotic depression and major depressive disorders. Unmada is divided into two broad categories –
(1) Nija- those caused by vitiation of dosa
(2) Agantunimitta- those caused by exogenous factors.
Taken from https://www.carakasamhitaonline.com/index.php?title=Unmada_Chikitsa
In this case report, a 21-year-old female patient had an onset of hallucination and disturbed sleep with bad dreams in 2018. She immediately consulted a psychiatrist, and the provisional biomedical diagnosis made was schizophrenia. She started psychiatric drugs as prescribed by the doctor. She developed associated symptoms like whole body shivering due to unknown fear, hair fall, puffiness of the face and weight gain. Despite taking psychiatric drugs, over a period of 3 years, the symptoms were on and off. So, she approached Dr Jyoti Joshi for ayurvedic management. The diagnosis was unmada. The line of treatment followed was unmada cikitsa sutra, amahara and kapha shamana.
Causes of unmada: Acarya Susruta mentions the factors responsible for causing unmada
विरुद्धदुष्टाशुचिभोजनानि प्रधर्षणं देवगुरुद्विजानाम्|
उन्मादहेतुर्भयहर्षपूर्वो मनोऽभिघातो विषमाश्च चेष्टाः||४||Viruddha, dusta and ashuci bhojana, possession by evil or good spirits, emotions like fear, happiness, feeling hurt and improper activities are the nidana.
Symptoms:
धीविभ्रमः सत्त्वपरिप्लवश्च पर्याकुला दृष्टिरधीरता च|
अबद्धवाक्त्वं हृदयं च शून्यं सामान्यमुन्मादगदस्य लिङ्गम्||६||Defective intellect, psychic agitation, restlessness in eyes, impatience, incoherent speech and feeling of emptiness in hridaya, are the general features of unmada.
Treatment
In the nija type of unmada, the treatment should be planned taking into consideration the dosa vitiated, the age, bala and agni. In agantu unmada is bali, mangala karma, homa, aushadhi-dharana, agada-dharana, satya-achara, tapa, jnana, pradana, niyama, vrata; worship of god, cows, brahmanas and guru, by sacred hymns and drugs are advocated.
-
Treatment
Name of Medicine Dosage Form Dosage Mode of Administrtation From - To (Date) Medicine Reference Citrakadi vati Vati 1 Tablet TDS, with warm water 2021-06-07 - 2021-12-15 Bhaishajya ratnavali. Vatavyadhi Cikitsa Pancagavya Ghrita Ghrita 1 Tablet TDS, with warm water 2021-06-07 - 2021-12-15 AH.Ci.12.19-23 Tila Taila Taila Required quantity Application on head 2021-06-15 - 2021-06-21 Kaiyyadeva Nighantu.Drava varga. 347-348 Vaca curna Curna Required quantity Udhvartanam 2021-06-07 - 2021-06-12 Anubhuta dravya yoga Gomutra haritaki Tablets 0-0-2 With warm water at bedtime 2021-06-15 - 2021-06-21 SS. Arsha Cikitsa -
Outcome Measures
OUTCOME MEASURES
A 21-year-old female patient had an onset of hallucination and disturbed sleep with bad dreams in 2018. She immediately consulted a psychiatrist, and the provisional biomedical diagnosis made was schizophrenia. She started psychiatric drugs as prescribed by the doctor. She developed associated symptoms like whole body shivering due to unknown fear, hair fall, puffiness of the face and weight gain. Despite taking psychiatric drugs, over a period of 3 years, the symptoms were on and off. So, she approached Dr Jyoti Joshi. The ayurvedic diagnosis was unmada. The line of treatment followed was unmada cikitsa sutra, amahara and kapha shamana.
Subjective parameters: With the Ayurveda treatment, the dose of psychiatric medicines could be tapered down in 4 months and completely stopped in 6 months. She got complete relief from her symptoms and all the ayurvedic medicines were stopped after 6 months. The patient is requested to come for regular follow-up.
Video 1: Patient narrating the timeline of events added below.
-



